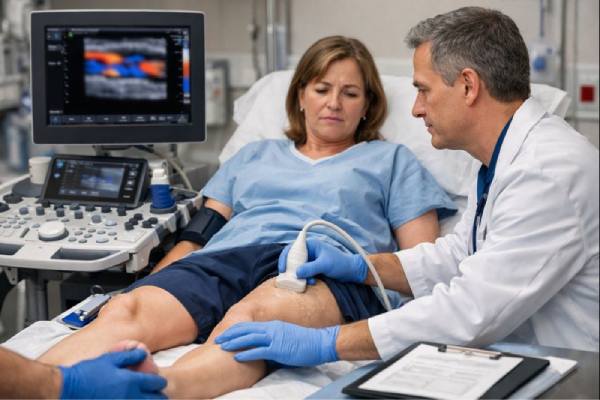
A clot in the femoral artery can turn an ordinary day into an emergency. The femoral artery is the main “highway” vessel that carries blood through the groin to the thigh and lower leg. When it becomes blocked by thrombosis (a blood clot inside a vessel), tissues downstream may be starved of oxygen. Sometimes the blockage develops slowly on top of long-standing artery narrowing; other times it forms suddenly, often after plaque rupture, a procedure, or dehydration and immobility. What matters most is timing: the sooner blood flow is restored, the better the chance of saving the limb and avoiding life-threatening complications. This guide explains what femoral artery thrombosis is, why it happens, how to recognize warning signs, what tests and treatments are commonly used, and how to reduce the risk of recurrence.
Table of Contents
- What is femoral artery thrombosis?
- Why does a clot form here?
- Early symptoms and danger signs
- How doctors confirm the diagnosis
- Treatment options and what to expect
- Recovery, prevention, and when to seek help
What is femoral artery thrombosis?
Femoral artery thrombosis means a blood clot forms inside the femoral artery and blocks blood flow to the leg. The femoral artery sits close to the skin crease of the groin, then continues down the thigh (as the superficial femoral artery) before becoming the popliteal artery behind the knee. Because it supplies a large territory, a blockage here can cause significant, fast-moving damage if not treated promptly.
A helpful way to understand this condition is to separate where the clot comes from:
- Thrombosis (in-situ clot): the clot forms right at the blockage site, usually on top of an already diseased artery. Plaque and calcium make the inner lining rough; blood tends to “catch” there, especially if flow slows.
- Embolism (traveling clot): a clot forms elsewhere (often the heart) and lodges in the femoral artery. People use the word “thrombosis” loosely, but your doctors will try to distinguish these because the long-term prevention plan can differ.
Femoral artery thrombosis can also be described by speed and context:
- Acute limb ischemia: sudden drop in blood flow over hours to days. This is the most urgent scenario.
- Acute-on-chronic ischemia: a sudden clot forms on top of a long-standing narrowing. Some people had calf pain when walking for months, then abruptly develop severe rest pain or numbness.
- Subacute or chronic occlusion: the artery closes gradually and the body sometimes grows small “detour” vessels (collaterals). Symptoms may be milder, but the risk of ulcers and tissue loss rises over time.
Why it matters: tissue can tolerate reduced blood flow only for so long. Nerves and muscles are particularly sensitive. If the limb becomes severely deprived of oxygen, the goal shifts from symptom relief to limb salvage—and sometimes to protecting life. That is why any sudden, severe leg symptoms should be treated as time-sensitive until proven otherwise.
Why does a clot form here?
A clot forms when blood flow, vessel lining, and clotting tendency combine in the wrong way. In practical terms, femoral artery thrombosis most often happens due to local artery disease plus a trigger.
Common underlying causes include:
- Atherosclerosis (plaque buildup): fatty, calcified plaque narrows the artery and disrupts the smooth lining. This is the most frequent setting for in-situ thrombosis.
- Prior artery repair or devices: stents, bypass grafts, or prior angioplasty can develop re-narrowing, turbulent flow, or device-related clotting, especially if antiplatelet therapy is interrupted.
- Aneurysm with clot: a bulging artery segment can encourage clot formation, which may extend or break off.
