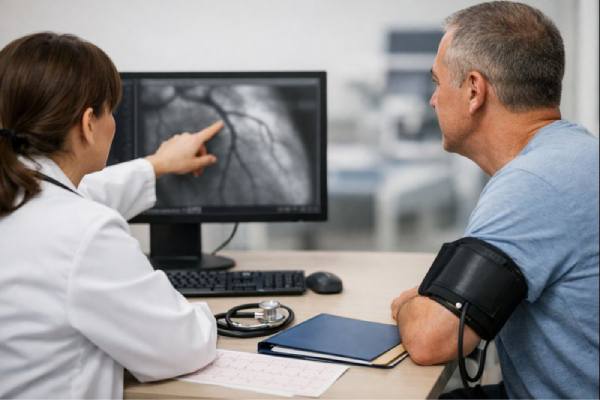
Graft vasculopathy is a long-term problem that can develop after an organ transplant, when the blood vessels of the graft slowly become narrower and stiffer. “Vasculopathy” means blood vessel disease. Over time, these vessel changes can reduce blood flow and gradually damage the transplanted organ—even when you feel well and routine labs look “almost normal.”
This condition matters because it is often quiet at first, but it can become one of the main reasons a transplanted organ loses function years later. The pattern also differs from typical artery disease: instead of one short blockage, graft vasculopathy often affects long segments of vessels and smaller branches. That is why regular follow-up, planned screening, and strong control of risk factors are central to long-term graft care.
Table of Contents
- What graft vasculopathy is and how it harms organs
- What causes graft vasculopathy?
- Who is at higher risk?
- Symptoms and complications by organ
- How graft vasculopathy is diagnosed
- Treatment options and what to expect
- Long-term management, prevention, and when to seek care
What graft vasculopathy is and how it harms organs
Graft vasculopathy is a form of chronic blood vessel injury that develops in transplanted organs. It is often described as a “chronic rejection–related” vessel disease, but it is best understood as the final common pathway of several stresses that repeatedly irritate the vessel lining over time.
What happens inside the vessels
The inner lining of blood vessels (the endothelium) helps keep blood flowing smoothly and signals the vessel to relax or tighten. In graft vasculopathy, this lining is repeatedly injured by immune activity and inflammation. The vessel wall responds by thickening and scarring. Two features are especially important:
- Diffuse narrowing: instead of one short blockage, narrowing may extend along long segments and into smaller branches.
- Small-vessel involvement: tiny vessels that cannot be stented or bypassed may also be affected, limiting blood flow in a more “global” way.
This is why a graft can have significant flow limitation even when a single scan does not show a dramatic focal blockage.
How it differs from ordinary atherosclerosis
Traditional atherosclerosis often builds cholesterol plaques over decades and may cause a “culprit” lesion. Graft vasculopathy can include atherosclerosis-like changes, but it also involves smooth, concentric wall thickening and immune-driven remodeling. Many patients have both processes at once: transplant-related vessel thickening plus classic risk-factor–driven plaque.
Why it can be silent for a long time
Symptoms depend on the organ. Heart transplant recipients, for example, may not develop typical chest pain because the transplanted heart’s nerve supply can be altered. Kidney transplant recipients may notice only a slow drift in kidney function. In other words, the organ can be under-perfused without obvious “alarm” symptoms—one reason transplant programs emphasize planned surveillance rather than waiting for warning signs.
Why early detection matters
Graft vasculopathy is often progressive, but its speed varies widely. When clinicians detect early changes, they can intensify prevention (lipids, blood pressure, glucose, infection prevention) and consider immunosuppression adjustments when appropriate. The goal is usually not a dramatic reversal, but a slower slope—preserving graft function for years longer.
What causes graft vasculopathy?
Graft vasculopathy rarely comes from a single cause. Most cases reflect a blend of immune-driven injury and non-immune stresses that keep the vessel lining inflamed. A useful way to think about it is: the vessels are reacting to repeated “hits.” The more hits, the higher the chance the vessels remodel in a harmful direction.
Immune-related causes
These are the drivers most specific to transplantation:
- Ongoing alloimmune response: the immune system recognizes donor tissue as “not self.” Even when immunosuppressive drugs prevent overt rejection, low-grade immune activity can persist.
- Acute rejection episodes: a history of cellular rejection or antibody-mediated rejection can leave lasting vessel injury.
- Donor-specific antibodies (DSA): antibodies that target donor tissue can attack the vessel lining and microcirculation, promoting chronic inflammation and scarring.
- Mismatch and sensitization: higher immunologic mismatch or a strongly sensitized recipient can increase long-term immune pressure on the graft.
- Ischemia-reperfusion injury: the transplant process itself can injure tissue—especially if the organ had prolonged cold time or early graft dysfunction—making vessels more vulnerable later.
