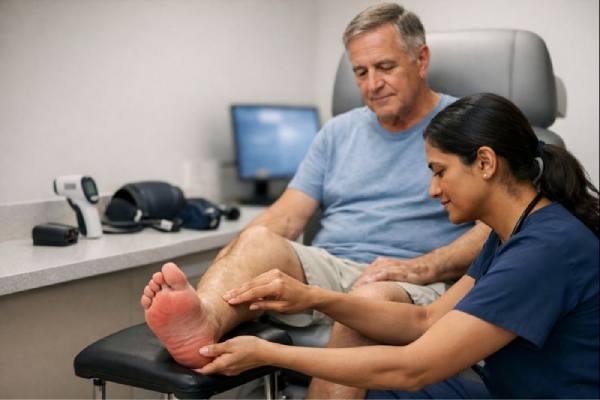
Erythromelalgia is a rare condition in which the feet, hands, or both develop episodes of burning pain, redness, and unusual warmth. Flares often arrive after heat, exercise, standing, tight shoes, or even a warm bed—then ease with cooling and elevation. Because symptoms can look dramatic and the pain can be intense, many people worry they are facing an infection, a circulation emergency, or a hidden nerve disorder.
The good news is that most patients can reduce flare frequency and severity once the pattern is recognized and triggers are mapped. The most important early step is separating “primary” erythromelalgia (often starting earlier in life) from secondary forms tied to another condition, such as a blood disorder or neuropathy. This guide explains what’s happening, what causes it, how doctors confirm it, and how to build a practical, safer plan for relief.
Table of Contents
- What erythromelalgia is and what happens in a flare
- Causes and risk factors: primary vs secondary
- Symptoms, patterns, triggers, and complications
- How erythromelalgia is diagnosed
- Treatments that can reduce pain and flares
- Daily management, prevention, and when to seek care
What erythromelalgia is and what happens in a flare
Erythromelalgia is defined by a classic trio: burning pain, redness, and heat in the affected skin—most often the feet, sometimes the hands, and occasionally the face or ears. Episodes tend to come and go. Many people can name a “switch” that flips symptoms on: a warm room, walking quickly, standing in line, stress, tight socks, or a hot shower. Relief usually follows cooling, rest, and elevation.
What’s happening under the surface
Erythromelalgia sits at the intersection of blood flow control and pain signaling:
- Blood vessel control is unstable. Small vessels may open too widely in the skin, creating warmth and redness. At the same time, the way blood is distributed can be inefficient—some flow may “shunt” through shortcuts instead of nourishing tiny capillaries well.
- Pain nerves become overly excitable. Many patients have features of small-fiber nerve dysfunction, which can amplify burning pain and make heat feel intolerable.
In primary erythromelalgia, nerve excitability can be driven by inherited changes in a sodium channel (often discussed in relation to the SCN9A gene). In secondary erythromelalgia, the same outward symptoms can be triggered by an underlying condition that affects blood viscosity, platelets, inflammation, or nerve health.
Why it can be mistaken for other problems
Erythromelalgia looks urgent because the skin can turn bright red or purple and feel hot. However, it behaves differently from common mimics:
- Unlike cellulitis, flares often appear quickly, vary by time of day, and improve with cooling rather than antibiotics.
- Unlike Raynaud phenomenon, which usually causes cold, pale, or bluish digits, erythromelalgia is heat-driven with redness and burning.
- Unlike a blood clot, symptoms are often symmetrical and episodic, not steadily worsening in one limb.
A practical hallmark is reproducibility: if warmth reliably triggers symptoms and cooling reliably helps, erythromelalgia moves higher on the list.
Still, the diagnosis should never be made casually. Clinicians need to rule out dangerous look-alikes and check for treatable secondary causes—especially blood disorders—because the treatment plan can change dramatically when a specific driver is found.
Causes and risk factors: primary vs secondary
Understanding the “why” behind erythromelalgia matters because it can turn a frustrating symptom condition into a treatable medical pathway. Clinicians usually sort causes into primary (often earlier onset, sometimes genetic) and secondary (linked to another condition or medication).
Primary erythromelalgia
Primary erythromelalgia often begins in childhood, adolescence, or early adulthood, though it can appear later. Clues include:
- Symptoms starting at a young age
- A family history of similar burning, heat-triggered flares
- Episodes that are strongly provoked by warmth and relieved by cooling
- Normal routine lab work early in the course
Some primary cases involve gain-of-function changes in sodium channels that make pain-sensing nerves fire too easily. This is why sodium-channel–blocking medicines sometimes help certain patients, while others do not respond.
