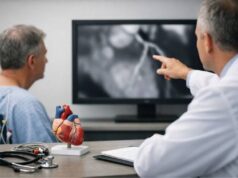
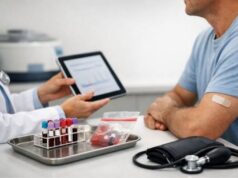
Gestational hypertension is high blood pressure that starts during pregnancy—usually after the midpoint—and was not present before. For many people, it arrives quietly: a normal-feeling day, a routine prenatal visit, and then an unexpected number on the cuff. Even without symptoms, these readings matter because they can signal stress on the body’s blood vessels and increase the chance of complications later in pregnancy or shortly after birth.
The reassuring part is that gestational hypertension is often manageable with close monitoring, timely treatment when needed, and a clear plan for delivery and postpartum follow-up. This article explains what the diagnosis means, why it can develop, what warning signs deserve urgent attention, how clinicians confirm it, and how to protect both parent and baby during pregnancy and beyond.
Table of Contents
- What gestational hypertension means for your body
- What causes it and who is at higher risk
- Symptoms, red flags, and complications
- How it is diagnosed and ruled from preeclampsia
- Treatments that work and what to expect
- Daily management, postpartum care, and when to seek help
What gestational hypertension means for your body
Gestational hypertension is diagnosed when blood pressure becomes elevated after 20 weeks of pregnancy and there are no clear signs of preeclampsia (a pregnancy complication involving blood pressure plus organ stress). In practice, clinicians usually use a threshold of 140/90 mmHg or higher on at least two readings taken apart in time, using proper technique. One high number can happen for many reasons—pain, anxiety, rushing into clinic—so the pattern over hours to days matters more than a single reading.
How it differs from other pregnancy blood pressure conditions
Pregnancy-related high blood pressure is not one single diagnosis. The timing and associated findings help separate common categories:
- Chronic hypertension: high blood pressure that existed before pregnancy or appears before 20 weeks.
- Gestational hypertension: new high blood pressure after 20 weeks without clear organ involvement.
- Preeclampsia: high blood pressure with evidence of organ stress (often kidney, liver, blood, brain, or placenta).
- Postpartum hypertension: high blood pressure that appears or worsens after delivery.
These distinctions are important because they change monitoring, medication decisions, and delivery planning.
What’s happening inside the body
Pregnancy naturally changes circulation. Blood volume increases, the heart pumps more each minute, and blood vessels usually relax to support placental blood flow. In gestational hypertension, that balance shifts: blood vessels can become less able to relax, and the body may respond with higher pressure to maintain flow. Sometimes the condition stays mild and stable. Other times, it is an early warning that the placenta and blood vessels are under strain, and preeclampsia can develop later.
Why the diagnosis matters even if you feel fine
Gestational hypertension is often symptom-free. Yet untreated or rapidly rising pressures can increase the risk of complications like stroke (rare, but serious), placental problems, and growth issues for the baby. The goal of care is not only to “lower a number,” but to:
- Spot worsening disease early
- Protect the brain, kidneys, liver, and placenta
- Decide the safest time for delivery
- Plan postpartum monitoring, when blood pressure can spike again
With a clear plan, many people go on to have healthy deliveries and recover fully—but follow-up matters because blood pressure changes can persist or return after birth.
What causes it and who is at higher risk
Gestational hypertension does not have a single cause. It appears to result from a mix of placental, vascular, metabolic, and genetic influences that vary from person to person. A useful way to think about it is this: pregnancy asks the body to build a high-flow circulation to the placenta. If the blood vessels do not adapt smoothly, blood pressure can rise—sometimes mildly, sometimes quickly.
Factors that may contribute
Researchers and clinicians commonly point to several overlapping contributors:
- Placental signaling and vessel adaptation: In some pregnancies, the placenta’s early development and blood vessel remodeling are less efficient. That can lead to higher resistance in placental circulation later.
- Baseline vascular health: If blood vessels were already “stiffer” or more reactive before pregnancy (even without a hypertension diagnosis), the normal drop in blood pressure seen early in pregnancy may be smaller.
