Carotid artery stenosis is narrowing of the carotid arteries in the neck—most often the internal carotid artery—caused by plaque buildup. Many people feel completely well until a warning sign appears, because the narrowing can progress quietly for years. The main danger is not simply “less blood getting through,” but plaque becoming unstable and releasing tiny clots that travel to the brain or eye, leading to a transient ischemic attack (TIA) or stroke. The encouraging part is that the risk can be reduced substantially with modern medical therapy, and procedures can add benefit for carefully selected patients. In the sections below, you will learn how carotid stenosis affects the body, which risk factors matter most, what symptoms require urgent care, how the diagnosis is confirmed, and what treatment and long-term management typically involve.
Table of Contents
- What it is and how it affects blood flow
- Causes and risk factors that drive narrowing
- Symptoms and complications to take seriously
- How carotid stenosis is diagnosed
- Treatment options and what to expect
- Management, prevention, and when to seek care
What it is and how it affects blood flow
Carotid artery stenosis means the inner channel of a carotid artery has narrowed, usually because of atherosclerotic plaque (a mix of cholesterol, inflammatory cells, fibrous tissue, and often calcium). The carotid arteries supply much of the brain’s oxygenated blood, so stenosis is closely linked to stroke risk.
Two mechanisms explain why carotid stenosis matters:
- Embolic risk (most common): As plaque grows, its surface can become irregular or ulcerated. Platelets can stick to that surface, forming clots that break off and travel to the brain or retina. This is why a person can have only moderate narrowing yet still have a TIA if the plaque is unstable.
- Low-flow risk (less common but important): If stenosis is very severe, overall blood delivery can drop, especially when blood pressure falls or if other brain arteries are also narrowed. This can contribute to “border-zone” (watershed) strokes.
Clinicians often describe stenosis by both degree and symptom status:
- Degree of stenosis: commonly grouped as mild, moderate, or severe (often framed around ranges such as 50% to 69% and 70% to 99%), with special attention to near-occlusion, where flow beyond the narrowing becomes markedly reduced and the downstream artery may look narrowed.
- Asymptomatic vs symptomatic: “Symptomatic” typically means a recent neurologic event attributable to that carotid artery, such as a TIA, minor stroke, or temporary vision loss in one eye on that side. Symptom status often drives urgency and whether a procedure is likely to help.
A useful “whole-body” perspective: carotid stenosis is rarely a stand-alone issue. It often signals atherosclerosis elsewhere—heart arteries, leg arteries, kidney arteries—so treating carotid disease well usually means treating cardiovascular risk broadly.
Finally, remember that the stenosis number is not a perfect predictor by itself. Clinicians also consider plaque appearance, ulceration, clot tendency, and how stable symptoms have been. The goal is not just to label a percentage, but to prevent a future stroke with the lowest overall risk.
Causes and risk factors that drive narrowing
Most carotid stenosis develops from atherosclerosis over many years. Plaque forms when LDL cholesterol particles penetrate the artery lining, triggering inflammation and scarring. Over time, the plaque enlarges and the artery may remodel. In some people it stays stable; in others it becomes “active” and more likely to shed debris.
Common causes
- Atherosclerosis (most common): driven by cholesterol burden, blood pressure stress, and inflammation.
- Radiation-associated vasculopathy: prior radiation to the head and neck can accelerate scarring and narrowing years later.
- Fibromuscular dysplasia (less common): a non-atherosclerotic vessel disorder that can affect the carotids, typically in younger patients than classic plaque disease.
- Carotid dissection (different process): a tear within the artery wall that narrows flow; it can mimic stenosis but is managed differently and often presents with neck pain or headache.
- Recurrent narrowing after a procedure: restenosis can occur after surgery or stenting, often detected during surveillance ultrasound.
Major risk factors
The most important modifiable risk factors are the familiar drivers of vascular disease:
- Smoking: promotes vessel injury, inflammation, and clotting tendency. Quitting meaningfully lowers risk even after years of smoking.
- High blood pressure: accelerates plaque formation and makes plaque more likely to rupture.
- High LDL cholesterol: higher lifetime exposure increases plaque burden; lowering LDL stabilizes plaque and reduces events.
- Diabetes and insulin resistance: worsen inflammation and impair vessel lining function.
- Chronic kidney disease: associated with faster vascular aging and higher event rates.
- Sedentary lifestyle and obesity: increase metabolic stress, blood pressure, and inflammation.