Secondary erythromelalgia
Secondary erythromelalgia can begin at any age and is more likely when symptoms are new, progressive, or accompanied by other systemic signs. Common associations include:
- Myeloproliferative neoplasms (blood disorders that raise platelets or red blood cell mass), such as essential thrombocythemia or polycythemia vera. In this subgroup, symptoms may respond strongly to antiplatelet therapy and treatment of the blood disorder.
- Small fiber neuropathy, diabetes, thyroid disease, vitamin deficiencies, or autoimmune-related neuropathies.
- Autoimmune and inflammatory disorders, where dysregulated inflammation affects vessels and nerves.
- Medication-related triggers in susceptible individuals (the pattern and timing help guide suspicion).
Risk factors and “when to look harder”
The following features increase the likelihood of a secondary cause and justify a more expanded workup:
- Onset after age 40–50 with no prior history
- Rapid escalation in severity over weeks to months
- Asymmetrical or one-limb predominance that persists
- Unexplained weight loss, night sweats, persistent fever, or fatigue
- History of blood clots, frequent headaches, unusual bruising, or very high platelet counts
- Signs of neuropathy beyond flares (numbness, tingling, reduced sweating, dizziness on standing)
Why triggers still matter even when a cause exists
Even when erythromelalgia is secondary, triggers often remain the day-to-day “fuel” for flares. Heat exposure, prolonged standing, tight shoes, and stress can still amplify symptoms. That means a good plan usually has two layers:
- Treat the driver (for example, a blood disorder, neuropathy, or inflammation).
- Reduce the flare environment (temperature control, pacing, skin protection, safer cooling).
This two-layer approach helps patients avoid a common trap: chasing symptom relief without identifying a reversible cause—or, conversely, treating an underlying condition while ignoring the practical daily triggers that keep flares frequent and disabling.
Symptoms, patterns, triggers, and complications
Erythromelalgia is more than “hot feet.” The pain can be severe enough to disrupt sleep, limit walking, and push people toward risky cooling behaviors. Symptoms vary widely, even within the same person.
Typical symptoms
During a flare, people commonly describe:
- Burning, stinging, or “on fire” pain
- Red to deep purple discoloration
- Marked warmth to the touch
- Swelling or a tight, pressure-like sensation
- Sensitivity to light touch (socks or bedsheets can hurt)
Episodes can last minutes to hours. Many people notice a daily rhythm, with flares worsening in late afternoon or evening, especially after a day of standing or walking.
Common triggers and relief patterns
Triggers often include:
- Heat (warm rooms, summer weather, heated car seats)
- Exercise or brisk walking
- Prolonged standing or sitting with feet down
- Tight shoes, compression, or friction
- Alcohol, spicy foods, emotional stress, or a warm bed
Relief often comes from:
- Moving to a cooler environment
- Elevating the limb(s)
- Gentle airflow (fans)
- Brief cool water exposure (not ice-cold)
A helpful insight: many patients feel trapped between pain relief and skin safety. Overcooling can temporarily reduce pain but can also injure skin and worsen long-term outcomes.
Complications people do not expect
Complications can come from the condition itself and from coping behaviors:
- Skin damage from cooling: prolonged ice-water immersion can cause maceration (water-logged skin), fissures, infection, and in extreme cases tissue injury.
- Secondary infection: cracked or injured skin increases cellulitis risk, which then complicates the picture.
- Sleep deprivation: night flares can lead to chronic insomnia, worsening pain sensitivity and mood.
- Mood and anxiety symptoms: chronic severe pain increases the risk of depression and health anxiety; this is a medical consequence of persistent symptoms, not a personal failing.
- Reduced mobility and deconditioning: avoiding walking can weaken muscles and reduce circulation efficiency, making daily activity even harder.
Red flags that require prompt medical evaluation
Seek urgent assessment if you have:
- New fever, rapidly spreading redness, or pus (possible infection)
- Sudden one-sided swelling, pain, or discoloration that does not behave like prior flares
- New weakness, numbness, or inability to move the limb
- Blackening skin, open ulcers, or severe blistering
- Chest pain, shortness of breath, or neurologic symptoms (especially if a blood disorder is suspected)
A practical tracking tool
Because flares can vanish before an appointment, a simple record can be diagnostic:
- Photos during flares (same lighting when possible)
- Trigger, start time, end time, and peak severity (0–10 scale)
- Temperature and activity context (walking, standing, warm bed)
- Cooling method used and how long
- Any skin changes afterward (cracks, blisters)
Patterns in this diary help clinicians separate erythromelalgia from mimics and guide a plan that lowers flare intensity without causing skin injury.
How erythromelalgia is diagnosed
Diagnosis is clinical—based on symptoms and pattern—but it should be supported by careful exclusion of mimics and a targeted search for secondary causes. Many patients are misdiagnosed early because they are evaluated between flares, when the skin looks normal.