- Inflammation or injury of the vessel wall: less common, but vasculitis, radiation damage, or trauma can promote thrombosis.
Key risk factors that raise the odds of plaque, clotting, or both:
- Smoking (current or past), which damages vessel lining and accelerates plaque.
- Diabetes, linked to more diffuse plaque and smaller-vessel disease below the knee.
- High blood pressure and high LDL cholesterol, which speed plaque growth.
- Kidney disease, associated with calcification and higher cardiovascular risk.
- Older age and male sex (though women are often underdiagnosed and may present later).
- History of peripheral artery disease, heart attack, or stroke.
- Atrial fibrillation or recent heart injury (more relevant when the issue is an embolus, but still essential to check).
Triggers that can tip a narrowed artery into a sudden clot include:
- Dehydration or low blood volume (vomiting, diarrhea, poor intake).
- Prolonged immobility (long travel, illness, recovery after surgery).
- Stopping antiplatelet or anticoagulant medicines without a clear plan.
- Acute infection or inflammation, which can increase clotting tendency.
- Recent vascular procedure in the groin or thigh (catheter access can irritate the artery).
In younger patients or those without obvious plaque, clinicians may also consider inherited or acquired clotting disorders, hormone therapy, pregnancy-related risks, or rare anatomical problems. The important takeaway is that the clot is often the final event in a longer story—so preventing recurrence usually means treating both the clot and the conditions that allowed it to form.
Early symptoms and danger signs
Femoral artery thrombosis can range from uncomfortable to immediately limb-threatening. Symptoms depend on how fast the blockage occurs, where it sits, and whether collateral vessels can compensate.
Sudden symptoms (hours to a day) should be treated as an emergency. Classic warning signs are sometimes taught as the “6 Ps,” but many people have only a few of them. Watch for:
- Pain: sudden severe leg pain, often below the blockage; pain at rest is particularly concerning.
- Pallor: the leg or foot looks unusually pale or “waxy.”
- Pulselessness: a person may notice a missing pulse at the ankle, or clinicians may not detect it with Doppler.
- Paresthesia: new numbness, tingling, or “pins and needles.”
- Poikilothermia: the foot feels markedly colder than the other side.
- Paralysis/weakness: trouble moving the foot or toes—this is a late, high-risk sign.
Other important clues include:
- Color changes that evolve: pale → bluish/purple mottling can signal worsening tissue distress.
- Skin sensitivity and severe tenderness: can appear as nerves become oxygen-starved.
- New sores or blackened areas: suggests advanced ischemia or tissue death.
- Sudden worsening of known walking pain (claudication): especially if it progresses to pain at rest.
Complications can be serious even after blood flow is restored:
- Reperfusion injury: when oxygen returns to deprived tissue, swelling and inflammation can worsen pain and damage.
- Compartment syndrome: pressure builds inside muscle compartments, causing escalating pain (often out of proportion), tight swelling, pain with toe movement, numbness, and weakness. This can require urgent surgical release.
- Kidney strain from muscle breakdown: severe ischemia can cause muscle injury that releases proteins into the blood, sometimes stressing the kidneys.
A practical self-check if symptoms are new and one-sided:
- Compare temperature with the other foot.
- Look for sudden color differences.
- Pay attention to new numbness or weakness.
- Note whether pain persists at rest and does not improve with repositioning.
If pain is sudden and severe, the foot becomes cold or numb, or weakness appears, do not “watch it overnight.” In acute ischemia, delays can mean the difference between full recovery and permanent damage.
How doctors confirm the diagnosis
Diagnosis aims to answer three urgent questions: Is blood flow critically reduced? Where is the blockage? How threatened is the limb right now? The process often begins at the bedside and moves quickly to imaging.
1) Focused history and examination
Clinicians ask about the onset (sudden vs gradual), prior walking pain, recent procedures, medication changes, dehydration, and heart rhythm history. The exam checks:
- Skin color and temperature
- Capillary refill in the toes
- Sensation (light touch) and motor strength
- Tenderness and swelling
- Pulses in the groin, knee, ankle, and foot (with hands and Doppler)
This exam also helps classify severity (often using a “limb viability” framework). The presence of numbness and weakness signals higher urgency.
