Carotid artery occlusion means a carotid artery in the neck—most often the internal carotid artery—has become severely narrowed or completely blocked. Because these vessels supply the brain, an occlusion can be silent for years or it can trigger a transient ischemic attack (TIA) or stroke without much warning. The practical challenge is that “occlusion” is not one single situation: a sudden blockage from a clot is managed differently than a long-standing blockage from plaque, and a near-occlusion behaves differently than a complete stop in flow. This article explains what carotid artery occlusion is, why it happens, who is most at risk, what symptoms to take seriously, how clinicians confirm the diagnosis, and what treatment and day-to-day prevention typically involve—so you can understand the decisions that matter.
Table of Contents
- What is carotid artery occlusion?
- What causes it and who is at risk?
- Symptoms, warning signs, complications
- How carotid occlusion is diagnosed
- Treatment options and what to expect
- Management, prevention, and when to seek care
What is carotid artery occlusion?
Your carotid arteries run along both sides of your neck. Each side has a common carotid artery that branches into:
- the internal carotid artery (ICA), which supplies much of the brain, and
- the external carotid artery, which mainly supplies the face and scalp.
A carotid artery occlusion usually refers to a complete blockage of the ICA, though the common carotid can also be involved. Clinically, it helps to think in “degrees of flow” rather than a single label:
- High-grade stenosis: severe narrowing but blood still passes through.
- Near-occlusion: the narrowing is so tight that flow beyond it becomes markedly reduced and the artery past the blockage may look shrunken (“string-like”).
- Complete occlusion: no meaningful forward flow through that segment.
Why this distinction matters: treatments that help severe stenosis do not automatically help complete occlusion. For example, carotid endarterectomy (surgical plaque removal) is commonly used for certain symptomatic stenoses, but it is generally not performed for a fully occluded ICA because there is no open channel to restore, and the procedural risks can outweigh benefits.
Another key concept is timing:
- Acute occlusion (sudden): often due to a clot forming on plaque or traveling from the heart; it can cause sudden neurologic symptoms.
- Chronic occlusion (long-standing): develops gradually, giving the body time to build “detours” (collateral circulation) through other arteries. Some people remain symptom-free because of strong collateral flow.
In practice, clinicians also describe occlusion as symptomatic (TIA/stroke on the same side) or asymptomatic (found incidentally). That symptomatic status strongly shapes urgency, medication choices, and whether any procedure is considered.
What causes it and who is at risk?
Most carotid occlusions develop from atherosclerosis—a build-up of cholesterol-rich plaque within the artery wall. Over time, plaque can narrow the channel, crack or ulcerate, and trigger clot formation. If clot growth outpaces blood flow, the vessel can close off completely.
Common causes include:
- Atherosclerotic plaque with thrombosis: the leading cause, especially in older adults and people with vascular risk factors.
- Embolism (traveling clot): less common as a cause of sustained cervical ICA occlusion, but important in acute stroke settings; clots may originate from atrial fibrillation, recent heart attack, or diseased heart valves.
- Carotid artery dissection: a tear in the artery wall that creates a false channel and can narrow or block flow; more common in younger or middle-aged adults and can follow neck trauma or occur spontaneously.
- Radiation-associated vasculopathy: prior radiation to the neck (for example, head and neck cancers) can accelerate arterial scarring and narrowing.
- Inflammatory conditions (rare): certain vasculitides can affect large vessels, though this is uncommon compared with atherosclerosis.
Risk factors cluster into “plaque-building” risks and “clot-forming” risks. The strongest, most actionable ones include:
- Smoking (current or recent)
- High blood pressure
- High LDL cholesterol
- Diabetes or insulin resistance
- Chronic kidney disease
- Obesity and sedentary lifestyle
- Family history of early cardiovascular disease
- Age and male sex (risk rises with age; sex differences narrow later in life)
There are also context-specific risks:
- Atrial fibrillation increases stroke risk even without carotid disease.
