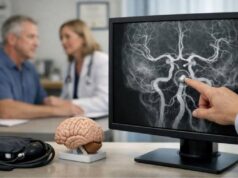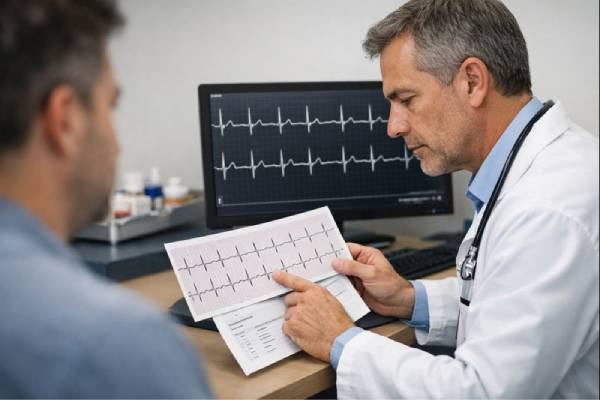
Bacterial myocarditis is inflammation and injury of the heart muscle caused by bacteria or bacterial toxins. It is far less common than viral myocarditis, but it can be more dangerous because it may arrive as part of a wider bloodstream infection, severe pneumonia, or a toxin-mediated illness like diphtheria. Some people become sick quickly with shock, rhythm disturbances, or sudden heart failure. Others have a slower course with chest pain, shortness of breath, and fatigue that can look like a heart attack or a viral “cold that moved into the chest.” The challenge is that the heart’s warning signals are limited, while the causes are diverse. A clear diagnosis usually depends on matching the story, blood tests, imaging, and—when needed—direct sampling of heart tissue. Treatment focuses on rapid antibiotics, supportive cardiac care, and close monitoring for complications that can change hour by hour.
Table of Contents
- What bacterial myocarditis is and how it damages the heart
- What causes bacterial myocarditis and who is at risk
- Symptoms, red flags and possible complications
- How bacterial myocarditis is diagnosed
- Treatment options and what to expect in hospital
- Recovery, prevention and when to seek urgent care
What bacterial myocarditis is and how it damages the heart
“Myocarditis” means inflammation of the myocardium, the muscle layer responsible for pumping blood. In bacterial myocarditis, that inflammation is triggered by bacteria directly invading the heart tissue, by bacterial toxins, or by an intense immune response set off by bacterial infection elsewhere in the body. What makes bacterial myocarditis clinically important is not just the inflammation itself, but how quickly it can disrupt the heart’s two core jobs: pumping and maintaining a stable rhythm.
Three main patterns clinicians think about
- Direct infection of the heart muscle (true bacterial invasion)
Bacteria can seed the myocardium during bacteremia (bacteria in the blood) and form tiny pockets of infection called microabscesses. This can happen in severe sepsis, in people with weakened immunity, or alongside infections like pneumonia or skin and soft tissue infections. The heart may look “inflamed” on imaging, and the patient can deteriorate rapidly. - Toxin-mediated injury
Some bacteria injure the heart mainly through toxins rather than heavy bacterial growth inside the myocardium. Diphtheria is the classic example: toxin can affect heart muscle and the electrical conduction system, leading to dangerous arrhythmias and heart failure, sometimes after the throat symptoms start to improve. - Inflammation linked to bacterial infection without heavy bacterial load in the heart
Lyme disease (caused by Borrelia) often targets the conduction system, leading to heart block and rhythm problems. The myocardium can be involved as well, and symptoms may overlap with myocarditis or pericarditis.
Why the heart is vulnerable
The heart is highly metabolic and depends on tight electrical coordination. Inflammation can cause:
- Reduced pumping strength (lower ejection fraction)
- Swelling that makes the heart stiff, impairing filling
- Irritable electrical pathways that trigger extra beats, ventricular tachycardia, or conduction block
- In severe cases, cardiogenic shock, where the body’s organs do not receive enough blood flow
A practical way to understand the risk is this: mild myocarditis may feel like chest discomfort and fatigue, but severe myocarditis can look like a sudden heart failure or an electrical storm. Bacterial myocarditis deserves urgent attention because the underlying driver—an active bacterial infection or toxin—may continue to cause damage until it is specifically treated.
