Glycogen storage cardiomyopathy is a group of inherited conditions where extra glycogen (the body’s stored form of sugar) builds up inside heart muscle cells. Over time, that buildup can make the heart wall thicken, stiffen, or weaken. The result is a cardiomyopathy—heart muscle disease that can affect pumping, rhythm, or both.
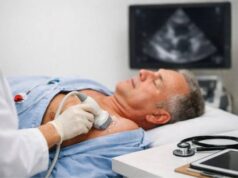
People often search for answers after an “unexpected” finding: a thickened heart on ultrasound, an abnormal ECG, or symptoms like shortness of breath, chest tightness, fainting, or racing heartbeats. These disorders matter because they can look like more common heart diseases, yet the best care may be very different and may include disease-specific therapies, family testing, and earlier rhythm monitoring. With a clear diagnosis and the right plan, many patients can reduce complications and protect heart function for years.
Table of Contents
- What it is and why glycogen builds up
- What causes it and who is at risk?
- Symptoms, red flags, and complications
- How it’s diagnosed and what tests show
- Treatments that protect the heart
- Daily management and when to seek urgent care
What it is and why glycogen builds up
“Glycogen storage cardiomyopathy” is not one single diagnosis. It’s an umbrella term for several genetic disorders in which the heart stores too much glycogen or handles glycogen in an abnormal way. Glycogen is normally a helpful fuel reserve. Heart cells keep small amounts on hand for quick energy needs. In these disorders, a missing enzyme or faulty transport step causes glycogen to accumulate inside the cell, where it begins to interfere with normal structure and function.
Over time, the heart can change in one or more of these ways:
- Thickened heart muscle (hypertrophy): the walls look enlarged, often like hypertrophic cardiomyopathy.
- Stiffness: the heart fills poorly, raising pressures and causing shortness of breath.
- Weakness (reduced pumping): the heart can eventually enlarge and pump less effectively.
- Electrical system disruption: abnormal glycogen storage can affect conduction tissue, increasing the risk of arrhythmias and heart block.
Common conditions that fall under this label
Clinicians often think about glycogen storage cardiomyopathy when they suspect a “phenocopy”—a condition that imitates a common cardiomyopathy but has a different cause. Examples include:
- Pompe disease: a lysosomal storage disorder that can cause heart thickening (especially in infants) and muscle weakness.
- Danon disease: often presents with severe cardiomyopathy and rhythm problems, sometimes with skeletal muscle and learning or vision differences.
- PRKAG2 syndrome: a glycogen-related heart condition that commonly causes thickening plus conduction disease and pre-excitation patterns on ECG.
- Some glycogen storage diseases with muscle/liver involvement (such as GSD III): can include cardiac thickening and heart failure risk in a subset of patients.
Why this diagnosis changes the conversation
In routine hypertrophic cardiomyopathy, the main focus may be symptom control and sudden death risk assessment. In glycogen storage cardiomyopathy, those still matter—but there is often more: earlier genetic confirmation, screening of relatives, attention to skeletal muscle or metabolic issues, and in some cases disease-specific therapy (such as enzyme replacement therapy for Pompe disease). The earlier the condition is recognized, the more options you typically have to prevent avoidable decline.
What causes it and who is at risk?
Glycogen storage cardiomyopathy is caused by inherited gene changes that disrupt how heart cells process glycogen. The specific gene determines the pattern of disease, age of onset, and which other organs may be involved. Some conditions primarily affect the heart’s electrical system and thickness. Others affect both heart and skeletal muscle, and some can involve liver or nervous system features.
Inheritance patterns you may hear about
Understanding inheritance helps with family planning and deciding who else in the family should be screened.
- Autosomal dominant: One changed gene copy can cause disease. PRKAG2 syndrome often follows this pattern, so multiple generations may be affected.
- Autosomal recessive: Two changed copies (one from each parent) are needed. Many classic glycogen storage diseases follow this pattern; parents may be healthy carriers.
- X-linked: The changed gene is on the X chromosome. Danon disease is commonly described this way; males often develop symptoms earlier and more severely, while females can still be significantly affected.
Who is at higher risk of having a glycogen storage cause
You cannot develop these conditions from diet, exercise, or stress alone. Risk comes from genetics and family history. Clinicians become more suspicious when they see any of the following:
- Cardiomyopathy at a young age, especially in childhood, teens, or early adulthood.