- Sleep apnea can worsen blood pressure control and vascular inflammation.
- Prior TIA or stroke signals a higher baseline risk for future events.
A practical way to think about risk: carotid occlusion is rarely an isolated neck problem. It is often a marker of systemic atherosclerotic disease, meaning the heart and leg arteries may also carry plaque. That is why treatment usually focuses as much on whole-body vascular protection as on the neck artery itself.
Symptoms, warning signs, complications
Carotid artery occlusion may cause no symptoms, especially when collateral vessels compensate. When symptoms occur, they are often sudden and reflect reduced blood flow or emboli reaching the brain or eye.
Common warning signs on the side supplied by the affected carotid include:
- TIA (“mini-stroke”) symptoms that resolve, often within minutes to an hour:
- sudden weakness or numbness of the face, arm, or leg—typically on one side
- trouble speaking or understanding speech
- sudden vision loss in one eye (often described as a curtain coming down)
- sudden imbalance, dizziness, or coordination difficulty (less typical for carotid, more common with posterior circulation issues, but can overlap)
- Stroke symptoms that persist beyond a brief window:
- persistent one-sided weakness, facial droop, severe speech trouble
- new confusion, severe neglect (not noticing one side of the body)
- vision field loss or permanent vision loss in one eye
A classic eye symptom tied to carotid disease is transient monocular blindness (amaurosis fugax). It suggests reduced flow or small emboli to the retina and should be treated as a medical emergency signal.
Complications can be immediate or delayed:
- Ischemic stroke: the most important complication, ranging from mild to disabling.
- Recurrent TIAs: particularly if unstable plaque or poor collateral flow exists.
- Cognitive and fatigue effects: some people with chronic, low-flow states report slower thinking or reduced stamina; this is complex and not always directly attributable, but it is clinically discussed, especially when perfusion studies show compromised reserve.
- “Watershed” infarcts: strokes that occur in border-zone areas between major brain artery territories, sometimes linked to low-flow conditions.
- Ocular ischemic syndrome (rare): chronic reduced blood flow to the eye can cause eye pain, blurred vision, and retinal changes.
A key nuance: headache or neck pain alone is not typical for carotid occlusion from plaque, but it can occur with carotid dissection, often alongside neurologic symptoms or a drooping eyelid/pupil changes (Horner syndrome). That pattern deserves urgent evaluation.
If someone has sudden neurologic symptoms—even if they improve—time matters. Many stroke treatments are strongly time-dependent, and early evaluation also reduces the risk of a second event in the following days.
How carotid occlusion is diagnosed
Diagnosis has two goals: confirm whether the artery is truly occluded (and where), and understand the brain’s risk (embolus risk, perfusion status, and alternative causes).
Clinicians usually start with history and exam—focusing on:
- timing and nature of symptoms (sudden vs gradual, resolved vs persistent)
- vascular risk factors (smoking, blood pressure, diabetes)
- heart rhythm history (atrial fibrillation)
- medication history (antiplatelets, anticoagulants, statins)
Common tests include:
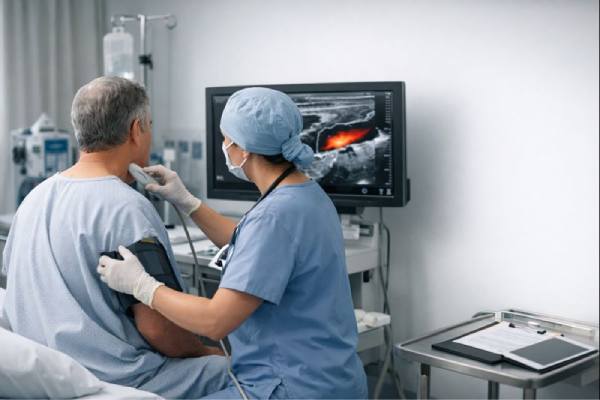
- Carotid duplex ultrasound
- Often the first-line test.
