A giant aortic aneurysm is a dangerously enlarged bulge in the body’s main artery, the aorta. Most aneurysms grow silently for years, but when the aorta becomes very large, the stakes change: the wall can tear (dissection) or burst (rupture), and either event can become life-threatening within minutes. “Giant” is not a single official size cutoff. Clinicians use the term when an aneurysm is far beyond typical repair thresholds, often because it has been missed, grown rapidly, or developed in a high-risk segment of the aorta.
If you or someone you love has been told they have a large or “giant” aortic aneurysm, you deserve clear answers. This guide explains what it is, why it happens, how it’s diagnosed, which treatments are most effective, and what daily management looks like before and after repair.
Table of Contents
- What makes an aortic aneurysm “giant”
- Causes and risk factors that drive growth
- Symptoms and emergencies you should not ignore
- How giant aortic aneurysms are diagnosed
- Treatment options: surgery and endovascular repair
- Long-term management, prevention, and follow-up
What makes an aortic aneurysm “giant”
An aortic aneurysm is an abnormal widening of the aorta caused by weakening of its wall. The aorta starts at the heart, curves through the chest, and continues into the abdomen, branching to supply every organ. Where the aneurysm sits matters because each segment has different normal diameters, different nearby structures, and different repair options.
Clinicians use “giant” as a practical warning label rather than a strict diagnosis. In day-to-day care, “giant” often implies at least one of the following:
- The aneurysm is far larger than the usual size at which repair is recommended.
- The aneurysm is expanding quickly (growth over months rather than years).
- The aneurysm is causing compression symptoms or signs of impending rupture.
- The aneurysm shape is especially concerning (for example, saccular or infected aneurysms).
Why size changes risk so sharply
As the aorta expands, wall tension rises. A helpful way to picture it is a balloon: the more it stretches, the more stress the wall must تحمل with every heartbeat. Larger aneurysms have a higher chance of tearing or rupturing, but “risk” is not determined by diameter alone. Aneurysms can become dangerous at smaller sizes in certain settings, such as:
- Genetic connective tissue conditions (for example, Marfan syndrome or Loeys-Dietz syndrome)
- Bicuspid aortic valve–associated aortopathy
- Aneurysms with symptoms (pain, hoarseness, trouble swallowing)
- Rapid growth documented on imaging
- Saccular aneurysms (a bulge on one side rather than a uniform widening)
Thoracic vs abdominal “giant” aneurysms
A giant aneurysm in the chest (thoracic aorta) can threaten the heart, brain, and spinal cord circulation, and it may also affect the aortic valve. A giant aneurysm in the abdomen (abdominal aortic aneurysm, AAA) is often most feared for sudden rupture, sometimes without warning. Thoracoabdominal aneurysms span both regions and can be especially complex because they involve branches to the kidneys, intestines, and spinal cord.
A key takeaway
If a report uses the word “giant,” treat it as a signal to act quickly and thoughtfully. It does not automatically mean “emergency surgery today,” but it does mean you need a specialist-led plan, clear thresholds, and a timeline that is measured in days to weeks—not “see you next year.”
Causes and risk factors that drive growth
Aortic aneurysms develop when the aortic wall loses strength and elasticity. That weakening can be gradual, like slow wear on a rope, or it can be accelerated by inflammation, infection, or genetic vulnerability. Giant aneurysms usually reflect either long-standing disease that went undetected or a process that causes faster expansion.
Common causes by location
In the abdomen, the most common driver is atherosclerotic degeneration—changes linked to age, smoking, and vascular disease. In the chest, causes are more mixed and include genetic and valve-related conditions more often.
Frequent contributors include:
- Smoking history: The strongest modifiable risk factor for AAA development and faster growth.
- High blood pressure: Raises mechanical stress on the wall and increases risk of complications.
- Atherosclerosis and vascular disease: Often travels with aneurysm risk, especially in the abdominal aorta.
- Family history: First-degree relatives with aneurysm or dissection raise suspicion of inherited risk.
- Connective tissue disorders: Conditions such as Marfan syndrome, Loeys-Dietz syndrome, and vascular Ehlers-Danlos syndrome can weaken the aorta at younger ages.
- Bicuspid aortic valve: Can be associated with enlargement of the ascending aorta.
- Inflammatory or autoimmune aortitis: Some immune-driven diseases inflame the aortic wall and speed damage.
