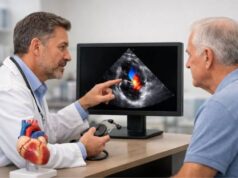
Danon cardiomyopathy is a form of heart muscle disease (cardiomyopathy: the heart muscle becomes thick, weak, or stiff) linked to Danon disease, a rare inherited condition. For many families, the first clue is not a genetics report—it is a teen or young adult who tires too easily, faints, or develops a fast or irregular heartbeat. Because Danon cardiomyopathy can progress quickly, early recognition matters: it can change how closely someone is monitored, when treatments begin, and when advanced options such as implantable devices or transplant evaluation should be discussed.
This guide explains what Danon cardiomyopathy is, why it happens, who is at risk, what symptoms to watch for, how doctors confirm the diagnosis, and what treatment and long-term management often look like in real life.
Table of Contents
- How Danon cardiomyopathy affects the body
- Genetic cause and risk in families
- First symptoms, progression, complications
- How Danon cardiomyopathy is diagnosed
- Treatment options and what to expect
- Day-to-day management and long-term outlook
How Danon cardiomyopathy affects the body
Danon cardiomyopathy refers to the heart problems that occur in Danon disease—most often a rapidly progressive cardiomyopathy paired with rhythm and conduction issues. Danon disease is a multisystem condition, meaning it can affect more than the heart (for example skeletal muscle, vision, and sometimes learning or attention). But the heart is usually the organ that drives the most serious risk, so cardiomyopathy is the clinical center of gravity.
In many people—especially males—Danon cardiomyopathy starts as hypertrophic cardiomyopathy (HCM), where the left ventricle becomes abnormally thick. Thick muscle can make it harder for the heart to fill between beats, raising pressures in the heart and lungs. Over time, some patients transition toward a “burned-out” phase that resembles dilated cardiomyopathy (DCM), where the ventricle enlarges and pumping strength (ejection fraction) declines. It is possible to see both thickening and weakness at different stages, which can be confusing unless the care team is familiar with the disease.
A second hallmark is electrical instability. The heart’s wiring system can develop:
- Pre-excitation patterns such as Wolff–Parkinson–White (WPW), which can trigger episodes of very fast heart rate
- Conduction delay or block, where signals travel too slowly through the heart
- Atrial arrhythmias (like atrial fibrillation or flutter) and ventricular arrhythmias, which can be life-threatening
The third major feature is fibrosis—scar tissue in the heart muscle. Fibrosis raises the risk of arrhythmias and can be an early warning sign of a more aggressive course. Cardiac MRI often detects this scarring even when a person still feels “mostly fine,” which is why imaging is not just about describing structure; it helps estimate risk and plan timing.
A practical way to think about Danon cardiomyopathy is as a condition with two tracks running in parallel: mechanical function (thickness, stiffness, pumping strength) and electrical risk (arrhythmias and conduction disease). Good care addresses both tracks at the same time, not one after the other.
Genetic cause and risk in families
Danon disease is caused by a change (pathogenic variant) in the LAMP2 gene on the X chromosome. LAMP2 is involved in the cell’s recycling system, which helps break down and clear worn-out proteins and energy stores. When this system fails, certain tissues—especially heart muscle—accumulate abnormal material inside cells. Over years, that buildup contributes to inflammation, scarring, and dysfunction.
Because LAMP2 is on the X chromosome, inheritance and severity often differ by sex:
- Males (with one X chromosome) are more likely to have earlier onset and faster progression, sometimes beginning in childhood or adolescence.
- Females (with two X chromosomes) can range from mild to severe. Symptoms often start later, but some females develop serious cardiomyopathy and arrhythmias and need advanced therapies as well.
From a family-planning standpoint, the key patterns are:
- An affected male passes the altered gene to all daughters and no sons.
- A female carrier/affected individual has a 50% chance to pass the altered gene to each child, regardless of sex.
- A person can be the first in the family due to a new (de novo) variant, but once present, it can be inherited across generations.
