A Gerbode defect is an uncommon heart condition where blood takes an abnormal shortcut between two chambers that normally do not connect. For many people, the first clue is not a dramatic symptom, but a “whooshing” heart sound heard during a routine exam. In others, the extra blood flow quietly strains the right side of the heart over months or years, leading to fatigue or shortness of breath that can be easy to blame on stress, age, or poor sleep.
The good news is that today’s imaging can usually pinpoint the problem accurately, and effective treatments—including catheter-based closure in selected cases—often restore normal heart circulation and quality of life. This guide explains what a Gerbode defect is, why it happens, how it’s found, and what treatment and long-term management typically involve.
Table of Contents
- What is a Gerbode defect
- What causes it and who is at risk
- Early symptoms and possible complications
- How doctors confirm the diagnosis
- Treatment options and what recovery looks like
- Living well, follow-up, and when to seek care
What is a Gerbode defect
A Gerbode defect is a rare type of heart shunt—an abnormal passage that lets blood flow where it shouldn’t. Specifically, it allows blood to move from the left ventricle (the main pumping chamber that sends blood to the body) into the right atrium (a receiving chamber on the right side of the heart). Because the left ventricle pumps at much higher pressure, blood tends to jet across the defect during each heartbeat.
Why that pathway matters
Under normal anatomy, oxygen-rich blood follows a “one-way loop”: left ventricle → body → right atrium → right ventricle → lungs → left side again. A Gerbode defect creates a shortcut that sends some oxygen-rich blood back to the right side. Over time, this can lead to:
- Volume overload of the right atrium and right ventricle (they handle more blood than designed).
- Extra flow to the lungs, which can cause breathlessness and reduced exercise tolerance.
- Enlargement of right-sided chambers and, later, strain on the left side as the lungs return more blood to the left heart.
Congenital versus acquired forms
Gerbode defects come in two broad categories:
- Congenital (present at birth): The heart’s internal wall (septum) doesn’t fully form in a small area near the heart valves.
- Acquired (develops later): The tissue between chambers is damaged by infection, surgery, trauma, or (less commonly) a heart attack affecting the septum.
“Direct” and “indirect” patterns
Clinicians often describe Gerbode defects by how the blood reaches the right atrium:
- Direct: Blood flows straight from left ventricle to right atrium through a thin portion of the septum near the valves.
- Indirect: Blood first crosses into the right ventricle through a nearby ventricular septal defect (VSD), then leaks into the right atrium because of an associated problem with the tricuspid valve.
This classification matters because it affects how the jet looks on ultrasound and how closure is planned.
Why it can be missed
A high-velocity jet into the right atrium can resemble other common findings—especially tricuspid valve leakage or pulmonary hypertension—unless the imaging team deliberately considers the possibility of a left-ventricle-to-right-atrium shunt.
What causes it and who is at risk
Gerbode defects form when the thin tissues separating the left ventricle from the right atrium are missing (congenital) or become disrupted (acquired). Understanding the cause isn’t just academic—it helps guide treatment, predicts whether the defect might enlarge, and flags related issues that also need attention.
Congenital causes
During early fetal development, several structures fuse to create the heart’s internal “walls” and valve supports. In a congenital Gerbode defect, a small region near the membranous septum (a thin area close to the aortic and tricuspid valves) does not develop normally. The result can be a tiny opening or a more substantial passage.
Congenital Gerbode defects are rare—often described as a very small fraction of congenital heart abnormalities. They may occur alone, but they can also appear with other defects such as:
- Perimembranous ventricular septal defects (a common nearby VSD type)
- Abnormalities of the tricuspid valve
- Left-sided valve issues (less common, but important to check)
Acquired causes
Acquired Gerbode defects are reported more often than congenital ones in modern practice, partly because more people undergo valve surgery and catheter-based procedures. Common acquired triggers include:
- Cardiac surgery: Especially operations involving the aortic or mitral valve, septal myectomy, or repair of nearby defects. The tissues near the valves can be thin or calcified, making them vulnerable.
- Infective endocarditis: Infection can erode septal tissue or valve structures, creating a new pathway between chambers.
