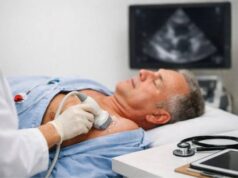
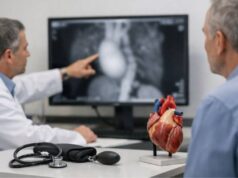
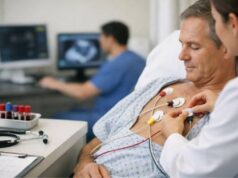
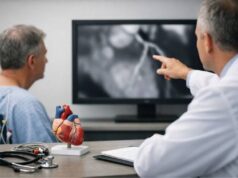
Giant cell arteritis is a treatable condition, but it asks for speed and clarity. It happens when certain blood vessels become inflamed and narrowed, most often in adults over 50. The first signs can feel ordinary—a new headache, scalp tenderness when brushing hair, or jaw pain while chewing—until something suddenly isn’t ordinary at all, like blurred vision or a shadow across one eye.
Because vision loss can become permanent, clinicians often start treatment as soon as giant cell arteritis is strongly suspected, even before every test result is back. That urgency can feel frightening, yet it reflects how responsive the disease is to the right therapy. In this guide, you’ll learn what the diagnosis means, why it happens, what symptoms matter most, how doctors confirm it, and how treatment and long-term follow-up protect your sight and overall health.
Table of Contents
- What giant cell arteritis does to arteries
- Causes and risk factors that matter most
- Symptoms, especially vision warning signs
- How it is diagnosed and why speed matters
- Treatment options: steroids, biologics, and tapers
- Management, prevention, and when to seek urgent care
What giant cell arteritis does to arteries
Giant cell arteritis (GCA) is a form of vasculitis—blood vessel inflammation—that most often targets medium and large arteries. In practical terms, the vessel wall becomes swollen and irritated. That swelling narrows the channel where blood flows, and the blood supply downstream can drop. When the arteries that feed the eyes are involved, reduced blood flow can injure the optic nerve or retina, sometimes quickly and permanently.
Which arteries are usually involved
Many people associate GCA with the “temporal arteries” at the sides of the head, because tenderness there is common and biopsy is often taken from that area. But GCA can involve a wider network:
- Arteries of the scalp and temples
- Branches that supply the jaw muscles
- Arteries that feed the eyes
- Larger vessels such as the aorta and its major branches (sometimes called “large-vessel GCA”)
This is why some people have classic head symptoms, while others mainly have arm fatigue with use, unexplained fevers, or chest and back discomfort from larger-vessel involvement.
How inflammation creates symptoms
GCA symptoms come from two main effects:
- Inflammation signals in the body
- Fatigue, low-grade fever, weight loss, and a general “unwell” feeling can show up because the immune system is activated.
- Reduced blood flow
- Headache and scalp tenderness can occur when scalp tissues get less blood.
- Jaw pain with chewing (jaw claudication) can occur when jaw muscles are under-supplied during activity.
- Vision changes happen when the circulation to the eye or optic nerve is compromised.
The close relationship with polymyalgia rheumatica
GCA overlaps strongly with polymyalgia rheumatica (PMR), which causes aching and stiffness in the shoulders, hips, and neck—often worst in the morning. Some people develop PMR first and then GCA; others have both together at diagnosis. This matters because PMR symptoms can be a valuable clue when someone’s headache seems “new but hard to explain.”
Why “giant cell” is in the name
Under the microscope, inflamed arteries sometimes show immune cells that fuse into larger “giant” cells. Not every biopsy shows them, and the absence of giant cells does not automatically rule the disease out. The bigger point is that GCA is a tissue-level inflammation problem, not a “blood pressure headache” or a simple migraine.
A calm but important takeaway
GCA is serious because of the risk to vision and major vessels, but it is also highly treatable. The most protective step is not waiting for symptoms to become dramatic—especially if you have a new, unusual headache after age 50 or any visual disturbance.
Causes and risk factors that matter most
Giant cell arteritis does not come from one single trigger. Most experts view it as an immune system misfire in a person who is biologically susceptible, often after an environmental nudge (such as an infection or seasonal immune activation). You did not “cause” it by stress, diet, or a single decision. Still, certain factors strongly shape who gets GCA and how it presents.
Strongest risk factors
These are the patterns clinicians rely on most:
- Age: GCA is uncommon under age 50 and becomes more likely with increasing age.
- Sex: It is diagnosed more often in women than men.
- Ancestry and geography: Rates are higher in people of Northern European descent and in regions where those populations are common.
- History of polymyalgia rheumatica: PMR raises the likelihood that new head or vision symptoms are related to GCA.
