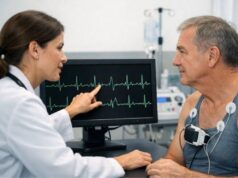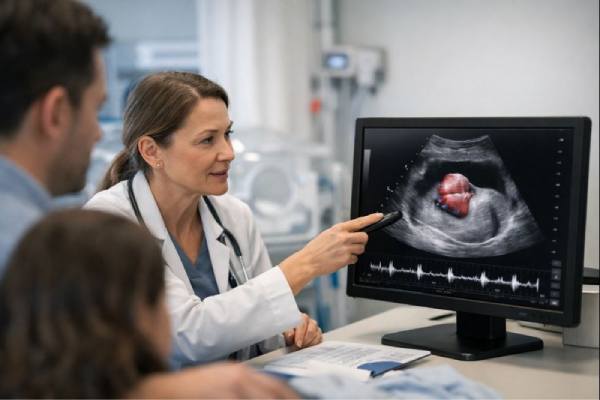
Ectopia cordis is a very rare condition present at birth in which a baby’s heart is located partly or completely outside the chest. The opening can be through the breastbone area or, less often, higher in the neck or lower toward the abdomen. Because the heart may be exposed and other organs may also be affected, ectopia cordis is a medical emergency at delivery and usually requires immediate, highly specialized care.
Families often meet this diagnosis in the most stressful way—during a prenatal scan or moments after birth. The questions are urgent and practical: What else is wrong? Can the heart be protected? Is surgery possible, and what is the outlook? This article explains what ectopia cordis is, why it happens, how it’s diagnosed, what treatment can look like in different severities, and how families can plan care with clarity and support.
Table of Contents
- What is ectopia cordis and what types exist?
- What causes it and which risk factors matter?
- Symptoms and complications before and after birth
- How it’s diagnosed and what tests are needed
- Treatment options and what to expect in hospital
- Management, prognosis, and when to seek urgent help
What is ectopia cordis and what types exist?
Ectopia cordis means the heart is positioned outside its usual protective home in the chest. In a typical baby, the breastbone (sternum), ribs, and skin form a sturdy “box” over the heart. In ectopia cordis, that front wall does not form fully, leaving the heart partially or completely outside the thoracic cavity. The heart may be covered by a thin membrane, or it may be exposed with little protection. This exposure matters because it increases the risk of dehydration of tissues, heat loss, bleeding, infection, and direct injury—especially during and after delivery.
Clinicians often describe ectopia cordis by location:
- Thoracic ectopia cordis: The heart sits outside the chest through a defect in the sternum. This is the most common type.
- Cervical ectopia cordis: The heart is positioned higher toward the neck. It is uncommon and often severe because the blood vessels and airway region are crowded.
- Thoracoabdominal ectopia cordis: The heart lies partly outside the chest and partly toward the upper abdomen, often with a larger midline defect.
- Abdominal ectopia cordis: Rarely, the heart may be located lower, associated with abdominal wall abnormalities.
Ectopia cordis is frequently linked with other midline defects, especially a group of findings called pentalogy of Cantrell (a set of chest and abdominal midline defects). Many babies also have structural heart differences inside the heart itself, such as holes between chambers or abnormal outflow pathways.
It helps to separate two problems that occur together:
- The chest-wall opening (where the heart is located and how well it is protected).
- The internal heart anatomy (how the heart is built and how well it can pump).
A baby may have a large opening but relatively simpler internal heart anatomy, or the opposite. Treatment planning depends on both.
Because this condition is so rare, care is usually concentrated in specialized centers that manage complex congenital heart disease, neonatal intensive care, and pediatric surgery. The first goal is always the same: protect the heart safely, stabilize breathing and circulation, and define the full anatomy so the team can decide what is realistically repairable.
What causes it and which risk factors matter?
Ectopia cordis develops very early in pregnancy, during the weeks when the baby’s chest wall, diaphragm, and heart structures are forming and closing along the midline. The most accepted explanation is a disruption in how the front body wall fuses. If that closure is incomplete, the sternum and nearby tissues may not protect the heart, leaving it outside the chest cavity.
In most cases, there is no single, identifiable cause. Families often ask, “Did I do something wrong?” The honest answer is that ectopia cordis is typically not caused by anything a parent did or didn’t do. It appears to be a rare developmental event that can occur even in otherwise healthy pregnancies.
