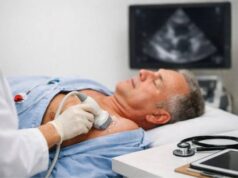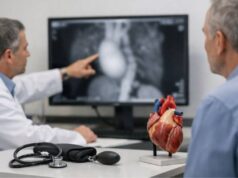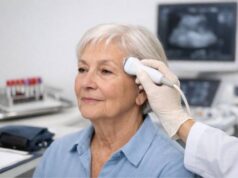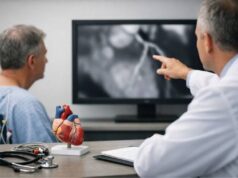
Giant cell myocarditis is a rare, aggressive form of myocarditis (inflammation of the heart muscle). It can move fast—sometimes over days—turning mild shortness of breath or chest discomfort into severe heart failure or dangerous rhythm problems. People are often healthy before symptoms begin, which makes the sudden change feel especially unsettling.
The encouraging truth is that outcomes improve when clinicians recognize the pattern early and start the right treatment quickly. Diagnosis usually depends on a heart tissue sample, and care often involves both heart-failure support and medicines that calm an overactive immune response. Because the condition can affect the heart’s electrical system, patients may also face arrhythmias (abnormal heart rhythms) that require urgent monitoring.
This article explains what giant cell myocarditis is, why it happens, how it shows up, how it is confirmed, and what treatment and long-term management typically look like.
Table of Contents
- What giant cell myocarditis does to the heart
- Causes and risk factors, including autoimmune links
- Symptoms and complications you should not ignore
- How doctors diagnose it and why biopsy matters
- Treatment: immunosuppression, support, and transplant options
- Living with recovery, monitoring, and when to seek urgent care
What giant cell myocarditis does to the heart
Giant cell myocarditis (GCM) is an inflammatory disease where immune cells attack the heart muscle. The “giant cell” name comes from what pathologists sometimes see under the microscope: unusually large, fused immune cells within areas of active injury. The key clinical point is not the label—it is the speed and intensity of damage. In many patients, the heart’s pumping strength drops quickly, and the electrical system that controls heartbeat can become unstable.
How it disrupts heart function
GCM tends to cause a mix of problems that can overlap and amplify each other:
- Weakening of the heart’s squeeze (pump failure): The left ventricle may struggle to circulate blood, leading to fluid buildup in lungs and severe fatigue.
- Inflammation-related stiffness: Even if squeezing looks “okay” early, the heart can fill poorly, causing breathlessness with minimal activity.
- Electrical system injury: Inflammation can irritate or destroy conduction pathways, leading to slow heart rhythms (heart block) or fast, dangerous rhythms from the ventricles.
Because the heart is both a pump and an electrical organ, symptoms can swing between “heart failure” and “rhythm emergency,” sometimes within the same week.
Fulminant versus subacute patterns
Clinicians often describe GCM presentations as:
- Fulminant: Sudden, dramatic decline—rapid heart failure, cardiogenic shock, or life-threatening arrhythmias.
- Subacute: Gradual worsening over weeks with persistent fatigue, shortness of breath, and intermittent palpitations before a turning point.
Neither pattern is “milder” in terms of importance. A slower onset can still end in a critical event if diagnosis is delayed.
Why it can be mistaken for other conditions
Early symptoms—chest tightness, shortness of breath, fatigue—can resemble viral myocarditis, coronary disease, panic symptoms, or asthma. Rhythm findings can look like other inflammatory heart conditions, particularly cardiac sarcoidosis. This is one reason tissue diagnosis is often essential: treatment strategy and urgency change when GCM is on the table.
A practical way to think about it
If typical myocarditis is a fire that might smolder, GCM is more like a fire that can leap rooms. Many people do not have a long “warning runway.” That is why clinicians move quickly with monitoring, biopsy planning, and early immune-targeting therapy once GCM is suspected.
Causes and risk factors, including autoimmune links
GCM is usually considered an immune-mediated condition—meaning the immune system misidentifies part of the heart as a threat and mounts an attack. In many cases, no single trigger is found, and the term “idiopathic” is used. Still, several associations appear often enough that clinicians actively look for them.
Commonly reported associations
GCM can occur on its own, but it may also appear alongside:
- Autoimmune diseases such as inflammatory bowel disease, thyroid autoimmunity, rheumatoid arthritis, or other immune-driven conditions
- Thymoma (a tumor of the thymus gland), which can disrupt immune “training” and tolerance
- Drug-related immune reactions in rare situations (for example, severe hypersensitivity syndromes)
- Cancer immunotherapy exposure (immune checkpoint inhibitors), where an activated immune system can inflame the heart; in some cases the biopsy pattern can resemble or include giant cells
These links do not mean that everyone with GCM has cancer or a tumor. They simply reflect the theme: GCM tends to appear when immune regulation is off balance.