- Trauma: Penetrating chest trauma and, rarely, blunt injury can disrupt septal structures.
- Myocardial infarction: A heart attack affecting the septum can rupture tissue; this is uncommon in the specific Gerbode pattern but possible.
Risk factors clinicians look for
Risk factors depend on whether the defect is congenital or acquired. Important ones include:
- History of valve surgery (aortic/mitral) or complex re-operations
- Known or suspected endocarditis risks, such as:
- Prosthetic heart valves
- Prior endocarditis
- Intravenous drug use
- Poor dental health with frequent gum bleeding
- Significant valve calcification, which can increase surgical complexity
- Prior congenital heart disease repairs near the membranous septum
A practical takeaway
If a new “murmur” appears after heart surgery—or if a person develops unexplained right-sided heart failure signs (leg swelling, abdominal fullness, jugular vein distension) after an infection—clinicians often consider an acquired shunt like a Gerbode defect among the possibilities.
Early symptoms and possible complications
Symptoms from a Gerbode defect vary widely. Some people feel completely well and learn about the condition only after a routine exam. Others develop symptoms that build slowly, especially if the shunt is moderate to large or if it develops abruptly after surgery or infection.
Early symptoms people often notice
The most common early experiences reflect the heart working harder to manage extra blood flow:
- Shortness of breath, especially with exertion (stairs, brisk walking)
- Fatigue that feels disproportionate to activity
- Reduced exercise tolerance—needing more breaks than usual
- Palpitations (awareness of heartbeat), sometimes due to atrial rhythm changes
- Chest discomfort or pressure (not typical, but can occur with strain or coexisting valve disease)
- In infants or children (congenital cases):
- Poor weight gain
- Sweating with feeds
- Rapid breathing
- Frequent respiratory infections
A key clinical clue is often a loud holosystolic murmur—a “blowing” sound that persists through the heartbeat. Because a left-ventricle-to-right-atrium jet can be fast and noisy, the murmur may sound striking even when symptoms are mild.
Complications to watch for
When the shunt is significant, complications generally relate to ongoing volume overload and turbulence:
- Right atrial and right ventricular enlargement
- Heart failure symptoms, often right-sided first:
- Leg swelling
- Abdominal bloating or discomfort
- Rapid weight gain from fluid retention
- Pulmonary hypertension (high pressure in lung arteries), especially if untreated for years
- Arrhythmias, such as atrial fibrillation or atrial flutter
- Valve problems, including tricuspid regurgitation or issues caused by jet impact
- Hemolysis (breakdown of red blood cells) in rare situations with very high-velocity jets
- Recurrent or persistent infection if the defect formed due to endocarditis
When symptoms suggest urgency
Seek urgent evaluation if any of the following occur, especially with a known or suspected defect:
- New fainting, severe breathlessness at rest, or bluish lips
- Rapid swelling of legs or abdomen over days
- Fever with chills plus new murmur or worsening fatigue (possible endocarditis)
- Sudden worsening after recent heart surgery or a procedure
Why timing matters
A small defect may remain stable for years, but a moderate or large shunt can gradually remodel the heart. Early recognition—before lung pressures rise or rhythm problems become persistent—often widens the range of safe, effective treatment options.
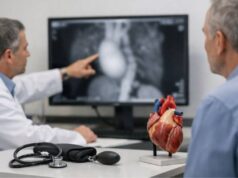
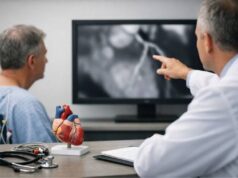
How doctors confirm the diagnosis
Diagnosing a Gerbode defect is mostly an imaging challenge: the clinician must prove that blood is moving from the left ventricle into the right atrium and not being mistaken for a more common problem. A careful, stepwise approach usually provides clarity.
