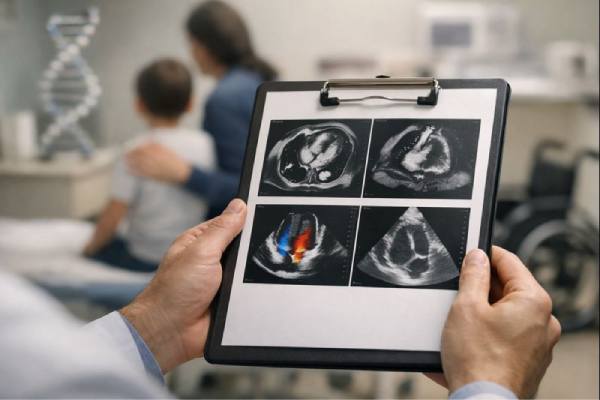
Duchenne cardiomyopathy is the heart-related part of Duchenne muscular dystrophy (Duchenne), a genetic condition that weakens muscles over time. While most families first notice walking or climbing difficulties, the heart can be affected quietly for years before symptoms appear. The challenge is that people with Duchenne may be less physically active, so typical “shortness of breath with exertion” can be easy to miss. The good news is that modern care focuses on early screening and early treatment—often before the heart feels weak—because that is when therapy can slow damage the most. This article explains how Duchenne affects the heart, which factors raise risk, what changes to watch for, how clinicians confirm the diagnosis, and what treatment and day-to-day management usually involve across childhood, adolescence, and adulthood.
Table of Contents
- How Duchenne affects the heart
- Why cardiomyopathy develops in Duchenne
- Early signs and serious complications
- How doctors screen and diagnose it
- Medicines and devices that help
- Daily management and when to seek care
How Duchenne affects the heart
In Duchenne muscular dystrophy, the body cannot make enough functional dystrophin (a protein that helps muscle cells stay stable). Most people think first of leg and arm weakness, but the heart is also a muscle—and it relies on the same kind of structural support. Over time, heart muscle cells become more fragile, small injuries accumulate, and the body replaces damaged areas with scar and fatty tissue. That remodeling can weaken the heart’s squeeze, change how it relaxes, and disrupt the electrical pathways that keep the heartbeat steady.
Duchenne cardiomyopathy often begins long before a person “feels” heart symptoms. The earliest changes are frequently found on imaging, such as subtle reductions in heart strain (how the muscle fibers deform with each beat) or small patches of fibrosis (scarring) on cardiac MRI. Clinically, many people develop a form of dilated cardiomyopathy (an enlarged, weaker left ventricle) during adolescence or young adulthood, though the timeline varies.
Several features make Duchenne cardiomyopathy unique:
- Silent progression: Reduced activity can hide early exercise-related symptoms.
- Patchy damage: Scarring may start in characteristic regions of the heart, then spread.
- Rhythm vulnerability: As scar increases, the risk of atrial arrhythmias and ventricular arrhythmias rises.
- Interdependence with lungs and spine: Breathing weakness, sleep-disordered breathing, and chest wall changes can increase strain on the heart and complicate symptom interpretation.
A practical insight for families is that “no symptoms” does not mean “no heart involvement.” In Duchenne, proactive screening is not optional extra care—it is part of the core plan, because the goal is to treat early, when the heart still has strong reserve. That approach can delay heart failure, reduce hospitalizations, and improve long-term stability.
Why cardiomyopathy develops in Duchenne
The root cause of Duchenne cardiomyopathy is the dystrophin problem, but the pathway from gene change to heart weakness has several steps. Understanding those steps helps explain why early treatment matters and why two people with Duchenne can have very different heart timelines.
At the cell level, dystrophin normally helps the muscle cell membrane handle the mechanical stress of contraction. Without it, heart cells are more likely to develop tiny tears and abnormal calcium movement. That triggers inflammation and, over time, replacement of healthy muscle with fibrous tissue. Fibrosis is a major turning point: scar tissue does not contract like heart muscle, and it can interrupt electrical signals, raising arrhythmia risk.