Nonmodifiable or less modifiable contributors include:
- Age: risk rises steadily with age.
- Sex: men develop atherosclerosis earlier on average; women’s risk rises later in life.
- Family history: early heart disease or stroke in close relatives suggests higher baseline risk.
Why some plaques cause symptoms
Two people can have a similar stenosis percentage and different stroke risk. Factors that tend to increase “plaque danger” include:
- Irregular or ulcerated plaque surface
- Intraplaque bleeding or a softer, lipid-rich core (seen on some imaging)
- Active smoking or uncontrolled blood pressure
- A prior TIA or stroke (the strongest practical warning sign)
A helpful way to frame prevention is to separate “plaque-building” from “plaque-stabilizing.” You cannot change past exposure, but you can reduce future risk by lowering LDL, controlling blood pressure, avoiding tobacco, and improving metabolic health. Those changes do not just slow narrowing; they make the plaque less likely to cause a sudden embolic event.
Symptoms and complications to take seriously
Many people with carotid stenosis have no symptoms. When symptoms appear, they are often sudden and focal—meaning they affect a specific function such as speech, vision, or movement—because a small clot has reached the brain or retina.
Symptoms that suggest TIA or stroke
Watch for sudden onset of any of the following:
- Weakness or numbness of the face, arm, or leg, typically on one side
- Speech trouble (slurring, word-finding difficulty) or trouble understanding speech
- Sudden confusion or inability to follow conversation
- Vision loss in one eye (often described as a curtain or shade coming down)
- Vision field loss (missing part of what you see)
- Sudden severe imbalance or coordination problems
A TIA is often defined by symptoms that resolve fully within minutes to hours. Even if you feel normal afterward, a TIA can be a high-risk warning that a larger stroke may follow soon.
Symptoms that are less specific
Dizziness, lightheadedness, headaches, or “brain fog” can happen for many reasons and are not classic, specific signs of carotid stenosis. They should be evaluated in context, but the most urgent carotid-related symptoms are typically sudden, focal neurologic deficits or temporary one-eye vision loss.
Complications clinicians focus on preventing
- Ischemic stroke: the most important complication, with severity ranging from mild symptoms to major disability.
- Recurrent TIAs: repeated episodes can signal unstable plaque and a need to intensify therapy quickly.
- Progression to near-occlusion or occlusion: narrowing can worsen over time, especially if risk factors remain uncontrolled.
- Cardiovascular events elsewhere: carotid stenosis often coexists with coronary artery disease and peripheral artery disease, so the overall cardiovascular risk profile matters.
Why “symptomatic” changes the urgency
If you have had a TIA or stroke attributable to the stenosed carotid artery, you are generally considered at higher near-term risk. In that setting, clinicians often:
- Intensify medical therapy immediately (antiplatelet strategy, high-intensity lipid lowering, risk-factor control)
- Evaluate quickly for whether a procedure could reduce the chance of recurrence
- Consider timing carefully, because benefits of certain procedures can be greatest when performed soon after a qualifying event in appropriate candidates
The most actionable message is simple: sudden neurologic symptoms are never “wait and see.” If symptoms resolve, treat that as a warning, not reassurance. Early evaluation can prevent the next event, and the window to reduce risk can be tight in the days after a TIA or minor stroke.
How carotid stenosis is diagnosed
Diagnosis aims to confirm the presence and severity of narrowing, determine whether it explains symptoms, and map anatomy well enough to guide treatment.
Clinical evaluation
Clinicians start with a careful history and focused neurologic exam. They look for:
- A clear timeline of symptoms (onset, duration, resolution)
- Whether symptoms fit a carotid territory (especially one-eye vision loss or one-sided weakness/speech difficulty)
- Vascular risk factors and current medications
- Competing stroke causes such as atrial fibrillation or small-vessel disease
A carotid bruit can be a clue, but it is not definitive. Some severe stenoses have no bruit, and some bruits occur with moderate stenosis or even normal arteries.