“Risk factors” for developing Danon cardiomyopathy are therefore mostly genetic and family-based rather than lifestyle-based. However, several factors can shape how the disease expresses itself:
- Age and sex (earlier and often more severe in males, but variable in females)
- Variant type (some variants may be associated with earlier or more heart-predominant disease, though predicting an individual course remains imprecise)
- Baseline heart findings at first evaluation (degree of thickening, presence of fibrosis, early rhythm abnormalities)
What about exercise, diet, or stress? These do not cause Danon cardiomyopathy, but they can influence symptom burden and safety. For example, intense competitive sports may raise arrhythmia risk in people with significant hypertrophy or scarring. This is less about “blame” and more about matching activity to a heart that is structurally and electrically vulnerable.
If Danon disease is suspected or confirmed in one person, cascade testing—systematically offering genetic testing to close relatives—can identify others early, before the first serious event. That early window is valuable, because surveillance and preventive strategies work best when started before advanced heart failure.
First symptoms, progression, complications
Symptoms can start subtly, and they do not always begin with “classic” heart failure. Many people first notice reduced exercise tolerance: they cannot keep up with peers, recover more slowly after activity, or feel unusually short of breath on stairs. Others present with a rhythm problem, sometimes before any obvious weakness of the heart’s pumping function.
Common early symptoms include:
- Shortness of breath with exertion, chest tightness, or reduced stamina
- Palpitations (a racing, pounding, or irregular heartbeat)
- Lightheadedness, near-fainting, or fainting (syncope), especially with activity
- Unexplained fatigue or needing more sleep than usual
- Swelling in ankles/legs or abdominal fullness (later signs of fluid retention)
Because Danon disease can affect skeletal muscle and other organs, some people also have:
- Mild muscle weakness, cramps, or trouble with sustained activity
- Elevated muscle enzymes on blood tests discovered incidentally
- Vision changes related to retinal involvement (often subtle at first)
- Learning differences, attention challenges, or mild cognitive issues in some patients
Progression is not identical for everyone, but clinicians watch for several predictable turning points:
- Increasing wall thickness and stiffness (common early), which raises filling pressures and can cause breathlessness.
- Development of fibrosis (scarring), which increases arrhythmia risk even if symptoms are mild.
- Declining systolic function (the heart’s squeeze weakens), leading to overt heart failure.
- Electrical instability (WPW pattern, atrial fibrillation/flutter, ventricular tachycardia), which can drive hospitalizations or sudden events.
Complications matter because they guide urgent decisions:
- Sudden cardiac death risk from dangerous ventricular arrhythmias
- Stroke risk if atrial fibrillation occurs, especially without anticoagulation when indicated
- Blood clots in the heart if pumping function declines, which can embolize
- Rapid heart failure progression in some patients, prompting early transplant evaluation
- Medication intolerance (for example low blood pressure limiting dose escalation)
A practical red-flag list for families is short and worth memorizing. Seek urgent medical care (often emergency evaluation) for:
- Fainting or near-fainting, especially during exertion
- New chest pain with shortness of breath
- Sustained palpitations with dizziness, weakness, or breathlessness
- Rapid weight gain over a few days, worsening swelling, or trouble breathing lying flat
- A “worst ever” decline in exercise capacity over weeks to months
In Danon cardiomyopathy, symptoms can lag behind risk. Someone may feel “okay” yet have significant scarring or a high-risk rhythm pattern. That is why routine monitoring is not optional—it is part of safety.
How Danon cardiomyopathy is diagnosed
Diagnosis typically combines three layers: (1) clinical pattern, (2) heart testing, and (3) genetic confirmation. Many people enter the system after an abnormal ECG, a murmur, fainting, or family history of cardiomyopathy or early transplant.
1) History and family clues
Clinicians look for early onset cardiomyopathy, arrhythmias, WPW pattern, and relatives with unexplained heart failure, sudden death, or transplant at a young age. They also ask about muscle symptoms, vision changes, and learning differences—not because these define the disease alone, but because the constellation increases suspicion.
2) Core heart tests
Most evaluations include:
- ECG (electrocardiogram): may show WPW/pre-excitation, conduction delay, abnormal voltages from thick muscle, or rhythm disturbances.
- Echocardiogram: measures wall thickness, chamber size, outflow obstruction, diastolic function, and ejection fraction. Serial echocardiograms show trajectory over time.
- Holter or event monitoring: captures intermittent arrhythmias over 24–48 hours or longer, especially if symptoms are sporadic.