- Infection (mycotic aneurysm): Bacterial seeding of the aorta can produce a fragile, fast-growing aneurysm.
- Prior aortic injury or surgery: Trauma, catheter procedures, or previous repair can create vulnerable segments.
Risk factors that help explain “why this got so big”
When clinicians see a giant aneurysm, they often look for reasons it escaped detection or grew faster than expected:
- Limited access to routine care or screening (common with AAA, which may be silent)
- “Normal” symptoms attributed to aging, reflux, or back strain
- Intermittent follow-up imaging or inconsistent measurement methods
- Under-treated blood pressure or ongoing smoking
- A genetic condition not yet recognized in the family
- A segment with unusual anatomy, such as an aberrant arch vessel or coarctation history
Growth patterns that raise concern
Aneurysms do not always grow smoothly. Some remain stable for long periods; others show spurts. Patterns that typically trigger urgent re-evaluation include:
- A clear increase in size over a short interval
- New symptoms localized to chest, back, abdomen, or jaw
- A change from a smooth, fusiform shape to a more irregular or saccular form
Practical insight
Ask not only “How big is it?” but also “How fast did it get here?” A carefully reconstructed timeline—old imaging, past chest X-rays, even incidental scans—can clarify whether the aneurysm is stable and long-standing or rapidly evolving and high-risk.
Symptoms and emergencies you should not ignore
Most aortic aneurysms cause no symptoms until they become large or complicated. Giant aneurysms are more likely to announce themselves, but the signals can still be subtle—pressure rather than pain, fatigue rather than collapse. The priority is knowing which symptoms are “watch closely” and which are “call emergency services now.”
Symptoms of a large or giant aneurysm
Symptoms depend on location and on whether the aneurysm is pressing on nearby structures:
Thoracic (chest) aneurysm may cause:
- Deep chest, upper back, or shoulder blade pain
- Shortness of breath with exertion, sometimes from airway compression
- Hoarseness (pressure on the recurrent laryngeal nerve)
- Trouble swallowing or a feeling of food sticking (esophageal compression)
- A persistent cough not explained by infection
- A new heart murmur if the aortic valve is affected
Abdominal aneurysm may cause:
- Pulsating sensation in the abdomen
- Deep abdominal, flank, or back pain that does not behave like muscle strain
- Early fullness after eating if the aneurysm presses on the stomach area
- Leg pain or discoloration if clot within the aneurysm sends debris downstream
Some people experience no pain but notice a decline in stamina or unexplained anxiety and “impending doom.” Those feelings do not diagnose an aneurysm, but they matter when paired with known aneurysm disease.
Signs of rupture or dissection: treat as an emergency
A rupture or dissection can be rapidly fatal without immediate care. Call emergency services for:
- Sudden, severe chest or back pain, often described as tearing or ripping
- Sudden abdominal or back pain with weakness, sweating, or collapse
- Fainting, confusion, or stroke-like symptoms (face droop, arm weakness, speech trouble)
- Severe shortness of breath, especially with chest pain
- New severe pain after known aneurysm diagnosis, even if it fluctuates
In rupture, blood pressure may drop, skin may become pale and clammy, and nausea or vomiting may occur. In dissection, pain can migrate as the tear extends, and symptoms may reflect blocked blood flow to the brain, kidneys, intestines, or legs.
Complications that can develop before an emergency
Even without rupture, giant aneurysms can cause serious problems:
- Blood clots forming inside the aneurysm and traveling to smaller arteries
- Progressive enlargement leading to valve leakage (ascending aorta)
- Kidney impairment from involvement of renal arteries (complex aneurysms)
- Spinal cord ischemia risk in extensive thoracic or thoracoabdominal disease, especially around repair planning
A clear rule
If pain is new, severe, unusual for you, or paired with faintness, weakness, or neurologic symptoms, do not “wait it out.” With a known large aneurysm, the safest plan is immediate evaluation.
How giant aortic aneurysms are diagnosed
Diagnosis has two goals: confirm the aneurysm’s size and exact location, and map the anatomy well enough to plan safe repair. For giant aneurysms, accuracy matters because small measurement errors can translate into big differences in perceived risk and device sizing.