2) Bedside blood flow assessment
Common tests include:
- Ankle-brachial index (ABI): compares blood pressure at the ankle to the arm. A very low ABI supports major flow reduction, though severe calcification can make readings unreliable.
- Toe pressures or toe-brachial index: useful when ankle arteries are stiff from calcification (common in diabetes and kidney disease).
- Handheld Doppler signals: a quick way to detect whether any blood is moving past the blockage.
3) Imaging to locate the clot
The choice depends on speed, kidney function, and local resources.
- Duplex ultrasound: often the first imaging test. It can show absent flow, measure severity, and identify a clot versus tight narrowing.
- CT angiography (CTA): fast and detailed; maps the arterial tree and helps plan a procedure. It is commonly used when urgent intervention is likely.
- MR angiography (MRA): an alternative when CTA contrast is not suitable, though it can take longer.
- Catheter angiography: performed in a procedure suite; it can diagnose and treat in the same session (for example, guiding thrombolysis or thrombectomy).
4) Testing for the source and contributing factors
Because treatment and prevention differ, teams often evaluate for:
- Heart rhythm problems (ECG for atrial fibrillation)
- Echocardiography if an embolic source is suspected
- Blood tests (kidney function, blood counts, clotting measures), especially before procedures
- Selected clotting-disorder workup in younger patients, recurrent events, or unusual presentations
A common and important step is separating embolism from in-situ thrombosis. A sudden event with little prior leg history plus a heart rhythm issue points toward embolism; a history of calf pain with walking, diabetes, or known plaque points toward thrombosis on chronic disease. Sometimes it is mixed, and the safest approach is to treat urgently while clarifying the cause during or after stabilization.
Treatment options and what to expect
Treatment depends on how threatened the limb is and what caused the blockage. In acute cases, the first priority is preventing the clot from extending and restoring blood flow quickly.
Immediate steps (often started right away)
- Urgent vascular evaluation: acute limb ischemia is typically treated as a time-critical emergency.
- Anticoagulation: many patients receive intravenous anticoagulation early (commonly unfractionated heparin) unless there is a strong reason not to, such as active major bleeding.
- Pain control and limb protection: keeping the limb at a neutral position (not elevated high), staying warm (without direct heat that can burn numb skin), and avoiding tight wraps.
Revascularization options (restoring blood flow)
The approach is individualized, but common strategies include:
- Catheter-directed thrombolysis
A thin catheter is placed into or near the clot, and a clot-dissolving medication is infused over hours. This can be especially helpful when:
- The clot is fresh
- The blockage involves a longer segment
- The limb is threatened but still has some sensation and movement
Risks include bleeding, which is why careful monitoring is required, sometimes in a higher-acuity unit.
- Mechanical thrombectomy or aspiration
Devices can physically remove or break up clot. These can be used alone or combined with limited thrombolysis (“pharmacomechanical” approaches). They may shorten treatment time and reduce drug dose in selected patients. - Balloon angioplasty and stenting
If the clot formed on top of a fixed narrowing, the team often treats the underlying problem by widening the artery and, in some cases, placing a stent to keep it open. This is common in femoropopliteal disease. - Open surgery
Surgical options may be preferred when ischemia is severe, symptoms are advanced, or endovascular methods are unlikely to work quickly enough. Examples include:
- Surgical thrombectomy (embolectomy-style removal): direct clot removal using a balloon catheter.
- Endarterectomy: removing plaque from the artery wall when disease is localized.
- Bypass surgery: rerouting blood around the blocked segment when disease is extensive.
What to expect after flow is restored
- Monitoring for reperfusion injury: swelling, rising pain, or changes in sensation.
- Checking for compartment syndrome: worsening pain with a tight, swollen calf or forearm-like firmness in the leg muscles requires urgent attention.
- Antithrombotic plan: most patients need ongoing antiplatelet therapy (and sometimes anticoagulation) based on the cause—plaque-driven thrombosis versus embolic disease.
- Aggressive risk-factor treatment: cholesterol lowering, blood pressure control, diabetes management, and smoking cessation are not “extras”—they are core to preventing recurrence.