- Cardiac MRI: adds detail on anatomy and, crucially, detects fibrosis (late gadolinium enhancement). The burden and pattern of scarring can influence risk discussions and timing of interventions.
3) Laboratory and multisystem assessment
Blood tests may reveal elevated creatine kinase (CK) or liver enzymes (AST/ALT) without primary liver disease—often reflecting muscle involvement. Eye evaluation may detect retinal changes. A neuromuscular assessment can document mild weakness and guide physical therapy.
4) Genetic testing (the confirmation step)
A pathogenic or likely pathogenic variant in LAMP2 confirms Danon disease in most modern diagnostic pathways. If a person has a compatible phenotype but genetic testing is negative or uncertain, specialists may broaden testing (larger cardiomyopathy gene panels, deletion/duplication analysis, or more comprehensive sequencing). In selected cases, tissue studies can show characteristic vacuoles or reduced LAMP2 protein, but biopsy is less commonly needed today because genetic testing is safer and more definitive.
Differential diagnosis (what Danon can mimic)
Danon cardiomyopathy can resemble sarcomeric HCM, other storage disorders (such as Fabry disease), mitochondrial disease, or inflammatory cardiomyopathies. The distinguishing features are often the speed of progression, early electrical findings (like WPW), fibrosis pattern on MRI, and the broader multisystem signals.
A helpful mindset is: diagnosis is not a single test—it is a risk-classification process. The goal is to name the condition early enough that monitoring and treatment stay ahead of the disease, rather than reacting after a crisis.
Treatment options and what to expect
There is no single “one-size” treatment for Danon cardiomyopathy, because care must match stage (hypertrophic vs dilated/weak), symptoms, and arrhythmia risk. Most treatment plans combine heart-failure therapy, rhythm management, and timely consideration of advanced options.
1) Medications for heart function and symptoms
Depending on the phenotype, clinicians may use:
- Beta-blockers to slow heart rate, reduce arrhythmias, and improve filling time in stiff hearts.
- ACE inhibitors/ARBs/ARNI (selected cases) to support remodeling and reduce heart-failure progression when systolic function declines.
- Mineralocorticoid receptor antagonists (such as spironolactone/eplerenone) for heart failure with reduced ejection fraction.
- Diuretics to relieve congestion (swelling, fluid in lungs) when fluid retention develops.
- SGLT2 inhibitors are increasingly used in heart failure broadly; eligibility depends on age, kidney function, blood pressure, and clinician judgment.
In hypertrophic phases with obstruction, medication choices and dosing are individualized, and some drugs used in systolic failure may be limited by low blood pressure.
2) Arrhythmia and conduction management
This often determines safety more than symptoms do.
- WPW or supraventricular tachycardias: electrophysiology (EP) evaluation may lead to catheter ablation of an accessory pathway when appropriate.
- Atrial fibrillation/flutter: rhythm or rate control plus careful consideration of anticoagulation to reduce stroke risk.
- Bradycardia or heart block: pacemaker implantation when conduction disease causes slow rates or pauses.
3) Implantable cardioverter-defibrillator (ICD) decisions
An ICD can treat life-threatening ventricular arrhythmias. In Danon cardiomyopathy, ICD conversations tend to happen earlier than in many other cardiomyopathies because arrhythmic risk can be substantial and fibrosis may appear early. The decision depends on factors such as prior sustained ventricular arrhythmias, fainting suspected to be arrhythmic, significant scarring, very thick heart muscle, or reduced ejection fraction.
4) Advanced heart failure therapy and transplant
For some patients, heart failure progresses despite optimal medications. At that point, timely referral to an advanced heart failure/transplant center is crucial. Evaluation does not mean “you must have a transplant now.” It means:
- Mapping trajectory and timing
- Addressing barriers early (nutrition, social support, vaccination status, other organ involvement)
- Considering mechanical circulatory support when needed
- Avoiding last-minute, high-risk emergency decisions
Outcomes after transplant in Danon disease are considered acceptable in published series, which supports transplant as a meaningful option when indicated. Post-transplant care is highly specialized and requires long-term follow-up.
5) Emerging and investigational therapies
Research into gene-targeted and disease-specific approaches is active, but most patients today are treated with best-practice cardiomyopathy and arrhythmia care. If clinical trials are available, they are typically coordinated through specialty centers familiar with Danon disease.
