Baroreflex failure is a rare but high-impact disorder in which the body loses its fastest, most reliable “autopilot” for blood pressure control. In healthy people, pressure sensors in the carotid arteries and aorta send beat-to-beat signals to the brainstem, which adjusts heart rate and blood vessel tone within seconds. When that feedback loop is damaged, blood pressure can swing dramatically—surging very high during stress or pain, then dropping low with standing or after meals. These shifts are not just uncomfortable; they can lead to fainting, falls, emergency visits, and long-term strain on the heart, brain, and kidneys. The condition is most often seen after neck radiation or surgery, but other causes exist. With the right diagnosis and a practical, personalized plan, many people can reduce the extremes and regain predictability in daily life.
Table of Contents
- What baroreflex failure is and what goes wrong
- Common causes and who is most at risk
- Symptoms, patterns and serious complications
- How baroreflex failure is diagnosed
- Treatments that reduce blood pressure swings
- Day-to-day management and when to seek urgent care
What baroreflex failure is and what goes wrong
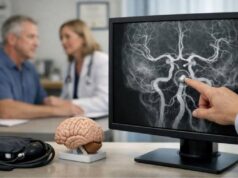
The baroreflex is the body’s rapid blood-pressure stabilizer. Specialized stretch receptors in the carotid sinus (neck) and aortic arch (chest) sense each pulse. When blood pressure rises, these receptors signal the brainstem to slow the heart and relax blood vessels. When pressure falls—such as when you stand—signals shift in the opposite direction, increasing heart rate and tightening vessels to keep blood flowing to the brain.
In baroreflex failure, that sensing-and-response loop becomes unreliable or disappears. The result is not “steady high blood pressure” or “steady low blood pressure,” but volatility: pressure and heart rate can rise together during surges and fall together during drops. People often describe it as feeling as though their body overreacts to ordinary events. A stressful conversation, a sudden loud noise, or pain can trigger a sympathetic surge with severe hypertension. Then, in quiet moments or when standing, the same person may have orthostatic hypotension and dizziness.
Clinicians often talk about two broad categories:
- Afferent baroreflex failure: damage to the sensory input from the carotid sinus or aortic receptors to the brainstem. This is the most classic pattern, frequently linked to neck radiation or surgery.
- Central or efferent patterns: problems in the brainstem processing centers or the outgoing autonomic pathways. These can overlap with other autonomic disorders and may produce a different mix of symptoms.
A helpful mental model is “loss of buffering.” The body still has stress hormones and sympathetic nerves, but the brake pedal is missing. Without the baroreflex, the brain cannot dampen pressure spikes or quickly correct pressure drops. Over time, repeated extremes can strain blood vessels and organs. Still, treatment does not usually aim for perfectly normal readings every hour. Instead, the goal is to reduce the peaks and valleys, prevent injuries from fainting, and lower the cumulative risk of stroke, heart failure, and kidney damage.
Because the condition is rare and can mimic more common problems—panic attacks, medication side effects, or labile essential hypertension—many patients benefit from care in a clinic familiar with autonomic disorders. Clear recognition of the pattern is often the turning point toward effective management.
Common causes and who is most at risk
Baroreflex failure usually happens when the nerves carrying signals from blood pressure sensors are injured, particularly around the carotid sinus in the neck. The most frequent real-world scenario is a person who has recovered from head and neck cancer treatment and later develops unpredictable blood pressure swings. Damage may be delayed because radiation can cause gradual scarring and nerve dysfunction over time.
Common causes include:
- Neck radiation therapy: especially when fields include the carotid sinus region. Risk rises with higher cumulative dose and broader treatment areas.
- Neck surgery: procedures that disturb the carotid sinus nerve or nearby structures, such as extensive tumor resections, bilateral carotid body tumor surgery, or radical neck dissection.
- Carotid interventions or trauma: less commonly, injury after carotid surgery or severe neck trauma can affect baroreceptor signaling.
- Brainstem lesions: stroke, tumors, inflammation, or degenerative disease affecting the nucleus tractus solitarius and related centers can disrupt baroreflex processing.
- Congenital or hereditary autonomic disorders: familial dysautonomia is a well-known example of congenital afferent dysfunction, though it is rare.
- Combined insults: some patients have a “double hit,” such as prior radiation plus later surgery, which increases the chance of clinically significant failure.
