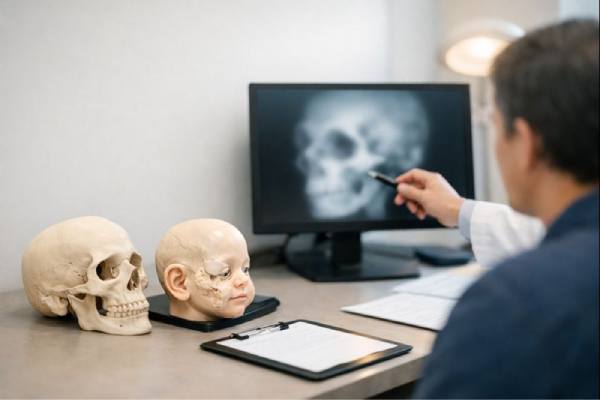
Goldenhar syndrome is a rare condition present at birth (congenital—“from birth”) that affects how parts of the face and nearby structures form early in pregnancy. Many families first notice one-sided facial difference, an underdeveloped ear, or small skin tags near the ear. Others learn about it after an eye finding, such as a small growth on the surface of the eye, or after a spine X-ray shows unusual vertebrae.
Because the condition can involve the ears, eyes, jaw, spine, and sometimes the heart or kidneys, it is best understood as a spectrum—meaning features and severity vary widely from one person to another. The most helpful care is usually not a single procedure, but a staged plan built by a coordinated team. With early screening, targeted treatments, and strong school and family supports, many children and adults do very well.
Table of Contents
- What it is and how it affects the body
- What causes Goldenhar syndrome?
- Symptoms and complications to watch for
- How it’s diagnosed and what to screen
- Treatment options and what to expect
- Long-term management and when to seek care
What it is and how it affects the body
Goldenhar syndrome is commonly used to describe a set of findings within the oculo-auriculo-vertebral spectrum (often shortened to OAVS). In plain terms, it involves differences in the development of structures that form the face and neck early in pregnancy—especially the jaw, ears, and soft tissues—often along with eye and spine differences. Many clinicians also discuss it alongside craniofacial microsomia, a broader term that focuses on underdevelopment (hypoplasia) of one side of the face. These labels overlap because the condition is not a single “one look” diagnosis; it is a range of patterns.
What parts of the body can be involved
The most typical features involve the head and neck:
- Face and jaw: one-sided facial asymmetry, a smaller lower jaw (mandible), or differences in cheek soft tissue.
- Ears: small outer ear (microtia), a narrowed or absent ear canal, preauricular tags, or middle-ear differences that affect hearing.
- Eyes: epibulbar dermoid (a benign growth on the eye surface), eyelid differences, or vision issues from astigmatism or irritation.
- Mouth and teeth: cleft lip/palate in some cases, misaligned bite, missing teeth, or delayed eruption.
Other systems may also be affected, which is why early screening is so important:
- Spine and ribs: fused or segmented vertebrae, scoliosis, or rib differences.
- Breathing and airway: smaller jaw and facial structure differences can increase risk of snoring, obstructive sleep apnea, or feeding-related airway problems in infancy.
- Heart and kidneys: some children have congenital heart defects or kidney/urinary tract differences, sometimes without obvious symptoms at first.
- Nervous system and development: many children have typical intelligence, but some may have speech/language delay, learning differences, or motor delays—often influenced by hearing, vision, sleep quality, and time spent in medical care.
Why “spectrum” matters for families
A spectrum diagnosis can feel vague, but it is clinically useful: it reminds everyone to look beyond the face alone. Two children can share the same label and still need very different care plans—one may need hearing support and orthodontics, while another needs airway monitoring, spine follow-up, and multiple staged surgeries. The best early goal is not to predict every future procedure, but to build a roadmap: what to screen now, what to watch over time, and which specialists should be involved at each stage.
What causes Goldenhar syndrome?
In most families, Goldenhar syndrome happens sporadically, meaning it appears in a child with no prior family history. Researchers view it as a complex developmental condition with more than one possible pathway. Rather than a single cause, the current understanding points to a mix of genetic susceptibility and early pregnancy factors that can disrupt how facial and neck structures form.
Early development: what goes off track
During the first weeks of pregnancy, the tissues that later become parts of the jaw, ears, and face must grow, move, and connect in a tightly timed sequence. If those steps are interrupted, one side may develop differently than the other. Two broad biological ideas are often discussed:
- Changes in cell migration and growth: especially in neural crest–derived tissues that help form craniofacial bones and connective tissue.