What clinicians look for first
A typical diagnostic pathway includes:
- A detailed history of the triad: burning pain, redness, and warmth
- Clear triggers (heat, exercise, standing) and consistent relief with cooling/elevation
- Distribution (feet, hands, or both; symmetry; whether symptoms spread)
- Time course (episodic vs constant; months/years vs sudden onset)
- Associated symptoms suggesting neuropathy (tingling, reduced sweating, light-touch pain)
Physical exam is useful even if a flare is not present. Clinicians check pulses, capillary refill, skin integrity, swelling patterns, and signs of neuropathy.
How to document a flare for diagnosis
Because flares can be intermittent, many clinicians encourage:
- Photographs or short videos during an episode
- A “trigger test” history (for example, symptoms after warm socks or exercise)
- A symptom diary, including cooling behaviors and skin effects afterward
This evidence can be more convincing than a normal exam in clinic.
Key conditions to rule out
The differential diagnosis often includes:
- Cellulitis or inflammatory skin disease
- Raynaud phenomenon and acrocyanosis
- Complex regional pain syndrome (especially after injury)
- Gout or inflammatory arthritis
- Peripheral artery disease (usually coldness, claudication, diminished pulses)
- Venous insufficiency or thrombosis (especially if one-sided and persistent)
These distinctions matter because treatments differ and some require urgent care.
Laboratory testing for secondary causes
A targeted workup often includes:
- Complete blood count (CBC) with platelet count to screen for myeloproliferative disorders
- Metabolic testing (glucose, kidney function)
- Thyroid testing when clinically indicated
- Vitamin levels (especially if neuropathy features exist)
- Additional tests for autoimmune disease when history suggests it
If a blood disorder is suspected, clinicians may pursue more specific hematology evaluation.
Neuropathy and genetics evaluation
When symptoms suggest small-fiber neuropathy or primary erythromelalgia, clinicians may consider:
- Skin biopsy for small-fiber nerve density (in selected cases)
- Autonomic testing in specialized centers
- Genetic testing when onset is early, family history is strong, or symptoms are severe and consistent with inherited patterns
A practical point: genetic testing can inform expectations about medication response in some patients, but it does not guarantee a “perfect match” treatment. Many people have erythromelalgia without an identifiable mutation.
The diagnosis becomes most useful when it leads to a tailored plan: identifying a treatable secondary cause, building a safer cooling strategy, and selecting therapies based on symptom drivers (neuropathic pain, vascular dysregulation, or platelet-mediated disease).
Treatments that can reduce pain and flares
Erythromelalgia treatment is often a stepwise process. No single medication works for everyone, and response can differ depending on whether the condition is primary, secondary, nerve-dominant, vascular-dominant, or platelet-mediated. The most effective plans combine trigger control with targeted therapies.
Start with the “must-not-miss” treatment: platelet-mediated disease
If erythromelalgia is linked to a myeloproliferative disorder (high platelets or related features), treatment can be dramatically different. Many patients in this category respond to antiplatelet therapy and treatment directed by hematology to control the underlying blood disorder. This is one reason a CBC is so important.
Topical therapies (often first-line)
Topicals can provide meaningful relief with fewer systemic side effects:
- Topical lidocaine (patches or compounded forms in selected cases)
- Compounded combinations used for neuropathic pain patterns (commonly discussed in relation to amitriptyline-ketamine mixtures)
- Cooling gels or barrier creams to reduce friction and protect compromised skin
Topicals are not “weak.” For patients with localized symptoms, they can reduce burning enough to improve sleep and mobility.
Systemic medications: matching drug to pattern
Common systemic options include:
- Neuropathic pain agents: gabapentin, pregabalin, duloxetine, or tricyclic antidepressants may help when burning pain and sensitivity dominate.
- Sodium channel blockers: mexiletine, carbamazepine, oxcarbazepine, or similar agents may help some primary cases, especially when nerve hyperexcitability is a key driver. These require careful medical supervision for safety and drug interactions.
- Vascular-modulating agents: in select patients, medications that affect microvascular tone or shunting have been used, though evidence varies and tolerability can limit use.
- Anti-inflammatory approaches: helpful when inflammation or autoimmune disease is part of the picture, guided by the underlying diagnosis rather than erythromelalgia alone.
A practical clinical reality is “trial with structure.” Because evidence is limited and responses vary, clinicians often use planned trials:
- one new therapy at a time,
- a defined duration (for example, several weeks unless side effects limit),
- a consistent flare diary to measure change.
Procedural and device-based options for refractory cases
When symptoms remain disabling despite optimized medical therapy, some patients explore procedural strategies through pain specialists. Options reported in the literature include:
- Sympathetic blocks or infusions
- Botulinum toxin injections in selected patterns
- Neuromodulation approaches such as spinal cord stimulation or dorsal root ganglion stimulation
These are not routine first steps. They are usually considered when quality of life is severely impaired, conservative measures have failed, and the patient is evaluated by a multidisciplinary team.
