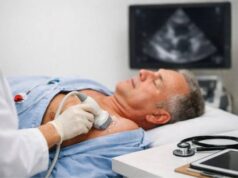
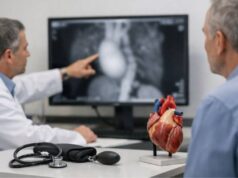
A giant coronary artery aneurysm is an unusually large bulge in one of the heart’s own arteries. These arteries supply oxygen to the heart muscle, so size is not the only concern—shape and blood flow matter just as much. When a coronary aneurysm becomes “giant,” blood can swirl and slow inside it, raising the chance of clotting, blockage downstream, or (rarely) pressure on nearby heart structures.
Many people have no symptoms until a complication happens. Others develop chest discomfort, shortness of breath, or signs of a heart attack. Because causes vary—from childhood inflammation to adult atherosclerosis or prior heart procedures—care needs to be tailored, not one-size-fits-all.
This guide explains what “giant” means, why these aneurysms form, how they are found, and what treatment and long-term monitoring usually involve.
Table of Contents
- What a giant coronary aneurysm means
- Why they happen and who is at risk
- Symptoms and complications to watch for
- How it’s diagnosed and sized accurately
- Treatment: medicines, stents, and surgery
- Long-term management, prevention, and when to seek care
What a giant coronary aneurysm means
A coronary artery aneurysm is a localized widening of a coronary artery segment—most commonly defined as a diameter at least 1.5 times the size of an adjacent “normal” segment. The word “giant” is used when the enlargement is far beyond typical aneurysms and the risks shift from “possible” to “probable” complications.
How “giant” is defined in practice
There is no single worldwide cutoff, so clinicians use context:
- Adults: Many publications define a giant coronary aneurysm as >20 mm in diameter, or more than 4 times the diameter of the reference vessel.
- Children (often after Kawasaki disease): “Giant” is frequently defined as an absolute diameter ≥8 mm or a Z-score ≥10 (a body-size-adjusted measurement).
Because these definitions differ, the most useful question is not “Does it meet a label?” but “Is it large enough that blood flow is abnormal and clot risk is high?”
Why size alone is not the whole story
Two aneurysms of the same diameter can behave very differently depending on:
- Shape:
- Saccular (a pouch with a narrower neck) tends to promote stagnation and clot formation and may carry a higher risk of rupture in other vascular beds.
- Fusiform (a longer, spindle-shaped enlargement) can involve a larger section of vessel and may be harder to exclude with a single device.
- Location: Left main or proximal arteries can have higher stakes because they supply large territories of heart muscle.
- Associated narrowing: Some aneurysms sit next to tight stenoses. Turbulence and low-flow zones make clotting more likely.
- Presence of a fistula: Rarely, an aneurysm connects to a heart chamber or vessel, changing flow patterns and treatment options.
What “giant” means for blood flow
In a normal coronary artery, blood moves forward in a streamlined way. In a giant aneurysm, the widened space can create a “whirlpool” effect where blood circulates in eddies instead of moving efficiently downstream. That increases the chance of:
- In-aneurysm thrombus (clot) formation
- Distal embolization (a clot fragment travels and blocks smaller arteries)
- Myocardial ischemia (too little oxygen to the heart muscle), even without classic plaque blockage
A useful mental model
Think of a giant coronary aneurysm less like a simple bulge and more like a high-risk flow environment. The goal of care is to prevent clot-related events, detect narrowing early, and decide when a mechanical solution (stent, coil, surgery) offers more benefit than medication alone.
Why they happen and who is at risk
Giant coronary artery aneurysms can be congenital (present from birth) or acquired (develop later). In real-world practice, most giant aneurysms are acquired, but the “why” depends heavily on age and clinical history.
Common causes by age group
Children and young adults (inflammatory origins are common):
- Kawasaki disease: The leading cause of coronary aneurysms in children in many regions. Giant aneurysms are more likely when treatment is delayed or inflammation is severe.