- Noninvasive, quick, and can estimate flow speed and detect no-flow patterns.
- Limitations: heavy calcification or a very high bifurcation can reduce accuracy; near-occlusion can be challenging to classify.
- CT angiography (CTA)
- Provides a detailed map from the aortic arch through the neck to intracranial vessels.
- Helpful to distinguish near-occlusion vs complete occlusion, identify plaque ulceration, and evaluate collateral flow.
- Often used in emergency stroke workups.
- MR angiography (MRA)
- Useful alternative when CTA is not ideal (for example, contrast concerns), depending on local protocols.
- Can also evaluate brain tissue for small strokes.
- Brain imaging (CT or MRI)
- Looks for signs of stroke, its pattern (embolic vs watershed), and whether bleeding is present.
- MRI with diffusion-weighted imaging is particularly sensitive for early ischemia.
- Perfusion imaging (selected cases)
- CT perfusion, MR perfusion, or other studies may assess how well the brain compensates.
- This can matter when symptoms suggest low-flow problems or when specialized centers consider advanced interventions.
- Cardiac evaluation
- ECG and often longer rhythm monitoring to detect atrial fibrillation.
- Echocardiogram if a cardiac embolus source is suspected.
A frequent diagnostic pitfall is mislabeling severe stenosis as occlusion (or vice versa). That matters because management changes substantially. When imaging is unclear, clinicians may repeat imaging, use a second modality, or refer to vascular specialists for interpretation—especially if treatment decisions depend on it.
Treatment options and what to expect
Treatment depends on three main factors: acute vs chronic, symptomatic vs asymptomatic, and complete occlusion vs near-occlusion/high-grade stenosis. The safest approach is individualized care led by a stroke team and/or vascular specialists.
Emergency treatment (suspected acute stroke)
If symptoms suggest stroke, emergency care focuses on restoring brain blood flow and preventing expansion of injury. Depending on eligibility and timing, options may include:
- IV thrombolysis (“clot-busting” medicine) in a narrow time window for certain ischemic strokes.
- Mechanical thrombectomy (catheter-based clot retrieval) for selected large-vessel occlusions, often guided by imaging and time since symptom onset.
- Supportive stroke-unit care: oxygen if needed, careful blood pressure strategy, glucose control, fever control, and swallowing evaluation to reduce aspiration risk.
Acute cervical ICA occlusion can be complex: sometimes the critical blockage is inside the skull, sometimes in the neck, and sometimes both. Treatment decisions often depend on detailed CTA and perfusion imaging.
Treatment for chronic carotid artery occlusion
For a chronic, complete ICA occlusion, the backbone of care is usually aggressive medical therapy:
- Antiplatelet therapy (commonly aspirin or another antiplatelet agent), unless anticoagulation is indicated for a different reason.
- High-intensity statin therapy (or equivalent LDL-lowering strategy), aiming for substantial LDL reduction.
- Blood pressure management, often with targets around the low 130s/80s or below depending on individual risk and clinician guidance.
- Diabetes management when applicable, with a focus on safe, sustained control.
- Smoking cessation and lifestyle interventions (diet, exercise, weight, sleep).
Procedures may be considered in selected symptomatic patients at experienced centers, but they are not routine for everyone:
- Endovascular recanalization (attempting to reopen the chronically occluded artery with wires, balloons, and stents) can be technically challenging and carries stroke and vessel-injury risks.
- Hybrid approaches (combining surgical and endovascular techniques) may be used in some anatomic patterns.
- EC–IC bypass surgery (connecting an external scalp artery to an internal brain artery) has been studied for symptomatic occlusion with impaired blood flow reserve; results across studies have been mixed, and candidacy is narrow.
The most realistic expectation for many patients is not “reopening the artery,” but lowering future stroke risk and stabilizing plaque disease elsewhere. When symptoms recur despite strong medical therapy, a specialist may reassess anatomy, collateral circulation, and alternative causes (such as atrial fibrillation or intracranial stenosis) before discussing any advanced options.