Key imaging tests
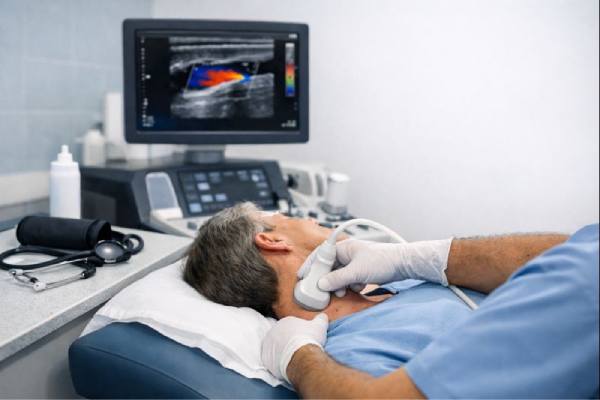
- Carotid duplex ultrasound: commonly the first test. It estimates stenosis using blood-flow velocities and visualizes plaque. It is also widely used for follow-up surveillance.
- CT angiography (CTA): provides a detailed view of the carotid lumen, plaque calcification, and vessel anatomy from the chest to the head. CTA is often used when planning a procedure or evaluating urgent symptoms.
- MR angiography (MRA): an alternative to CTA in many settings, often paired with brain MRI to evaluate recent ischemia.
- Catheter angiography (selected cases): used when noninvasive imaging is unclear or when an endovascular procedure is planned and high-detail mapping is needed.
How stenosis is measured and reported
Stenosis is frequently reported as a percentage. Practical interpretation involves:
- Consistency: the same imaging method over time reduces measurement noise.
- Context: stenosis severity is interpreted alongside symptoms, plaque features, and overall risk.
- Special category: near-occlusion can be under-recognized but matters because it may behave differently from “standard” severe stenosis.
Tests often paired with carotid workups
If a TIA or stroke occurred, clinicians usually also evaluate:
- Brain imaging (CT or MRI): to confirm stroke, define the pattern, and guide urgency.
- Heart rhythm monitoring: to detect atrial fibrillation, which can cause embolic stroke independent of carotid disease.
- Echocardiography (when indicated): to look for structural heart sources of clots.
- Intracranial vessel assessment: because narrowing inside the skull can coexist with neck carotid disease.
A high-quality diagnostic process ends with clear answers: which side is involved, how severe the narrowing is, whether symptoms are attributable, and whether anatomy is suitable for surgery or stenting if needed. That clarity prevents both undertreatment (missed high-risk disease) and overtreatment (procedures unlikely to help).
Treatment options and what to expect
Treatment for carotid stenosis is designed to reduce stroke risk. Most patients benefit from optimized medical therapy, and some—especially those with significant symptomatic stenosis—may benefit from a procedure.
Best medical therapy
Medical therapy aims to stabilize plaque and reduce clot formation. Plans vary by individual risk, but commonly include:
- Antiplatelet therapy: aspirin is commonly used; in some situations after TIA/minor stroke, clinicians may prescribe short-term dual antiplatelet therapy. Typical aspirin doses used in practice range from 81 mg to 325 mg daily, selected based on bleeding risk and clinician preference.
- High-intensity lipid lowering: lowering LDL reduces vascular events and stabilizes plaque. Common high-intensity statin regimens include atorvastatin 40–80 mg or rosuvastatin 20–40 mg daily, adjusted for tolerance and interactions. Some people require additional LDL-lowering agents.
- Blood pressure control: steady control reduces stroke risk and plaque stress. Targets are individualized, but many prevention strategies aim near 130/80 mmHg when tolerated.
- Diabetes management and kidney protection: improving metabolic control lowers long-term vascular risk.
- Smoking cessation and lifestyle therapy: stopping tobacco, regular exercise, and a Mediterranean-style diet can meaningfully reduce events.
Procedures that restore flow and reduce embolic risk
Procedures are not “one size fits all.” They are most often considered when:
- Stenosis is significant and the patient is symptomatic, or
- Stenosis is very high-grade and the patient has a favorable risk profile for intervention.
Common procedures include:
- Carotid endarterectomy (CEA): open surgery that removes plaque from the artery. It has decades of outcomes data and is often preferred for many symptomatic patients when surgical risk is low and anatomy is favorable.
- Carotid artery stenting (CAS): a catheter-based procedure that places a stent, usually with embolic protection devices. It can be useful when surgical access is difficult or when specific medical or anatomic factors make surgery higher risk.
- Transcarotid artery revascularization (TCAR): a hybrid approach used in some centers that employs flow reversal during stent placement to reduce emboli.
What risks and recovery look like
All procedures aim to reduce future stroke risk, but they carry peri-procedural risks, including stroke, bleeding, heart complications, and—after surgery—temporary or rarely persistent cranial nerve effects (hoarseness, tongue weakness, swallowing changes). After stenting, ongoing antiplatelet therapy is especially important to prevent stent clotting.