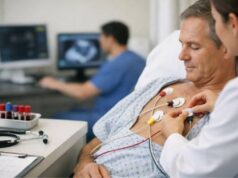
Step 1: History and physical exam
Clinicians start by asking about:
- Exercise tolerance changes, breathlessness, swelling, palpitations
- Past heart surgery, catheter procedures, chest trauma, or recent bloodstream infection
- Fever, night sweats, or unexplained weight loss (signals of possible endocarditis)
On exam, they listen for a murmur and look for signs of fluid overload (leg swelling, enlarged neck veins) or lung congestion.
Step 2: Echocardiography as the workhorse
A standard ultrasound of the heart (transthoracic echocardiogram, TTE) is often the first test. Using color Doppler (a technique that shows blood flow direction), the team looks for a high-velocity jet entering the right atrium.
Because anatomy near the valves can be hard to visualize through the chest wall, many patients benefit from transesophageal echocardiography (TEE), where the ultrasound probe sits in the esophagus behind the heart. TEE can:
- Clarify the exact origin of the jet
- Distinguish a Gerbode jet from tricuspid valve leakage
- Detect vegetations, abscesses, or valve injury in suspected endocarditis
- Help plan catheter-based closure by measuring the defect more precisely
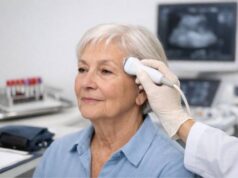
Step 3: Cross-sectional imaging when needed
If echo images are limited or the anatomy is complex, other tests can add precision:
- Cardiac MRI: Measures chamber sizes and estimates shunt volume, often without radiation.
- Cardiac CT: Useful when valve calcification, surgical patches, or device planning requires detailed anatomy.
Step 4: Cardiac catheterization for hemodynamics
A catheter study is not always necessary, but it can be valuable when:
- Lung pressures must be measured accurately
- The team needs a reliable estimate of shunt severity (often expressed as Qp:Qs, pulmonary-to-systemic flow ratio)
- Closure is planned and detailed mapping is needed
Common diagnostic pitfalls
A Gerbode defect can be misread as:
- Severe tricuspid regurgitation
- Pulmonary hypertension
- A standard ventricular septal defect without atrial involvement
A useful “double-check” is to confirm that the jet begins in the left ventricle (or left ventricular outflow tract area) and enters the right atrium with the expected timing and velocity pattern.
Treatment options and what recovery looks like
Treatment depends on the defect’s size, the amount of extra blood flow, symptoms, and whether the defect is congenital or acquired. The goal is simple: reduce harmful overload on the right heart and lungs while protecting nearby valves and conduction tissue.
When careful monitoring is enough
Small defects with minimal shunting may be managed with observation, especially if:
- The person has no symptoms
- Right-sided chambers are not enlarging
- Lung pressures are normal
- There is no history of endocarditis related to the defect
Monitoring typically involves periodic echocardiograms and symptom check-ins. The interval varies, but many clinicians reassess more frequently early on to confirm stability.
Medical therapy as a bridge or support
Medicines do not “close” the defect, but they can reduce symptoms and stabilize the heart before definitive repair:
- Diuretics to reduce fluid overload and breathlessness
- Medications to control heart rhythm if atrial arrhythmias occur
- Treatment of contributing valve disease or high blood pressure when present
If endocarditis is the cause, IV antibiotics and close specialist management are essential, and the decision about closure often depends on infection control and tissue integrity.
Definitive closure: surgery or catheter-based repair
Closure is usually recommended when the shunt is hemodynamically significant—meaning it is causing symptoms, enlarging the right heart, or raising lung pressures. There are two main approaches:
1) Surgical repair
Surgeons close the opening using stitches or a patch. Surgery is often preferred when:
- The anatomy is complex or very close to valves
- There is active or recent infection with damaged tissue that needs reconstruction
- Valve repair or replacement is needed at the same time
2) Transcatheter device closure
In selected patients, an interventional cardiologist can deliver a closure device through blood vessels (usually from the groin) and seal the defect without open-heart surgery. This approach is more likely when:
- The defect has suitable rims for device anchoring
- Surgical risk is high (for example, after prior operations)
- The defect is acquired and well-defined
What recovery typically involves
Recovery differs by approach:
- After catheter closure: Many patients go home within 1–2 days if stable. Activity restrictions are usually shorter, with gradual return to normal routines over a few weeks.
