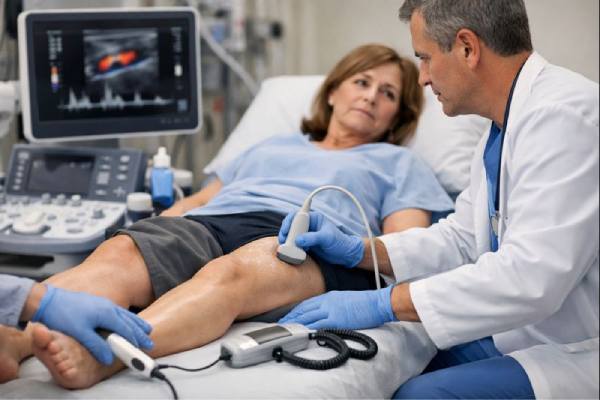
A femoral artery occlusion is a blockage in one of the main arteries that supplies blood to your leg. When that flow slows or stops, the muscles and skin downstream may not get enough oxygen, especially during walking or when resting. The change can be gradual, building over years, or sudden, happening in hours. The difference matters because a sudden blockage can threaten the limb if treatment is delayed. People often first notice calf or thigh pain with activity, a foot that feels unusually cold, or a sore that will not heal. This guide explains what femoral artery occlusion is, why it happens, how it feels, and what clinicians do to confirm and treat it—so you can recognize warning signs and understand the choices ahead.
Table of Contents
- What femoral artery occlusion means
- Why the femoral artery gets blocked
- Early symptoms and red-flag signs
- How doctors confirm the diagnosis
- Treatment options from medicines to surgery
- Recovery, prevention, and when to seek urgent care
What femoral artery occlusion means
The femoral artery is the large blood vessel that runs from the groin into the thigh and continues as the superficial femoral artery (SFA) toward the knee. A femoral artery occlusion means that blood flow through part of this pathway is blocked. The blockage can be partial (severe narrowing) or complete (no meaningful flow through that segment). In day-to-day practice, “femoral artery occlusion” often refers to an SFA blockage because that segment is a common site for plaque build-up.
What you feel depends on how fast the occlusion develops and how well your body can reroute blood through smaller side vessels (collaterals). Two patterns matter most:
- Chronic occlusion (gradual): Plaque slowly narrows the artery. Your body may build detours over time. Symptoms may start as exertional leg pain and gradually limit walking distance.
- Acute occlusion (sudden): A clot forms on a plaque (thrombosis) or travels from elsewhere (embolus) and blocks flow quickly. This can cause a rapid, painful loss of circulation and may become an emergency.
It also helps to separate leg symptoms from heart-and-brain risk. Femoral artery occlusion is a form of peripheral artery disease, and that usually means the same underlying process—atherosclerosis—may also affect coronary and carotid arteries. In other words, a leg blockage can be a warning sign for higher risk of heart attack and stroke, even if the leg symptoms feel “local.”
Clinicians often describe severity by how circulation behaves at rest and with activity:
- Intermittent claudication: predictable pain or cramping with walking that improves with rest.
- Chronic limb-threatening ischemia: persistent rest pain, ulcers, or gangrene from severely reduced blood flow.
- Acute limb ischemia: a sudden drop in perfusion that can threaten limb viability.
Understanding which bucket you fit into guides everything that follows—testing, urgency, and treatment goals.
Why the femoral artery gets blocked
Most femoral artery occlusions result from atherosclerosis, a long-term build-up of fatty plaque and scar tissue in the artery wall. Over time, plaque can narrow the channel, stiffen the vessel, and create a rough surface that encourages clot formation. In the SFA, bending and twisting with movement adds mechanical stress, which may help explain why this segment is prone to disease.
Common causes and contributors include:
Gradual blockage from plaque
- Smoking exposure: one of the strongest and most modifiable drivers of peripheral artery disease.
- Diabetes: accelerates plaque formation and impairs small-vessel circulation, wound healing, and nerve sensation.