That said, clinicians still evaluate risk factors and associations because they can guide counseling and testing:
- Mostly sporadic occurrence: Most families have no prior history of ectopia cordis.
- Possible genetic contribution in some cases: Ectopia cordis can appear alongside chromosomal differences or broader syndromes, especially when multiple organs are affected. This is why prenatal genetic testing is often discussed after diagnosis.
- Association with midline defect patterns: When ectopia cordis occurs with abdominal wall defects, diaphragmatic defects, and pericardial defects, it may fit a recognized pattern (such as pentalogy of Cantrell). The pattern can help predict surgical complexity and survival chances.
- Co-occurring structural heart defects: Many babies have internal heart malformations in addition to the external position. These are not “risk factors,” but they strongly shape prognosis and treatment options.
- Environmental exposures: For ectopia cordis specifically, clear exposure-based causes are not well established the way they are for some other birth defects. However, prenatal teams still review medications, infections, and medical conditions because overall fetal development can be affected by many factors.
One original, practical insight: families often focus on “cause,” but the more actionable question is “configuration.” Two babies can share the same diagnosis and have very different paths depending on:
- Whether the heart is fully exposed or covered by a membrane
- Whether the lungs have enough space to develop and expand
- Whether the internal heart has one repairable defect or several complex ones
- Whether there are additional major anomalies (brain, kidneys, abdominal organs)
When ectopia cordis is diagnosed prenatally, counseling is most helpful when it is specific and visual: a clear map of what is outside the body, what is inside the heart, and what else is affected. That map is what guides delivery planning and determines whether the goal is surgical repair, staged repair over time, or comfort-focused care.
Symptoms and complications before and after birth
Ectopia cordis is often identified before birth on ultrasound, sometimes as early as the first trimester in experienced hands, but more commonly during the mid-pregnancy anatomy scan. Before birth, the “symptom” is usually the imaging finding itself. The pregnant parent typically feels no different, which can make the diagnosis feel sudden and unreal.
Before birth, possible associated findings may include:
- Visible heart positioned outside the chest on ultrasound
- An abdominal wall defect (such as an omphalocele) or a large midline opening
- Signs of fluid overload in the fetus (hydrops), which can suggest heart strain
- Abnormal heart structure on fetal echocardiography (a detailed fetal heart scan)
At birth, ectopia cordis can cause urgent problems because the heart is not protected. The baby may have:
- Breathing distress (from small lungs, chest-wall instability, or associated anomalies)
- Low oxygen levels if the heart structure or circulation is complex
- Low blood pressure or poor circulation if the heart cannot pump effectively
- Heat loss and fluid loss from exposed tissues
- Higher infection risk over time if tissues are exposed or fragile
Complications depend heavily on severity and associated anomalies, but common concerns include:
- Tissue injury and bleeding: An exposed heart is vulnerable during handling and transport. Even minor pressure can be dangerous.
- Infection (sepsis): Open defects and prolonged intensive care increase infection risk, especially if repair requires staged procedures.
- Cardiac instability: Rhythm disturbances and reduced pumping effectiveness can occur, particularly when internal defects are complex.
- Limited space for the heart and lungs: Even if surgeons can reposition the heart, the chest cavity may be too small to close safely without compressing the heart or limiting lung expansion.
- Feeding and growth challenges: Babies who survive the initial period may need long-term nutritional support due to high energy needs and prolonged recovery.
A key point for families: many urgent issues are not “heart problems” alone—they are “protection and space” problems. The baby needs a safe covering for the heart and a strategy that avoids compressing the heart and lungs. That is why early care often focuses on stabilization and protection first, then careful planning for reconstruction.
If ectopia cordis is diagnosed prenatally, the most important “symptom management” is actually delivery planning: choosing a center that can provide neonatal resuscitation, pediatric cardiac evaluation, surgical teams, and immediate protective measures. Where and how the baby is delivered can change what options are available in the first critical hours.
How it’s diagnosed and what tests are needed
Diagnosis is usually straightforward once imaging shows the heart outside the chest, but the essential next step is defining the full anatomy. Ectopia cordis is rarely an isolated issue, and treatment decisions depend on details that standard ultrasound alone may not fully answer.
Prenatal diagnosis typically includes:
- Detailed obstetric ultrasound: Confirms location and extent of the defect and looks for associated abdominal wall, diaphragm, and sternum abnormalities.