- Other vasculitides: Conditions such as polyarteritis nodosa can involve medium-sized arteries and, rarely, coronaries.
- Congenital coronary anomalies: Uncommon, but structural weakness can predispose to dilation.
Middle-aged and older adults (degenerative and iatrogenic causes become more common):
- Atherosclerosis: Chronic inflammation and degeneration of the arterial wall can weaken the media (the vessel’s muscular layer), leading to dilation.
- Post-procedural injury: Coronary interventions—such as stent placement, atherectomy, or balloon angioplasty—can, in rare cases, lead to aneurysm formation at the treated segment.
- Infections (rare): Certain infections can damage the arterial wall (sometimes called “mycotic” aneurysms), especially in immunocompromised settings.
Medical conditions that raise suspicion
Even when a single cause is not obvious, clinicians look for clues that suggest a vulnerable vessel wall:
- Connective tissue disorders (for example, Marfan or vascular Ehlers-Danlos syndromes), which can reduce structural integrity of arteries
- Systemic inflammatory disease (autoimmune or vasculitic conditions)
- History of unexplained fevers or rashes in childhood (a possible missed Kawasaki pattern)
- Prior coronary bypass or stenting near the aneurysm site
Risk factors for complications (not just formation)
It helps to separate “risk factors for developing an aneurysm” from “risk factors for an aneurysm causing harm.” Complication risk tends to rise with:
- Very large diameter (especially “giant” ranges)
- Slow-flow zones or visible clot within the aneurysm
- Multivessel involvement (more than one artery affected)
- Associated stenosis that limits downstream flow
- History of myocardial infarction, angina, or embolic events
- Aneurysms involving the left main coronary artery or critical proximal segments
Why understanding the cause matters
Cause influences treatment in concrete ways:
- If the aneurysm is part of an active inflammatory disease, controlling inflammation can be as important as antithrombotic therapy.
- If it formed after an intervention, the structure may be more amenable to a covered stent or targeted exclusion.
- If atherosclerosis is central, aggressive risk-factor management (lipids, blood pressure, smoking cessation) becomes a major pillar of care.
A practical takeaway
Many patients ask, “Did I do something to cause this?” Often, the answer is no. Giant coronary aneurysms frequently arise from conditions that are not lifestyle-driven. What is actionable is identifying the likely driver and matching the prevention strategy—clot prevention, inflammation control, or mechanical repair—to the aneurysm’s behavior and risk profile.
Symptoms and complications to watch for
A giant coronary artery aneurysm may be silent for years, but when symptoms appear, they often reflect blood-flow disruption or clot-related events rather than the aneurysm “bursting.” Rupture can occur but is uncommon compared with thrombosis, embolization, and progressive narrowing.
Common symptom patterns
Many patients fall into one of these categories:
- No symptoms: The aneurysm is found incidentally on CT coronary angiography, invasive angiography, or imaging done for another reason.
- Stable exertional symptoms: Chest pressure, shortness of breath, or reduced exercise capacity due to downstream ischemia, sometimes from associated stenosis or microvascular dysfunction.
- Acute coronary syndrome: A heart attack or unstable angina caused by a clot forming within the aneurysm or embolizing downstream.
Symptoms that can point to coronary ischemia include:
- Chest pressure, tightness, or heaviness (often with exertion, sometimes at rest)
- Shortness of breath out of proportion to activity
- Unexplained nausea, sweating, or lightheadedness (especially in older adults)
- Fatigue that is sudden and not typical for the person
Key complications clinicians worry about
1) Thrombosis inside the aneurysm
Blood can stagnate in a large, widened segment. That makes clot formation more likely. A clot may:
- partially obstruct flow within the aneurysm, or
- break off and block smaller branches, causing a heart attack.
2) Distal embolization
Even if the aneurysm itself remains open, small clot fragments can travel and lodge downstream. This can produce:
- episodic chest pain,
- transient ECG changes, or
- “patchy” infarcts that can be missed without careful evaluation.