Non-immune causes that still matter
Many transplant recipients develop classic cardiovascular and metabolic risks, sometimes worsened by immunosuppression. These factors can accelerate vessel disease in the graft:
- High LDL cholesterol and triglycerides
- High blood pressure
- Diabetes or insulin resistance
- Chronic kidney disease
- Smoking exposure (active or secondhand)
- Obesity, inactivity, and untreated sleep apnea
Infections and inflammation as accelerators
Infections can temporarily raise inflammatory signals and clotting tendency, stressing the endothelium. Certain viral infections have been linked to faster vascular changes in some transplant settings. Even when the infection resolves, the “aftershock” of inflammation can contribute to ongoing vessel remodeling.
Medication-related contributors
Immunosuppressive drugs are essential, but they can indirectly raise risk by worsening blood pressure, lipids, glucose, or kidney function. This is not a reason to stop them; it is a reason to manage side effects aggressively and keep immunosuppression stable and consistent.
The main practical takeaway: in many patients, graft vasculopathy forms when immune pressure plus traditional risk factors converge. Effective prevention usually targets both sides at once.
Who is at higher risk?
Risk is not identical across all transplant recipients. Two people can have the same organ transplant and very different long-term vessel outcomes. Clinicians usually estimate risk by combining transplant-related factors, medical conditions, and day-to-day stability (especially medication adherence).
Transplant-related risk factors
These factors often set the baseline level of vulnerability:
- Older donor age or donor vascular disease: donor vessels may already have early plaque or reduced resilience.
- Early graft dysfunction: when an organ struggles soon after transplant, the vascular bed may be more prone to later remodeling.
- Longer ischemic time: longer time without warm blood flow can increase endothelial injury.
- Rejection history: multiple episodes, severe episodes, or antibody-mediated rejection increase long-term vessel risk.
- Presence or development of donor-specific antibodies: persistent or rising antibodies can signal ongoing immune stress on vessels.
Medical risk factors that amplify vessel damage
These often determine how quickly disease progresses:
- High LDL cholesterol: persistent elevation increases plaque formation and endothelial dysfunction.
- Hypertension: chronically high pressure mechanically stresses vessel walls and speeds scarring.
- Diabetes: increases inflammation, impairs vessel repair, and worsens small-vessel disease.
- Kidney dysfunction: contributes to vascular calcification and limits medication options.
- Chronic inflammatory conditions: autoimmune disease, uncontrolled infections, or ongoing inflammatory states can raise baseline risk.
Behavioral and systems factors that are surprisingly important
These are common, real-world reasons graft vasculopathy progresses faster than expected:
- Medication nonadherence: missed or late doses of immunosuppression can trigger “mini-rejections” that add up over time.
- Inconsistent follow-up: missing surveillance testing may allow silent progression for years.
- Unmanaged side effects: nausea, tremor, swelling, or mood changes can quietly erode adherence unless treated directly.
- Smoking, vaping, or ongoing nicotine exposure: strongly linked with vascular injury and worse long-term outcomes.
A practical way to think about your personal risk
Many transplant teams informally group risk into three buckets:
- Immune risk: rejection pattern, antibodies, stability of immunosuppression
- Metabolic risk: LDL, blood pressure, glucose, body weight, kidney function
- Lifestyle/system risk: smoking, activity, sleep, follow-up consistency, medication access
If two buckets are elevated, clinicians usually tighten surveillance and prevention. If all three are elevated, the focus often shifts to building a “durable plan” that makes adherence and risk control realistic—not just ideal on paper.
Symptoms and complications by organ
Graft vasculopathy can look very different depending on the transplanted organ. The shared theme is reduced blood flow and chronic injury, but the day-to-day signals vary—sometimes so subtly that only structured testing detects the problem early.
Heart transplant
In heart recipients, graft vasculopathy often affects the coronary arteries in a diffuse way and may involve small vessels. Symptoms can be atypical. Possible signs include:
- New shortness of breath with exertion
- Unusual fatigue or declining exercise tolerance
- Palpitations, dizziness, or fainting
- Fluid retention (leg swelling, rapid weight gain)
- Chest pressure may occur, but it may be absent even with significant disease
Complications can include silent ischemia, heart failure, arrhythmias, myocardial infarction, and sudden cardiac death—especially when disease is advanced or rapidly progressive.
Kidney transplant
In kidney recipients, graft vasculopathy may be part of chronic rejection affecting small vessels and larger arteries. Common presentations include:
- Gradual rise in creatinine or slow loss of estimated kidney function
- New or worsening high blood pressure
- Protein in the urine (sometimes increasing over time)
- Swelling from fluid retention if function declines significantly
Complications include chronic graft scarring, progressive kidney failure, higher cardiovascular risk, and eventual return to dialysis or evaluation for retransplantation.
Liver transplant
In liver recipients, vascular problems may contribute to ischemic-type biliary injury or chronic graft dysfunction in selected cases. Symptoms can be non-specific (fatigue, itching, abdominal discomfort) and are often detected through lab trends and imaging rather than early symptoms.
