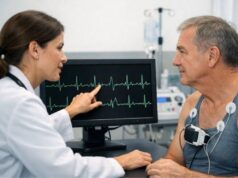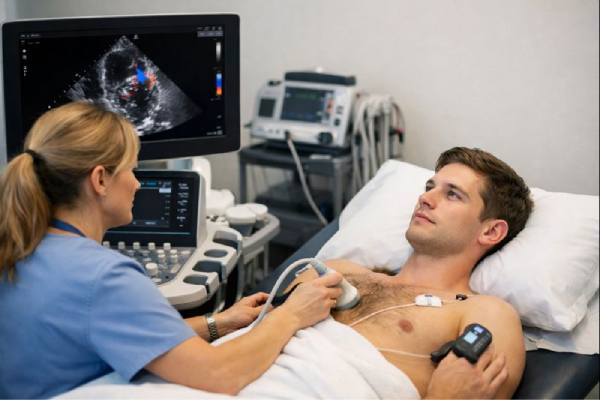
Ebstein anomaly is a heart condition you’re born with (congenital—present at birth) that mainly affects the tricuspid valve (the valve between the right upper and right lower heart chambers). In this condition, parts of the valve sit lower than usual and may not close well. That can make blood leak backward and can change how the right side of the heart grows and works over time.
The experience of Ebstein anomaly varies widely. Some people have mild changes and few symptoms for decades. Others—especially newborns with severe forms—need urgent care early in life. If you’ve just heard this diagnosis, the most helpful next step is learning what “severity” means in your case, what symptoms deserve attention, and which treatments are available now.
Table of Contents
- What is Ebstein anomaly in the heart?
- What causes it and who is at risk?
- Symptoms and complications by age
- How it’s diagnosed and how severe it is
- Treatment options and what to expect
- Long-term management and when to seek care
What is Ebstein anomaly in the heart?
Ebstein anomaly is a structural difference in the right side of the heart that centers on the tricuspid valve. In a typical heart, the tricuspid valve leaflets open and close like flexible doors, allowing blood to move from the right atrium (upper chamber) into the right ventricle (lower chamber), then onward to the lungs. In Ebstein anomaly, two key things often happen:
- The valve leaflets are positioned lower than normal inside the right ventricle (often described as “apical displacement”).
- The leaflets may be malformed or stuck to the heart muscle, so they do not meet and seal properly.
When the valve doesn’t seal, blood can leak backward with each heartbeat. That leak is called tricuspid regurgitation (backflow through the tricuspid valve). Over time, the right atrium may enlarge to handle the extra volume, and the working portion of the right ventricle may be smaller than expected.
Another concept you may hear is “atrialized right ventricle.” This means a segment of the right ventricle behaves more like the atrium because the valve sits lower, effectively moving the “functional” valve opening downward. It’s not that the ventricle becomes an atrium, but that part of it becomes less effective at pumping.
Ebstein anomaly often comes with related findings:
- An opening between the atria, such as an atrial septal defect (a hole between the upper chambers) or a patent foramen ovale. This can allow blood mixing and contribute to low oxygen levels (cyanosis), especially in infants.
- Arrhythmias (abnormal heart rhythms), including extra electrical pathways that can trigger rapid heart rates.
- Changes in right ventricular muscle function, which can influence stamina and fluid balance.
A useful takeaway is that Ebstein anomaly is not a single “one-size” diagnosis. It’s a spectrum. The same label can describe someone who is active with mild valve leakage and someone who needs complex treatment soon after birth. The goal of evaluation is to map where you fall on that spectrum and plan care accordingly.
What causes it and who is at risk?
Ebstein anomaly forms during early fetal development when the tricuspid valve and right ventricle are taking shape. In many cases, there is no single identifiable cause. Instead, clinicians think of it as the result of altered development of valve tissue and its separation from the heart wall.
What is known about causes and risk factors:
- Mostly sporadic, sometimes genetic: Most people have no family history. Still, Ebstein anomaly can occasionally cluster in families or appear with broader genetic syndromes. If there are other congenital differences, developmental delays, or a strong family history of heart defects, genetic counseling may be recommended.
- Medication exposure in pregnancy (notably lithium): Older and newer research has linked first-trimester lithium exposure with an increased risk of certain heart malformations, including Ebstein anomaly. Importantly, the absolute risk for any one pregnancy remains small, and decisions about lithium during pregnancy require careful, individualized balancing of maternal mental health stability and fetal risk.