What causes bacterial myocarditis and who is at risk
Bacterial myocarditis is uncommon, but it tends to appear in settings where bacteria or bacterial toxins have a clear path to harm the heart. Knowing the typical causes and risk patterns can help clinicians and patients move faster when symptoms start.
Common bacterial and toxin-related causes
- Sepsis-related myocardial infection or microabscesses
Organisms like Staphylococcus aureus and streptococci are frequently implicated when bacteremia is present. In these cases, myocarditis may occur alongside infection in the lungs, skin, bones, or bloodstream. - Diphtheria toxin
Corynebacterium diphtheriae can produce a toxin that injures heart muscle and the conduction system. Myocarditis may develop days after initial respiratory symptoms and can present with rhythm problems before obvious heart failure. - Lyme-associated cardiac involvement
Borrelia infection can inflame cardiac tissue and often affects conduction, leading to varying degrees of atrioventricular block. Symptoms may be subtle, and a person may not recall a tick bite or rash. - Less common bacterial sources
Some cases involve organisms linked to specific exposures or immune states, such as Salmonella in immunocompromised patients, meningococcal infection in severe systemic illness, or tuberculosis in chronic disease patterns.
Risk factors that raise suspicion
Bacterial myocarditis should be considered more strongly when myocarditis-like symptoms occur in someone with:
- Recent or active bacterial infection (pneumonia, skin infection, urinary infection, dental infection)
- Fever with signs of sepsis (low blood pressure, confusion, rapid breathing, rising lactate)
- Immunosuppression (cancer therapy, transplant medicines, high-dose steroids, advanced HIV)
- Hemodialysis or frequent vascular access
- Injection drug use or long-term IV access devices
- Travel or vaccination gaps relevant to diphtheria risk
- Outdoor exposure in endemic regions for tick-borne illness
Why “cause” matters more than the label
Two people can both be told “myocarditis,” yet need very different care. Viral myocarditis is often treated with supportive measures. Bacterial myocarditis may require urgent antibiotics, toxin-directed therapy (for example, antitoxin in diphtheria when indicated), and aggressive monitoring for conduction failure. The most useful mindset is: myocarditis is a syndrome, and bacterial myocarditis is a high-stakes subgroup where identifying the trigger is not optional—it is the treatment.
Symptoms, red flags and possible complications
Bacterial myocarditis can start with symptoms that are easy to misread—especially when the body is also fighting a lung infection, throat infection, or bloodstream infection. The heart’s early warnings are often nonspecific, but there are patterns that deserve attention.
Common symptoms
Many people experience a mix of:
- Chest pain or chest pressure (sometimes sharp, sometimes heavy)
- Shortness of breath, especially with exertion or when lying flat
- Palpitations (a sense of fluttering, racing, or skipped beats)
- Fatigue and unusual weakness
- Lightheadedness or near-fainting
- Fever or chills when infection is active
- Swelling in legs or rapid weight gain if fluid builds up
In toxin-mediated or conduction-focused disease, chest pain may be minimal. Instead, the first clue can be dizziness, fainting, or a slow pulse.
Red flags that warrant urgent evaluation
Seek urgent care if any of these occur:
- Fainting, repeated near-fainting, or new confusion
- Sudden shortness of breath at rest, frothy sputum, or a feeling of suffocation when lying down
- Sustained heart racing, new severe palpitations, or a very slow heart rate
- Chest pain with sweating, nausea, or radiating discomfort
- Signs of shock: cold clammy skin, very low blood pressure symptoms, minimal urine output
- New neurologic symptoms (weakness, facial droop, speech difficulty), which can occur if infection elsewhere causes embolic events or if severe illness triggers clot risk
Complications to understand
Bacterial myocarditis can lead to complications that shape both treatment and recovery:
- Arrhythmias and conduction block
Inflammation can irritate the ventricles or disrupt the atrioventricular node. Lyme-related involvement is well known for causing varying degrees of heart block. Diphtheria can cause both conduction problems and dangerous ventricular rhythms. - Acute heart failure
The heart may weaken suddenly, leading to pulmonary edema and low oxygen levels. Some cases progress to cardiogenic shock. - Mixed shock states
Severe infection can cause distributive shock (from sepsis) while myocarditis causes cardiogenic shock. This combination is especially dangerous and requires specialized critical care. - Long-term remodeling
Even after infection clears, some patients are left with reduced pumping function or a dilated cardiomyopathy pattern. Others recover fully, especially when treated early and monitored closely.
