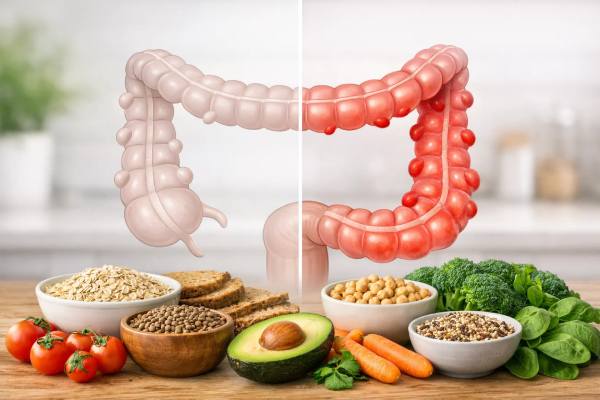
Diverticular disease is often described as a single condition, but it is really two related states with very different meanings. Diverticulosis refers to small pouches in the colon wall that are common with age and often cause no symptoms at all. Diverticulitis is what happens when one or more of those pouches becomes inflamed, sometimes with infection, leading to pain and systemic symptoms that may require medical treatment. Knowing the difference matters because the diet that supports comfort during a flare is not the same diet that supports long-term prevention. It also helps you recognize which symptoms are typical, which are not, and when it is safer to stop self-care and seek urgent evaluation. This guide explains how diverticulosis and diverticulitis differ, what symptoms point toward each, how food choices change across phases, and which prevention strategies are worth prioritizing for the long run.
Essential Insights
- Diverticulosis is common and usually silent, while diverticulitis is an inflammatory flare that often causes steady pain and may include fever or nausea.
- Short-term low-fiber eating can ease symptoms during a diverticulitis flare, but fiber is typically a long-term ally for bowel regularity and prevention.
- New bleeding, worsening pain, persistent fever, vomiting, or inability to hydrate should prompt medical care rather than diet-only management.
- After a flare improves, rebuild fiber gradually over 2–4 weeks, increasing only when pain is stable and stools are moving comfortably.
Table of Contents
- Diverticulosis and diverticulitis explained
- Symptoms that help you tell them apart
- How doctors diagnose and treat each
- Diet during diverticulitis a practical phased plan
- Diet with diverticulosis building a prevention pattern
- Prevention beyond food habits that matter
Diverticulosis and diverticulitis explained
Diverticula are small outpouchings that form in weak spots of the colon wall, most often in the lower part of the large intestine. When you have diverticula, the condition is called diverticulosis. When one or more diverticula becomes inflamed, the condition is called diverticulitis. They sound similar, but their day-to-day impact can be completely different.
Diverticulosis is common and often harmless
Diverticulosis becomes more common with age, and many people never know they have it until it is found on colonoscopy or a scan done for another reason. Importantly, diverticulosis does not automatically mean you will develop diverticulitis. Some people live their whole lives with diverticula and never have a flare.
Diverticulosis can still matter, though, because it can be associated with:
- Changes in bowel habits for some people (often constipation, sometimes bloating)
- Anxiety about food and “what is safe”
- A separate complication called diverticular bleeding (discussed later)
Diverticulitis is an inflammatory event
Diverticulitis is not simply “diverticula acting up.” It is an inflammatory process that can range from mild and uncomplicated to severe and complicated. Complications may include abscess, perforation, fistula, or obstruction. These terms can sound alarming, but they are also a reason to take a flare seriously and to avoid assuming that diet alone is always enough.
Why the difference changes diet advice
During diverticulitis, the colon can be tender and sensitive to stretch. Large meals and bulky stools can worsen discomfort even if they did not cause the flare. A short-term shift toward lower-fiber, gentler foods can reduce symptom load while recovery begins.
With diverticulosis, the long-term goal is often the opposite: building a pattern that supports softer, easier-to-pass stools and less straining. That usually involves adequate fiber, hydration, and a generally high-quality diet. The key is timing. Comfort during a flare and prevention after recovery are related goals, but they are not achieved with the same menu.
