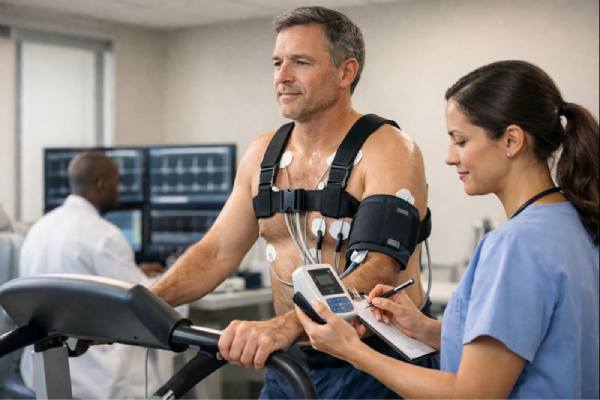
Exertional hypertension means your blood pressure rises higher than expected during physical activity, such as a treadmill test, cycling, or a hard climb up stairs. Some people feel fine and only discover it during a checkup. Others notice pounding in the chest, breathlessness, or a “too much, too soon” feeling when exercise gets intense. Either way, it can be an early clue that your arteries are stiffer than they should be, that you have hidden high blood pressure outside the clinic, or that your heart is working against more resistance than expected.
This does not mean you should avoid exercise. It means you should learn what your numbers are, why they might be elevated, and how to train and treat safely. A clear plan can protect long-term heart and brain health while keeping you active.
Table of Contents
- What exertional hypertension is
- Why it happens and who gets it
- Symptoms, red flags, and complications
- How it’s diagnosed and measured
- Treatment options that work
- Training, daily management, and when to seek care
What exertional hypertension is
Blood pressure normally rises during exercise. Your muscles need more blood flow, your heart pumps faster and harder, and the pressure in the arteries increases to deliver oxygen. Exertional hypertension describes a rise that is higher than expected for the workload or the person’s age, sex, and fitness level.
You may also hear the terms exaggerated blood pressure response to exercise or exercise hypertension. There is no single universal cutoff, which is one reason this topic can feel confusing. In many clinical settings, a peak exercise systolic (top number) around 210 mmHg for men or 190 mmHg for women during a standard treadmill test has been used as a flag for an exaggerated response, but protocols vary and those numbers are not “one size fits all.” Trained athletes can reach high peak pressures because they can sustain higher workloads, while some people show a steep rise early at modest effort, which can be more concerning.
A practical way to think about exertional hypertension is to look at three patterns:
- High at rest and higher with exercise: consistent with established hypertension that needs better control.
- Normal in the clinic, high during activity: may suggest masked hypertension (normal readings in a medical setting but high in daily life) or early artery stiffness.
- Steep rise early in exercise: blood pressure spikes at low-to-moderate workloads, sometimes linked to poor blood vessel relaxation, higher stress-hormone response, or untreated sleep apnea.
Why it matters is not the number alone, but what it can signal. Repeated high pressures during activity can reflect strain on the heart and arteries. Over time, that strain can contribute to thickening of the heart muscle, higher risk of developing sustained hypertension, and greater risk of cardiovascular events—especially when combined with other risk factors like smoking, diabetes, or high cholesterol.
At the same time, exercise is one of the most effective tools for lowering long-term blood pressure and improving vessel function. The goal is not to stop moving. The goal is to identify your pattern, confirm whether you have hidden hypertension, and match your training and treatment to your risk.
Why it happens and who gets it
Exertional hypertension usually comes from a mismatch between how much blood the heart pumps during exercise and how well the blood vessels can widen to accommodate that flow. When vessels do not relax enough, pressure rises higher for the same workload.
Common contributors include:
- Early or established hypertension: Some people have normal clinic readings but elevated pressures at home, at work, or during exercise. Exercise testing can “unmask” this pattern.
- Arterial stiffness: Healthy arteries expand with each heartbeat. Stiffer arteries act more like rigid pipes, so pressure climbs faster when flow increases.