Risk is shaped by a mix of biology, age, and health context:
- Age and disease duration: Heart involvement becomes more common as people get older, especially through adolescence and adulthood.
- Genetic modifiers: The exact mutation and other genes may influence how quickly fibrosis and dysfunction appear.
- Steroid exposure: Long-term corticosteroids are used primarily for skeletal muscle function, but many studies suggest they may also delay cardiac decline in a preventive sense.
- Blood pressure and heart rate load: Even mild, persistent elevations in heart rate or blood pressure can accelerate remodeling in a heart that already has less resilience.
- Respiratory status: Untreated sleep apnea or low nighttime oxygen can increase stress hormones and strain the heart.
- Nutrition and body composition: Both undernutrition (less muscle reserve) and excess weight (higher workload) can worsen overall cardiovascular strain.
A key nuance: Duchenne cardiomyopathy is not just “heart failure that happens later.” It is a progressive muscle disease of the myocardium, often starting with microscopic changes years before ejection fraction drops. That is why many experts support starting certain heart-protective medicines before overt symptoms—because the goal is to slow fibrosis and remodeling, not simply respond once the heart is clearly weak.
Finally, emotional and practical stressors matter. Missed follow-up visits, difficulty tolerating tests, or fragmented specialty care can delay detection. Families do best when cardiology, neurology, pulmonology, rehabilitation, and primary care share a single, coordinated plan.
Early signs and serious complications
Symptoms in Duchenne cardiomyopathy can be subtle, and they often overlap with fatigue from muscle weakness, sleep issues, anemia, infections, or the general effort of daily activities. That makes pattern recognition important: new changes that persist, worsen, or cluster together deserve attention even if they seem mild.
Common early symptoms can include:
- Lower stamina compared with the person’s baseline (needing longer rests, tiring sooner with routine tasks)
- New shortness of breath during transfers, wheelchair propulsion, or speaking in long sentences
- Resting fast heartbeat or a “pounding” sensation in the chest
- Poor sleep quality, morning headaches, or daytime sleepiness (sometimes reflecting breathing problems that also strain the heart)
- Reduced appetite or early fullness, which can occur when fluid builds up in the abdomen
As cardiomyopathy advances, signs of fluid retention become more noticeable:
- Swelling in feet, ankles, or lower legs
- Rapid weight gain over several days (often fluid, not fat)
- Belly bloating, nausea, or discomfort
- Needing more pillows to sleep comfortably, or waking up breathless
Arrhythmias may present differently than classic heart failure symptoms. Watch for:
- Palpitations (fluttering or racing)
- Lightheadedness, near-fainting, or fainting
- Episodes of sudden weakness or gray-out feelings
Serious complications can include worsening heart failure, blood clots (especially when the heart chamber enlarges and flow slows), and ventricular arrhythmias. Because some individuals with Duchenne may have limited ability to describe symptoms, caregivers should also notice behavioral clues such as new irritability, reduced participation in usual activities, unexplained sweating, or a new preference for sitting upright.
Seek urgent medical care if any of the following occur:
- Severe breathlessness at rest or difficulty speaking due to shortness of breath
- Fainting, repeated near-fainting, or new confusion
- Chest pain that persists, especially with sweating or nausea
- A sustained rapid heartbeat that does not settle within minutes
- Rapidly worsening swelling, reduced urination, or bluish lips
A practical home tool is a short weekly check-in: resting heart rate, swelling, sleep quality, and a simple “is today harder than last month?” question. In Duchenne cardiomyopathy, small changes can be early warning signs.
How doctors screen and diagnose it
Diagnosis in Duchenne cardiomyopathy is as much about planned surveillance as it is about responding to symptoms. Because early disease is often silent, clinicians typically follow a structured schedule that starts in childhood and continues throughout life.
Most evaluations begin with:
- History and symptom review: fatigue patterns, breathing changes, swelling, palpitations, fainting, and sleep quality.