Symptoms that help you tell them apart
Digestive symptoms overlap across many conditions, so it helps to focus on patterns. The “feel” of diverticulitis is often distinct: steady, localized pain with systemic features, rather than occasional cramps that move around.
Diverticulosis usually has no symptoms
Most people with diverticulosis feel normal. If symptoms occur, they tend to be nonspecific:
- Bloating that fluctuates
- Constipation or irregular stools
- Mild, intermittent discomfort that improves after a bowel movement
These symptoms can also come from common issues like constipation itself, diet changes, stress, or disorders of gut-brain interaction. Diverticulosis is often a background finding rather than the primary explanation for daily discomfort.
Diverticulitis symptoms often look like a flare pattern
Typical diverticulitis symptoms include:
- Steady abdominal pain, often in the lower left abdomen (location can vary)
- Tenderness to touch
- Fever or chills in some cases
- Nausea and reduced appetite
- Constipation or diarrhea
- A sense of feeling unwell beyond the gut
Pain that is new, persistent, and progressively worsening over hours to a day deserves medical attention even if you suspect a “familiar flare.” Recurrent patterns should still be evaluated because not every episode of abdominal pain in someone with diverticula is diverticulitis.
Diverticular bleeding is different from diverticulitis
Diverticular bleeding usually causes painless rectal bleeding, often bright red or maroon, and can be brisk. It does not usually present with fever or steady localized pain. Any new bleeding should be discussed with a clinician, and heavy bleeding requires urgent care.
Red flags that should override diet plans
Seek prompt medical evaluation if you have:
- Worsening or severe abdominal pain, especially with guarding or rigidity
- Persistent fever
- Repeated vomiting or inability to keep fluids down
- Fainting, confusion, or signs of dehydration
- New rectal bleeding, black stools, or dizziness with bleeding
- Symptoms that worsen steadily over 24–48 hours
These signs can indicate complicated disease or an alternative diagnosis that needs imaging and treatment, not just dietary adjustment.
How doctors diagnose and treat each
Understanding the basic diagnostic approach helps you use diet appropriately. Many people delay care because they assume a flare will “settle” if they restrict food enough. In reality, the key question is whether the episode is uncomplicated and stable, or complicated and escalating.
Diagnosis often relies on imaging and clinical context
Diverticulosis is commonly found during colonoscopy or imaging. Diverticulitis is often suspected based on symptoms, but imaging (such as a CT scan) may be used to confirm the diagnosis, assess severity, and look for complications.
This distinction matters because other problems can mimic diverticulitis, including appendicitis, kidney stones, gynecologic conditions, inflammatory bowel disease, ischemic colitis, and even colon cancer. A clear diagnosis prevents repeated flares from being treated blindly.
Treatment depends on severity and risk factors
Management varies by person and by episode. Common elements include:
- Pain control and hydration
- A diet plan matched to symptom severity
- Antibiotics in select situations (not always needed for mild uncomplicated cases)
- Hospital care or procedures if complications are present
If you are immunocompromised, older, frail, or have significant comorbidities, clinicians often take a lower threshold for antibiotics, imaging, and observation because the risk profile changes.
Follow-up after a diverticulitis episode
After an episode, clinicians may discuss whether you need follow-up testing such as colonoscopy, depending on your history, the severity of the episode, and how recently you were screened. The goal is to rule out other conditions that can look similar and to plan prevention strategies.
Where diet fits in the medical plan
Diet is supportive, not diagnostic. It is most helpful when used to:
- Maintain hydration and energy during recovery
- Reduce discomfort related to bulky stool and large meals
- Prevent constipation from low intake or pain medications
- Provide a structured “return to normal” so you do not remain overly restricted
If your symptoms are severe or escalating, treat dietary changes as a comfort measure while you seek evaluation, not as a substitute for care.