- Associated congenital heart conditions: Ebstein anomaly can occur alongside other structural findings, particularly atrial-level shunts. These combinations can influence symptoms (like cyanosis) and treatment choices.
- Electrical system differences: Some people have an extra electrical connection between the atria and ventricles (often described as an accessory pathway). This can predispose to episodes of very fast heart rhythm. While this isn’t a “cause” of the valve problem, it is a common companion issue and a major driver of symptoms.
Who is more likely to be diagnosed early?
- Newborns with severe forms may show cyanosis, breathing difficulty, or heart failure signs and are diagnosed immediately.
- Children may be identified because of a heart murmur, reduced exercise tolerance, or episodes of rapid heart rate.
- Adults with mild disease may be diagnosed after an ECG or echocardiogram done for palpitations, a murmur, pregnancy evaluation, or an incidental finding.
A practical point: severity at diagnosis is influenced by who gets screened. Mild cases can go unnoticed for years, which is why prevalence estimates vary by study and setting. That variation does not mean the condition is “changing”; it reflects the wide spectrum and the timing of detection.
If you’re planning a pregnancy and you have Ebstein anomaly, your risk assessment is less about “what caused it” and more about how your heart handles extra blood volume during pregnancy. That planning is a key part of long-term management and can be done proactively.
Symptoms and complications by age
Ebstein anomaly can look very different across life stages. Symptoms depend on how much the valve leaks, how well the right ventricle pumps, whether there is an atrial-level shunt, and whether rhythm problems occur.
In newborns (highest variability):
- Bluish color (cyanosis) from blood mixing at the atrial level
- Fast breathing, poor feeding, sweating with feeds
- Signs of heart strain, such as enlarged liver or poor weight gain
- In severe cases, dangerously low oxygen levels or unstable circulation
Newborn symptoms can shift quickly because early life circulation changes in the first days to weeks after birth. A baby who looks stable at first can worsen as fetal pathways close, which is why close monitoring matters.
In children and teens:
- Shortness of breath with activity, tiring easily
- Slower growth or reduced endurance in sports
- A heart murmur noted on routine exams
- Palpitations or episodes of sudden fast heartbeat (supraventricular tachycardia—an abnormally fast rhythm starting above the ventricles)
In adults:
- Reduced exercise tolerance, especially over years
- Swelling of legs or abdomen if right-sided heart failure develops
- Palpitations, skipped beats, or sustained fast rhythms
- Symptoms that worsen with pregnancy, anemia, thyroid disease, or untreated sleep problems
Key complications to understand:
- Arrhythmias: Ebstein anomaly has a strong association with rhythm disturbances. Accessory pathways can trigger rapid rhythms; atrial enlargement can predispose to atrial flutter or atrial fibrillation. These rhythms can cause dizziness, shortness of breath, chest pressure, or fainting.
- Heart failure symptoms: Long-standing valve leakage can lead to right-sided congestion—leg swelling, abdominal fullness, and reduced stamina.
- Stroke risk in selected patients: If there is an atrial-level shunt, a blood clot from the veins can (rarely) cross to the left side and travel to the brain. This risk rises with certain arrhythmias and other factors.
- Sudden worsening episodes: Fever, dehydration, stimulant use, or untreated arrhythmia can unmask symptoms in people who previously felt well.
Red flags that deserve urgent evaluation:
- Fainting without warning, especially with palpitations
- New cyanosis, especially at rest
- Rapid heart rate that does not settle within minutes
- Chest pain with shortness of breath or severe weakness
- In infants: poor feeding, grunting breathing, or persistent bluish color
A helpful mindset is to track change over time. Many people live well with mild Ebstein anomaly. The goal is to catch the signs that the heart is working harder than it should—and intervene before that strain becomes permanent.
How it’s diagnosed and how severe it is
Diagnosis usually starts with an echocardiogram (heart ultrasound). This test can show the position and movement of the tricuspid valve leaflets, the degree of leakage, and the size and function of the right-sided chambers. Because Ebstein anomaly is a spectrum, the work-up focuses on both confirming the anatomy and grading severity in a way that supports decisions.