Immune and vessel biology: what likely goes wrong
The immune system normally patrols vessel walls quietly. In GCA, immune cells become overactive in the artery wall layers and release inflammatory signals. Those signals can:
- Thicken the vessel wall
- Damage elastic fibers that help the artery stretch smoothly
- Encourage the inner lining to grow inward, narrowing the channel
- Promote clotting in severely narrowed areas
This helps explain why a person can feel systemically ill (from inflammation) while also developing very focal symptoms (from reduced flow to one region).
Genetics and family history
GCA is not usually inherited in a simple pattern like some single-gene conditions. However, family history can matter. If a close relative had GCA or PMR, clinicians may lower their threshold to evaluate symptoms promptly. Genetic influences likely affect how the immune system recognizes threats and how strongly it reacts.
Triggers and timing
Many patients describe a “before-and-after” moment—weeks of fatigue, a lingering viral-like illness, or a sudden new headache that does not match their prior pattern. This does not prove a specific infection caused GCA, but it fits with the idea that immune activation can unmask vulnerability.
Risk factors for more complicated disease
Certain features make clinicians more alert to large-vessel involvement or relapse risk:
- Limb symptoms (arm fatigue with use, arm blood pressure differences, new bruits)
- Unexplained anemia or high inflammation markers without strong head symptoms
- Early imaging showing aorta or branch vessel involvement
- Difficulty tapering steroids without symptom return
A practical insight that helps patients
If you are over 50 and you develop a headache that is “new for you,” the comparison point should be your own history, not someone else’s. A mild headache that feels unfamiliar, paired with jaw pain or shoulder stiffness, can be more meaningful than a severe headache that behaves like your typical migraine. Bring that pattern to your clinician—what’s new, what’s different, and what’s persistent.
Symptoms, especially vision warning signs
GCA symptoms often cluster into three buckets: head and face symptoms, whole-body inflammation symptoms, and large-vessel symptoms. Not everyone has all three. Some people have classic temporal artery tenderness; others mainly have fatigue and arm pain. The most time-sensitive symptoms are those involving vision.
Common symptoms that should raise suspicion
Many people with GCA notice one or more of the following:
- New headache, often at the temples but sometimes diffuse
- Scalp tenderness (pain when combing hair, resting head on a pillow, or wearing a hat)
- Jaw pain or fatigue with chewing (jaw claudication)
- Unexplained fatigue, low-grade fever, night sweats, or weight loss
- Shoulder and hip aching with morning stiffness (PMR symptoms)
- Tongue pain with use, throat discomfort, or facial pain
Headache in GCA can feel “deep” or “pressure-like,” and it often does not respond like a typical tension headache.
Vision symptoms: treat as urgent
GCA can reduce blood flow to the optic nerve or retina. Vision symptoms can be subtle at first and then accelerate. Seek urgent evaluation for:
- Sudden vision loss in one eye (even if it improves)
- Blurred vision that is new and persistent
- Double vision
- A gray curtain or shadow in part of the visual field
- Brief episodes of vision dimming (“like a light switch flickering”)
Even short, reversible episodes can be a warning that a permanent loss is possible without prompt treatment.
Large-vessel symptoms
When larger arteries are involved, symptoms may include:
- Arm fatigue or pain when using the arms (for example, brushing hair or carrying groceries)
- One arm feeling cooler or weaker than the other
- Dizziness, faintness, or neurologic symptoms if blood flow to the brain is affected
- Chest, back, or abdominal pain that is new or unexplained (less common, but important)
- Differences in blood pressure between arms
Large-vessel involvement can also be silent and only discovered on imaging, which is why some clinicians recommend baseline imaging in selected cases.
Complications to understand
GCA complications range from treatable to life-changing. Key ones include:
- Permanent vision loss: The most feared complication, often preventable with early therapy.
- Stroke: Risk can rise when arteries supplying the brain are involved.
- Aortic aneurysm or dilation: Over time, inflammation can weaken the aortic wall.
- Relapse: Symptoms can recur during steroid taper, especially if disease is active or large vessels are involved.
- Medication harm: Long courses of steroids can cause osteoporosis, diabetes, infections, cataracts, and mood changes if not proactively managed.
A useful rule of thumb
Headache plus jaw claudication is a particularly strong combination for GCA. Add any visual symptom, and the situation becomes urgent. If you are unsure whether a symptom “counts,” err on the side of evaluation. In GCA, time matters more than toughness.
How it is diagnosed and why speed matters
Diagnosing GCA is a balance of clinical judgment and targeted testing. The stakes are high because delaying treatment can risk vision, yet unnecessary high-dose steroids also carry real harms. Clinicians aim to confirm the diagnosis quickly while starting treatment promptly when suspicion is strong.