- A “hypertrophic cardiomyopathy” diagnosis plus unusual ECG features, such as pre-excitation or early conduction disease.
- A family history of pacemakers, sudden cardiac death, or unexplained heart failure at younger ages.
- Cardiac findings plus muscle symptoms, such as exercise intolerance, weakness, frequent cramps, or elevated muscle enzymes.
- Cardiac findings plus systemic clues, such as learning difficulties, liver enlargement, high creatine kinase, or a history of metabolic crises.
- Consanguinity (parents related by blood), which increases the chance of recessive conditions in a family.
Why “risk factors” matter even after diagnosis
Once someone is diagnosed, risk becomes less about “who gets it” and more about “who gets complications.” Factors that can increase complication risk include:
- Prior fainting episodes, especially during exertion.
- Documented arrhythmias (atrial fibrillation, ventricular tachycardia, rapid accessory pathway conduction).
- Progressive thickening or declining heart function on imaging.
- Delays in diagnosis, which can mean less time to benefit from targeted treatments and monitoring.
A useful mindset is this: genetics may set the stage, but early recognition and consistent follow-up strongly influence outcomes.
Symptoms, red flags, and complications
Symptoms vary widely because glycogen storage cardiomyopathy is not one disease. Some people feel well and are diagnosed after a routine ECG or sports screening. Others first present with heart failure symptoms, dangerous arrhythmias, or severe disease in infancy. Many patients fall somewhere in between, noticing gradually worsening stamina or episodes that are easy to dismiss until they recur.
Common symptoms
Symptoms often reflect either reduced heart performance or rhythm instability:
- Shortness of breath with exertion or when lying flat
- Reduced exercise capacity and easy fatigue
- Chest pressure or discomfort, sometimes during exertion
- Palpitations (skipped beats, racing, fluttering)
- Lightheadedness or fainting
- Swelling in legs or abdomen in more advanced heart failure
- Poor feeding, sweating with feeds, or failure to thrive in infants with severe forms
Clues that suggest a glycogen storage cause
Doctors often look for features that are less typical of standard hypertrophic cardiomyopathy:
- Pre-excitation on ECG (a shortcut pathway that can trigger fast rhythms)
- Early conduction disease (unusually slow heart rates, heart block, need for pacemaker at young age)
- Rapid progression of thickening or symptoms
- Multisystem features, such as muscle weakness, high creatine kinase, liver enzyme abnormalities, or developmental/learning differences
- Family patterns that do not match typical sarcomeric cardiomyopathy
Complications to understand and plan for
The main complications tend to cluster into rhythm problems and heart failure.
- Arrhythmias
- Atrial fibrillation can worsen symptoms and increase stroke risk.
- Ventricular arrhythmias can cause fainting or sudden cardiac death.
- Accessory pathway–related tachycardias can be fast and destabilizing, particularly in PRKAG2-related disease.
- Conduction failure
- Damage to the heart’s electrical wiring can lead to bradycardia or heart block, sometimes requiring a pacemaker.
- Heart failure
- Some patients develop a stiff heart with high filling pressures; others progress to reduced pumping and dilation.
- Advanced heart failure may lead to transplant evaluation in selected cases.
When symptoms should be treated as urgent
Seek immediate medical attention for:
- Fainting during exercise or with palpitations
- New chest pain with shortness of breath, sweating, or nausea
- Rapid, sustained racing heartbeat that does not settle within minutes
- Sudden shortness of breath at rest, pink frothy sputum, or severe swelling
- Neurologic symptoms (weakness, trouble speaking) that could suggest stroke
Knowing the “red flags” is not about living in fear. It is about acting quickly when timing matters most.
How it’s diagnosed and what tests show
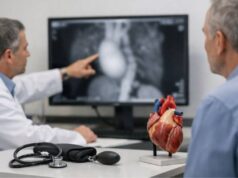
Diagnosis usually starts with a familiar pathway—an ECG or echocardiogram suggests cardiomyopathy—then becomes more targeted when the pattern looks atypical or the patient’s age and history raise suspicion. Because these conditions can mimic more common cardiomyopathies, a careful workup helps avoid missed treatment opportunities and improves family screening accuracy.
