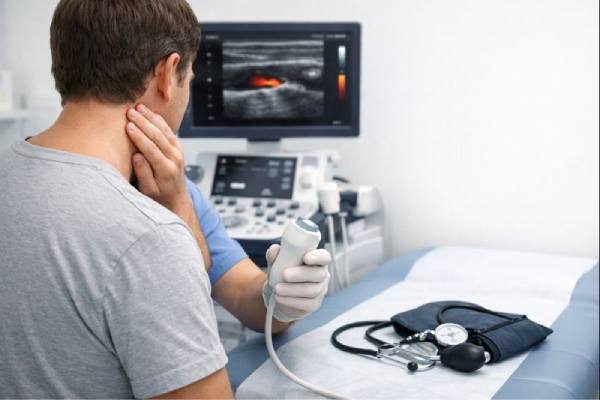
Carotidynia is a clinical pattern—usually one-sided pain and tenderness along the front side of the neck—centered over the carotid artery, the main blood vessel that supplies the brain. In recent years, many clinicians use a more specific name for a common modern explanation of this symptom pattern: TIPIC syndrome (transient perivascular inflammation of the carotid artery). In TIPIC, the tissues around the carotid artery briefly become inflamed, creating localized pain that can feel alarming because of where it sits and what the carotid artery represents.
The reassuring news is that carotidynia/TIPIC is often self-limited and responds well to anti-inflammatory treatment. The important caveat is that neck pain in this location can also signal urgent conditions, so the goal is to recognize the typical features, rule out dangerous look-alikes, and recover with a clear plan.
Table of Contents
- What is carotidynia?
- What causes it and who is at risk?
- Symptoms, red flags, and complications
- How it’s diagnosed
- Treatment and what recovery looks like
- Management, prevention, and when to seek care
What is carotidynia?
Carotidynia describes pain and tenderness over the carotid artery, typically near where the artery divides in the neck (the carotid bifurcation). People often notice a small, very specific “hot spot” that hurts when pressed, when turning the head, or sometimes when swallowing. The pain can radiate upward toward the jaw, ear, or temple, which is why some people first assume it is dental pain, a throat infection, or a migraine variant.
Today, carotidynia is commonly discussed alongside TIPIC syndrome (transient perivascular inflammation of the carotid artery). TIPIC is considered a clinico-radiologic entity—meaning the diagnosis relies on both the clinical pattern (focal neck pain over the carotid) and imaging that shows a short segment of inflammation around the artery. Instead of a blockage inside the vessel, the problem is usually inflammation in the tissues surrounding the artery wall, often appearing as a localized thickening or “cuff” around part of the carotid.
A helpful way to think about it: the carotid artery is a large pipe, but it is also wrapped in living tissue with nerves and immune cells. When that outer region becomes inflamed, the artery itself may still carry blood normally, yet the area can become surprisingly painful because of how sensitive the neck’s structures are.
Carotidynia/TIPIC is generally considered benign in the sense that it does not typically cause stroke by itself. Episodes often improve over days to a couple of weeks, especially with anti-inflammatory medication. However, the location and symptom overlap with serious vascular problems means the first priority is always to confirm that you are not dealing with carotid artery dissection, vasculitis, clot, infection, or another dangerous condition.
What causes it and who is at risk?
The exact cause of carotidynia—especially TIPIC syndrome—is still being clarified. Most evidence points to a transient inflammatory process affecting the carotid artery’s outer layers and the tissue immediately around it. What triggers that inflammation may differ from person to person, which helps explain why some cases appear “out of the blue,” while others follow a recognizable stressor.
Potential contributors and associations include:
- Recent viral or upper-respiratory illness: Some people report symptoms after a cold-like infection, suggesting immune activation may play a role.
- Local mechanical strain: Prolonged neck posture (long drives, desk work), sudden head turning, or minor neck strain may sensitize the area, though this is not proven as a direct cause.
- Underlying inflammatory tendency: A subset of patients appears to have coexisting autoimmune or inflammatory conditions. This does not mean carotidynia is an autoimmune disease, but it may reflect a more reactive immune environment.
- Atherosclerosis nearby: Some imaging descriptions note carotid plaque in or near the affected segment. Whether plaque is a trigger or simply a common incidental finding (especially with aging) is not always clear.
- Medication or systemic triggers (rare): Case reports describe TIPIC-like presentations in the context of certain systemic illnesses or treatments, but these are uncommon.
Risk factors are best understood as “who shows up with it,” rather than guaranteed predictors. Carotidynia/TIPIC is considered uncommon, and it can occur in adults across a wide age range. In published series, many patients are middle-aged, and women may be represented somewhat more often than men, but it can affect anyone.
It is also important to separate carotidynia from other causes of carotid-area pain that have clearer risk profiles:
- Carotid artery dissection is more likely after neck trauma (even minor), connective tissue disorders, or sudden severe neck pain with neurologic symptoms.
- Giant cell arteritis is primarily a disease of older adults and often comes with headache, jaw pain with chewing, vision changes, and elevated inflammatory markers.
- Infection (deep neck space infections, lymphadenitis) tends to produce fever, progressive swelling, and systemic illness.