- Vascular disruption: reduced or altered blood flow to a developing region may limit growth in a localized way, which could help explain why many cases are one-sided.
These are frameworks, not “proof” for any one child—but they guide screening and research.
Genetic factors
A small percentage of cases run in families, which supports a genetic contribution in at least some patients. Genetics can involve:
- Single-gene changes that affect early developmental pathways.
- Copy number variants (small deletions or duplications of DNA) that alter gene dosage.
- Incomplete penetrance and variable expression, meaning a parent might carry a change with mild or subtle features, while a child is more affected.
Because the genetic picture is diverse, genetic testing may or may not identify a clear cause. Even when it does not, the result can still be useful by ruling out other syndromes that have different health risks.
Maternal and pregnancy-associated risk factors
Certain exposures and pregnancy conditions have been reported more often in affected pregnancies, though they do not “explain” most cases on their own. Reported associations include:
- Maternal diabetes (especially if glucose control is poor early in pregnancy)
- Multiple pregnancy (twins or higher-order multiples)
- Assisted reproductive technologies in some reports (association does not mean causation)
- Smoking and vasoactive drug exposure in some studies
- Certain medications with known fetal risk (classic historical examples include thalidomide)
It is important to interpret these carefully: many parents with these factors have unaffected children, and many affected children have none of these exposures. For families, the most practical takeaway is not blame, but planning—especially around future pregnancies, where preconception diabetes control and medication review can reduce broad congenital risk.
Recurrence risk for future children
For most sporadic cases, the chance of recurrence is low, but not zero. If genetic testing finds a specific inherited change, recurrence risk can be higher and depends on inheritance pattern. A genetic counselor can help translate testing results into clear, family-specific numbers and discuss options such as targeted testing for relatives.
Symptoms and complications to watch for
Goldenhar syndrome can be obvious at birth or subtle enough that it is recognized later, especially if ear differences are mild and facial asymmetry becomes more noticeable with growth. Symptoms also change with age: infancy often focuses on feeding, breathing, and hearing; school years bring speech and learning needs; adolescence and adulthood may involve orthodontics, jaw alignment, hearing technology upgrades, and psychosocial support.
Common physical features
Many children have a combination of:
- Facial asymmetry: often one cheek and jaw are smaller, with the chin pointing slightly toward the smaller side.
- Ear differences: microtia, preauricular tags, ear canal narrowing, or recurrent ear infections.
- Hearing loss: commonly conductive hearing loss from outer or middle ear differences; some have mixed or sensorineural components.
- Eye findings: epibulbar dermoid or lipodermoid, eyelid coloboma, chronic irritation, or astigmatism that can reduce vision if untreated.
- Mouth and dental issues: cleft palate in some, misaligned bite, crowding, missing teeth, or differences in tooth size.
- Spine differences: fused vertebrae, hemivertebrae, scoliosis, or neck mobility differences.
Functional symptoms families often notice
These “day-to-day” issues often drive care decisions more than appearance alone:
- Feeding difficulty in infancy: slow feeding, choking, poor weight gain, or reflux.
- Noisy breathing or snoring: possible obstructive sleep apnea, especially with small jaw.
- Speech delay or unclear speech: often influenced by hearing loss, palate function, and dental alignment.
- Frequent ear infections or fluid: can worsen hearing and speech development.
- Neck or back pain later on: sometimes related to spinal curvature or vertebral differences.
Complications to monitor proactively
Most complications are preventable or manageable when detected early:
- Vision loss risk in early childhood: untreated astigmatism or eye surface problems can lead to amblyopia (“lazy eye”). Early eye exams matter.
- Language and learning gaps: even mild hearing loss can affect classroom learning. Early hearing support can prevent avoidable delays.
- Sleep-related problems: untreated sleep apnea can worsen attention, mood, growth, and school performance.
- Spinal progression: scoliosis can progress with growth spurts; regular monitoring helps time therapy or surgery appropriately.
- Hidden organ differences: congenital heart or kidney issues may be silent early, which is why screening is recommended even in children who “seem fine.”
When symptoms should be treated as urgent
Seek urgent evaluation if a child has:
- Persistent breathing difficulty, blue color around lips, or repeated choking episodes
- Signs of severe sleep apnea (pauses in breathing, gasping, daytime sleepiness, behavioral changes)
- Sudden hearing change, severe ear pain with fever, or drainage in a child with ear canal anomalies
- Eye redness with pain, light sensitivity, or sudden vision changes
- Weakness, severe headache, or new neurologic symptoms
A useful framing is this: Goldenhar syndrome is rarely a constant emergency, but it does require systematic follow-up so that small problems do not become big ones.