Recovery timelines vary. Some people walk within days; others need longer rehabilitation, wound care, or repeat procedures. The most reliable predictor of a smoother course is early treatment before nerve and muscle injury occurs.
Recovery, prevention, and when to seek help
After femoral artery thrombosis, prevention is not a single pill—it is a coordinated plan that lowers clot risk and protects the artery long-term. Think in three layers: medications, lifestyle, and follow-up surveillance.
1) Medications (your clinician tailors these)
Many patients are treated with a combination of:
- Antiplatelet therapy to reduce clotting on plaque or stents.
- Cholesterol-lowering therapy (often a high-intensity statin), aimed at stabilizing plaque and lowering cardiovascular risk.
- Blood pressure and diabetes medications to reduce vessel damage over time.
- Anticoagulation when there is a clear clot-from-the-heart risk (such as atrial fibrillation) or certain clotting disorders.
Practical tips that reduce avoidable setbacks:
- Do not stop antiplatelet or anticoagulant medicines without a plan (even for dental work) unless instructed by your clinician.
- Ask what to do if you miss a dose.
- Report unusual bleeding, black stools, coughing blood, severe headaches, or sudden weakness immediately.
2) Lifestyle measures that change outcomes
These steps are not cosmetic—they influence walking ability, wound healing, and recurrence risk.
- Stop smoking: it is one of the strongest predictors of progression and repeat blockages. If you need support, nicotine replacement or prescription aids can improve success.
- Structured walking plan: supervised or structured walking (often several sessions per week) improves symptoms and builds collateral circulation over time.
- Heart-healthy eating pattern: focus on vegetables, legumes, fish, whole grains, and unsalted nuts; limit processed meats, sugary drinks, and highly refined snacks.
- Foot and skin care: inspect feet daily if you have diabetes or reduced sensation. Treat blisters early, wear well-fitting shoes, and seek care for any non-healing sore.
- Hydration and mobility during travel: stand and walk periodically on long trips, and avoid becoming dehydrated, especially if you have known peripheral artery disease.
3) Follow-up and surveillance
Follow-up often includes:
- Repeat pulse and Doppler checks
- ABI or toe pressure measurements
- Ultrasound surveillance after stents or bypass grafts (your team sets the schedule)
- Evaluation for heart rhythm issues if an embolic source is possible
When to seek urgent or emergency care
Call emergency services or go to an emergency department immediately if you develop:
- Sudden severe leg pain, a cold foot, new numbness, or weakness
- Rapid color change (pale or blue/purple)
- Inability to move toes or foot
- Severe swelling and pain that worsens after a procedure
Contact your clinician promptly (same day if possible) for:
- New rest pain at night
- A new sore that is not improving
- Increasing walking pain that limits daily activity
- Signs of infection around wounds (redness, warmth, drainage, fever)
A well-executed recovery plan often improves walking distance and lowers future risk—especially when prevention is treated as a long-term partnership rather than a short course of care.
References
- 2024 ACC/AHA/AACVPR/APMA/ABC/SCAI/SVM/SVN/SVS/SIR/VESS Guideline for the Management of Lower Extremity Peripheral Artery Disease: A Report of the American College of Cardiology/American Heart Association Joint Committee on Clinical Practice Guidelines 2024 (Guideline)
- 2024 ESC Guidelines for the management of peripheral arterial and aortic diseases 2024 (Guideline)
- Acute limb ischemia 2023 (Clinical Review)
- Treatment Strategies and Prognostic Outcomes in Acute Limb Ischemia: A Systematic Review and Meta-Analysis Comparing Thrombolytic Therapy and Open Surgical Interventions 2025 (Systematic Review/Meta-Analysis)
Disclaimer
This article is for general education and does not replace medical advice, diagnosis, or treatment from a licensed clinician. Femoral artery thrombosis can be a medical emergency. If you have sudden severe leg pain, a cold or numb foot, weakness, or rapid color change, seek emergency care immediately. Treatment choices and medication plans must be individualized based on your symptoms, test results, bleeding risk, and other health conditions.
If you found this guide helpful, please share it on Facebook, X (formerly Twitter), or any platform you prefer, and follow us on social media. Your support through sharing helps our team keep producing clear, reliable health content.