Because the “risk factor” that matters most is missing a dangerous diagnosis, the practical approach is to treat carotidynia/TIPIC as a diagnosis made after careful exclusion of urgent conditions—especially at the first episode.
Symptoms, red flags, and complications
The hallmark symptom is focal pain and tenderness over one carotid artery, usually on the front side of the neck. Many people can point to a specific spot that feels bruised or sharply tender. The pain may be constant, throbbing, or aching, and it can worsen with:
- Turning the head or extending the neck
- Swallowing or yawning
- Pressing on the tender area
- Physical exertion (sometimes)
Pain can radiate to nearby regions, including the jaw angle, ear, or temple. Some people describe a sense of “fullness” or mild swelling in the area, though obvious swelling is not always present.
What carotidynia/TIPIC typically does not cause is just as important:
- It usually does not cause persistent neurologic deficits (weakness, numbness, difficulty speaking).
- It usually does not cause a sustained high fever.
- It usually does not cause a progressive enlarging neck mass.
Commonly reported time course:
- Symptoms often peak over 1–3 days, then gradually improve.
- Many episodes resolve within about 1–2 weeks, though longer courses can occur.
- Recurrence is possible, sometimes months later.
Red flags that need urgent evaluation
Seek urgent care (emergency services if needed) if neck pain over the carotid area occurs with any of the following:
- Sudden or “worst-ever” neck pain or headache
- Weakness, numbness, facial droop, slurred speech, confusion, trouble walking
- New vision loss, double vision, or a curtain-like visual change
- Fainting, severe dizziness, or new trouble coordinating movements
- Fever with rapidly worsening neck swelling, redness, or difficulty breathing/swallowing
- A new pulsating neck mass, or a bruit (whooshing sound) noted by a clinician
- Recent neck trauma or chiropractic manipulation followed by symptoms
Complications
Carotidynia/TIPIC itself is generally considered self-limited. The “complication” clinicians worry about is misattribution—assuming carotidynia when the true diagnosis is carotid dissection, vasculitis, thrombosis, infection, or another condition that needs immediate treatment. That is why imaging and a structured evaluation matter, especially with a first presentation.
How it’s diagnosed
Diagnosis starts with a careful history and exam focused on two goals: (1) confirm the pattern fits carotid-area focal pain, and (2) look for signs that point to a more dangerous cause.
A clinician will usually ask:
- Where exactly is the pain, and can you point to it with one finger?
- Did symptoms start suddenly or gradually?
- Any recent infection, dental work, neck strain, or trauma?
- Any neurologic symptoms (even brief ones)?
- Any systemic symptoms (fever, weight loss, night sweats)?
- Any history of migraine, autoimmune disease, clotting disorders, or vascular disease?
On exam, the key finding is localized tenderness over the carotid artery without more widespread throat or muscle tenderness. Clinicians also check blood pressure, neurologic status, and signs of infection or inflammation elsewhere.
Imaging: the cornerstone for TIPIC
Because carotidynia/TIPIC sits at the intersection of benign inflammation and potentially high-risk vascular disease, imaging is often used early—especially for a first episode.
Common imaging tools include:
- Carotid ultrasound (Doppler): Often the first test because it is quick and noninvasive. In TIPIC, ultrasound may show localized wall or perivascular thickening with preserved blood flow, and it can help exclude major narrowing or clot.
- CT angiography (CTA) or MR angiography (MRA): These are used when clinicians need a clearer vascular map or when there are red flags for dissection, aneurysm, or significant stenosis.
- MRI with vessel wall or soft tissue sequences: MRI can be particularly helpful in showing perivascular inflammation and confirming the “around the vessel” nature of the finding.
Lab tests: supportive, not definitive
Blood tests vary based on the clinical picture. They may include inflammatory markers (such as ESR/CRP), a complete blood count, and other targeted tests if vasculitis, infection, or systemic disease is suspected. In TIPIC, labs may be normal or mildly abnormal—so normal results do not automatically rule it in or out.
Differential diagnosis: what must be ruled out
Clinicians typically consider:
- Carotid artery dissection
- Giant cell arteritis or other vasculitis
- Thrombosis or significant atherosclerotic disease
- Deep neck infection, lymphadenitis, or thyroiditis
- Tumors or masses in the neck
- Musculoskeletal pain (sternocleidomastoid strain, cervical facet pain)
In practice, a TIPIC diagnosis becomes most confident when imaging shows the characteristic localized perivascular inflammation and other high-risk explanations have been excluded.
Treatment and what recovery looks like
Treatment for carotidynia/TIPIC is usually symptom-focused because the inflammation tends to resolve. The plan often balances comfort, safety, and follow-up to confirm improvement.
First-line treatment
Most clinicians start with:
- NSAIDs (nonsteroidal anti-inflammatory drugs): These reduce pain and inflammation and are often effective within several days. They are commonly used for 5–14 days depending on symptom severity and medical history.
- Acetaminophen/paracetamol: Can be used if NSAIDs are not appropriate, or as an add-on for pain control.