Risk factors are therefore often medical-history driven rather than lifestyle driven. People at higher risk include:
- Survivors of head and neck cancers who received radiotherapy, particularly with additional neck surgery.
- Individuals with bilateral carotid body tumors or paragangliomas requiring surgery on both sides.
- Patients with a history of repeated neck procedures, complex cervical spine trauma, or invasive vascular work near the carotid bifurcation.
- People with known autonomic disorders, especially those that already affect blood pressure regulation.
Medication factors can worsen symptoms without being the root cause. Drugs that lower blood pressure aggressively, cause dehydration, or blunt compensatory heart-rate responses can deepen hypotension. Conversely, stimulants, decongestants, high-dose thyroid hormone, and heavy caffeine intake can amplify hypertensive surges in susceptible individuals.
One practical insight is timing. In radiation-related cases, symptoms may emerge months to years after treatment, so it is easy to miss the connection. If someone develops new episodes of extreme hypertension and tachycardia alternating with orthostatic hypotension—especially with a history of neck radiation—baroreflex failure should move high on the list.
Understanding the cause is not only about labeling. It guides what clinicians screen for (for example, carotid artery disease in radiation survivors), how aggressively they pursue autonomic testing, and how they tailor treatment to avoid making the swings worse.
Symptoms, patterns and serious complications
Baroreflex failure is defined by its pattern: large, rapid blood pressure variability that feels out of proportion to the trigger. Many people have both high-pressure surges and low-pressure episodes, sometimes within the same day.
Typical hypertensive surge symptoms include:
- Sudden pounding headache, facial flushing, and sweating
- Chest tightness or pressure, tremor, and anxiety-like distress
- Palpitations with a fast pulse, often rising in parallel with blood pressure
- Blurred vision or a “pressure” sensation behind the eyes
- Nausea, especially when surges are intense
Common low-pressure and orthostatic symptoms include:
- Lightheadedness or “greying out” on standing
- Weakness, fatigue, and brain fog
- Visual dimming, unsteady gait, and near-fainting
- True syncope, particularly after standing still, hot showers, or large meals
- Worsening symptoms in the morning, after dehydration, or during illness
Triggers can be surprisingly ordinary. Emotional stress, pain, exertion, temperature extremes, and even sudden noises may provoke surges. Orthostatic drops often worsen with dehydration, alcohol, prolonged standing, or medications that dilate blood vessels. Some people also notice post-meal hypotension, especially after carbohydrate-heavy meals.
Complications fall into two main groups: injury risk from drops and organ risk from spikes.
- Falls and trauma: fainting can lead to fractures, head injury, and fear-driven activity restriction.
- Stroke and vascular injury: repeated severe hypertension can raise the risk of hemorrhagic events and accelerate vascular damage, especially in older adults or those with carotid disease.
- Heart strain: surges increase afterload, potentially aggravating heart failure, causing demand ischemia, or provoking arrhythmias in susceptible people.
- Kidney stress: large pressure swings can worsen kidney function over time, particularly if baseline disease exists.
- Quality-of-life burden: unpredictability can lead to hypervigilance, sleep disruption, and social withdrawal. These effects are real and deserve clinical attention rather than dismissal as “just anxiety.”
A key distinction is that baroreflex failure can mimic panic attacks, but it has a physiologic signature: blood pressure rises dramatically and heart rate changes do not show the normal reflex pattern. People may feel anxious because their body is in a sympathetic surge, not the other way around.
Seek urgent evaluation when symptoms suggest end-organ compromise or dangerous hypotension: new neurologic symptoms (weakness, speech changes), chest pressure with shortness of breath, fainting with injury, or sustained very high blood pressure accompanied by headache, confusion, or vision changes. These episodes may require emergency management even if you have a known diagnosis.
How baroreflex failure is diagnosed
Diagnosis begins with pattern recognition and careful exclusion of more common, treatable mimics. Clinicians look for extreme blood pressure lability—often with parallel changes in heart rate—combined with a history that plausibly injures baroreceptor pathways, such as neck radiation or surgery.