- Overactive stress response: Higher sympathetic (fight-or-flight) activity can increase heart rate, tighten blood vessels, and raise pressure.
- Poor fitness or deconditioning: If everyday movement feels like high effort, the body reaches higher heart rates and pressures sooner.
- Excess body weight and insulin resistance: These can increase blood volume, raise vessel tone, and impair vessel relaxation.
- Sleep apnea: Repeated oxygen drops at night can keep stress hormones elevated and raise daytime pressures, including during exercise.
- High sodium intake and low potassium intake: This can increase fluid retention and vascular tone in salt-sensitive individuals.
- Alcohol excess and stimulants: Heavy drinking, certain decongestants, energy products, and illicit stimulants can elevate exercise blood pressure.
- Kidney disease or endocrine causes: Less common, but important when blood pressure is severe, resistant, or appears at a young age.
Risk factors often overlap with standard hypertension risks:
- family history of hypertension or early cardiovascular disease
- age (risk rises over time)
- smoking or nicotine use
- high LDL cholesterol
- diabetes
- chronic stress and poor sleep
- sedentary lifestyle
A special note for athletes: a high peak blood pressure during maximal testing can sometimes reflect high performance rather than disease. What raises concern is a pattern such as a steep rise at moderate workloads, unusually high pressures compared with peers at similar workloads, or high readings outside training.
Exertional hypertension can also appear after a long break from exercise, during illness, dehydration, or extreme heat. These situational spikes matter, but the most useful information comes from repeated measurements and trends over time.
The most important next step, once exertional hypertension is suspected, is to determine whether it reflects hidden day-to-day hypertension, a reversible trigger (like sleep apnea or medications), or early vessel changes that benefit from targeted lifestyle and, sometimes, medication.
Symptoms, red flags, and complications
Many people with exertional hypertension have no symptoms. That is why it is often discovered during a treadmill test, a sports physical, or a routine fitness assessment.
When symptoms occur, they can be subtle and easy to dismiss, especially if you assume you are just “out of shape.” Possible symptoms include:
- pounding heartbeat, especially during intervals or hill climbs
- shortness of breath that feels out of proportion to effort
- headache during or soon after intense activity
- facial flushing, dizziness, or a “pressure” sensation in the head
- unusual fatigue or a sharp drop in performance compared with your baseline
These symptoms are not specific. They can also come from dehydration, low iron, asthma, anxiety, or overtraining. The differentiator is the pattern: symptoms that reliably track with rising intensity and coincide with high measured blood pressure deserve attention.
Potential complications depend on whether exertional hypertension is an early marker or part of established hypertension. Over time, repeated high pressures can contribute to:
- sustained hypertension: higher risk of developing consistently high resting blood pressure
- heart muscle thickening: the heart may enlarge or stiffen as it pumps against higher pressure
- vascular damage: chronic high pressure can injure artery walls, accelerating plaque formation
- higher stroke risk: especially if hypertension becomes sustained and untreated
- kidney strain: hypertension can worsen kidney function, and reduced kidney function can further raise blood pressure
Red flags that should prompt urgent medical evaluation include:
- chest pressure, tightness, or pain during activity
- fainting, near-fainting, or new severe dizziness
- severe shortness of breath at low effort or sudden breathing difficulty
- new neurologic symptoms (weakness, trouble speaking, vision changes)
- a severe “worst headache,” especially with high blood pressure readings
- blood pressure readings that are extremely high and do not come down with rest
If you already have known hypertension and notice a sudden change—your exercise tolerance drops, your readings are consistently higher than usual, or symptoms appear that were not present before—treat that as meaningful. It can signal medication issues, sleep disruption, kidney changes, stimulant exposure, or progression of underlying cardiovascular risk.
The reassuring point is that most people improve with a structured approach: confirm the pattern, address reversible causes, and use training and treatment that lower pressure over time rather than provoking repeated spikes.
How it’s diagnosed and measured
Diagnosis hinges on measurement quality. A single high reading during a stressful test is less informative than a consistent pattern across properly measured sessions.