The starting point: history and exam
Clinicians often focus on a few high-yield questions:
- When did the headache start, and how is it different from past headaches?
- Is there jaw pain with chewing, tongue pain, or scalp tenderness?
- Any visual symptoms, even brief ones?
- Any PMR symptoms (shoulder/hip stiffness, trouble raising arms in the morning)?
- Any systemic symptoms (fever, weight loss, night sweats)?
On exam, they may check temporal artery tenderness, reduced pulse, or thickening, and they will assess vision and neurologic status. They also often measure blood pressure in both arms and listen for bruits.
Blood tests: helpful but not perfect
Inflammation markers are commonly elevated:
- ESR (erythrocyte sedimentation rate)
- CRP (C-reactive protein)
Many patients have anemia or higher platelet counts as well. However, normal ESR/CRP does not fully exclude GCA, especially if symptoms are strongly suggestive or if treatment has already begun.
Imaging: faster answers, especially with modern ultrasound
Imaging is increasingly used early, and in many centers it is central to diagnosis:
- Ultrasound of temporal and axillary arteries: Can show a “halo sign,” representing vessel wall swelling. Including axillary arteries helps detect large-vessel involvement.
- MRI or CT angiography: Helpful for extracranial vessels and aorta assessment in selected cases.
- FDG-PET: Can identify inflammation in large vessels, especially when symptoms suggest large-vessel GCA.
Imaging is especially useful when symptoms are atypical, when biopsy is difficult, or when clinicians suspect large-vessel involvement that a temporal biopsy might miss.
Temporal artery biopsy: still important in many cases
A biopsy removes a small segment of the temporal artery for microscopic evaluation. It can provide strong confirmation, but it has limits:
- Inflammation can be “patchy,” so a biopsy may miss affected sections.
- Steroid treatment can reduce diagnostic yield over time, though biopsy can still be informative after treatment has started, especially if performed promptly.
- Biopsy assesses cranial disease better than large-vessel disease.
Many clinicians use a combined approach: immediate treatment when needed, plus imaging and/or biopsy to confirm and guide long-term management.
Why speed matters—and what “fast” should look like
If GCA is strongly suspected, clinicians often start high-dose steroids the same day, especially if there are visual symptoms. The diagnostic process then continues in parallel. From the patient perspective, a good “fast pathway” includes:
- Same-day or next-day clinical evaluation when symptoms are high-risk
- Rapid access to ultrasound or biopsy planning
- Clear instructions about what symptoms require emergency care
- A follow-up plan within days, not weeks
This approach protects vision while still aiming for a confident diagnosis.
Treatment options: steroids, biologics, and tapers
Treatment for GCA is highly effective, but it must be managed carefully. The main goals are to prevent vision loss and stroke, control symptoms, minimize relapse, and reduce treatment side effects—especially those from glucocorticoids (steroids).
Immediate treatment: why steroids are started quickly
High-dose steroids can calm vessel inflammation rapidly and reduce the risk of further ischemic injury. The starting dose depends on severity and whether vision is threatened:
- Without visual symptoms: Many clinicians start high-dose oral prednisone/prednisolone.
- With visual symptoms or very high concern for vision loss: Some use intravenous steroids for a short period before switching to oral therapy.
Steroids can improve headache and systemic symptoms within days. PMR symptoms often improve even faster. If symptoms do not respond as expected, clinicians reconsider the diagnosis or look for complications.
Tapering: the most delicate part of care
A steroid taper is not simply “take less over time.” The taper is a structured experiment: reduce dose slowly enough to prevent relapse, but quickly enough to limit toxicity. Relapses often occur during tapering, especially in the first 1–2 years. A typical plan includes:
- Gradual step-down over months
- More frequent check-ins early and at each major dose reduction
- Repeat labs and symptom review to detect relapse early
- Clear guidance on what to do if symptoms return
A key nuance: inflammation blood tests may become less reliable in people taking certain biologic medications, so clinicians rely more on symptoms and, sometimes, imaging.
Steroid-sparing therapies: reducing long-term steroid harm
Many patients benefit from medications that reduce relapse risk and allow a lower cumulative steroid dose:
- Tocilizumab (IL-6 receptor inhibitor): Often used in patients at higher relapse risk or those who develop steroid toxicity. It has strong evidence for improving sustained remission rates while reducing steroid exposure.
- Methotrexate: Sometimes used as an alternative or add-on, particularly when biologics are not suitable.
- Other immunomodulating approaches may be considered in selected cases under specialist care, especially when disease is refractory.