- Fetal echocardiography: A specialized ultrasound that maps internal heart anatomy, blood flow direction, valve function, and major vessel connections.
- Fetal MRI (selected cases): Helps clarify relationships between the heart, chest cavity, abdominal organs, and lungs, especially when ultrasound views are limited. MRI can also support surgical and delivery planning by showing “space constraints” in more detail.
- Genetic testing options: Depending on associated findings, teams may discuss screening tests or diagnostic testing (such as chromosomal microarray). The goal is not blame; it is to understand whether a broader condition is present and to support accurate counseling.
After birth, urgent diagnostic steps often include:
- Physical assessment with strict protection: The baby’s heart and defect area must be protected while clinicians assess breathing and circulation. Gentle handling is crucial.
- Postnatal echocardiogram: Confirms internal heart defects and measures how well the heart is pumping in real-life circulation.
- Chest and abdominal imaging: Used to understand chest size, lung expansion, and the position of organs. The team may use X-ray and other imaging depending on stability.
- Laboratory testing: Assesses oxygenation, acid-base balance, infection markers, and organ function, which helps guide immediate intensive care decisions.
Clinicians also classify ectopia cordis severity using practical questions:
- Is the heart partially outside or completely outside?
- Is there any protective covering (skin or membrane), or is the heart fully exposed?
- How large is the chest cavity, and can it safely accommodate the heart if repositioned?
- Are there major associated anomalies (abdominal wall defect, diaphragmatic defect, complex intracardiac lesions)?
- How stable is the baby’s breathing and blood pressure?
One original, family-centered insight: ask the team to draw a simple “three-box diagram”:
- Outside (what structures are exposed)
- Border (what walls/diaphragm/sternum are missing)
- Inside (what the heart and organs look like internally)
That diagram keeps discussions anchored to reality and reduces the confusion that comes with unfamiliar medical language. It also helps families understand why some cases can proceed toward repair while others face limits that surgery cannot overcome safely.
Treatment options and what to expect in hospital
Treatment for ectopia cordis is highly individualized and usually occurs in stages. The immediate priorities are stabilization, protection of exposed tissues, and careful evaluation of what repair is possible. Because the condition is rare and complex, outcomes often depend on coordinated care between neonatology, pediatric cardiology, cardiac surgery, pediatric surgery, anesthesia, and nursing teams experienced in fragile congenital anomalies.
Immediate steps after birth often include:
- Protect the heart and exposed tissues: The team covers the area with sterile, moisture-retaining materials to prevent drying, heat loss, and injury.
- Support breathing and circulation: Many babies need oxygen and may require mechanical ventilation. Medications may be used to support blood pressure and heart function.
- Prevent infection: Strict sterile handling is essential. Antibiotics may be considered depending on exposure and surgical plans.
- Rapid imaging: Echocardiography and other imaging clarify internal defects and guide the next decision.
Surgical strategies depend on anatomy and stability. Common goals include:
- Providing safe coverage: If the heart is exposed, surgeons aim to protect it with available tissue or biocompatible materials when primary closure is not possible right away.
- Creating space without compression: Closing the chest too tightly can dangerously compress the heart and lungs. In many cases, gradual closure or staged reconstruction is safer than a single “complete closure.”
- Repairing internal heart defects (when feasible): Some intracardiac problems can be corrected in the same operation or later. Timing depends on stability and complexity.
- Addressing associated midline defects: If there is an abdominal wall defect or diaphragmatic defect, the team coordinates repairs to avoid worsening breathing or circulation.
Because space is often the limiting factor, many teams use a staged approach:
- Stage 1: Protect and stabilize, sometimes with temporary coverage and partial closure.
- Stage 2: Repositioning and reconstruction as the baby stabilizes and as the team determines what closure the chest can tolerate.
- Stage 3: Later repair of internal defects or additional reconstruction, if survival and stability allow.
When surgery cannot offer a realistic path to survival, care may shift toward comfort-focused goals. This is not “giving up.” It is a medically and ethically appropriate option when anatomy and physiology make meaningful recovery unlikely. Good teams communicate this clearly, involve palliative care early, and support families in making decisions aligned with their values.