Common tests and what they add:
- Echocardiogram (core test): Confirms valve displacement, measures tricuspid regurgitation, estimates pressures, and looks for an atrial-level opening. In infants, it also helps assess blood flow patterns that affect oxygen levels.
- Electrocardiogram (ECG): Looks for rhythm clues such as pre-excitation (signs of an accessory pathway), conduction delays, or atrial enlargement patterns.
- Holter or event monitor: Captures intermittent rhythm episodes over 24–48 hours or longer. This is especially helpful if you have palpitations, unexplained dizziness, or fainting.
- Cardiac MRI: Offers detailed measurement of right ventricular size and function and can quantify leakage with high accuracy. It can be especially useful when echo images are limited or when surgical planning requires precise chamber volumes.
- Exercise testing: Measures functional capacity and oxygen response during exertion and can uncover abnormal blood pressure or rhythm responses.
- Cardiac catheterization (selected cases): Measures pressures directly, evaluates oxygen levels, and helps plan complex interventions. It is not required for everyone.
How clinicians think about “severity”:
- Valve leakage and chamber size: More leakage typically means more right atrial enlargement and a higher chance of symptoms over time.
- Right ventricular performance: A smaller or weaker functional right ventricle may limit exercise capacity and raise the need for tailored surgical approaches.
- Presence of shunts and oxygen levels: If blood mixing causes low oxygen, decisions about closure or timing of repair become more urgent and nuanced.
- Arrhythmia burden: Frequent or dangerous rhythm episodes can drive treatment even when valve leakage is moderate.
- Trend over time: A stable echo for years suggests a different strategy than steady enlargement, worsening leakage, or declining exercise tolerance.
One of the most valuable outputs of the diagnostic phase is a clear, plain-language summary you can repeat back:
- How severe is the valve leak?
- How well is the right ventricle working?
- Is there an atrial-level opening or low oxygen issue?
- Are arrhythmias present or likely?
- What is the follow-up schedule and the trigger for escalation?
That summary turns a complex diagnosis into an actionable care plan.
Treatment options and what to expect
Treatment is individualized. Some people need careful observation only. Others benefit from rhythm control, valve repair, or—rarely—single-ventricle style palliation when the right ventricle cannot support normal circulation.
1) Observation and follow-up (common in mild cases)
If symptoms are minimal and heart size/function are stable, clinicians often recommend:
- Regular cardiology visits (often yearly or every 1–2 years, depending on findings)
- Periodic echocardiograms to track valve leakage and chamber size
- Rhythm monitoring if palpitations occur
2) Medications (symptom control, not a “cure”)
Medication choices depend on the main issue:
- Diuretics (water pills) can reduce swelling and congestion in right-sided heart failure symptoms.
- Rate or rhythm medicines may help control rapid heart rhythms or prevent recurrence in selected patients.
- Anticoagulation (blood thinners) may be recommended for certain arrhythmias or clot-risk profiles, especially if atrial fibrillation occurs.
3) Catheter-based rhythm procedures
If an accessory pathway or specific rhythm circuit is identified, catheter ablation can be considered. This involves threading thin tubes through the veins to the heart to map and treat abnormal electrical tissue. In Ebstein anomaly, ablation can be more complex because anatomy is altered, but it can be highly effective in experienced centers.
4) Surgery for the tricuspid valve and associated lesions
Surgical decisions often revolve around timing: intervene early enough to prevent irreversible right ventricular remodeling, but not so early that benefits are uncertain. The modern “workhorse” approach in many centers is cone reconstruction, a repair technique that reshapes the leaflets into a more functional valve. Depending on anatomy and age, options may include:
- Tricuspid valve repair (often preferred when feasible)
- Tricuspid valve replacement (selected cases)
- Closure of atrial-level defects, sometimes with a strategy that allows pressure relief when needed
- Additional procedures to address right ventricular size, rhythm, or blood flow patterns
5) Neonatal and infant management (severe cases)
Severely affected newborns may need intensive support for oxygenation and circulation, and sometimes staged surgical approaches. Decisions can include stabilizing blood flow pathways, managing pulmonary blood flow, and choosing between biventricular repair strategies versus palliation. These choices are highly specialized and depend on oxygen levels, right ventricular capacity, and overall stability.
What to expect emotionally and practically:
- Treatment planning often takes multiple visits and imaging steps.
- Outcomes are best when managed at centers familiar with congenital heart disease across the lifespan.