- Physical exam: heart rate, blood pressure, signs of fluid retention, lung sounds, and circulation.
- Electrocardiogram (ECG): checks rhythm, conduction changes, and patterns that can occur in Duchenne.
- Echocardiogram: measures heart size, pumping function (ejection fraction), valve function, and sometimes strain imaging to detect early weakness.
Cardiac MRI adds important detail, especially when echocardiography images are limited by body habitus or chest wall mechanics. MRI can detect:
- Fibrosis (scar) patterns that may appear before ejection fraction falls
- Changes in chamber size and function with high precision
- Clues pointing to inflammation or other contributors
Blood tests may support the picture, especially when symptoms worsen:
- BNP or NT-proBNP (markers of cardiac stretch)
- Troponin in selected situations (marker of injury)
- Kidney and liver function tests (important when fluid overload is suspected)
- Electrolytes (especially if diuretics or rhythm concerns are present)
Because arrhythmias can be intermittent, clinicians may add:
- Holter monitoring (24–48 hours or longer)
- Event monitors if symptoms are episodic
- Device checks for patients with pacemakers or defibrillators
A crucial part of the diagnostic process is separating heart symptoms from respiratory contributors. In Duchenne, breathing weakness and sleep-disordered breathing can mimic or worsen heart failure symptoms. Many teams coordinate cardiac assessments with pulmonary function testing and sleep evaluations to avoid missing either problem.
Monitoring is not “one test.” It is a trend over time. Clinicians watch for:
- A drop in ejection fraction or worsening strain
- Increasing chamber size
- New or expanding fibrosis on MRI
- Rising heart rate burden or new arrhythmias
- Increasing need for diuretics or oxygen support
Families can help by keeping a medication list, a brief symptom timeline, and prior test dates. That information makes it easier for the care team to detect meaningful change early and adjust treatment before the heart is in crisis.
Medicines and devices that help
Treatment for Duchenne cardiomyopathy has two goals: slow progression (especially fibrosis and remodeling) and treat heart failure or rhythm problems when they appear. Many people benefit most when therapy starts early—often before severe symptoms—because early treatment aims to preserve function, not only rescue it.
Common medication groups include:
- ACE inhibitors or ARBs: often used as foundational therapy to reduce remodeling and lower stress on the heart muscle. Many clinicians start them in late childhood or early adolescence, even when pumping function is still normal, depending on the overall risk profile and imaging findings.
- Beta-blockers: lower heart rate and reduce stress hormones. They are especially helpful when the heart is working harder, the rate is persistently high, or systolic function has begun to decline.
- Mineralocorticoid receptor antagonists (such as eplerenone or spironolactone): used to limit fibrosis and support remodeling. They may be added early when imaging suggests early damage or when ejection fraction starts to fall.
- SGLT2 inhibitors: increasingly used in heart failure care in appropriate patients; the decision depends on age, kidney function, blood pressure, and the clinician’s comfort in neuromuscular populations.
- Diuretics: relieve fluid overload (swelling, breathlessness). They help symptoms quickly but do not replace remodeling-protective therapy.
Medication plans in Duchenne need careful tailoring because low blood pressure, low body mass, kidney function changes, and drug interactions can limit how quickly doses can be increased. Many teams use a “start low, adjust often” approach with follow-up every few weeks during titration.
When advanced disease or high arrhythmia risk is present, devices may be considered:
- Implantable cardioverter-defibrillator (ICD): for selected patients at higher risk of dangerous ventricular rhythms.
- Cardiac resynchronization therapy (CRT): may help when electrical dyssynchrony contributes to weak pumping.
- Temporary or long-term mechanical support: in selected advanced cases, specialized centers may discuss ventricular assist devices on a case-by-case basis.