- Metabolic strain: Insulin resistance, higher inflammation, and higher body mass can increase vascular stress.
- Genetic and family tendency: A family history of hypertensive disorders in pregnancy raises risk, suggesting inherited vulnerability.
None of these means you “caused” the condition. Many people with risk factors never develop gestational hypertension, and some people with no clear risk factors do.
Who is at higher risk
Risk increases when pregnancy places higher demands on circulation or when a person starts pregnancy with less cardiovascular reserve. Common risk factors include:
- First pregnancy, or first pregnancy with a new partner
- Previous gestational hypertension or preeclampsia
- Pregnancy with twins or higher-order multiples
- Pre-pregnancy obesity or significant weight gain early in pregnancy
- Maternal age over 35
- Chronic kidney disease or diabetes (type 1, type 2, or significant gestational diabetes)
- Autoimmune disease (such as lupus or antiphospholipid syndrome)
- Pre-existing high blood pressure that was previously mild or undiagnosed
- Assisted reproduction (including some IVF pregnancies)
Social and structural factors matter too. Limited access to prenatal care, higher chronic stress load, and barriers to follow-up can increase the chance that rising blood pressure is detected later than it should be.
A practical, patient-centered insight
In clinic, the most actionable “risk factor” is often not a trait—it is a missed trend. A slow climb from 110/70 to 128/82 to 138/88 can be easy to overlook if visits are spaced out or readings are taken under rushed conditions. Consistent measurement—same arm, correct cuff size, seated rest—often reveals the true pattern early enough to intervene calmly rather than urgently.
Symptoms, red flags, and complications
Many people with gestational hypertension feel completely normal. That can be unsettling—how can something important have no symptoms? The reason is that blood pressure is a “silent” signal until it becomes severe or triggers organ stress. This is why regular prenatal checks and, in some cases, home monitoring are so valuable.
Common symptoms (and why they can be misleading)
Gestational hypertension itself may cause no symptoms, but some people notice:
- Mild headaches
- Feeling “puffy” or swelling in hands/feet
- Shortness of breath with exertion
- A sense of racing heart or anxiety
These can overlap with normal pregnancy changes. The key is change and intensity—a new symptom that is persistent, worsening, or severe deserves prompt evaluation.
Red flags that need urgent assessment
Some symptoms suggest severe hypertension or possible progression toward preeclampsia. Contact your maternity care team urgently (or emergency services if severe) if you have:
- Severe or persistent headache that does not improve with rest or recommended medication
- Visual changes (blurred vision, flashing lights, spots, temporary loss of vision)
- New pain in the right upper abdomen or under the ribs
- Sudden swelling of face/hands or rapid weight gain over 1–2 days
- Chest pain, severe shortness of breath, or fainting
- Decreased fetal movement
- Blood pressure readings at home in the severe range (often 160/110 mmHg or higher)
Possible complications
Most people with gestational hypertension do well, especially with monitoring. Still, clinicians take it seriously because it can increase risk for both parent and baby.
Maternal risks may include:
- Progression to preeclampsia
- Placental abruption (placenta detaches too early)
- Stroke (rare, usually associated with severe blood pressure)
- Fluid in the lungs (pulmonary edema), especially with severe disease
- Cesarean delivery, often related to induction or fetal concerns
- Postpartum blood pressure spikes, sometimes after discharge
Baby-related risks may include:
- Growth restriction if placental blood flow is reduced
- Preterm birth, often because early delivery becomes the safest option
- Low amniotic fluid in some cases
- Admission to neonatal intensive care if born early
The “trajectory” matters as much as the diagnosis
Two people can share the same label but have very different experiences. A stable blood pressure around 140–150/90–95 with normal labs and reassuring fetal growth is a different scenario than pressures climbing week by week with new symptoms. That is why care plans are built around trends: repeated blood pressure checks, symptom review, lab monitoring when needed, and fetal surveillance tailored to risk.
How it is diagnosed and ruled from preeclampsia
The diagnosis of gestational hypertension is straightforward in concept—new high blood pressure after 20 weeks—but careful in execution. Clinicians aim to confirm the blood pressure pattern accurately and then check whether any signs point to preeclampsia or another cause.