Clinicians typically start by clarifying:
- what exercise you were doing, at what intensity, and for how long
- whether symptoms occurred and when
- your resting blood pressure history and family history
- medications, supplements, caffeine, nicotine, and decongestant use
- sleep quality and snoring (a clue for sleep apnea)
- training status and recent illness or weight change
Common tools used to confirm exertional hypertension and rule out masked hypertension include:
- Standard treadmill or cycle stress testing: Blood pressure is measured at rest, during increasing workloads, and during recovery. The trend matters: early steep rise, very high peak, or slow recovery can each provide clues.
- Ambulatory blood pressure monitoring (24 hours): This is one of the best ways to detect masked hypertension. It shows daytime, nighttime, and activity-related blood pressure patterns.
- Home blood pressure monitoring: When done correctly, home readings can be highly useful. A typical plan is twice daily measurements for 5–7 days, discarding day one and averaging the rest.
- Exercise blood pressure checks in training: For some people, supervised measurement during a standardized workout (same bike resistance or treadmill pace) helps confirm real-world responses.
Clinicians also look for conditions that can drive high exercise pressures:
- basic blood tests for kidney function and electrolytes
- screening for diabetes and cholesterol risk
- evaluation for anemia if symptoms suggest it
- assessment for sleep apnea when history fits
- review of medication and supplement triggers
In some cases—especially if symptoms, abnormal ECG findings, or high-risk factors are present—additional cardiovascular tests may be appropriate. The goal is to ensure that high blood pressure during exercise is not occurring alongside heart disease that needs separate treatment.
To get trustworthy numbers, measurement technique matters:
- use the correct cuff size
- keep the arm supported at heart level
- avoid talking during the reading
- allow a few minutes of quiet rest before baseline measurements
- repeat readings when a value is unexpectedly high
A helpful “next-step” question to ask after diagnosis is: is this likely an early marker (risk signal), masked hypertension (hidden condition), or uncontrolled established hypertension (treatment gap)? Each one leads to a slightly different plan.
Treatment options that work
Treatment focuses on two goals: lowering day-to-day blood pressure and improving how your vessels respond during activity. The best plan depends on whether you have normal resting blood pressure, masked hypertension, or confirmed hypertension.
Lifestyle interventions are first-line for most people and often produce meaningful changes within 8–12 weeks:
- Aerobic exercise (structured, consistent): Most people benefit from building toward about 150 minutes per week of moderate-intensity activity (or an equivalent mix), spread across the week. If you are new to training, start with shorter sessions (10–20 minutes) and build duration before intensity.
- Resistance training (smart dosing): Strength training supports blood pressure control, but technique matters. Use steady breathing, avoid breath-holding, and favor moderate loads with controlled repetitions. Very heavy lifts and straining can spike pressure.
- Weight management: Even modest weight loss can lower blood pressure and improve exercise responses, especially when combined with fitness gains.
- Diet pattern and sodium reduction: A DASH-style approach (fruits, vegetables, legumes, whole grains, low-fat dairy, nuts, and fewer processed foods) often helps. Many people benefit from lowering sodium and improving potassium intake through foods, if kidney function allows.
- Alcohol and nicotine: Reducing alcohol and stopping nicotine can lower blood pressure and improve vessel function.
- Sleep apnea treatment: Treating sleep apnea can reduce overall blood pressure and blunt excessive stress responses.
- Stress and recovery: Chronic stress, poor sleep, and overtraining can keep blood pressure elevated. Recovery is not optional; it is part of treatment.