How it’s diagnosed and what to screen
Diagnosis is primarily clinical—based on physical findings and pattern recognition—supported by targeted imaging and screening tests. Because the condition overlaps with other craniofacial syndromes, the evaluation aims to (1) confirm the pattern, (2) map which body systems are involved, and (3) set a monitoring plan that matches the child’s needs.
Clinical evaluation: the cornerstone
A clinician experienced in craniofacial conditions typically assesses:
- Facial symmetry, jaw size, bite relationship, and soft-tissue volume
- Ear shape, ear canal status, and signs of middle-ear disease
- Eye surface and eyelid structure
- Mouth and palate structure
- Spine alignment and neck movement
- Facial nerve function (smile symmetry, eyelid closure)
Many teams document findings using structured systems (for example, OMENS and related classification methods). The point is not to “score” a child, but to communicate clearly across specialists and track changes over time.
Recommended screening tests (often early in life)
Because involvement can extend beyond the face, most craniofacial teams recommend a baseline screening set, tailored to severity:
- Hearing evaluation: newborn screening is not enough for many children with ear canal differences. A full audiology assessment and repeat testing as the child grows are important.
- Eye exam: early ophthalmology evaluation to detect dermoids, astigmatism, and amblyopia risk.
- Spine imaging: X-ray or other imaging when clinically indicated to identify vertebral differences and guide scoliosis monitoring.
- Heart evaluation: many clinicians recommend echocardiography at least once, especially in infants and young children, to detect congenital heart defects.
- Kidney/urinary tract screening: renal ultrasound is commonly used because kidney differences can be silent early.
- Sleep evaluation: if there is snoring, labored breathing, poor growth, or daytime behavior changes, a sleep study may be recommended.
Genetic testing: when it helps
Genetic testing can be useful when:
- Features are more widespread or atypical
- There is developmental delay, major organ involvement, or multiple affected relatives
- A family wants clearer recurrence counseling for future pregnancies
Testing may include chromosomal microarray and/or gene panels. Even if no single cause is found, genetic evaluation often helps rule out other syndromes with different medical risks.
Prenatal detection
Some cases are suspected on prenatal ultrasound—such as facial asymmetry, ear anomalies, clefting, or vertebral differences—but many are not identified until after birth. If prenatal suspicion exists, fetal echocardiography and targeted anatomy review can help plan delivery and newborn care.
A well-done diagnostic process answers the questions families actually have: “What else should we check?” “What should we watch for next year?” and “Who should be on the care team?”
Treatment options and what to expect
Treatment is individualized and usually staged over years. The most effective approach comes from a coordinated multidisciplinary team—often including craniofacial surgery, ENT/audiology, ophthalmology, orthodontics, speech-language therapy, genetics, and psychology—so that interventions happen in the safest order and at developmentally appropriate times.
Early priorities: safety, function, development
In infancy and early childhood, the focus is often on function rather than appearance:
- Airway and feeding support
- Positioning strategies, feeding therapy, reflux management, and in some cases airway evaluation by ENT.
- If sleep apnea is suspected, evaluation and treatment can improve growth and daytime functioning.
- Hearing support
- Early amplification (such as bone-conduction hearing devices when the ear canal is narrow/absent) can protect speech and learning.
- Management of middle-ear fluid and infections may include tubes when anatomy allows.
- Eye protection and vision development
- Dermoids may require monitoring or removal based on size, irritation, and vision impact.
- Early correction of astigmatism and amblyopia prevention strategies (glasses, patching when needed) can preserve vision.
Reconstructive and orthodontic care: staged and timed
As children grow, teams often coordinate skeletal and soft-tissue work with dental development:
- Cleft palate or lip repair when present, timed to support feeding and speech milestones.
- Orthodontics to guide dental alignment and jaw growth; some children benefit from early expanders or braces in stages.
- Jaw procedures (in selected patients)
- Mandibular distraction or other jaw surgeries may be considered for significant asymmetry, airway issues, or bite problems.
- Timing depends on severity, airway status, and growth patterns; “earlier is better” is not always true.
- Ear reconstruction
- Options may include rib cartilage reconstruction, synthetic frameworks, or prosthetics, depending on anatomy and family preference.
- Canal reconstruction (atresiaplasty) is not appropriate for everyone and is usually considered only after detailed imaging and hearing planning.
- Soft-tissue balancing
- Fat grafting or other soft-tissue procedures may help symmetry, often after skeletal relationships are clearer.
Spine and other organ treatments
- Scoliosis management may include observation, bracing, or surgery depending on curve size and progression.