The most important “what to expect” message is this: treatment is usually a sequence, not a single decision. Regular reassessment lets the care team shift strategies as the heart changes over time.
Day-to-day management and long-term outlook
Living well with Danon cardiomyopathy is less about perfection and more about consistency: keeping appointments, tracking symptoms, and making decisions early—before the heart forces urgent choices.
Surveillance that actually protects you
Most people benefit from a structured schedule that may include:
- Regular cardiology visits with ECG and symptom review
- Echocardiography at intervals based on severity and rate of change
- Periodic rhythm monitoring (Holter/event monitor), even if symptoms are quiet
- Cardiac MRI when clinically useful to track fibrosis and function
- Lab checks for kidney function and electrolytes when on heart medications
If Danon disease is confirmed, multidisciplinary care matters. Eye exams, neuromuscular input, and genetics counseling are not “extras”—they help anticipate problems and improve quality of life.
Safe activity and exercise
Movement is important, but the dose and type matter. Many patients can do moderate aerobic activity, flexibility work, and carefully selected resistance training, while avoiding extremes that raise arrhythmia risk. A practical approach:
- Aim for regular, moderate activity most days if cleared by cardiology.
- Avoid sudden all-out exertion, dehydration, and stimulant-heavy supplements.
- Ask for a specific exercise prescription if there is significant hypertrophy, fibrosis, a history of fainting, or arrhythmias.
Nutrition and fluids
There is no single “Danon diet,” but heart-failure principles often apply:
- If fluid retention is present, sodium reduction and fluid guidance can reduce symptoms.
- Maintain adequate protein and calories, especially if muscle weakness or poor appetite appears.
- Avoid unregulated performance supplements; some can provoke arrhythmias or interact with medications.
Medication habits that prevent crises
Many hospitalizations happen after missed doses, abrupt stopping due to side effects, or mixing medications with over-the-counter products. Use a simple system:
- One pharmacy when possible
- A weekly pill organizer
- A written list of medications and doses in the phone
- A clear plan for what to do if vomiting/illness prevents taking pills
Long-term outlook and planning
Prognosis varies widely, especially between males and females, and between early hypertrophic stages and later heart-failure stages. What improves outlook most is early identification, close monitoring, and timely escalation to advanced therapies when needed. Families should also plan for:
- Genetic counseling and testing of relatives
- School/work accommodations when fatigue or monitoring demands increase
- Emergency planning: knowing which hospital can manage complex arrhythmias and cardiomyopathy
- Conversations about ICDs, transplant evaluation, and goals of care before decisions become urgent
When to see a doctor sooner than planned
Call your cardiology team promptly for:
- New or worsening shortness of breath, swelling, or rapid weight gain
- New fainting, near-fainting, or sustained palpitations
- A marked drop in exercise capacity over days to weeks
- Medication side effects that lead you to consider stopping a drug
Danon cardiomyopathy asks for a more proactive rhythm than many conditions. The goal is not to live in fear; it is to build a routine that makes serious events less likely and keeps options open.
References
- International Consensus on Differential Diagnosis and Management of Patients With Danon Disease: JACC State-of-the-Art Review – PubMed 2023 (Guideline/Consensus Review)
- Danon Disease – GeneReviews® – NCBI Bookshelf 2024 (Expert Review)
- Focusing in on the Danon Disease Heart – PMC 2024 (Review/Commentary)
- Cardiac Transplantation in Danon Disease – PubMed 2022 (Outcomes Study)
- An International Longitudinal Natural History Study of Patients With Danon Disease: Unique Cardiac Trajectories Identified Based on Sex and Heart Failure Outcomes – PubMed 2025 (Cohort/Natural History Study)
Disclaimer
This article is for general education and does not replace individualized medical care. Danon cardiomyopathy can progress quickly and may raise the risk of dangerous heart rhythms and heart failure, so diagnosis, monitoring, activity guidance, and treatment choices should be made with a qualified clinician—ideally a cardiologist experienced in inherited cardiomyopathies. If you have chest pain, fainting, severe shortness of breath, or sustained palpitations, seek urgent medical attention.
If you found this article useful, please consider sharing it on Facebook, X (formerly Twitter), or any platform you prefer, and follow us on social media. Your shares help more families find reliable health information and support our team in producing high-quality content.