- High LDL cholesterol and metabolic syndrome: promote plaque growth and inflammation.
- High blood pressure: damages artery lining over years.
- Kidney disease: increases vascular calcification and event risk.
- Age and male sex at birth: risk rises with age; patterns differ by sex and hormones, but both sexes are affected.
Sudden blockage on top of plaque
A chronic narrowing can abruptly become an acute occlusion when a clot forms at the diseased segment. Triggers include dehydration, acute illness, prolonged immobility, or stopping antithrombotic medications without medical guidance.
Embolus traveling into the femoral artery
A clot can form in the heart (for example, with atrial fibrillation) or inside an aneurysm and then lodge in the femoral artery. Embolic occlusions often produce a sudden onset of severe symptoms and may occur even without a long history of leg pain.
Less common causes
- Artery injury from procedures or trauma.
- Popliteal artery entrapment or external compression (more often affects younger athletes, usually lower in the leg).
- Vasculitis (inflammatory vessel disease) or rare clotting disorders.
A practical way to think about “why” is to ask two questions:
- Is the blockage chronic or sudden?
- Is it mostly plaque, mostly clot, or a combination?
Those answers shape the urgency and the best treatment approach.
Early symptoms and red-flag signs
Femoral artery occlusion can be quiet at first. Many people chalk early changes up to aging, back problems, or being “out of shape.” The most useful clue is a repeatable pattern—symptoms that show up with activity and ease with rest, or a sudden change that does not fit your usual baseline.
Typical symptoms of chronic occlusion
- Calf, thigh, or buttock pain with walking that improves within minutes of resting (intermittent claudication). With SFA disease, calf pain is especially common; thigh pain can also occur.
- Reduced walking distance: needing to stop sooner than you used to, especially on hills or stairs.
- Cooler skin temperature in one foot compared with the other.
- Weak or absent pulses in the groin, behind the knee, or at the ankle (often noticed by clinicians).
- Slow-healing cuts, blisters, or sores on toes, heel, or foot edges.
- Changes in skin and nails: shiny skin, hair loss on the lower leg, thickened toenails.
Symptoms suggesting severe or limb-threatening disease
- Rest pain: burning or aching in the foot at night that improves when you dangle the leg off the bed or stand up.
- Non-healing ulcers or blackened tissue (gangrene), especially in people with diabetes.
- New numbness or weakness that accompanies pain or coldness.
Red flags of acute limb ischemia
A sudden femoral occlusion can be an emergency. Seek urgent care immediately if you develop a rapid onset of:
- Severe leg pain (often out of proportion to what you see).
- Marked paleness or bluish discoloration of the foot.
- Cold, “dead” feeling in the lower leg or foot.
- New numbness or inability to move toes/ankle.
- No detectable pulse in the foot (if previously present).
Clinicians often summarize acute limb ischemia with “pain, pallor, pulselessness, paresthesia (tingling/numbness), paralysis, poikilothermia (cold).” You do not need all of these to be in danger. The key is sudden change—especially pain plus coldness, numbness, or weakness.
One more important nuance: people with diabetes or neuropathy may have less pain even when circulation is poor. In that situation, a new sore, spreading redness, drainage, or foul odor may be the first sign of trouble—and it deserves prompt assessment.
How doctors confirm the diagnosis
Diagnosis starts with a careful history and focused vascular exam. Clinicians listen for the story—where the pain is, what triggers it, and how quickly it resolves—then check pulses, skin temperature, color, capillary refill, and wounds. They also look for non-vascular mimics such as spinal stenosis, hip arthritis, nerve compression, or chronic venous disease.
Bedside tests that often come first
- Ankle-brachial index (ABI): compares ankle blood pressure to arm blood pressure. An ABI below normal supports peripheral artery disease. In long-standing diabetes or kidney disease, arteries may be stiff and falsely elevate ABI, so additional tests may be needed.