Step 1: History that guides testing
Clinicians typically ask about:
- Age at symptom onset and speed of progression
- Fainting, palpitations, exercise-related symptoms, or seizures
- Family history of cardiomyopathy, sudden death, pacemakers, or transplant
- Muscle symptoms (weakness, cramps, exercise intolerance)
- Early childhood clues (feeding issues, delayed motor milestones)
- Medication history and any prior “unexplained” hospitalizations
Step 2: Core cardiac tests
Most patients will have:
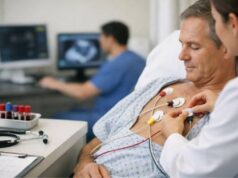
- ECG: may show thickening patterns, conduction delays, or pre-excitation.
- Echocardiogram: assesses wall thickness, pumping function, valve behavior, and outflow obstruction.
- Holter or patch monitor (24 hours to 2 weeks): looks for silent arrhythmias.
- Cardiac MRI: can clarify anatomy and detect tissue changes (such as fibrosis) that influence risk planning.
These tests help answer a practical question: is the main issue thickness, stiffness, rhythm, or declining pump function—or a combination?
Step 3: Labs and metabolic clues
Blood tests do not “diagnose” glycogen storage cardiomyopathy by themselves, but they can provide powerful clues:
- Creatine kinase (CK): may be elevated when skeletal muscle is involved.
- Liver enzymes and fasting labs: can suggest broader metabolic involvement in some glycogen storage diseases.
- Biomarkers related to heart strain may help track severity over time.
In infants or young children with suspected Pompe disease, newborn screening results or enzyme activity testing may be part of the evaluation in some regions.
Step 4: Genetic testing as a decision point
A cardiomyopathy gene panel or targeted testing often becomes central. A confirmed genetic diagnosis can:
- Clarify the exact condition (for example, Pompe vs PRKAG2 vs Danon)
- Prompt screening of relatives who may be at risk but symptom-free
- Guide rhythm monitoring strategy and procedure decisions
- Open access to disease-specific therapies or clinical trials when appropriate
When biopsy is considered
Heart biopsy is not routine, but it may be used when noninvasive tests are inconclusive or when tissue confirmation could change treatment. Biopsy can show storage material patterns and help distinguish among metabolic, inflammatory, and infiltrative causes.
A clear diagnosis is not just a label. It’s the map that helps clinicians choose the right monitoring intensity, the right therapy, and the right family plan.
Treatments that protect the heart
Treatment depends on the specific genetic disorder and the patient’s current heart status. Most care plans combine (1) disease-specific therapy when available, (2) standard cardiology treatments tailored to the condition’s rhythm and pumping risks, and (3) proactive planning for procedures and life stages such as pregnancy, athletics, or advanced heart failure.
Disease-specific therapies
Some glycogen storage cardiomyopathies have targeted treatments that address the underlying metabolic problem.
- Pompe disease: Enzyme replacement therapy (ERT) is a cornerstone of care. It is typically given by IV infusion on a scheduled basis and is managed by a multidisciplinary team. ERT may stabilize or improve certain outcomes, but response can vary by age of onset, disease stage, and other factors. Newer ERT options and supportive agents have expanded choices in some settings.
- Other glycogen-related cardiomyopathies: For conditions like Danon disease, disease-modifying therapies are an active area of research. Even when a definitive “metabolic fix” is not yet standard, early recognition still improves outcomes through rhythm protection and timely advanced heart failure planning.
Heart failure treatment
When symptoms or imaging suggest heart failure, clinicians may use standard medications, chosen carefully based on blood pressure, rhythm status, and whether outflow obstruction is present. Treatment may include:
- Medications to reduce congestion (diuretics)
- Medications that support remodeling and reduce hospitalizations in appropriate patients
- Salt and fluid guidance tailored to symptoms and lab results
- Cardiac rehabilitation or supervised exercise planning when safe
In advanced cases, teams may discuss mechanical support or heart transplantation. Transplant is not right for everyone, but it can be lifesaving when heart failure progresses despite maximal therapy.
Arrhythmia and conduction management
Rhythm planning is often as important as heart failure planning in glycogen storage cardiomyopathy.
- Monitoring: repeat Holter/patched monitoring may be scheduled even when symptoms are mild, because dangerous rhythms can be silent.