Confirming blood pressure the right way
Accurate readings depend on technique. A reliable clinic or home measurement typically includes:
- Seated rest for 5 minutes
- Back supported, feet flat, arm supported at heart level
- Correct cuff size (too small can falsely raise readings)
- No smoking, caffeine, or exercise right before measurement when possible
- Two readings taken 1–2 minutes apart, averaged
Clinicians usually look for two elevated measurements separated in time (often at least several hours apart) to avoid labeling a temporary spike as a diagnosis.
What clinicians check to rule out preeclampsia
Because gestational hypertension can evolve into preeclampsia, clinicians often order tests at diagnosis and repeat them if symptoms or blood pressure worsen. Typical evaluation may include:
- Urine protein testing: dipstick screening plus a protein-to-creatinine ratio or 24-hour urine if needed
- Blood tests to assess organ stress:
- Platelet count (clotting cells)
- Liver enzymes
- Kidney function (creatinine)
- Symptom review: headache, visual changes, abdominal pain, breathing difficulty
- Fetal assessment: growth ultrasound, amniotic fluid evaluation, and sometimes nonstress testing
If any of these suggest organ involvement, the diagnosis shifts away from “gestational hypertension alone” toward preeclampsia or another hypertensive disorder.
Home blood pressure monitoring: useful, but structured
Home monitoring can be a major advantage when done consistently. It helps distinguish:
- True hypertension vs “white coat” elevation
- Stable pressures vs an upward trend between visits
A practical approach many clinicians recommend is taking readings twice daily for 3–7 days when first evaluating the pattern (for example, morning and evening), then adjusting frequency based on stability. The most helpful logs include the date, time, reading, and any symptoms.
When diagnosis is more complicated
A few situations require extra care:
- Earlier-than-expected high blood pressure: may suggest previously unrecognized chronic hypertension.
- Very rapid onset after normal readings: raises concern for evolving preeclampsia or a secondary cause.
- Other medical conditions: kidney disease, thyroid disease, or medication effects can influence readings.
The guiding principle is safety: confirm the diagnosis, determine severity, and repeat assessment whenever symptoms change.
Treatments that work and what to expect
Treatment for gestational hypertension is individualized. The plan depends on how high the blood pressure is, how far along the pregnancy is, whether labs are reassuring, how the baby is growing, and whether symptoms appear. In most cases, the strategy combines monitoring, targeted medication when thresholds are met, and delivery planning.
Monitoring is a treatment
For mild-range gestational hypertension, frequent check-ins can prevent emergencies. Monitoring may include:
- More frequent prenatal visits for blood pressure and symptom review
- Home blood pressure checks with clear parameters for when to call
- Periodic lab tests to watch for preeclampsia
- Ultrasounds to track fetal growth and amniotic fluid
- Fetal testing in later pregnancy if indicated
This approach works because complications often develop gradually, and early warning signs are detectable before they become dangerous.
When medication is used
Medication decisions balance maternal safety and fetal well-being. Clinicians commonly treat:
- Severe-range pressures (often around 160/110 mmHg or higher) urgently
- Persistent moderate elevations, especially if there are additional risk factors or signs of worsening
Commonly used blood pressure medications in pregnancy include:
- Labetalol
- Nifedipine (extended release)
- Methyldopa (used less often in some settings but still an option)
Some medications used outside pregnancy are avoided because they can harm fetal kidney development or amniotic fluid levels (for example, ACE inhibitors and ARBs). Your clinician will also consider asthma, heart rate, migraine history, and other factors when choosing a medication.
Timing of delivery: the “definitive” cure
Delivery is the only complete resolution for pregnancy-related hypertension, though blood pressure may remain elevated for days to weeks postpartum. For gestational hypertension without severe features, many care plans aim for delivery at or near term (often around 37 weeks), depending on stability and local protocols. Earlier delivery may be recommended if:
- Blood pressure becomes severe or hard to control
- Lab tests suggest organ stress
- Symptoms develop
- Fetal growth or testing becomes concerning
What to expect after birth
Many people see improvement after delivery, but postpartum is not “risk-free.” Blood pressure can rise again—often peaking several days after birth—so clinicians may recommend:
- Blood pressure checks before discharge and within days after going home
- Medication continuation or adjustment postpartum, including breastfeeding-safe options
- Clear instructions for urgent symptoms (headache, vision changes, chest pain, shortness of breath)
A good treatment plan feels specific: it should tell you what numbers matter, what symptoms matter, and exactly what the next step is.