3) Progressive stenosis and late scarring
Some aneurysms, especially those following inflammatory disease, can evolve toward:
- localized narrowing at the inlet/outlet of the aneurysm,
- calcification, and
- chronic ischemia.
4) Compression of nearby structures (uncommon, but possible in very large aneurysms)
Extremely large aneurysms can press on adjacent cardiac structures, sometimes causing atypical symptoms such as persistent breathlessness or rhythm irritation.
5) Rupture (rare)
Rupture is discussed often because it is alarming, but it is typically not the most common event in coronary aneurysms. Still, clinicians take very rapid enlargement seriously.
Why symptom timing matters
A useful clue is change over time:
- Stable, predictable exertional discomfort suggests chronic ischemia or associated plaque disease.
- Sudden, severe chest pain or rapidly worsening shortness of breath raises concern for an acute clot event.
When symptoms are not “classic”
Some people—particularly older adults, patients with diabetes, and women—can have less typical signs of ischemia, such as shortness of breath, jaw discomfort, back discomfort, or sudden fatigue without intense chest pain. With a known giant coronary aneurysm, these symptoms deserve a low threshold for evaluation.
A grounded takeaway
The most important complication to prevent is clot-related myocardial infarction. That is why many treatment plans emphasize antithrombotic strategies and surveillance, even when the aneurysm itself is not causing daily symptoms.
How it’s diagnosed and sized accurately
Diagnosis has two goals: confirm the aneurysm and measure it accurately, then understand the risk environment—including flow patterns, clot presence, and any nearby narrowings. Because management depends on details, clinicians often combine imaging methods rather than relying on a single test.
First steps: history, exam, and basic testing
A clinician typically starts by clarifying:
- prior Kawasaki disease or severe childhood febrile illness,
- autoimmune/inflammatory history,
- prior coronary stents or cardiac surgery,
- symptoms suggestive of angina or prior myocardial infarction.
Basic tests often include:
- ECG (for prior infarct patterns or active ischemia)
- cardiac biomarkers when symptoms are acute
- lipid profile and diabetes screening to assess atherosclerosis risk
Imaging options and what each adds
Echocardiography
- Especially useful in children and young adults after Kawasaki disease.
- Can visualize proximal coronary segments and track aneurysm size over time.
- Also assesses heart function and valve performance.
CT coronary angiography (CTCA)
- Excellent for defining anatomy, diameter, length, calcification, and relation to nearby structures.
- Helpful for surgical or interventional planning.
- Can detect mural thrombus (clot along the wall) in many cases.
Invasive coronary angiography
- Provides real-time lumen imaging and allows intervention if needed.
- May underestimate aneurysm size if thrombus lines the wall (you see the flowing channel, not the full outer diameter).
Intravascular imaging (IVUS or OCT)
- These catheter-based tools can clarify whether an aneurysm is “true” (wall layers intact) or a pseudoaneurysm (wall disruption).
- They help define landing zones for covered stents and identify hidden stenoses.
Stress testing for ischemia
When symptoms are stable but concerning, clinicians may use stress echocardiography, nuclear perfusion imaging, or stress MRI to see whether the aneurysm and any associated stenosis are limiting blood supply during exertion.
How “giant” is measured and tracked
Sizing is not only a single diameter. Clinicians often document:
- maximum diameter (in mm),
- length of involved segment,
- presence and extent of thrombus,
- involvement of multiple branches,
- changes over time (growth rate is crucial).
In Kawasaki-related disease, Z-scores may be used to adjust measurements for body surface area—especially important in growing children.
Diagnosing the cause
Cause is often inferred from the combination of:
- age and history (childhood Kawasaki versus adult atherosclerosis),
- location and morphology (proximal, diffuse ectasia, post-stent focal aneurysm),
- evidence of systemic inflammation or connective tissue disease.
Sometimes the cause remains uncertain, but risk stratification can still be precise if imaging is detailed.
A practical takeaway
Accurate measurement is not academic—it changes therapy. A plan that is appropriate for a moderate aneurysm may be inadequate for a giant aneurysm with slow flow or thrombus. If your clinicians recommend repeat imaging at defined intervals, it is usually because the “trajectory” (stable vs enlarging) is one of the strongest predictors of what to do next.