Managing side effects proactively
Steroids can be life-changing for GCA control—and also for side effects. A strong plan typically includes:
- Bone protection strategies (calcium and vitamin D intake targets, weight-bearing activity when safe, and medication for high-risk patients)
- Diabetes and blood pressure monitoring
- Infection risk reduction (vaccinations timed appropriately, and prompt evaluation for fevers)
- Eye monitoring for cataracts and glaucoma in longer courses
- Stomach protection in selected patients, based on individual risk
Some clinicians also consider low-dose aspirin in certain cases to reduce ischemic risk, but this decision is individualized based on bleeding risk and comorbidities.
What successful treatment feels like
Success is not “never think about it again.” It often looks like:
- Headache and jaw symptoms resolve and stay resolved
- No new visual symptoms
- A taper that continues without repeated “rescues” back to high doses
- Side effects anticipated and managed rather than discovered late
The most important message: if you are told to start steroids urgently for suspected GCA, that is a protective step. The rest of treatment is then about precision—confirming diagnosis, tapering safely, and preventing complications.
Management, prevention, and when to seek urgent care
Living with GCA is a combination of medical follow-up and practical self-management. Most people can return to meaningful routines, but the condition rewards attentiveness—especially during the first year, when relapse risk and medication side effects are highest.
Follow-up that actually reduces risk
A useful follow-up plan is specific and predictable. It often includes:
- Regular visits during the first months of treatment and at key taper milestones
- Symptom check-ins that focus on headache pattern changes, jaw pain, PMR symptoms, and any vision concerns
- Periodic labs (ESR/CRP and blood counts), with the understanding that labs may be less informative on certain biologic therapies
- Blood pressure, glucose, and weight monitoring during steroid therapy
- Bone health assessment and prevention planning
If large-vessel involvement is suspected or confirmed, clinicians may recommend baseline imaging of the aorta and major branches and repeat imaging later to screen for dilation or aneurysm development.
Everyday habits that support recovery
No lifestyle step replaces medication, but several can improve resilience and reduce complications:
- Medication routines: Take steroids in the morning when possible to reduce sleep disruption, and use a consistent schedule.
- Muscle and bone support: Aim for safe, regular walking or gentle strength work when approved; inactivity accelerates muscle loss on steroids.
- Nutrition that fits real life: Prioritize protein, fiber, and adequate calcium; limit highly processed foods that worsen fluid retention and blood sugar swings.
- Sleep protection: Steroids can disrupt sleep; a stable bedtime routine and morning dosing can help.
- Infection awareness: Report fevers early; do not ignore persistent cough, urinary symptoms, or skin infections while immunosuppressed.
Preventing long-term cardiovascular risk
GCA is an inflammatory vascular disease, and steroids can raise blood pressure, cholesterol, and blood sugar. Ask your clinician about a simple cardiovascular plan:
- Blood pressure targets and home monitoring if needed
- Lipid and glucose screening during and after therapy
- Smoking cessation support if relevant
- Exercise guidance tailored to your symptoms and vessel involvement
When to seek urgent care
Treat these as urgent—same day evaluation or emergency care depending on severity:
- Any new vision change, even if it lasts minutes
- New severe headache that is different from your recent pattern
- Jaw claudication that is new or worsening
- Stroke-like symptoms: facial droop, arm weakness, trouble speaking, sudden imbalance
- Chest pain, severe back pain, or shortness of breath that is new and concerning
- High fever or chills while on immunosuppressive therapy
- Severe steroid side effects such as confusion, severe mood changes, or uncontrolled blood sugar symptoms
A steady perspective
Many people with GCA worry that every twinge means relapse. A more helpful approach is to define your “personal red flags” with your care team—specific symptoms and thresholds that matter most for you. That clarity reduces anxiety and improves safety. Over time, most patients learn the difference between ordinary aches and symptoms that deserve a call, and they regain confidence in their bodies again.
References
- 2021 American College of Rheumatology/Vasculitis Foundation Guideline for the Management of Giant Cell Arteritis and Takayasu Arteritis 2021 (Guideline)
- EULAR recommendations for the use of imaging in large vessel vasculitis in clinical practice: 2023 update 2024 (Guideline)
- Current management of giant cell arteritis and its complications 2024 (Review)
- Trial of Tocilizumab in Giant-Cell Arteritis 2017 (RCT)
Disclaimer
This article is for educational purposes only and does not replace medical advice, diagnosis, or treatment from a qualified clinician. Giant cell arteritis can threaten vision and cause serious vascular complications, and treatment decisions depend on your symptoms, exam findings, imaging, lab results, and overall health. If you develop sudden vision changes, stroke-like symptoms, severe new headache, jaw pain with chewing, chest or back pain, fainting, or severe shortness of breath, seek urgent medical care immediately.
If you found this article helpful, please share it on Facebook, X (formerly Twitter), or any platform you prefer, and follow us on social media. Your support through sharing helps our team continue producing reliable, high-quality health content.