A focused history often explores:
- Timing and triggers of surges and drops
- Relationship to posture, meals, hydration, pain, or stress
- Medication list, including over-the-counter decongestants and stimulants
- Prior head and neck cancer treatment, cervical surgery, or carotid procedures
- Symptoms of broader autonomic failure (bowel, bladder, sweating changes)
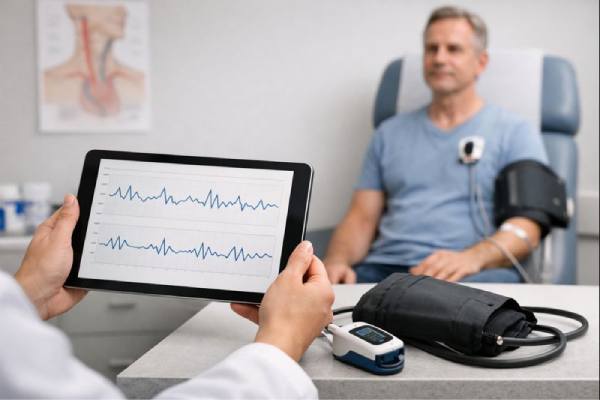
Home and ambulatory data can be more revealing than a single clinic reading. Many patients benefit from:
- A structured home log: seated and standing readings, symptoms, and triggers
- Ambulatory blood pressure monitoring: captures day-night variability and nocturnal hypertension or hypotension patterns
Autonomic testing is often the most definitive tool when available. Common components include:
- Valsalva maneuver: in afferent baroreflex failure, the normal heart-rate response to blood pressure changes is reduced or absent, and blood pressure recovery patterns can be abnormal.
- Deep breathing tests: assess cardiovagal function and heart-rate variability.
- Tilt-table testing: evaluates orthostatic hypotension, heart-rate patterns, and symptom reproduction in a controlled setting.
- Baroreflex sensitivity estimates: quantify how effectively the body adjusts heart rate in response to pressure shifts.
Clinicians also rule out endocrine and tumor causes of episodic hypertension, particularly pheochromocytoma and paraganglioma, which can look similar. Blood or urine catecholamine testing may be used based on the presentation. Other important differentials include:
- Medication-induced lability (short-acting antihypertensives, withdrawal states)
- Panic disorder (usually without extreme measured blood pressure spikes)
- Hyperthyroidism, obstructive sleep apnea, and stimulant use
- Autonomic neuropathies and neurodegenerative autonomic failure syndromes
Imaging is not always required for diagnosis, but it may be clinically important in certain groups. For example, patients with prior neck radiation may need evaluation for carotid artery disease, especially if neurologic symptoms occur. Brain imaging is considered if there are signs of a central lesion.
A practical diagnostic summary is: baroreflex failure is likely when blood pressure shows severe swings, heart rate fails to compensate normally, autonomic testing demonstrates impaired reflex control, and the clinical history supports injury to baroreceptor pathways. Clear diagnosis matters because standard hypertension strategies can backfire, worsening hypotension and increasing fall risk.
Treatments that reduce blood pressure swings
Treatment aims to narrow the swings, not chase a perfect single number. Many patients do best with a two-part plan: blunt sympathetic surges and support blood pressure when it drops—while avoiding therapies that worsen the opposite extreme.
Core principles:
- Prefer steady, longer-acting approaches over short-acting “rescue” cycles.
- Treat triggers and amplifiers: pain, anxiety spirals, dehydration, and poor sleep.
- Accept individualized targets: the safest plan is the one that reduces symptoms and prevents injury.
Medications commonly used to reduce hypertensive surges include:
- Central sympatholytics: longer-acting options can dampen stress-driven surges by reducing sympathetic outflow. Some clinicians use transdermal formulations or longer-acting oral agents to avoid rebound effects.
- Carefully selected beta blockers: may help when tachycardia is prominent, but they can worsen orthostatic symptoms in some patients. They are most useful when chosen thoughtfully and monitored with standing pressures.
- Adjuncts for predictable triggers: for some people, planned dosing before known stressors (travel, procedures, physical therapy) can reduce spikes, but this should be individualized to avoid post-dose hypotension.
Managing hypotension and orthostatic symptoms typically starts with non-drug measures:
- Hydration and salt strategies when medically appropriate
- Compression garments (waist-high is often more effective than knee-high)
- Physical counter-maneuvers: leg crossing, calf pumping, and slow positional changes
- Small, frequent meals and reduced rapid carbohydrate loads to lessen post-meal drops
When non-drug measures are not enough, short-acting pressor support may be used:
- Midodrine: often used for daytime orthostatic symptoms, timed around upright activities. The key is timing and avoiding doses too close to bedtime to limit supine hypertension.