The imaging tests clinicians rely on
Different tests answer different questions:
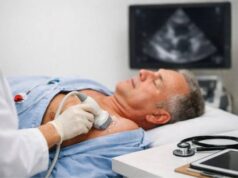
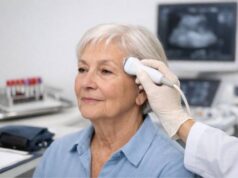
- Ultrasound: Often the first-line test for abdominal aneurysms. It is fast, painless, and good for measuring diameter in many patients. It is less informative for the chest and for complex branch anatomy.
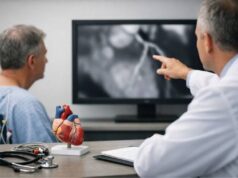
- CT angiography (CTA): The workhorse for detailed planning. It shows the full aorta, nearby branches, calcification, clot inside the aneurysm, and relationships to organs. For repair planning, CTA provides the “roadmap” surgeons and endovascular teams need.
- MR angiography (MRA): Offers excellent detail without ionizing radiation. It can be helpful for surveillance in younger patients or those needing repeated imaging, but it may be less available in urgent settings.
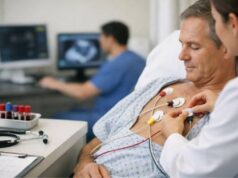
- Echocardiography: A key tool for ascending aortic aneurysms and aortic valve assessment. It helps evaluate valve leakage, heart function, and the aortic root.
How size is measured and why technique matters
Aneurysm size depends on where and how the measurement is taken. Clinicians aim to measure the aorta perpendicular to blood flow, not diagonally. For giant aneurysms, this matters because the aorta may be tortuous or irregular, and diagonal measurements can overestimate true diameter.
Helpful questions to ask your team include:
- Which segment is enlarged (root, ascending, arch, descending, abdominal, iliac)?
- What is the maximum diameter, and where exactly is it measured?
- What was the prior measurement, and over what time interval?
- Are there features that increase risk beyond size (saccular shape, symptoms, infection, rapid growth)?
Assessing overall surgical risk
Before deciding on repair, clinicians typically evaluate the whole person, not just the aneurysm:
- Heart and lung function, including coronary disease risk
- Kidney function, because contrast and major surgery can stress kidneys
- Frailty and functional status, which influence recovery
- Other artery disease that can affect access for endovascular devices
Surveillance vs urgent planning
Small aneurysms can be followed with periodic imaging. Giant aneurysms usually shift the conversation from “surveillance intervals” to “pre-op planning.” Even then, the best teams still move stepwise: confirm measurements, optimize blood pressure, assess anatomy, and choose the safest approach rather than rushing into the wrong procedure.
Treatment options: surgery and endovascular repair
For a giant aortic aneurysm, treatment is usually procedural—meaning repair rather than medication alone—because the risk of catastrophic complications rises with size, symptoms, and growth. The best approach depends on location, anatomy, and patient-specific factors.
Two main repair strategies
1) Open surgical repair
Surgeons replace the weakened aortic segment with a synthetic graft. Open surgery is often preferred when:
- The aneurysm involves the ascending aorta or aortic root
- Valve repair or replacement is needed
- The anatomy is not suitable for stent-grafting
- Infection is present or suspected (infected tissue may require removal)
Open repair is durable and time-tested, but it involves major surgery, longer recovery, and higher short-term stress on the body.
2) Endovascular repair (stent-grafting)
A stent-graft is delivered through arteries (often from the groin) to line the inside of the aorta and exclude the aneurysm from blood pressure. Common forms include:
- EVAR for abdominal aneurysms
- TEVAR for descending thoracic aneurysms
- Fenestrated or branched endovascular repair for complex aneurysms involving kidney or intestinal branches
Endovascular approaches often reduce early recovery time and blood loss, but they require careful anatomical suitability and long-term imaging follow-up to detect issues like endoleaks (persistent blood flow into the aneurysm sac).