Recovery planning usually includes:
- Short-term neurologic monitoring and blood pressure management
- Clear medication strategy (antiplatelets, statins)
- Follow-up ultrasound surveillance to detect restenosis
- Reinforcement that procedures complement, not replace, medical therapy
A practical expectation: for most people, the largest long-term benefit comes from sustained risk-factor control plus the right procedure only when the likelihood of benefit clearly outweighs risk.
Management, prevention, and when to seek care
Managing carotid artery stenosis is a long game. The goal is to prevent stroke while also lowering overall cardiovascular risk. The most effective plans are specific, measurable, and revisited regularly.
Day-to-day management that actually works
Focus on a small set of repeatable actions:
- Take medications consistently. If side effects occur (muscle symptoms, cough, dizziness), report them early. Adjustments are often possible without losing protection.
- Track blood pressure at home. Use a validated cuff, measure at consistent times, and bring averages—not single readings—to appointments.
- Follow lipid results over time. LDL lowering is one of the strongest tools for plaque stabilization, but it must be measured to confirm it is working.
- Build activity into the week. Many prevention programs aim for about 150 minutes per week of moderate aerobic activity, plus strength work twice weekly, adapted to safety and ability.
- Choose a vascular-friendly eating pattern. Emphasize vegetables, legumes, whole grains, fish, unsalted nuts, and unsaturated oils; limit ultra-processed foods, sugary drinks, and excess sodium.
- Stop smoking completely. If needed, combine counseling with medication support, which improves success rates.
Follow-up and surveillance
Clinicians often use duplex ultrasound to monitor:
- Progression of stenosis in medically managed patients
- Restenosis after surgery or stenting
- Plaque changes if symptoms evolve
Follow-up frequency depends on stenosis severity, stability, and whether an intervention was performed. If you have a new neurologic event, reassessment should be prompt regardless of the next scheduled scan.
Common “decision points” to anticipate
Over time, management may shift based on:
- New symptoms (TIA, stroke, temporary one-eye vision loss)
- Rapid progression of narrowing on surveillance imaging
- Worsening risk-factor control (blood pressure, LDL, diabetes)
- Changes in overall health that alter procedural risk
When to seek urgent or emergency care
Seek emergency care immediately for any sudden neurologic symptom, even if it resolves:
- face droop, arm weakness, or speech trouble
- sudden vision loss in one eye
- sudden confusion or inability to speak normally
- sudden severe imbalance with other neurologic symptoms
Contact your clinician promptly for:
- New episodes of transient neurologic symptoms
- Medication intolerance that leads you to stop therapy
- New bleeding concerns if on antiplatelets or anticoagulants
Carotid stenosis is often manageable, but it demands seriousness about prevention. The best outcomes come from treating the artery disease as a clear signal to protect the brain and the heart—consistently, not occasionally.
References
- Editor’s Choice – European Society for Vascular Surgery (ESVS) 2023 Clinical Practice Guidelines on the Management of Atherosclerotic Carotid and Vertebral Artery Disease 2023 (Guideline)
- Society for Vascular Surgery clinical practice guidelines for management of extracranial cerebrovascular disease 2022 (Guideline)
- 2021 Guideline for the Prevention of Stroke in Patients With Stroke and Transient Ischemic Attack: A Guideline From the American Heart Association/American Stroke Association 2021 (Guideline)
- Second asymptomatic carotid surgery trial (ACST-2): a randomised comparison of carotid artery stenting versus carotid endarterectomy 2021 (RCT)
- Screening for asymptomatic carotid artery stenosis in the general population: updated evidence report and systematic review for the US Preventive Services Task Force 2021 (Systematic Review)
Disclaimer
This article is for educational purposes only and does not provide medical advice, diagnosis, or treatment. Carotid artery stenosis can increase the risk of TIA and stroke and may require time-sensitive evaluation and treatment based on imaging, symptoms, and overall health. If you develop sudden weakness, facial droop, speech trouble, or sudden vision loss—even if it resolves—seek emergency care immediately. Do not start, stop, or change antiplatelet drugs, anticoagulants, blood pressure medicines, or cholesterol-lowering therapy without guidance from a qualified clinician.
If you found this article helpful, please share it on Facebook, X (formerly Twitter), or any platform you prefer, and follow us on social media. Your support through sharing helps our team continue producing clear, reliable health content.