What to avoid
Many patients inadvertently worsen symptoms by “overcooling.” Prolonged ice-water immersion can injure skin and lead to infection, which then amplifies pain and flare frequency. Another common pitfall is starting multiple new treatments at once, making it impossible to know what helped or harmed.
The most successful treatment plans are realistic: reduce flare frequency, shorten flare duration, improve sleep, and protect skin integrity—while continuing to screen for and treat secondary drivers over time.
Daily management, prevention, and when to seek care
Daily management is where most improvement happens. Even when medications help, flares often remain sensitive to heat, standing, and friction. A practical plan protects skin, reduces triggers, and gives you safer tools for relief.
Safer cooling: relief without skin injury
Aim for cooling methods that reduce heat without damaging tissue:
- Use fans, cool air, or a cooling pack wrapped in cloth (never directly on skin for long periods).
- Prefer brief cool water exposure over prolonged soaking.
- Dry skin thoroughly afterward and apply a gentle moisturizer or barrier cream if cracking is an issue.
- Avoid sleeping with feet in cold water or against ice packs; this is a common path to maceration and infection.
A simple rule: if cooling causes numbness, whitening, or skin breakdown, it is too aggressive.
Trigger reduction that fits real life
Small changes often add up:
- Choose breathable shoes with a wider toe box; avoid tight socks and friction seams.
- Plan walking in shorter “intervals” rather than long continuous bouts, especially in warm settings.
- Keep the bedroom cool and use light bedding to reduce night flares.
- Reduce alcohol if it reliably triggers episodes.
- Consider temperature strategies before predictable triggers (warm commutes, crowded events, standing in lines).
Skin and foot care essentials
Because skin injury can turn a flare condition into a wound problem:
- Inspect feet and hands daily for cracks, blisters, or ulcers.
- Treat athlete’s foot and minor skin breaks early to reduce infection risk.
- Ask clinicians about wound-care support if sores develop or do not heal.
Movement without flare escalation
Avoiding all activity often backfires. Many people do better with a graded approach:
- Start with short, cool-environment walks.
- Add gentle strengthening (calf, foot, and hip muscles) to improve endurance.
- Increase duration slowly while tracking flare response.
This helps reduce deconditioning and improves confidence.
When to seek urgent care
Seek prompt medical evaluation if you have:
- Fever, rapidly spreading redness, pus, or worsening pain that does not match your typical flare pattern
- New one-sided swelling or discoloration that persists, especially with calf pain or shortness of breath
- Skin ulceration, blackened areas, severe blistering, or signs of tissue injury
- New neurologic symptoms (weakness, confusion) or chest pain
- New onset symptoms in midlife or later without a clear pattern, especially if CBC abnormalities are present
How to work with your clinician efficiently
Bring three items to appointments:
- Photos of flares
- A 2–4 week flare diary with triggers and cooling methods
- A medication and supplement list (including “pre-workout” products and vasodilating supplements)
Erythromelalgia is manageable, but it usually requires persistence and iteration. The best outcomes come from protecting skin, identifying secondary causes early, and building a plan that balances symptom relief with long-term safety.
References
- Comparative Efficacy and Tolerability of Treatments for Erythromelalgia: A Systematic Review 2025 (Systematic Review)
- Procedural interventions for erythromelalgia: A narrative review 2024 (Review)
- Erythromelalgia: A Review of Medical Management Options and Our Approach to Management 2023 (Review)
- SCN9A Neuropathic Pain Syndromes – GeneReviews® – NCBI Bookshelf 2020 (Clinical Review)
- The prostaglandin E1 analog misoprostol reduces symptoms and microvascular arteriovenous shunting in erythromelalgia-a double-blind, crossover, placebo-compared study 2004 (RCT)
Disclaimer
This article is for educational purposes only and does not provide medical advice, diagnosis, or treatment. Erythromelalgia can resemble conditions that require urgent care, including infection, blood clots, severe circulation problems, or acute inflammatory disorders. If you develop chest pain, sudden shortness of breath, new weakness or confusion, fever with rapidly spreading redness, severe one-sided swelling, blackened skin, open ulcers, or any sudden worsening that does not match your usual flare pattern, seek urgent medical attention immediately. For personalized evaluation and treatment, consult a licensed clinician who can assess your symptoms, examine you during or after flares, review medications, and check for underlying causes.
If you found this article helpful, please share it on Facebook, X (formerly Twitter), or any platform you prefer, and follow us on social media. Your support by sharing helps our team continue producing quality content.