Daily management, postpartum care, and when to seek help
Living with gestational hypertension is less about perfection and more about consistency: reliable measurements, realistic routines, and a low threshold for asking questions when something changes. The goal is to keep you safe now and reduce long-term risk after pregnancy.
Daily management that makes monitoring easier
A practical day-to-day plan often includes:
- Home blood pressure routine: take readings at the same times each day, seated and rested, and record them.
- Symptom checkpoints: a short daily scan—headache, vision, upper abdominal pain, sudden swelling, shortness of breath, reduced fetal movement.
- Hydration and nutrition basics: regular meals with adequate protein and fiber; avoid extreme restriction or “detox” approaches.
- Activity: gentle movement (such as walking) if your clinician approves; avoid pushing through dizziness, chest discomfort, or severe breathlessness.
- Sleep and stress load: not as a cure, but as a stabilizer. Poor sleep and high stress can worsen readings and make symptoms harder to interpret.
Salt restriction is not usually a standalone treatment in pregnancy hypertension, but very high-salt processed foods can worsen fluid retention. Think “steady, balanced,” not punitive.
Postpartum care: the part many people are not warned about
Blood pressure problems can continue—or even appear for the first time—after delivery. Postpartum planning should include:
- A scheduled blood pressure check within the first week after birth (earlier if you had severe readings)
- Clear medication instructions, including what is compatible with breastfeeding if you choose to breastfeed
- Guidance on when to return to clinic or go to emergency care
- A follow-up visit around 6 weeks, and often another check later if readings remain elevated
Long-term health after gestational hypertension
Even if blood pressure returns to normal, gestational hypertension can be a marker of future risk. Many clinicians recommend:
- Yearly blood pressure checks
- Periodic screening for cholesterol and blood sugar, especially if there are additional risk factors
- Heart-healthy habits that are realistic in the postpartum season: gradual return to activity, supportive nutrition, and weight management when appropriate
If you plan another pregnancy, ask early about prevention strategies. In many cases, clinicians consider low-dose aspirin in future pregnancies for people with a history of hypertensive disorders, but the decision is individualized.
When to seek urgent help
Go to urgent care or emergency services if you have:
- Severe headache, vision changes, or confusion
- Chest pain, severe shortness of breath, fainting, or seizure
- Severe blood pressure readings at home (often 160/110 mmHg or higher) or a rapid jump from your usual numbers
- Heavy bleeding, severe abdominal pain, or a sudden decline in how you feel
You deserve a plan that feels clear and supportive. If you leave a visit unsure what to watch for, ask for written thresholds and a step-by-step “if this, then that” guide.
References
- The 2021 International Society for the Study of Hypertension in Pregnancy classification, diagnosis & management recommendations for international practice 2022 (Guideline)
- A summary of the 2023 Society of Obstetric Medicine of Australia and New Zealand (SOMANZ) hypertension in pregnancy guideline 2024 (Guideline)
- Hypertension in Pregnancy and Postpartum: Current Standards and Opportunities to Improve Care 2025 (Review)
- Hypertension in pregnancy: diagnosis and management 2023 (Guideline)
Disclaimer
This article is for educational purposes only and does not replace personalized medical advice, diagnosis, or treatment. Gestational hypertension can change quickly and may overlap with other pregnancy complications that require urgent evaluation. If you have high blood pressure readings, new or worsening symptoms (such as headache, vision changes, chest pain, shortness of breath, or reduced fetal movement), or you feel that something is not right, contact your maternity care team promptly or seek emergency care.
If this guide was helpful, please consider sharing it on Facebook, X (formerly Twitter), or any platform you prefer, and follow us on social media. Your support through sharing helps our team keep producing clear, trustworthy health information.