- Toe pressures or toe-brachial index: helpful when ABI is unreliable, and often more reflective of small-vessel perfusion to the foot.
- Handheld Doppler signals: assesses whether flow is present and the character of the signal (a quick triage tool, especially in urgent settings).
Imaging to locate and define the blockage
- Duplex ultrasound: usually the first imaging choice. It can show where blood flow accelerates (narrowing) or stops (occlusion), and it estimates severity without radiation or contrast dye.
- CT angiography (CTA): provides a detailed map of arteries from the aorta to the foot. It is useful for planning interventions but uses radiation and iodinated contrast.
- MR angiography (MRA): offers high-quality images and can sometimes reduce contrast risk, though availability and device compatibility matter.
- Catheter angiography: often done when an endovascular procedure is planned. It provides real-time detail and allows treatment in the same session, but it is invasive.
How clinicians decide urgency
The diagnostic pathway changes if acute limb ischemia is suspected. In that scenario, teams prioritize rapid clinical classification of limb viability and immediate vascular consultation. Imaging may be streamlined so treatment is not delayed.
In chronic disease, diagnosis also includes a broader health review because the leg is rarely the only issue. Expect assessment and management of:
- Blood pressure, cholesterol, diabetes control, kidney function
- Smoking status and cessation support
- Medication review (antiplatelet therapy, lipid-lowering therapy)
- Walking function and quality of life goals
A practical takeaway: good diagnosis is not just “Do you have an occlusion?” but “How severe is it, how urgent is it, and what is the safest path to restore function and prevent limb loss and cardiovascular events?”
Treatment options from medicines to surgery
Treatment has two parallel goals: protect life and vessels (reduce heart attack and stroke risk) and protect the leg (improve walking, heal wounds, prevent amputation). The right plan depends on symptom pattern, imaging, and overall health.
Foundational medical therapy for most patients
Even if you eventually need a procedure, medical therapy is the base layer:
- Antiplatelet medication: commonly used to reduce clot-related events in peripheral artery disease.
- Cholesterol lowering: high-intensity statin therapy is often recommended when tolerated; it stabilizes plaque and lowers cardiovascular risk.
- Blood pressure control and diabetes optimization: target ranges are individualized, but consistent control matters.
- Smoking cessation: often the single most powerful change for symptom progression and event risk.
- Structured exercise therapy: a supervised or structured walking program is one of the most effective treatments for improving claudication distance and daily function. Many programs use interval walking (walk until moderate symptoms, rest, repeat) several times per week.
For some patients with claudication, symptom-relief medications may be considered when appropriate and safe, alongside exercise and risk-factor treatment.
Endovascular treatments (minimally invasive)
These are performed through small catheters, usually from the groin:
- Balloon angioplasty: expands a narrowed segment.
- Stenting: props the artery open when recoil or dissection risk is high.
- Drug-coated balloons or drug-eluting stents: may reduce re-narrowing in selected lesions.
- Atherectomy: removes plaque in specific situations, often paired with other tools.
Endovascular therapy is commonly used for femoropopliteal disease, especially when anatomy is favorable and surgical risk is higher.
Surgical options
- Bypass surgery: creates a new route around the occlusion using a vein graft or synthetic conduit. It can be durable for extensive disease, especially in chronic limb-threatening ischemia or when endovascular options are limited.
- Endarterectomy: removes plaque from certain artery segments (more common in the groin region).
Acute occlusion: time-sensitive treatment
If the leg is suddenly threatened, treatment may include:
- Immediate anticoagulation (when appropriate) to prevent clot propagation.
- Catheter-directed thrombolysis: dissolves clot over hours to a day or more in selected patients.
- Mechanical thrombectomy or aspiration: removes clot through catheters.
- Open embolectomy or thrombectomy: surgical clot removal, sometimes paired with a patch repair or bypass if underlying plaque is severe.