A useful practical point: the most serious events in myocarditis often happen early, before the diagnosis feels “certain.” That is why persistent chest symptoms in the context of bacterial infection, unexplained fainting, or new rhythm abnormalities should be treated as time-sensitive.
How bacterial myocarditis is diagnosed
Diagnosis aims to answer two questions at the same time: “Is this myocarditis?” and “Is bacteria or bacterial toxin the driver?” The second question changes treatment urgency and antibiotic choices.
Initial evaluation and bedside clues
Clinicians typically start with:
- History of recent infection, tick exposure, vaccination status relevant to diphtheria, immune status, and IV access risks
- Vital signs (fever, low blood pressure, fast breathing) suggesting sepsis or shock
- Physical exam for fluid overload, new murmurs, lung crackles, rash, or neurologic changes
Core tests
- ECG
May show ST-T changes, conduction delays, heart block, or ventricular ectopy. In Lyme disease, fluctuating atrioventricular block is a classic clue. - Cardiac biomarkers
Troponin often rises due to myocardial injury. BNP or NT-proBNP can rise when heart failure develops. These tests support the diagnosis but do not specify the cause. - Blood work for infection
CBC, CRP, procalcitonin (in some settings), lactate, kidney and liver tests help assess infection severity and organ impact. - Blood cultures
If bacterial myocarditis is possible, cultures are important before antibiotics when feasible and safe. Positive cultures can identify the organism and guide targeted therapy. - Echocardiography
Ultrasound can show reduced heart function, wall motion abnormalities, pericardial effusion, and evidence of heart failure. It also helps rule out other emergencies and can identify endocarditis features when present. - Cardiac MRI
When available and the patient is stable, MRI can characterize inflammation, edema, and tissue injury patterns. It is especially helpful when symptoms mimic a heart attack but coronary arteries appear normal.
When the cause is still unclear
- Coronary evaluation
Because myocarditis can mimic acute coronary syndrome, clinicians may evaluate coronary arteries when the presentation suggests a heart attack. - Targeted infectious testing
Examples include serology for Lyme disease in an appropriate epidemiologic setting or specific testing when diphtheria is suspected. - Endomyocardial biopsy in selected cases
Biopsy is not routine for everyone, but it can be critical in severe, rapidly worsening cases, in refractory arrhythmias, or when a specific diagnosis would change management. Biopsy can help confirm myocarditis, look for bacterial invasion, and guide therapy decisions.
A helpful way to frame the diagnostic process: bacterial myocarditis is often not proven by a single test. It is built from a pattern—cardiac injury plus an infection signal plus imaging or rhythm evidence—then refined as microbiology results return.
Treatment options and what to expect in hospital
Treatment usually happens in the hospital because bacterial myocarditis can shift quickly from “concerning” to “unstable.” The plan typically combines infection control, heart support, and continuous monitoring.
Antibiotics and infection-directed therapy
- Empiric antibiotics when bacterial cause is plausible
If a patient is critically ill or sepsis is suspected, antibiotics are started promptly after obtaining blood cultures when possible. The initial regimen is chosen based on likely sources (skin, lungs, urinary tract), local resistance patterns, and patient-specific risks. - Targeted antibiotics once the organism is identified
When cultures or other tests identify the organism, therapy is narrowed to the most effective option. Duration varies widely depending on the organism, whether bacteremia persists, and whether other sites (like valves, lungs, or bones) are involved. - Toxin-focused care when relevant
In suspected diphtheria, time-sensitive management may include antitoxin alongside antibiotics and airway support, depending on clinical guidance and availability. The cardiac component often needs prolonged monitoring because conduction problems can appear after the initial infection is recognized. - Lyme-related cardiac care
Antibiotics are used, and the route (oral vs IV) depends on illness severity and conduction findings. Patients with significant heart block may require hospitalization and temporary pacing support until conduction improves.