What makes “giant” aneurysms technically challenging
Giant aneurysms can distort anatomy. The aorta may be elongated, sharply curved, or heavily calcified. The aneurysm sac may contain clot, and nearby branches may be stretched or displaced. These features can affect:
- Device sizing and sealing zones for endovascular repair
- Access vessel size (some devices require larger arteries)
- Risk of bleeding or rupture during manipulation
- Need for staged procedures to protect the spinal cord or kidneys
Risks and complications to understand
Any repair carries risks. The major ones clinicians plan around include:
- Bleeding, infection, and heart complications
- Stroke risk with arch or ascending procedures
- Kidney injury, especially with contrast and complex repair
- Spinal cord ischemia in extensive thoracic or thoracoabdominal repair
- Endoleaks and reintervention after endovascular repair
What “success” looks like
A good outcome is not only survival through the operation. It also includes:
- Stable graft or stent position
- No ongoing aneurysm sac expansion
- Preserved kidney and neurologic function
- A realistic recovery plan with rehabilitation and follow-up imaging
For many patients, the safest path is care at a high-volume center with both open and endovascular expertise, so the team can choose the best tool rather than forcing one approach.
Long-term management, prevention, and follow-up
Whether you are awaiting repair, recovering after a procedure, or living with a repaired aorta, daily management is not a side note—it is risk reduction. The aorta responds to pressure, inflammation, and vascular health over years. A practical plan helps you control what is controllable and recognize what is not.
Blood pressure and heart-rate control
Lowering stress on the aortic wall is a core goal. Your clinician may recommend:
- A specific home blood pressure target and how often to measure
- Medications that reduce blood pressure and pulse pressure swings
- Avoiding sudden strain, such as heavy lifting or breath-holding during exertion
Ask for clear guidance on exercise. Many people can do moderate aerobic activity safely, but heavy resistance training or maximal effort lifting may be restricted—especially with unrepaired giant aneurysms or connective tissue disorders.
Lifestyle steps that meaningfully change risk
The highest-yield habits are often straightforward:
- Stop smoking: This is one of the most powerful ways to slow aneurysm growth and lower overall cardiovascular risk.
- Treat cholesterol and vascular disease risk: Diet changes, statins when appropriate, and diabetes control can protect arteries broadly.
- Build steady fitness: Regular walking, cycling, or swimming improves blood vessel function and recovery capacity.
- Protect sleep and stress load: These do not replace medical care, but they support steadier blood pressure and healthier routines.
Surveillance after repair
Follow-up imaging is non-negotiable after endovascular repair and often important after open surgery as well. Surveillance commonly aims to detect:
- Endoleaks or graft migration (endovascular repair)
- New aneurysms in other aortic segments
- Changes in branch vessels or graft connections
- Progressive disease if a genetic condition is present
Keep a personal record of:
- Aneurysm location and last measured diameter
- Date and type of repair (open, EVAR, TEVAR, branched/fenestrated)
- Device or graft details if available
- Your imaging schedule and where scans are performed
When to seek care quickly
Call your clinician promptly for:
- New chest, back, or abdominal pain
- New leg pain, numbness, or color change
- Fever or chills after repair, especially with persistent fatigue
- Worsening shortness of breath or swelling
Seek emergency care for sudden severe pain, fainting, neurologic symptoms, or signs of shock.
The long view
A giant aneurysm can feel like a single crisis, but it is often part of a lifelong vascular story. With expert repair, consistent follow-up, and strong risk-factor control, many patients return to active lives—and reduce the chance of future aortic events.
References
- 2022 ACC/AHA Guideline for the Diagnosis and Management of Aortic Disease: A Report of the American Heart Association/American College of Cardiology Joint Committee on Clinical Practice Guidelines 2022 (Guideline)
- Editor’s Choice — European Society for Vascular Surgery (ESVS) 2024 Clinical Practice Guidelines on the Management of Abdominal Aorto-Iliac Artery Aneurysms 2024 (Guideline)
- Aortic aneurysm: pathophysiology and therapeutic options – PMC 2024 (Review)
- Comparison of short-and long-term outcomes between endovascular and open repair for descending thoracic aortic aneurysm: a systematic review and meta-analysis – PMC 2025 (Systematic Review)
Disclaimer
This article is for general educational purposes and does not replace medical advice from your clinician. A giant aortic aneurysm can become dangerous without warning, and treatment decisions depend on aneurysm location, exact measurements, growth rate, symptoms, medical history, and imaging details. If you have sudden severe chest, back, or abdominal pain, fainting, stroke-like symptoms, severe shortness of breath, or signs of shock, seek emergency care immediately.
If you found this article useful, please share it on Facebook, X (formerly Twitter), or any platform you prefer, and follow us on social media. Your support through sharing helps our team continue producing high-quality, trustworthy health content.