- Ablation: in patients with accessory pathways or recurrent tachycardias, catheter ablation may be considered.
- Pacemaker: may be needed for significant bradycardia or heart block.
- ICD (defibrillator): may be recommended for patients with higher-risk features (such as prior sustained ventricular arrhythmias or certain imaging/risk profiles).
What to expect after treatment starts
A realistic expectation is “stepwise improvement.” Symptoms may improve before imaging changes do. Rhythm protection reduces catastrophic risk but does not eliminate the need for follow-up. Many patients benefit from a written plan that spells out: medications, monitoring schedule, exercise limits, and what to do if symptoms suddenly change.
Daily management and when to seek urgent care
Daily management is about protecting heart function while maintaining a full life. The best plans are practical: they identify what to monitor, what to avoid, how to exercise safely, and when to call for help. Because glycogen storage cardiomyopathy can change over time, consistency matters more than perfection.
Follow-up habits that make a real difference
Many patients do best with structured follow-up that includes:
- Regular cardiology visits with symptom review and medication adjustments
- Scheduled rhythm monitoring (Holter/patch) based on diagnosis and risk profile
- Periodic echocardiograms to track thickness, stiffness, and pumping function
- Cardiac MRI when indicated to refine risk assessment or clarify changes
- Coordination with genetics and metabolic specialists when the condition affects other organs
Keep a simple symptom log that tracks: palpitations, fainting/near-fainting, exercise tolerance, swelling, sleep position (how many pillows), and new chest discomfort. Patterns often appear before crises do.
Exercise, sports, and daily activity
Activity recommendations should be individualized, but these principles are common:
- Favor moderate, steady activity over sudden bursts or all-out sprinting unless your clinician explicitly clears it.
- Avoid dehydration and overheating, which can trigger symptoms and worsen rhythm stability.
- If you have a history of fainting, significant arrhythmias, or severe thickening, your team may advise limits on competitive sports.
- Ask for a clear plan for school, work, travel, and altitude if you notice symptoms in those settings.
Medication and lifestyle cautions
Because rhythm and conduction problems are common, do not start new supplements, stimulants, or “performance” products without asking your clinician. Some can worsen palpitations or interact with heart medications. If you have heart failure, follow individualized guidance on salt and fluid—blanket rules can backfire.
Family screening and planning ahead
Because these are genetic conditions, family care is part of personal care:
- Encourage first-degree relatives to discuss screening and/or genetic testing when a pathogenic variant is identified.
- Consider genetic counseling for family planning decisions.
- Keep a concise medical summary available for emergencies and for any new clinician.
When to seek urgent care
Go to urgent or emergency care for:
- Fainting, especially during activity or with palpitations
- New or worsening shortness of breath at rest
- Chest pain that is new, severe, or accompanied by sweating or nausea
- Sustained rapid heart rate, severe dizziness, or confusion
- Signs of stroke (face droop, arm weakness, speech trouble)
Timely care is a form of prevention. In glycogen storage cardiomyopathy, acting early can prevent a manageable change from becoming a dangerous event.
References
- Cardiovascular involvement in glycogen storage diseases – PubMed 2025 (Review)
- International Consensus on Differential Diagnosis and Management of Patients With Danon Disease: JACC State-of-the-Art Review – PubMed 2023 (Review/Consensus)
- PRKAG2 Syndrome: Clinical Features, Imaging Findings and Cardiac Events – PMC 2025 (Clinical Study/Review)
- Enzyme replacement therapies in adults with Pompe disease: from trials to real-world data – PMC 2025 (Review)
Disclaimer
This article is for educational purposes only and does not provide medical advice, diagnosis, or treatment. Glycogen storage cardiomyopathy includes rare genetic disorders that can affect heart rhythm and heart function, sometimes with rapid changes in risk around arrhythmias or heart failure. If you have symptoms such as fainting, chest pain, sudden shortness of breath, or sustained palpitations, seek urgent medical care. For individualized guidance—especially about exercise, pregnancy, procedures, and family screening—consult a qualified clinician, ideally a cardiologist with experience in inherited and metabolic cardiomyopathies.
If you found this article useful, please share it on Facebook, X (formerly Twitter), or any platform you prefer, and follow us on social media. Your support through sharing helps our team continue producing trustworthy, high-quality health content.