Who is at risk
Unlike some vascular conditions tied closely to older age, GCM can affect adults across a broad range, including young and middle-aged people. Risk is not usually defined by lifestyle. Many patients are active and previously well. That “out of nowhere” quality can delay care because people try to push through symptoms they would normally dismiss as stress or a lingering respiratory infection.
What might trigger the immune attack
In many immune conditions, the story is “susceptibility plus a spark.” Possible sparks include:
- A recent infection that broadly activates immune pathways
- A new medication or immune therapy
- A period of immune system instability (for example, after major illness)
For most patients, clinicians cannot identify a single culprit with certainty. What matters more is recognizing the syndrome early and treating it effectively.
Why risk factors matter for treatment planning
Knowing an associated condition can shape decisions such as:
- How aggressively to search for extracardiac disease (for example, signs of sarcoidosis)
- Whether an oncology team should coordinate care if checkpoint inhibitors are involved
- Which immunosuppressive combinations are most appropriate
- How long immune therapy might be needed to reduce relapse risk
A grounded takeaway
If you are diagnosed with GCM, it is reasonable to ask, “Why did this happen to me?” In many cases, medicine cannot offer a single clean cause. What it can offer is a practical framework: look for associated immune conditions, treat the heart urgently, and reduce the chance of recurrence with structured follow-up.
Symptoms and complications you should not ignore
GCM symptoms often reflect two threats at once: declining pump function and electrical instability. Some people present mainly with heart failure; others present with rhythm problems first. Because the condition can evolve quickly, the “pattern over time” is as important as any single symptom.
Early and common symptoms
Many patients notice a cluster that worsens over days to weeks:
- Shortness of breath with activity, then at rest
- Chest pressure or discomfort (not always sharp pain)
- Unusual fatigue, reduced exercise tolerance, or “I can’t do my normal day”
- Palpitations or a sensation of skipped, racing, or pounding beats
- Lightheadedness, near-fainting, or fainting
- Swelling in legs or rapid weight gain from fluid retention
A key red flag is rapid progression—symptoms that noticeably worsen from one day to the next.
Rhythm-related warning signs
Inflammation can disrupt the heart’s conduction system. Seek urgent evaluation for:
- Fainting or near-fainting, especially with palpitations
- Slow pulse with dizziness or confusion
- Episodes of sudden rapid heartbeat with chest pressure or breathlessness
- New heart block found on an ECG, even if you “feel okay”
People sometimes interpret these episodes as anxiety. With GCM, it is safer to assume the heart may be involved until proven otherwise.
Heart failure and shock symptoms
As pump function drops, circulation can become inadequate. Emergency symptoms include:
- Severe shortness of breath, inability to lie flat, or coughing up frothy sputum
- Cold, clammy skin; blue lips; confusion; extreme weakness
- Very low blood pressure or inability to stay awake
- Marked decrease in urine output
These can signal cardiogenic shock, which requires immediate hospital-level support.
Complications clinicians watch closely
Complications are not rare in GCM, which is why care often happens in specialized centers:
- Sustained ventricular arrhythmias that can cause sudden cardiac arrest
- Advanced heart block requiring temporary or permanent pacing
- Cardiogenic shock requiring medications or mechanical support
- Thromboembolism (clots) when the heart is weak and blood flow slows
- Need for transplant if heart damage is extensive or unresponsive to therapy
- Relapse during tapering of immune-suppressing medicines
A practical self-check that helps
If you are experiencing symptoms that could fit GCM, focus on three questions when deciding urgency:
- Are symptoms new and escalating quickly?
- Are there fainting spells, severe palpitations, or marked breathlessness?
- Is your usual daily activity suddenly impossible?
A “yes” to any of these should push you toward urgent evaluation, not watchful waiting.
How doctors diagnose it and why biopsy matters
GCM is a diagnosis where speed and precision both matter. Clinicians need to stabilize the patient and determine the exact myocarditis type, because treatment choices differ substantially between GCM, lymphocytic myocarditis, eosinophilic myocarditis, and cardiac sarcoidosis. The most definitive step is often an endomyocardial biopsy—sampling small pieces of heart tissue through a catheter.