Medication may be recommended when:
- resting blood pressure is consistently elevated
- ambulatory or home monitoring confirms masked hypertension
- there is evidence of heart muscle thickening or other target-organ effects
- lifestyle measures are not enough, or risk is high
Common medication classes include:
- ACE inhibitors or ARBs: often used for long-term protection, especially with diabetes, kidney disease, or heart changes
- calcium channel blockers: can reduce vascular tone and are useful in some exercise-related patterns
- thiazide-like diuretics: effective for many people, especially with salt sensitivity
- beta blockers: may be chosen when heart rate is high, anxiety-related surges are prominent, or there are specific heart indications; in some athletic contexts they can affect performance, so selection is individualized
If you exercise regularly, ask how your medication timing interacts with training. Some people do best taking certain medications away from peak training sessions to reduce dizziness, while others benefit from steadier coverage throughout the day. Do not adjust dosing without clinician guidance.
The best outcomes come from combining a clear exercise plan, home or ambulatory monitoring, and targeted therapy aimed at both resting and activity-related blood pressure patterns.
Training, daily management, and when to seek care
With exertional hypertension, daily management is about training in a way that improves vessel flexibility and lowers your baseline pressure—without repeatedly provoking extreme spikes.
A practical approach is to build a “blood-pressure-aware” training plan:
- Choose a safe intensity anchor. For most people, moderate intensity means you can speak in short sentences but not sing. Stay mostly in this range while building endurance.
- Warm up and cool down. Spend 5–10 minutes gradually increasing effort at the start, and 5–10 minutes easing down at the end. Sudden starts and stops can exaggerate pressure swings.
- Progress slowly. Increase weekly volume by small amounts (for example, 5–10% per week). Add intensity last.
- Limit strain-based spikes. Avoid breath-holding, “max effort” sets, and grinding repetitions. Exhale on exertion. Consider slightly lighter loads and more controlled reps.
- Watch recovery. Poor sleep, dehydration, and stress raise exercise blood pressure. Treat recovery as a training variable.
Monitoring makes the plan safer and more effective:
- Track home blood pressure trends (not single readings).
- Note when exercise feels unusually hard, and whether that matches higher readings.
- Recheck technique if readings change suddenly: cuff size, arm position, and timing matter.
A simple “day-of-exercise” checklist can prevent spikes:
- hydrate normally
- avoid heavy alcohol the night before
- be cautious with stimulants and decongestants
- do not train hard when sick or severely sleep-deprived
When to contact a clinician soon:
- home or ambulatory readings suggest masked or sustained hypertension
- your exercise threshold drops sharply (high readings at much lower effort)
- you develop frequent headaches, dizziness, or new breathlessness
- medication side effects interfere with training or daily function
When to seek urgent or emergency care:
- chest pain or pressure during activity
- fainting, near-fainting, or severe dizziness
- new neurologic symptoms (weakness, speech trouble, vision changes)
- severe shortness of breath at low effort
- very high readings with symptoms that do not settle with rest
Most importantly, avoid the trap of “all or nothing.” You do not need perfect numbers before you move. You need a plan that gradually improves your physiology, confirms whether hidden hypertension is present, and uses treatment that lowers long-term risk while keeping you active.
References
- 2023 ESH Guidelines for the management of arterial hypertension The Task Force for the management of arterial hypertension of the European Society of Hypertension: Endorsed by the International Society of Hypertension (ISH) and the European Renal Association (ERA) 2023 (Guideline)
- Blood Pressure Responses During Exercise: Physiological Correlates and Clinical Implications 2022 (Review)
- Clinical and Prognostic Value of Exaggerated Blood Pressure Response to Exercise 2023 (Review)
- Effects of aerobic exercise on blood pressure in patients with hypertension: a systematic review and dose-response meta-analysis of randomized trials 2024 (Systematic Review)
Disclaimer
This article is for educational purposes only and does not provide medical advice, diagnosis, or treatment. Blood pressure concerns can be serious, especially when paired with chest pain, fainting, severe shortness of breath, or neurologic symptoms. If you have alarming symptoms or very high readings that do not improve with rest, seek emergency care immediately. For personal guidance on exercise intensity, testing, and medication choices, consult a qualified clinician who knows your medical history.
If you found this article helpful, please share it on Facebook, X (formerly Twitter), or any platform you prefer, and follow us on social media. Your support through sharing helps our team continue producing clear, trustworthy health information.