- Rhythm issues and valve issues are tightly linked; a good plan addresses both.
A clear treatment plan should specify not only “what,” but “why now,” and what markers (symptoms, chamber size changes, oxygen level shifts) would change the timeline.
Long-term management and when to seek care
Long-term management is about protecting heart function, preventing avoidable complications, and making life predictable—even with a diagnosis that can feel uncertain at first.
Routine care that makes the biggest difference
- Structured follow-up: Keep the recommended schedule even if you feel well. Ebstein anomaly can change gradually, and early detection of chamber enlargement or worsening leakage can widen treatment options.
- Rhythm vigilance: Track episodes of rapid heartbeat—how long they last, what triggers them, and whether you feel dizzy or faint. If symptoms are intermittent, ask about extended monitoring rather than relying on a single in-office ECG.
- Exercise with guardrails: Many people can stay active. The safest approach is individualized: aim for steady aerobic activity and strength training appropriate to your symptoms and clinician guidance, while avoiding “push through” training that provokes dizziness, chest pain, or sustained palpitations.
- Infection and dental planning: Ask your clinician whether you need antibiotics before certain dental procedures. Recommendations depend on your specific anatomy and prior surgeries.
Pregnancy and family planning
Pregnancy increases blood volume and heart workload. Many women with mild-to-moderate disease do well, but planning matters:
- Get a pre-pregnancy evaluation of valve leakage, right ventricular function, oxygen levels, and arrhythmia history.
- Coordinate care with a team experienced in adult congenital heart disease and high-risk obstetrics when needed.
- Have a plan for palpitations, swelling, and blood pressure changes, and know which symptoms require urgent assessment.
Preventing avoidable triggers
- Stay well hydrated, especially during illness or heat.
- Avoid stimulant-heavy supplements and unregulated “pre-workout” mixes.
- Treat fever and respiratory infections promptly, especially if they worsen breathing or provoke palpitations.
- If you take diuretics or rhythm medications, review electrolyte monitoring and side effects periodically.
When to seek urgent care
Seek same-day or emergency evaluation if you have:
- Fainting without warning, especially with palpitations
- Rapid heartbeat that lasts more than 15–20 minutes or causes chest pain, severe shortness of breath, or near-fainting
- New or worsening cyanosis at rest
- Rapid swelling, sudden weight gain over a few days, or new abdominal distension
- In infants: poor feeding, persistent fast breathing, blue color, or unusual sleepiness
Original, practical tip: build a one-page “heart snapshot.”
Keep a simple document with your key details: most recent echo findings (leak severity, right ventricle function), known rhythm diagnosis, surgeries/ablations, current medications with doses, and your cardiologist’s contact plan. In urgent settings, that single page can prevent delays and repeated testing.
With consistent follow-up and the right timing of intervention when needed, many people with Ebstein anomaly can plan school, careers, pregnancy, and exercise with confidence rather than constant uncertainty.
References
- 2025 ACC/AHA/HRS/ISACHD/SCAI Guideline for the Management of Adults With Congenital Heart Disease: A Report of the American College of Cardiology/American Heart Association Joint Committee on Clinical Practice Guidelines – PubMed 2025 (Guideline)
- The American Association for Thoracic Surgery (AATS) 2024 expert consensus document: Management of neonates and infants with Ebstein anomaly – PubMed 2024 (Guideline/Consensus)
- Narrative review of Ebstein’s anomaly beyond childhood: Imaging, surgery, and future perspectives – PubMed 2021 (Review)
- Ebstein’s Anomaly: Review of Arrhythmia Types and Morphogenesis of the Anomaly – PubMed 2021 (Review)
Disclaimer
This article is for general education and does not replace personalized medical advice, diagnosis, or treatment. Ebstein anomaly ranges from mild to severe, and the right plan depends on your valve anatomy, heart function, oxygen levels, rhythm history, age, and pregnancy plans. If you have fainting, sustained rapid heartbeat, new bluish discoloration, chest pain with shortness of breath, or severe weakness—seek urgent medical care. Always discuss new symptoms, medication changes, supplements, and exercise limits with a qualified clinician, ideally one experienced in congenital heart disease.
If this article helped you, please share it on Facebook, X (formerly Twitter), or any platform you prefer, and follow us on social media. Your support through sharing helps our team continue producing clear, trustworthy health content.