Choosing among these is not one-size-fits-all; clinicians weigh bleeding risk, symptom duration, limb viability, clot location, and the likelihood of durable flow restoration.
Recovery, prevention, and when to seek urgent care
Recovery is not only what happens in the hospital or procedure suite. Long-term outcomes depend on habits, medication consistency, foot care, and follow-up—especially because peripheral artery disease tends to progress unless risks are controlled.
After diagnosis: what “good management” looks like
- A clear walking plan: many people do best with interval walking 3–5 days per week, gradually increasing total walking time. If supervised exercise therapy is available, it often provides faster, safer gains.
- Medication adherence: antiplatelet therapy and cholesterol-lowering therapy only work when taken consistently. If you have side effects, ask about alternatives rather than stopping abruptly.
- Risk-factor checkpoints: regular reviews of blood pressure, LDL cholesterol, and diabetes markers help keep the plan on track.
- Foot protection: especially important in diabetes.
- Inspect feet daily for blisters, cracks, redness, or drainage.
- Keep skin moisturized (but avoid soaking).
- Wear properly fitted shoes and clean socks.
- Treat fungal infections and nail problems early.
After an intervention: practical expectations
- You may still need exercise therapy. Restoring blood flow improves potential, but walking training builds function.
- Follow-up imaging or pulse checks may be scheduled to detect restenosis (re-narrowing) before symptoms return.
- Wound care can be slow. Ulcers may take weeks to months to heal even after flow improves, especially with diabetes or infection.
Prevention: changes that have outsized impact
- Stop smoking completely (including nicotine delivery products if advised), and ask for a structured cessation plan.
- Aim for heart-healthy eating patterns: higher fiber, fewer refined carbs, and saturated fat reduction can support lipid and glucose control.
- Move daily: beyond formal exercise sessions, reduce prolonged sitting with short walking breaks.
- Vaccination and infection management: infections can destabilize chronic vascular disease and trigger clotting risk.
When to seek urgent care
Go urgently (or call emergency services) if you develop:
- Sudden severe leg pain, coldness, numbness, weakness, or color change
- Rapidly worsening rest pain
- A foot wound with spreading redness, fever, foul drainage, or black tissue
- New inability to walk because of pain or weakness
If you already carry a diagnosis of femoral artery occlusion, treat a sudden symptom change as a new event until proven otherwise. Rapid assessment can be the difference between a straightforward procedure and permanent tissue loss.
References
- 2024 ACC/AHA/AACVPR/APMA/ABC/SCAI/SVM/SVN/SVS/SIR/VESS Guideline for the Management of Lower Extremity Peripheral Artery Disease: A Report of the American College of Cardiology/American Heart Association Joint Committee on Clinical Practice Guidelines 2024 (Guideline)
- 2024 ESC Guidelines for the management of peripheral arterial and aortic diseases 2024 (Guideline)
- Editor’s Choice — European Society for Vascular Surgery (ESVS) 2024 Clinical Practice Guidelines on the Management of Asymptomatic Lower Limb Peripheral Arterial Disease and Intermittent Claudication 2024 (Guideline)
- Treatment Strategies and Prognostic Outcomes in Acute Limb Ischemia: A Systematic Review and Meta-Analysis Comparing Thrombolytic Therapy and Open Surgical Interventions 2025 (Systematic Review)
Disclaimer
This article is for educational purposes only and does not replace medical advice, diagnosis, or treatment from a licensed clinician. Femoral artery occlusion can become an emergency—especially when symptoms start suddenly or rapidly worsen. If you have severe leg pain, a cold or numb foot, weakness, color change, or a wound that looks infected or turns black, seek urgent medical care immediately. Always discuss medications and treatment decisions with your healthcare team, particularly if you take blood thinners or have diabetes, kidney disease, or a history of bleeding.
If you found this article helpful, please consider sharing it on Facebook, X (formerly Twitter), or any platform you prefer, and follow us on social media. Your support through sharing helps our team keep producing high-quality health content.