- Cardiac or renal anomalies are managed with standard specialty care; many are treatable, especially when detected early.
What families can expect emotionally and practically
Treatment can feel like a marathon. Many families benefit from:
- A written long-term plan with “next 6 months” and “next 2 years” goals
- Clear communication about which procedures are elective versus function-critical
- Support for school accommodations (hearing, speech, fatigue after surgeries)
- Mental health support when social stress, teasing, or medical fatigue builds up
A strong team helps families avoid two common extremes: rushing into unnecessary procedures, or delaying critical supports (like hearing and vision care) that directly affect development.
Long-term management and when to seek care
Long-term management is about protecting health, supporting development, and helping the child (and later the adult) feel confident and capable in daily life. Because needs change with age, many families do best with a “living plan” that is reviewed annually and adjusted during growth spurts, school transitions, and planned procedures.
Ongoing follow-up that prevents avoidable problems
Many craniofacial programs recommend structured follow-up in these areas:
- Hearing: repeat audiology on a schedule; check device fit and school listening support (classroom microphones when appropriate).
- Vision: periodic ophthalmology visits in childhood to ensure stable vision and detect irritation or amblyopia risk early.
- Sleep and breathing: reassess snoring, restless sleep, daytime attention, and growth; repeat sleep studies if symptoms recur.
- Dental and jaw growth: orthodontic monitoring often continues for years; jaw alignment can change during adolescence.
- Spine: periodic checks during growth spurts; earlier review if posture changes or pain appears.
- Speech and learning: speech therapy, language support, and school accommodations should match the child’s current needs, not last year’s plan.
A practical home tool is a one-page “medical summary” listing diagnoses, key surgeries, current devices, allergies, and main specialists. It saves time in emergencies and new-care settings.
Prevention and daily-life strategies
Some helpful habits are simple but powerful:
- Protect hearing by treating ear infections promptly and ensuring devices are used consistently.
- Prioritize sleep routines; untreated sleep problems can affect behavior and learning as much as hearing loss can.
- Build strong dental hygiene early, especially if teeth are crowded or enamel is weaker.
- Encourage age-appropriate self-advocacy: children can learn to explain their hearing device or medical differences in a calm, confident way.
- Watch for social stress. Peer relationships often become harder in late elementary and middle school; proactive support can prevent isolation.
Adolescence and adulthood: shifting goals
As patients mature, goals often shift toward:
- Final orthodontic alignment and bite stability
- Decisions about elective symmetry procedures
- Long-term hearing technology choices
- Career planning and transition to adult specialty care
- Family planning conversations, including genetic counseling when appropriate
When to seek urgent medical care
Get urgent evaluation for:
- Breathing trouble, repeated choking, or signs of severe sleep apnea
- Eye pain, new light sensitivity, or sudden vision change
- Sudden or worsening hearing changes, severe infection, or high fever with ear pain
- New neurologic symptoms (weakness, severe headache, seizure)
- Rapidly worsening spinal pain or visible curve change, especially during growth spurts
Most people with Goldenhar syndrome can build a healthy, full life. The key is not constant intervention, but consistent monitoring and timely support—especially for hearing, vision, sleep, and learning.
References
- Oculo-auriculo-vertebral spectrum: new genes and literature review on a complex disease – PubMed 2022 (Review)
- European Guideline Craniofacial Microsomia – PubMed 2020 (Guideline)
- European Guideline on Craniofacial Microsomia: A Version for Patients and Families – PubMed 2022 (Guideline Summary/Review)
- Evaluation of Research Diagnostic Criteria in Craniofacial Microsomia – PubMed 2023 (Multicenter Study)
- Oculo Auriculo Vertebral Spectrum – StatPearls – NCBI Bookshelf 2023 (Clinical Review)
Disclaimer
This article is for educational purposes only and does not provide medical advice, diagnosis, or treatment. Goldenhar syndrome (oculo-auriculo-vertebral spectrum) can involve the ears, eyes, jaw, spine, and sometimes internal organs, so evaluation and care should be individualized by qualified clinicians—often through a craniofacial team. If you or your child has breathing difficulty, severe snoring with pauses in breathing, sudden vision changes, significant infection symptoms, or fainting or neurologic symptoms, seek urgent medical care. For personalized guidance on screening, surgery timing, hearing/vision support, and genetic counseling, consult your healthcare team.
If you found this article helpful, please share it on Facebook, X (formerly Twitter), or any platform you prefer, and follow us on social media. Your support through sharing helps our team continue producing high-quality health content.