Typical first-line testing
Most evaluations begin with tests that assess damage, function, and rhythm risk:
- ECG: may show heart block, ventricular arrhythmias, or nonspecific changes
- Blood tests: troponin (heart injury marker), natriuretic peptides (heart strain), inflammatory markers, and organ-function tests
- Echocardiogram: assesses pumping strength, chamber size, valve function, and fluid around the heart
- Continuous rhythm monitoring: because dangerous rhythms can occur unpredictably
- Cardiac MRI: can show inflammation and scarring patterns, and helps rule in myocarditis broadly
These tests often raise suspicion but usually cannot confirm GCM on their own.
Why biopsy is often essential
Biopsy provides information that imaging cannot reliably provide:
- The specific inflammatory pattern (giant cells, degree of necrosis, cell types)
- Whether there are features that favor sarcoidosis or other histologic diagnoses
- Clues that guide immunosuppressive choice and intensity
Because heart inflammation can be patchy, biopsy sometimes requires multiple samples, and occasionally repeat biopsy if clinical suspicion remains high but the first sample is nondiagnostic.
How clinicians decide who needs urgent biopsy
Biopsy is more likely when a person has “high-risk myocarditis” features such as:
- Rapidly worsening heart failure
- Ventricular arrhythmias or high-grade heart block
- Cardiogenic shock or need for intensive care support
- Inadequate explanation for the severity of symptoms based on imaging alone
In these situations, waiting weeks for “watch and see” is not appropriate. Clinicians push for a diagnosis that can justify aggressive immune therapy.
Differential diagnosis: what GCM can resemble
Two common look-alikes are important:
- Cardiac sarcoidosis: can also cause ventricular arrhythmias and conduction disease; treatment overlaps but long-term strategy can differ.
- Eosinophilic myocarditis: may require different immune therapy and is often linked to drug reactions or specific systemic diseases.
A careful history—new medications, systemic symptoms, immune conditions—and targeted testing help narrow the field, but tissue frequently settles the question.
What patients can expect during diagnostic hospitalization
Many patients feel overwhelmed by the pace. A typical pathway may include:
- Stabilization (oxygen, diuretics, blood pressure support if needed)
- Continuous rhythm monitoring and rapid imaging
- Biopsy planning and performance, often within days
- Early initiation of therapy once suspicion is strong, adjusted as pathology returns
If the team recommends transfer to a tertiary center, it often reflects the need for biopsy expertise, advanced heart failure support, or transplant-level resources—not a sign that recovery is impossible.
Treatment: immunosuppression, support, and transplant options
Treatment for GCM has two pillars: immediate cardiac stabilization and immune-directed therapy to stop ongoing injury. Because GCM can deteriorate quickly, clinicians often treat in parallel—support the heart first while confirming the diagnosis and tailoring immunosuppression.
Immediate cardiac support
Support depends on severity and may include:
- Heart failure therapy: diuretics for congestion, vasodilators when appropriate, and guideline-based medications if blood pressure and kidney function allow
- Rhythm control: antiarrhythmic medicines, temporary pacing for heart block, or urgent procedures for unstable arrhythmias
- Intensive care support: inotropes (medicines that strengthen contraction) and vasopressors (support blood pressure) in shock
- Mechanical circulatory support: devices such as intra-aortic balloon pump, percutaneous ventricular assist devices, or ECMO when circulation is critically compromised
Mechanical support can be a bridge—either to recovery while inflammation is treated, or to transplant evaluation if the heart does not rebound.
Immunosuppression: stopping the immune attack
Most contemporary approaches use combination immunosuppression, because steroids alone often do not provide durable control. Regimens vary by center and patient factors, but commonly include:
- High-dose corticosteroids early (sometimes intravenous “pulse” dosing in severe cases, then high-dose oral therapy)
- A calcineurin inhibitor such as cyclosporine or tacrolimus
- An additional agent in selected cases, such as azathioprine or mycophenolate mofetil
- Alternative or add-on therapies for refractory disease in specialist hands (for example, targeted biologic therapies)
The goal is to halt myocardial destruction quickly, then taper in a controlled way once stability is achieved.
Device therapy and transplant considerations
Because rhythm risk can persist even as inflammation improves, clinicians may consider:
- Temporary wearable defibrillator during early recovery in selected patients
- Implantable cardioverter-defibrillator (ICD) if sustained ventricular arrhythmias occur or risk remains high after initial stabilization
- Permanent pacemaker if conduction disease does not recover
For patients with severe, persistent dysfunction despite therapy, heart transplantation may be lifesaving. Importantly, GCM can recur in the transplanted heart, so transplant teams typically plan careful surveillance and immunosuppression strategies.