If pain is severe or persistent, some clinicians consider:
- A short course of corticosteroids: This may be used when symptoms are not responding to NSAIDs, or when imaging shows prominent inflammation. Steroids can reduce inflammation quickly, but they are not used casually because they have meaningful side effects and can complicate infection evaluation.
Supportive strategies
These are not “cures,” but they can make recovery smoother:
- Gentle neck range-of-motion (avoid aggressive stretching during peak pain)
- Heat or cold packs for 10–15 minutes, 2–3 times daily, based on preference
- Sleep positioning that avoids neck twisting
- Temporary reduction of intense exercise if it clearly worsens pain
What recovery often looks like
A typical trajectory is:
- Pain is focal and bothersome for several days.
- After anti-inflammatory therapy, pain often improves steadily.
- Symptoms commonly resolve within about 1–2 weeks, though some people report longer recovery or residual tenderness.
Some people experience recurrence months later. If recurrence happens, clinicians often reassess to confirm the pattern remains consistent and that no new risk factors or red flags have emerged.
Follow-up and repeat imaging
Follow-up is important for two reasons:
- To confirm symptoms are improving as expected
- To document that imaging abnormalities (when present) are resolving
Some clinicians repeat ultrasound or other imaging within weeks to months, especially if symptoms were prolonged, imaging findings were pronounced, or recurrence occurs. If your symptoms do not improve within the expected window—or they worsen—re-evaluation is essential.
Treatments to avoid without guidance
Because carotid-area pain can represent serious vascular disease, it is wise to avoid:
- Neck manipulation or forceful massage over the tender area
- Self-starting steroids without medical assessment
- Ignoring new neurologic symptoms because “it’s probably the same thing”
The safest strategy is targeted anti-inflammatory care after appropriate evaluation has confirmed a benign course.
Management, prevention, and when to seek care
Living with carotidynia/TIPIC is often less about daily restrictions and more about having a clear playbook: how to respond to symptoms, how to reduce recurrence risk, and when to escalate care.
Day-to-day management during an episode
If you have been evaluated and TIPIC/carotidynia is the working diagnosis:
- Take medications exactly as directed, including stomach-protection strategies if advised.
- Keep pain notes for 7–14 days: location, triggers, response to medication, and any new symptoms.
- Use gentle activity rather than bed rest. Light walking and normal daily movement often help prevent stiffness.
- Avoid pressing repeatedly on the tender spot—checking it can keep the area irritated.
Practical prevention strategies
There is no guaranteed prevention, but these steps may reduce neck strain and improve vascular health:
- Posture breaks: Every 30–60 minutes, reset your neck and shoulders if you work at a desk or drive often.
- Neck-friendly ergonomics: Screen at eye level, shoulders relaxed, avoid cradling a phone between ear and shoulder.
- Risk-factor control: If you have hypertension, diabetes, or high cholesterol, managing them lowers overall vascular risk and can simplify future evaluations.
- Avoid risky neck forces: Be cautious with high-velocity neck manipulation, especially if you have recurrent symptoms or vascular risk factors.
When to seek care promptly
Even if you have had carotidynia/TIPIC before, seek prompt medical review if:
- The pain is different in character (sudden, tearing, or spreading)
- It occurs after trauma or a forceful neck movement
- It lasts longer than 2 weeks despite treatment
- You develop fever, progressive swelling, or difficulty swallowing
- You notice any neurologic symptoms, even if they are brief
Questions to ask your clinician
Arriving prepared helps you get clarity quickly:
- What diagnoses were considered and ruled out?
- Which imaging was done, and what did it show around the carotid?
- Should I have follow-up imaging, and when?
- What is my safest pain-control plan given my medical history?
- What symptoms should trigger an emergency visit?
Outlook
Most people recover fully from an episode. The most meaningful long-term step is ensuring your first episode (and any unusual recurrence) is evaluated carefully so that “carotidynia” is not used as a shortcut label. With that foundation, management tends to be straightforward: treat inflammation, monitor improvement, and know the red flags.
References
- Transient perivascular inflammation of the carotid artery (TIPIC) syndrome 2022 (Observational Study)
- Long-term clinical and ultrasound follow-up after transient perivascular inflammation of the carotid artery (TIPIC) syndrome: a multicenter study 2024 (Multicenter Study)
- Tips for Transient Perivascular Inflammation of the Carotid Artery Syndrome 2024
- Transient Perivascular Inflammation of the Carotid Artery (TIPIC) Syndrome: An Atypical Cause of Neck Pain 2023
Disclaimer
This article is for educational purposes only and does not replace individualized medical advice, diagnosis, or treatment. Neck pain over the carotid artery can sometimes signal urgent conditions (including vascular emergencies). If you have sudden severe pain, neurologic symptoms, vision changes, fever with worsening swelling, or trouble breathing or swallowing, seek emergency medical care. For medication decisions—especially NSAIDs or corticosteroids—consult a qualified clinician who can account for your health history, other medications, and risk factors.
If you found this article helpful, please consider sharing it on Facebook, X (formerly Twitter), or any platform you prefer, and follow us on social media. Your support through sharing helps our team keep producing clear, reliable health content.