Management, prevention, and when to seek care
Living with carotid artery occlusion is largely about preventing the next vascular event. The most effective plan is consistent, measurable, and reviewed regularly with your clinician.
A practical prevention checklist
Medication adherence (daily, long-term):
- Take antiplatelet or anticoagulant medication exactly as prescribed.
- Continue LDL-lowering therapy (often a statin; sometimes combined with other agents).
- Treat blood pressure reliably—missed doses are a common reason for “mysterious” spikes.
Targets to discuss with your clinician (individualized):
- Blood pressure goals (often near or below 130/80, depending on tolerance and stroke profile).
- LDL goals (many high-risk patients aim for very low LDL levels using high-intensity therapy).
- Diabetes goals (often an A1c near 7% for many adults, adjusted for age, comorbidities, and hypoglycemia risk).
Lifestyle actions with the best evidence:
- Stop smoking completely. If needed, use a structured plan (counseling plus medication support).
- Exercise most days: aim for about 150 minutes/week of moderate aerobic activity plus strength work 2 days/week, adjusted for ability and medical guidance.
- Diet pattern: prioritize vegetables, legumes, whole grains, fish, nuts, and unsaturated oils; reduce ultra-processed foods, trans fats, and excess sodium.
- Sleep and stress: treat sleep apnea if present; build routines that support consistent sleep.
Monitoring and follow-up
Even with a stable occlusion, follow-up matters because risk is systemic:
- Review blood pressure logs and lipid panels.
- Reassess symptoms and medication side effects.
- Evaluate for atrial fibrillation if symptoms or history suggest it.
- Repeat imaging may be done in selected cases, especially if symptoms change.
When to seek urgent or emergency care
Call emergency services immediately for any sudden neurologic symptom, even if it lasts only a few minutes:
- face droop, arm weakness, speech trouble
- sudden loss of vision in one eye
- sudden severe imbalance or inability to walk
- sudden confusion or inability to understand speech
Also seek urgent evaluation for:
- new, unusual one-sided headache or neck pain with neurologic symptoms (possible dissection)
- recurrent TIAs, especially clustered over days (“crescendo TIAs”)
The single most important habit is treating every possible TIA as a true warning shot. Rapid evaluation can prevent a larger stroke, and early changes in therapy often have the biggest payoff in the first days and weeks.
References
- Editor’s Choice – European Society for Vascular Surgery (ESVS) 2023 Clinical Practice Guidelines on the Management of Atherosclerotic Carotid and Vertebral Artery Disease 2023 (Guideline)
- Society for Vascular Surgery clinical practice guidelines for management of extracranial cerebrovascular disease 2022 (Guideline)
- 2021 Guideline for the Prevention of Stroke in Patients With Stroke and Transient Ischemic Attack: A Guideline From the American Heart Association/American Stroke Association 2021 (Guideline)
- Extracranial-Intracranial Bypass and Risk of Stroke and Death in Patients With Symptomatic Artery Occlusion: The CMOSS Randomized Clinical Trial 2023 (RCT)
- Comparison of the treatment strategies for symptomatic chronic internal carotid artery occlusion 2025 (Systematic Review, Meta-Analysis)
Disclaimer
This article is for educational purposes only and does not provide medical advice, diagnosis, or treatment. Carotid artery occlusion and stroke symptoms can be medical emergencies, and care must be individualized based on imaging, timing, medical history, and medications. If you have sudden weakness, facial droop, speech trouble, or sudden vision loss, seek emergency care immediately. Always consult a qualified clinician for personal guidance, especially before starting or stopping antiplatelet drugs, anticoagulants, blood pressure medicines, or cholesterol-lowering therapy.
If you found this helpful, please consider sharing it on Facebook, X (formerly Twitter), or any platform you prefer—and follow us on social media. Your support through sharing helps our team keep producing clear, high-quality health content.