Treatment: medicines, stents, and surgery
Treatment aims to prevent heart attack, reduce symptoms, and address aneurysms that are enlarging or mechanically dangerous. Because randomized trials are limited, management often relies on best-available evidence, expert consensus, and individualized risk assessment.
Medication strategies: preventing clots and controlling drivers
Antithrombotic therapy is often the backbone of care, especially for giant aneurysms where flow is slow.
Depending on anatomy and clinical history, clinicians may consider:
- Antiplatelet therapy (commonly low-dose aspirin) to reduce platelet-driven clotting
- Anticoagulation (such as warfarin or low-molecular-weight heparin in certain settings) when aneurysm size, thrombus presence, or prior events suggest high risk
- Dual antiplatelet therapy (aspirin plus another antiplatelet agent) in selected high-risk scenarios, sometimes alongside anticoagulation when risk is extreme and bleeding risk is acceptable
In Kawasaki-related giant aneurysms, combination approaches (antiplatelet plus anticoagulation) are frequently used when Z-scores are very high or absolute diameters reach “giant” thresholds.
If atherosclerosis contributes, clinicians also typically emphasize:
- high-intensity lipid lowering (often a statin),
- blood pressure control,
- diabetes optimization,
- smoking cessation (if applicable).
When an intervention is considered
Mechanical treatments are considered when the aneurysm’s risk profile outweighs procedural risks. Common triggers include:
- Symptoms of ischemia not controlled with medication
- Evidence of recurrent thrombosis or embolization
- Rapid enlargement or extremely large size
- Associated fistula or compression of nearby structures
- Coexisting severe stenosis requiring revascularization
Percutaneous options (catheter-based)
For selected aneurysms—especially those with a suitable shape and “landing zones”—interventional cardiologists may use:
- Covered stents to exclude the aneurysm from the circulation while keeping the artery open
- Coils, plugs, or occlusion devices to close a feeding segment in specific anatomical scenarios
- Stent-in-stent strategies in complex lesions, sometimes to improve healing characteristics and reduce leak risk
These approaches can be attractive in patients who are high surgical risk, or when the aneurysm is relatively short.
Surgical options
Surgery is often considered when the aneurysm is very large, involves complex branching, or coexists with disease that needs bypass. Surgical approaches may include:
- Coronary artery bypass grafting (CABG) to reroute blood around the diseased segment
- Aneurysm exclusion or ligation (closing the aneurysm’s inflow/outflow) alongside bypass
- Resection in rare cases where anatomy allows safe removal
Surgical decision-making is highly anatomy-driven, which is why detailed CT and angiographic planning matters.
Balancing clot prevention and bleeding risk
Aggressive antithrombotic therapy can reduce ischemic events but increases bleeding risk. Clinicians typically individualize therapy by considering:
- history of bleeding or anemia,
- age and fall risk,
- need for other blood thinners (for example, atrial fibrillation),
- planned procedures.
A practical takeaway
For many patients, the best plan is staged: start with robust clot prevention and risk-factor control, then reassess with follow-up imaging and symptom tracking. In others—especially with very large, symptomatic, or growing aneurysms—early mechanical exclusion or surgery may offer the clearest protection against future events.
Long-term management, prevention, and when to seek care
Living with a giant coronary artery aneurysm is usually less about daily symptoms and more about staying ahead of risk. A strong long-term plan combines medical therapy adherence, structured monitoring, and clear rules for when to seek urgent evaluation.
Follow-up and surveillance imaging
Your clinician may recommend periodic imaging to confirm stability and detect new narrowing or clot. The interval depends on:
- aneurysm size and location,
- whether there is thrombus,
- whether you have had prior ischemic events,
- whether the aneurysm is stable or enlarging.