Diet during diverticulitis a practical phased plan
The best diverticulitis diet is not a single list. It is a phased plan that matches symptom intensity and improves step-by-step. Some people can tolerate soft foods from day one; others need a short period of liquids. The goal is to avoid two extremes: eating heavy meals too soon, and staying on minimal intake long after symptoms improve.
Phase 1: first 24 to 48 hours if symptoms are intense
If pain is significant, nausea is present, or eating worsens symptoms quickly, a short clear-liquid or mostly-liquid period may help. Options include broth, oral rehydration solutions, diluted juice without pulp, gelatin, and tea.
Practical guardrails:
- Sip consistently rather than forcing large volumes at once.
- If sugary drinks worsen diarrhea, prioritize broth and oral rehydration solutions.
- If symptoms do not improve within 48 hours, contact a clinician rather than extending restriction indefinitely.
Phase 2: low-fiber foods as pain settles
As pain and nausea improve, transition to low-fiber foods that reduce stool bulk:
- Refined grains: white rice, pasta, cream of wheat, plain crackers
- Soft proteins: eggs, fish, tofu, tender poultry
- Smooth dairy if tolerated: yogurt, mild cheese
- Cooked and peeled produce in small portions: applesauce, canned peaches, well-cooked carrots
- Soups with noodles or rice
Helpful tactics:
- Eat smaller meals more often rather than large portions.
- Avoid very spicy, greasy, or deep-fried foods if they trigger cramping.
- If constipation develops, increase fluids and gentle walking rather than cutting food further.
Phase 3: gradual return to fiber over 2 to 4 weeks
Once pain is mild and stable and bowel movements are occurring without major straining, begin rebuilding fiber slowly:
- Start with soluble-fiber choices that are often gentler: oats, well-cooked vegetables, peeled fruits, and soups with blended vegetables.
- Increase one step every 3–4 days if symptoms remain calm.
- Save large salads, bran cereals, and big portions of beans for later in the ramp.
The most common mistake is jumping from very low fiber to very high fiber overnight, which can cause gas and discomfort that feels like relapse. A gradual plan reduces that risk.
When to pause the ramp and call your clinician
Stop advancing and seek guidance if you notice:
- Pain returning and building rather than fading
- New fever
- Repeated vomiting
- Increasing bloating with inability to pass gas or stool
- New bleeding
During recovery, you are aiming for steady improvement, not perfection. Mild day-to-day fluctuations can happen, but worsening trends should not be ignored.
Diet with diverticulosis building a prevention pattern
With diverticulosis, the primary dietary goal is usually to support regular bowel movements and reduce chronic straining. While no diet guarantees prevention, higher diet quality and adequate fiber are consistently linked with better bowel function and a lower likelihood of diverticulitis in many populations.
Fiber as a long-term tool not a quick fix
Fiber helps stool hold water and move more easily through the colon. That can reduce constipation, decrease straining, and lower the pressure spikes that many clinicians believe contribute to diverticula forming and becoming symptomatic.
A practical approach is to aim for a fiber intake you can maintain. For many adults, that may fall in the 25–30 grams per day range, but your best target is the amount that produces:
- Soft, formed stools
- Minimal straining
- Predictable frequency
- Manageable gas
If you currently eat very little fiber, start slowly. A sudden jump can cause bloating even when the direction is correct.
Build fiber from foods you tolerate
A steady, prevention-oriented plate often includes:
- Vegetables and fruits (cooked or raw depending on tolerance)
- Whole grains (oats, barley, brown rice, whole-grain bread)
- Legumes (lentils, beans, chickpeas) introduced gradually
- Nuts and seeds if tolerated
- Lean proteins and fish
- Healthy fats in moderate amounts
If you have sensitive digestion, you can still build fiber with gentler choices: oats, chia or ground flax in small amounts, peeled fruits, and well-cooked vegetables.
Hydration and fiber work together
Fiber without adequate fluid can worsen constipation. You do not need to obsess over water math, but do watch for signs of under-hydration: dark urine, hard stools, and frequent straining. If you increase fiber, increase fluids and consider a short walk after meals to support motility.