- Fludrocortisone: can expand plasma volume in selected patients, but requires monitoring for swelling, low potassium, and worsening hypertension.
- Other options in specialized settings: some patients with congenital forms may respond to targeted therapies; clinicians tailor choices to the underlying physiology and comorbidities.
Sleep and nighttime management are often overlooked. Many patients experience supine hypertension at night and orthostatic hypotension in the morning. Strategies may include head-of-bed elevation and carefully timed evening medication plans designed by a clinician experienced in autonomic blood pressure disorders.
Because evidence-based data are limited, successful treatment often looks like iterative engineering: adjust one variable, observe standing and supine trends, then refine. The most effective plans are simple enough to follow, specific about timing, and built around the person’s real daily routine.
Day-to-day management and when to seek urgent care
Daily management is where most quality-of-life gains occur. The goal is to reduce surprises and build routines that protect you during predictable high-risk moments: mornings, heat exposure, prolonged standing, emotional stress, and large meals.
A practical home strategy often includes:
- A structured blood pressure routine: check seated and standing readings at consistent times, and also when symptoms appear. Track the trigger, the reading, and what helped.
- Hydration planning: many people do better with scheduled fluids earlier in the day rather than “catch-up” drinking after symptoms begin. During illness, travel, or hot weather, increase fluids proactively if your clinician agrees.
- Posture discipline: stand up in stages—lying to sitting for 30–60 seconds, then standing. If you feel lightheaded, sit back down rather than pushing through.
- Heat and shower modifications: hot showers can provoke vasodilation and drops. Consider warm (not hot) water, a shower chair, and slower transitions afterward.
- Meal design: smaller meals with balanced protein and fiber can reduce post-meal hypotension. If carbohydrate-heavy meals trigger symptoms, reduce portion size and spread intake across the day.
- Exercise choices: recumbent cycling, rowing, and resistance training may be better tolerated than prolonged upright endurance early on. Build slowly and avoid sudden stops after exertion.
Stress is a physiologic trigger in baroreflex failure, so stress-management is not “just lifestyle advice.” Techniques such as paced breathing, structured relaxation training, and cognitive strategies to prevent spiraling can meaningfully reduce the frequency and intensity of surges for some people, especially when paired with steady medication coverage. Pain control also matters; untreated pain can trigger repeated sympathetic surges.
Planning for medications can be the difference between stability and a roller coaster. Many patients benefit from:
- A written dosing schedule that distinguishes baseline medication from rescue medication
- Clear rules for when to hold a dose (for example, if standing systolic pressure is below a clinician-set threshold)
- A plan for travel days, procedures, and infections
Seek urgent care or emergency evaluation if you have:
- Fainting with injury, repeated near-fainting, or inability to stand safely
- New neurologic symptoms such as weakness, facial droop, speech changes, or severe confusion
- Chest pressure with shortness of breath, sweating, or nausea
- Severe headache with very high blood pressure plus vision changes or confusion
- Persistent very low blood pressure with signs of poor perfusion (cold clammy skin, minimal urine output)
Long-term follow-up is important, especially for those with prior neck radiation. Monitoring for carotid artery disease, heart strain, and kidney function may be appropriate based on your history. With consistent tracking and a tailored plan, many people learn to anticipate their patterns, reduce emergency episodes, and return to a fuller, more confident daily life.
References
- Natural History of Afferent Baroreflex Failure in Adults 2021 (Clinical Study)
- Standardized Autonomic Testing in Patients with Probable Radiation-Induced Afferent Baroreflex Failure 2021 (Clinical Study)
- Evaluation and Diagnosis of Afferent Baroreflex Failure 2021 (Clinical Review)
- Blood Pressure Management in Afferent Baroreflex Failure 2019 (Clinical Review)
Disclaimer
This article is for educational purposes and does not replace medical advice, diagnosis, or treatment from a qualified clinician. Baroreflex failure can cause dangerous blood pressure extremes that may lead to fainting, injury, stroke, or cardiac complications. If you experience chest pressure, new neurologic symptoms, repeated fainting, severe headache with confusion or vision changes, or any sudden worsening of symptoms, seek urgent medical care. Treatment choices and medication timing must be individualized based on your medical history, test results, and the balance between hypertension surges and hypotension episodes.
If you found this article helpful, please share it on Facebook, X (formerly Twitter), or any platform you prefer, and follow us on social media. Your support through sharing helps our team continue producing high-quality content.