Supportive cardiac treatment
Because myocarditis can impair pumping and trigger arrhythmias, supportive measures are often just as important as antibiotics:
- Oxygen and diuretics if fluid overload is present
- Guideline-based heart failure medications when blood pressure and kidney function allow
- Treatment of arrhythmias with appropriate medications, cardioversion when needed, and electrolyte optimization
- Temporary pacing for symptomatic bradycardia or high-grade heart block
- Intensive care therapies for shock, including vasopressors, inotropes, and mechanical circulatory support in select severe cases
Monitoring that patients should expect
Many hospitals use:
- Continuous telemetry for rhythm monitoring
- Repeat troponin and inflammatory markers to follow the trend
- Repeat echocardiography if symptoms change or shock develops
- Repeat blood cultures if bacteremia was present or fever persists
What a “good response” looks like
Improvement is often measured by:
- Fever resolving and cultures clearing
- Blood pressure stabilizing without escalating medications
- Reduced oxygen needs
- Rhythm normalizing or heart block improving
- Echocardiographic recovery of function over days to weeks
Treatment can feel intense, but it is structured around a simple priority: stop the bacterial driver and protect the heart while it heals.
Recovery, prevention and when to seek urgent care
Recovery from bacterial myocarditis is often a “two-track” process: infection recovery plus cardiac recovery. Even when bacteria are cleared, fatigue and reduced exercise tolerance can persist for weeks. A good recovery plan anticipates that reality and builds in follow-up and safety nets.
After discharge: what helps most
- Follow-up with cardiology and, when relevant, infectious diseases
Follow-up usually includes symptom review, medication adjustment, and repeat imaging or ECG monitoring. - Activity restrictions and gradual return
Many clinicians recommend avoiding strenuous activity for a period, then reintroducing exercise gradually as symptoms, rhythm, and heart function allow. A paced return is safer than “pushing through” early fatigue. - Medication adherence and monitoring
Heart failure medicines, diuretics, or rhythm-related prescriptions work best when taken consistently. Lab checks may be needed for kidney function and electrolytes. - Watching for relapse or late complications
Reasons to contact a clinician promptly include return of fever, worsening shortness of breath, new swelling, or new palpitations.
Prevention strategies that match real-world risks
Prevention depends on the pathway that led to illness:
- Treat bacterial infections early (skin abscesses, pneumonia, urinary infections) and complete prescribed antibiotics
- Reduce bloodstream infection risk by careful line care if IV access is required
- Harm reduction and treatment support for injection drug use, when applicable
- Tick bite prevention in endemic regions: protective clothing, repellents, and prompt tick removal
- Vaccination updates where appropriate, including maintaining diphtheria-containing vaccine boosters according to local schedules
When to seek urgent care
Get urgent medical help if you have:
- Fainting, severe dizziness, or a very slow or very fast heart rate
- New chest pain that is severe, persistent, or accompanied by sweating or nausea
- Shortness of breath at rest, blue lips, or rapid worsening breathing
- Sudden weakness, facial droop, difficulty speaking, or severe headache
- Signs of shock: confusion, extreme sleepiness, cold clammy skin, or inability to stay awake
A final practical note: many people do recover well, especially when the cause is identified early and monitored closely. The goal is not only survival of the acute illness, but also protecting long-term heart function through follow-up, medication optimization, and safe return to activity.
References
- 2025 ESC Guidelines for the management of myocarditis and pericarditis 2025 (Guideline)
- Infectious factors in myocarditis: a comprehensive review of common and rare pathogens 2024 (Systematic Review)
- Clinical Practice Guidelines by the Infectious Diseases Society of America (IDSA), American Academy of Neurology (AAN), and American College of Rheumatology (ACR): 2020 Guidelines for the Prevention, Diagnosis, and Treatment of Lyme Disease 2021 (Guideline)
- Novel Clinical Monitoring Approaches for Reemergence of Diphtheria Myocarditis, Vietnam 2022 (Clinical Review)
- Clinical management of diphtheria: guideline, 2 February 2024 2024 (Guideline)
Disclaimer
This article is for educational purposes and does not replace medical advice, diagnosis, or treatment from a qualified clinician. Bacterial myocarditis can be life-threatening and may require urgent hospital care, including antibiotics and intensive cardiac monitoring. If you have chest pain, shortness of breath, fainting, a racing or very slow heartbeat, or fever with signs of severe illness, seek emergency evaluation right away. Never start, stop, or change antibiotics, heart medicines, or activity restrictions based on an article; follow the plan given by your healthcare team.
If this article helped you, please share it on Facebook, X (formerly Twitter), or any platform you prefer, and follow us on social media. Your support through sharing helps our team continue producing reliable, high-quality health content.