- After surgery: Hospital stay may be about a week (varies widely). Fatigue can last several weeks, and full recovery often takes 6–12 weeks.
In both cases, follow-up imaging confirms that the shunt is closed (or reduced to a tiny “trivial” leak) and that the valves and heart rhythm remain stable.
Living well, follow-up, and when to seek care
A Gerbode defect is treatable, but it benefits from structured follow-up—especially because the defect sits close to heart valves and the electrical conduction system. Whether you are monitoring a small defect or recovering after closure, day-to-day choices and surveillance can meaningfully affect long-term outcomes.
Follow-up that protects the heart over time
Many patients do best with a cardiologist who has experience in congenital or structural heart conditions. Follow-up commonly includes:
- Periodic echocardiograms to track chamber size, valve function, and any residual shunt
- Rhythm checks (ECG, or longer monitoring if palpitations occur)
- Review of exercise tolerance and fluid status
If you have had closure, early visits confirm device or patch stability and ensure that the right heart is remodeling in the expected direction.
Activity, fitness, and travel
In general, movement is helpful—but the right intensity depends on your heart’s current workload.
- If symptoms are present, start with low-impact activity (walking, cycling) and build gradually.
- If you have significant pulmonary hypertension or ongoing heart failure signs, ask your cardiology team before starting vigorous exercise.
- For long travel, discuss precautions if you have arrhythmias, anticoagulation, or recent surgery.
Infection awareness and heart health habits
Because acquired defects can be linked to infection, and turbulent flow can increase endocarditis risk in some settings, it’s wise to take prevention seriously:
- Prioritize dental hygiene and regular dental care (healthy gums reduce bloodstream bacteria exposure).
- Don’t ignore persistent fevers—especially if you have a history of valve surgery or a prior heart infection.
- Keep vaccinations current (influenza and other recommended vaccines), particularly if you have heart failure.
Antibiotic prophylaxis before dental procedures is not universal for every patient with a Gerbode defect; eligibility depends on individual risk factors. Your cardiologist can clarify whether you fall into a group for whom prophylaxis is recommended.
Pregnancy and special situations
If you are pregnant or planning pregnancy, early counseling matters. The key considerations are:
- Shunt size and symptoms
- Lung pressures
- Heart rhythm stability
- Any residual valve disease
Many people do well, but planning allows teams to reduce avoidable risk and coordinate delivery care.
When to seek care promptly
Contact a clinician quickly (same day or urgent care) for:
- New or worsening shortness of breath, swelling, or rapid weight gain
- Palpitations with dizziness or chest pressure
- Fever lasting more than 24–48 hours, especially with a heart murmur history
Go to emergency care for severe breathlessness at rest, fainting, chest pain that doesn’t resolve, or signs of stroke (face droop, arm weakness, speech difficulty).
References
- Congenital Gerbode Defect: A Left Ventricular to Right Atrial Shunt—State-of-the-Art Review of Its General Data, Diagnostic Modalities, and Treatment Strategies – PMC 2024 (Review)
- 2020 ESC Guidelines for the management of adult congenital heart disease – PubMed 2021 (Guideline)
- Transcatheter closure of residual Gerbode defect after aortic valve replacement surgery – PMC 2022 (Case Report)
- When Two Chambers Collide: A Rare Case of an Acquired Gerbode Defect in Infective Endocarditis – PMC 2025 (Case Report)
Disclaimer
This article is for educational purposes only and does not replace personalized medical care. A Gerbode defect can overlap in symptoms and exam findings with other heart conditions, and treatment decisions depend on imaging details, lung pressures, valve involvement, and individual risk factors. If you have symptoms such as shortness of breath, swelling, fever, chest pain, fainting, or palpitations—especially after heart surgery or a recent infection—seek prompt evaluation by a qualified clinician or emergency services when appropriate.
If you found this helpful, please consider sharing it on Facebook, X (formerly Twitter), or any platform you prefer, and following us on social media. Your support through sharing helps our team continue producing clear, reliable health content.