What to expect during treatment
Patients often notice:
- Symptom improvement (breathlessness, fatigue) over days to weeks if the heart begins to recover
- A prolonged recovery period even after stabilization, because heart muscle needs time to remodel
- Close lab monitoring for medication side effects (kidney function, blood counts, liver tests, drug levels)
- A structured plan for tapering steroids and other immune therapies to reduce relapse risk
A helpful mindset is that GCM treatment is not one decision; it is a sequence of decisions that evolve with rhythm stability, imaging, biopsy findings, and functional recovery.
Living with recovery, monitoring, and when to seek urgent care
Recovery after GCM can be physically and emotionally intense. Even when the heart improves, patients may feel fragile for a time, and medications can introduce their own burdens. A strong plan focuses on relapse prevention, rhythm safety, medication side effects, and rebuilding strength.
Follow-up that reduces risk
Most patients need coordinated care involving cardiology (often advanced heart failure) and an immunology-aware specialist team. Follow-up commonly includes:
- Frequent visits early (every 1–4 weeks), then spaced out as stability improves
- Symptom review focused on breathlessness, palpitations, dizziness, and exercise tolerance
- Repeat echocardiograms to track function and chamber size
- Rhythm surveillance (Holter monitor, device checks, or telemetry depending on risk)
- Lab monitoring for immunosuppressant toxicity and steroid effects (glucose, lipids, kidney function, blood counts)
Some centers use follow-up biopsy or advanced imaging in selected patients, especially if symptoms recur or tapering triggers concern.
Medication safety: what patients can do day to day
Immunosuppression works best when it is taken consistently and monitored carefully. Practical habits that help include:
- Keep a single updated medication list and bring it to every visit
- Take medicines at the same time daily; do not “double up” without instructions
- Ask which over-the-counter drugs and supplements are unsafe with your regimen
- Track blood pressure, weight, and resting pulse at home, especially during early recovery
- Discuss vaccination timing and infection precautions with your clinicians
Steroids can affect sleep, mood, blood sugar, bones, and muscle strength. If you feel “not like yourself,” say so early—dose adjustments and supportive care can make treatment more tolerable.
Returning to activity
A common mistake is to either do too much too soon or avoid activity entirely. Many patients benefit from:
- Gradual, structured increases in walking and light activity
- Cardiac rehabilitation when clinicians approve it
- Clear guidance about driving restrictions if fainting or dangerous arrhythmias occurred
- A plan for returning to work that respects fatigue and immune suppression risks
When to seek urgent care
Because GCM can relapse or cause rhythm events, treat these as urgent:
- Fainting, near-fainting, or severe dizziness
- Rapid, sustained palpitations with chest pressure or shortness of breath
- New or worsening breathlessness at rest, or inability to lie flat
- Sudden swelling, rapid weight gain over a few days, or reduced urine output
- Chest pain that is severe, persistent, or accompanied by sweating or nausea
- Fever, chills, or signs of infection while on immunosuppression
- New confusion, profound weakness, or very low blood pressure symptoms
A steadier long-term outlook
Many people improve substantially with modern combination therapy, but the course can be unpredictable. The most protective approach is proactive: build a follow-up rhythm plan, taper immune therapy cautiously, and treat new symptoms as data—not as a personal failure. With the right monitoring and support, many patients regain meaningful quality of life, even if their recovery includes detours.
References
- Giant Cell Myocarditis: An Updated Review of Pathogenesis, Clinical Presentation, and Modern Management Approaches 2025 (Review)
- Management of Patients With Giant Cell Myocarditis: JACC Review Topic of the Week 2021 (Review)
- Immunomodulatory Therapy for Giant Cell Myocarditis: A Narrative Review 2023 (Review)
- 2024 ACC Expert Consensus Decision Pathway on Strategies and Criteria for the Diagnosis and Management of Myocarditis: A Report of the American College of Cardiology Solution Set Oversight Committee 2025 (Guideline)
Disclaimer
This article is for educational purposes only and does not provide medical advice, diagnosis, or treatment. Giant cell myocarditis can be life-threatening and may require urgent hospitalization, specialized testing, and intensive therapies. If you have chest pain, fainting, severe shortness of breath, rapid or irregular heartbeat, new confusion, or signs of shock—or if you develop fever or infection symptoms while taking immunosuppressive medicines—seek emergency care immediately. Treatment decisions must be individualized by a qualified clinical team based on your symptoms, exam findings, imaging, biopsy results, and overall health.
If you found this article helpful, please share it on Facebook, X (formerly Twitter), or any platform you prefer, and follow us on social media. Your support through sharing helps our team continue producing reliable, high-quality health content.