What families can expect during hospitalization:
- Rapid decision-making in the first hours to days
- Frequent updates that may evolve as imaging clarifies anatomy
- Discussions about best-case, most-likely, and worst-case scenarios
- Emotional support needs that are as real as the medical ones
A practical tip: ask for one daily summary that answers three questions—“What changed today? What are we watching overnight? What decision is coming next?” That structure can make an overwhelming ICU experience more navigable.
Management, prognosis, and when to seek urgent help
Management and prognosis in ectopia cordis depend on a few powerful predictors: how exposed the heart is, whether the chest can be safely reconstructed, the severity of internal heart defects, and whether other major anomalies are present. Because the spectrum is wide, families deserve individualized, plain-language counseling rather than general statistics.
Prognosis (what families should understand clearly):
- Ectopia cordis is often life-threatening, especially when the heart is fully exposed and internal defects are complex.
- Survival is more likely when the heart is partially outside, has some protective covering, internal defects are repairable, and the chest cavity can be reconstructed without compressing the heart and lungs.
- Outcomes also depend on available resources—timely access to specialized surgery, neonatal intensive care, infection control, and long-term follow-up.
Long-term management for survivors can involve:
- Ongoing pediatric cardiology follow-up for heart function, valve performance, and rhythm monitoring
- Repeat surgeries for chest-wall reconstruction or internal heart defects
- Developmental and nutritional support, because prolonged ICU stays can affect feeding, growth, and motor development
- Care coordination across specialties, often through a congenital heart program
Family planning and future pregnancies:
Most cases are isolated and sporadic, but after one affected pregnancy, families often want a clear plan:
- Early targeted ultrasound in the next pregnancy
- Fetal echocardiography when appropriate
- Genetic counseling if there were multiple anomalies or a suspected chromosomal condition
Prevention:
There is no proven prevention strategy for ectopia cordis because the cause is usually not controllable. However, general preconception and pregnancy health measures still matter for overall fetal development:
- Review medications with clinicians before and during pregnancy
- Optimize chronic health conditions
- Attend recommended prenatal visits and screening
When to seek urgent help (prenatal and postnatal):
- During pregnancy: If ectopia cordis is suspected, urgent referral to a fetal medicine team is appropriate. Decisions about delivery location and timing should not be delayed.
- After birth: Any baby with ectopia cordis requires emergency-level neonatal care immediately. For survivors at home later, urgent evaluation is needed for:
- Breathing difficulty, persistent fast breathing, or bluish color
- Fever (because infection can escalate quickly)
- Poor feeding, repeated vomiting, or signs of dehydration
- Unusual sleepiness, limpness, or decreased responsiveness
An original, practical “continuity” tool: create a one-page care passport that includes diagnosis details, surgeries, current medications, baseline oxygen level if relevant, and direct contact instructions for the congenital heart team. In emergencies, that page can prevent dangerous delays and reduce repeated testing.
Finally, families deserve support that is not purely medical. Social work, mental health care, spiritual care (if desired), and palliative care teams can help parents make decisions, cope with uncertainty, and stay grounded—whether the goal is repair and survival or comfort and time together.
References
- Ectopia cordis: prenatal diagnosis, perinatal outcomes, and postnatal follow-up of an international multicenter cohort case series – PubMed 2023 (Multicenter Cohort Case Series)
- Prenatal diagnosis of fetal ectopia cordis by fetal cardiovascular magnetic resonance imaging – PubMed 2022 (Retrospective Study)
- Ectopia Cordis as a Lethal Neonatal Condition: A Case Report from Bahrain and a Literature Review – PubMed 2022 (Literature Review)
- Clinical and Surgical Perspectives on Isolated Thoracic Ectopia Cordis: A Rare Case Report – PubMed 2025 (Case Report)
- Surgical Repair of Ectopia Cordis in a Sub-Saharan African Country (Benin) – PubMed 2025 (Case Report)
Disclaimer
This article is for educational purposes only and does not provide medical advice, diagnosis, or treatment. Ectopia cordis is a rare, high-risk congenital condition that requires urgent evaluation and individualized care from a specialized medical team. If ectopia cordis is suspected during pregnancy, seek prompt referral to fetal medicine and pediatric cardiology. If a newborn has ectopia cordis or appears to have a heart or chest-wall defect, call emergency services immediately. Always follow the guidance of qualified clinicians who know the patient’s full medical situation.
If you found this article helpful, please share it on Facebook, X (formerly Twitter), or any platform you prefer, and follow us on social media. Your support through sharing helps our team continue producing clear, trustworthy health content.