Do you need to avoid nuts seeds and popcorn
Most modern guidance does not require routine avoidance for everyone with diverticulosis. Many people tolerate nuts and seeds well, and some evidence suggests they are not harmful and may be neutral or protective as part of an overall high-quality diet. If a specific food reliably triggers symptoms for you, personalize the plan, but avoid turning outdated rules into lifelong restriction without evidence from your own experience.
Prevention beyond food habits that matter
Diet is central, but prevention is broader than fiber alone. Diverticulitis risk is influenced by weight, smoking status, physical activity, and medication exposures. The most effective prevention plan is often a bundle of “boring but powerful” habits that reduce inflammation and support normal bowel function.
Maintain a healthy weight and move routinely
Higher body weight is consistently associated with higher diverticulitis risk. Physical activity appears protective, likely through effects on motility, metabolic health, and inflammation. You do not need extreme training. Consistent movement is the point:
- A daily walk after meals
- Two to three sessions per week of strength training
- More standing and less prolonged sitting when possible
If you have constipation, gentle movement can be a surprisingly effective part of prevention.
Avoid smoking and moderate alcohol
Smoking is linked with higher risk of diverticular complications and worse outcomes. If you smoke, quitting is one of the most meaningful risk-reduction steps you can take for the colon and for overall health. Alcohol in excess can worsen sleep, hydration, and inflammation, and it may indirectly worsen bowel habits.
Be thoughtful about regular NSAID use
Frequent use of nonsteroidal anti-inflammatory drugs has been associated with diverticulitis complications in many clinical discussions. Do not stop prescribed medications on your own, but do tell your clinician if you use NSAIDs regularly (for example, multiple times per week). There may be safer pain-management strategies depending on your health history.
Prevent constipation with a plan you can repeat
Constipation management is often prevention management. A simple plan includes:
- Consistent meal timing (especially breakfast)
- Fiber that is increased gradually
- Adequate fluids
- A predictable bathroom routine without rushing or straining
- Early intervention when stools harden (more fluid, more soluble fiber, more walking)
If you frequently rely on stimulant laxatives or have persistent straining, discuss it with your clinician. Pelvic floor dysfunction and other treatable causes can hide behind the word “constipation.”
Know your personal recurrence signals
Many people can identify early warning signs: a few days of constipation, new localized tenderness, appetite drop, or fatigue. Tracking those signals can help you respond early with hydration, gentle meals, and medical guidance when appropriate. The goal is not fear. It is preparedness.
References
- AGA Clinical Practice Update on Medical Management of Colonic Diverticulitis: Expert Review 2021 (Guideline)
- Diagnosis and Management of Acute Left-Sided Colonic Diverticulitis: A Clinical Guideline From the American College of Physicians 2022 (Guideline)
- Colonoscopy for Diagnostic Evaluation and Interventions to Prevent Recurrence After Acute Left-Sided Colonic Diverticulitis: A Clinical Guideline From the American College of Physicians 2022 (Guideline)
- Lifestyle factors, genetic susceptibility and risk of incident diverticulitis: an integrated analysis of four prospective cohort studies and electronic health records-linked biobank 2025 (Cohort Study)
- Are Nuts Safe in Diverticulosis? A Mixed-Methods Systematic Review of Available Evidence 2025 (Systematic Review)
Disclaimer
This article is for educational purposes and does not provide medical advice, diagnosis, or treatment. Diverticulitis can range from mild inflammation to serious complications that require urgent evaluation. Seek prompt medical attention for worsening or severe abdominal pain, persistent fever, repeated vomiting, inability to keep fluids down, fainting, confusion, black stools, or significant rectal bleeding. If you are immunocompromised, pregnant, older, or have major medical conditions, contact a qualified clinician early when symptoms arise. Dietary changes can support comfort and recovery, but they should not delay appropriate medical care.
If you found this article useful, please share it on Facebook, X (formerly Twitter), or any platform you prefer so others can better understand diverticulosis and diverticulitis and make safer, more informed choices.