Common elements of follow-up can include:
- echocardiography (especially in Kawasaki-related disease),
- CT coronary angiography at intervals to track size and anatomy,
- stress testing when symptoms suggest ischemia or when clinicians need functional risk information,
- device checks if you have a stent or surgical grafts.
A useful concept is the trend line: a stable aneurysm over multiple studies is managed differently from one that grows measurably over months.
Medication adherence and safety habits
If you are on antiplatelet or anticoagulant therapy, consistency is protective. Practical habits that help include:
- keeping a single updated medication list,
- informing every clinician and dentist about blood thinners before procedures,
- avoiding over-the-counter medications that increase bleeding risk unless approved,
- reporting signs of bleeding early (black stools, unusual bruising, prolonged nosebleeds).
If warfarin is part of your plan, regular INR monitoring and attention to diet-medication interactions become central.
Lifestyle and prevention: what still matters
Even when the aneurysm was not caused by lifestyle factors, prevention still helps reduce downstream risk:
- Aim for heart-healthy activity as advised by your clinician, often starting with moderate, steady aerobic exercise rather than sudden intense bursts.
- Prioritize sleep and stress management because they influence blood pressure and symptom perception.
- Treat blood pressure, lipids, and diabetes as “secondary prevention,” especially if atherosclerosis plays any role.
- Avoid tobacco exposure; it increases clotting tendency and vascular inflammation.
Special situations worth discussing early
Bring these topics up proactively rather than waiting for a problem:
- Planned surgeries or invasive procedures (how to manage blood thinners safely)
- Pregnancy planning (hemodynamic changes and antithrombotic strategy may need adjustment)
- New medications (some interact with anticoagulants or increase bleeding risk)
When to seek urgent or emergency care
Seek urgent evaluation for symptoms that could reflect an acute coronary event or dangerous clotting:
- Chest pressure or pain that is new, severe, persistent, or occurs at rest
- Sudden shortness of breath, fainting, or near-fainting
- Rapid or irregular heartbeat with dizziness or chest discomfort
- New weakness, confusion, or signs of stroke (sudden facial droop, speech difficulty)
- Any symptom pattern that feels like a heart attack, even if it is “not classic”
Seek urgent evaluation for bleeding if you are on blood thinners:
- black/tarry stools, vomiting blood, coughing blood,
- severe headache after a fall or head impact,
- uncontrolled bleeding from any site.
A steady long-term outlook
Many people with giant coronary aneurysms live for years with careful monitoring and well-chosen therapy. The most effective strategy is active partnership: understand your risk markers (size, thrombus, stenosis, symptoms), follow the monitoring plan, and treat warning symptoms as time-sensitive—not something to “wait out.”
References
- Giant coronary artery aneurysms: a case series and management recommendations – PMC 2025 (Review/Case Series)
- Pathophysiology, Diagnosis, and Management of Coronary Artery Aneurysms: A Review – PMC 2025 (Review)
- Update on Diagnosis and Management of Kawasaki Disease: A Scientific Statement From the American Heart Association – PubMed 2024 (Guideline/Scientific Statement)
- Diagnosis of coronary artery abnormalities in Kawasaki disease: recent guidelines and z score systems – PMC 2021 (Guideline Summary/Review)
- Management and Outcomes of Coronary Artery Aneurysms: A Patient-Level Systematic Review – PubMed 2025 (Systematic Review)
Disclaimer
This article is for educational purposes only and does not provide medical advice, diagnosis, or treatment. A giant coronary artery aneurysm can increase the risk of blood clots, heart attack, and other serious complications, and care often requires individualized decisions about imaging, blood thinners, and sometimes procedures or surgery. If you have new or worsening chest pain, shortness of breath, fainting, stroke-like symptoms, or signs of severe bleeding—especially if you take antiplatelet or anticoagulant medicines—seek emergency care immediately. Always follow guidance from your cardiology team, who can tailor decisions to your anatomy, symptoms, and overall health.
If you found this article helpful, please share it on Facebook, X (formerly Twitter), or any platform you prefer, and follow us on social media. Your support through sharing helps our team continue producing reliable, high-quality health content.