Cardiac care also interacts with Duchenne-specific therapies. Corticosteroids, respiratory support, infection prevention, and careful anesthesia planning can indirectly protect the heart by reducing physiologic stress. Conversely, dehydration, uncontrolled pain, untreated sleep apnea, and recurrent respiratory infections can tip a fragile cardiovascular system into decompensation.
What to expect: improvement is possible, especially when treatment starts early and is steadily optimized. Even when full recovery is not realistic, many people achieve meaningful stabilization—fewer symptoms, fewer hospitalizations, and a slower decline.
Daily management and when to seek care
Living well with Duchenne cardiomyopathy depends on consistent routines, early recognition of change, and coordinated specialty care. Families often do best when they treat heart management as a long-term maintenance plan rather than a response to emergencies.
Daily and weekly habits that help:
- Medication consistency: take heart medicines at the same time each day. Missed doses can trigger fluid buildup or rhythm instability.
- Simple tracking: record swelling, sleep quality, and “harder than usual” days. If possible, track resting heart rate and blood pressure a few times per week.
- Weight monitoring: if feasible, weigh at least weekly (daily is ideal when heart failure is established). Rapid weight gain over a few days can signal fluid retention.
- Hydration balance: avoid extremes. Dehydration can worsen kidney function and limit medication options; overhydration can worsen congestion.
- Nutrition with purpose: aim for adequate protein and calories to maintain strength, and discuss sodium goals with the care team—especially if swelling is an issue.
- Vaccination and infection planning: respiratory infections can stress the heart. A clear plan for early treatment and airway clearance can prevent spirals.
Activity is usually beneficial when paced correctly. Many people tolerate gentle, regular movement better than sporadic bursts of effort. A practical approach is:
- Choose low-intensity activity that is comfortable and repeatable.
- Increase duration slowly (minutes per week, not leaps).
- Stop early if dizziness, chest discomfort, or unusual breathlessness appears.
Coordination with respiratory care is essential. Nighttime ventilation support, treatment of sleep apnea, and cough-assist strategies can reduce strain on the heart and improve day-to-day energy. Similarly, scoliosis management and seating/positioning can affect breathing mechanics and comfort, indirectly influencing cardiac symptoms.
Know when to call the clinician promptly:
- New swelling, rapid weight gain, or reduced urination
- New shortness of breath, especially at rest or at night
- Persistent resting heart rate that is clearly higher than usual
- New palpitations, dizziness, or near-fainting
- Reduced appetite with abdominal bloating or nausea
Seek urgent or emergency care for severe breathlessness, fainting, chest pain that persists, bluish lips, confusion, or a sustained rapid heartbeat with weakness.
Finally, plan ahead. Ask your team for a written “what to do if” guide that covers medication adjustments during illness, hydration guidance, and when to use urgent services. In Duchenne cardiomyopathy, preparation reduces fear and improves outcomes.
References
- Cardiac treatment for Duchenne muscular dystrophy: consensus recommendations from the ACTION muscular dystrophy committee – PubMed 2025 (Practice Guideline)
- 2022 HRS expert consensus statement on evaluation and management of arrhythmic risk in neuromuscular disorders – PubMed 2022 (Guideline)
- Pharmacological management of dilated cardiomyopathy in Duchenne muscular dystrophy: A systematic review – PubMed 2023 (Systematic Review)
- Duchenne muscular dystrophy – PubMed 2021 (Review)
- Fighting for every beat: cardiac therapies in Duchenne muscular dystrophy – PubMed 2025 (Review)
Disclaimer
This article is for educational purposes and does not replace professional medical advice, diagnosis, or treatment. Duchenne cardiomyopathy can be serious and requires individualized care, especially when symptoms change, medications are being adjusted, or procedures requiring anesthesia are planned. Do not stop or change prescription medications without guidance from your clinical team. If severe shortness of breath, chest pain, fainting, or rapidly worsening swelling occurs, seek urgent medical attention.
If this article helped you, please share it on Facebook, X (formerly Twitter), or any platform you prefer, and follow us on social media. Your support through sharing helps our team continue producing high-quality health content.