Lung transplant and other grafts
In lung transplantation, the best-known long-term complication is chronic graft dysfunction that often involves airways more than large vessels, but microvascular injury and chronic immune activation still matter. In vascularized composite allografts (such as hand or face transplants), chronic vascular changes can contribute to tissue injury over time.
General red flags across graft types
Regardless of organ, take these patterns seriously:
- A steady decline in function on routine labs or home measurements
- New exercise intolerance, breathlessness, or swelling
- New rhythm symptoms (palpitations, fainting)
- Recurrent infections or inflammatory flares that destabilize the course
- Any abrupt change after missed immunosuppression doses
Because early symptoms may be subtle, consistent follow-up and scheduled surveillance are often the “early symptom” that matters most.
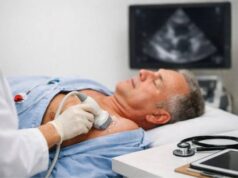
How graft vasculopathy is diagnosed
Diagnosis relies on matching the test to the organ and the suspected vessel level (large vessels vs microvasculature). In many cases, clinicians monitor for early disease even when you feel well, because waiting for symptoms can mean missing the window where interventions have the greatest impact.
Core principles of evaluation
Most transplant programs try to answer four questions:
- Is there evidence of vessel narrowing or impaired blood flow?
- Is the problem diffuse, focal, or microvascular?
- Is graft function affected yet?
- Is immune activity (rejection or antibodies) contributing right now?
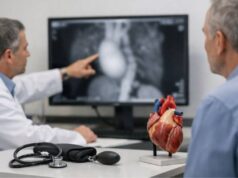
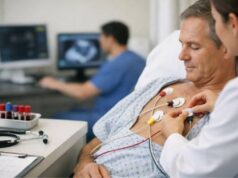
Heart transplant testing
Common tools include:
- Coronary angiography: maps the vessel lumen and can identify significant narrowing, but early diffuse disease may be missed.
- Intravascular imaging: ultrasound or high-resolution catheter imaging can detect early wall thickening even when angiography looks near-normal.
- Physiologic flow assessment: specialized measurements may show reduced reserve or microvascular dysfunction.
- Noninvasive stress imaging: selected stress tests can evaluate perfusion and help track progression in some patients.
Clinicians often use a “baseline plus surveillance” approach, increasing testing frequency if risk is higher or changes appear.
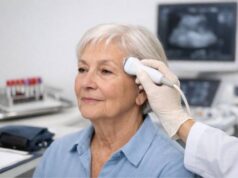
Kidney transplant testing
Kidney graft vasculopathy is often evaluated through a combination of:
- Blood and urine trends: creatinine trajectory, proteinuria changes, and blood pressure patterns
- Doppler ultrasound: assesses blood flow and can detect significant stenosis, resistive changes, or other vascular concerns
- Allograft biopsy: often the most definitive way to identify chronic rejection patterns and microvascular injury
- Antibody testing: detects donor-specific antibodies that can signal ongoing immune-driven damage
Because many kidney issues mimic each other (medication toxicity, infection, obstruction, dehydration), clinicians often interpret biopsy and antibody results alongside imaging and clinical context.
Staging and tracking progression
Staging varies by organ and center, but progression is often assessed by:
- Comparing imaging year-to-year (or test-to-test)
- Tracking function trends (echo parameters, creatinine slope, oxygen needs, etc.)
- Watching for immune signals (antibodies, biopsy activity, inflammatory markers where used)
A helpful patient question is: “Are we seeing stability, slow progression, or rapid progression—and what is our plan for the next 6–12 months based on that?”
Treatment options and what to expect
Treatment aims to slow progression, protect graft function, and reduce major events. Plans are usually layered: adjust immune drivers when appropriate, control traditional vascular risk factors aggressively, and consider procedures only when anatomy allows meaningful benefit.
1) Optimize immunosuppression and treat active immune injury
If testing suggests ongoing immune damage (for example, active rejection patterns or harmful antibodies), clinicians may:
- Adjust immunosuppressive dosing for better long-term stability
- Treat active rejection episodes promptly
- Address adherence barriers (side effects, complex schedules, medication access)
In many patients, the most powerful “treatment” is not a new drug—it is consistent, stable immunosuppression that prevents repeated immune flares.
2) Aggressive risk-factor control
Because graft vessels are vulnerable, many teams manage risk factors more intensively than in non-transplant patients:
- Lipid lowering: statins are commonly used, especially after heart transplant, and may help beyond cholesterol reduction.
- Blood pressure control: often requires more than one medication; steady control protects both vessels and organ function.
- Glucose management: preventing large glucose swings and improving insulin sensitivity can reduce vascular stress.
- Kidney protection strategies: avoiding dehydration and carefully balancing medications can preserve long-term function.
3) Antiplatelet and anticoagulation decisions
Some patients benefit from antiplatelet therapy (such as aspirin) depending on graft type and vascular findings. Anticoagulation is more selective and depends on competing risks (bleeding history, other clot risks, organ function, and the clinical setting). The safest approach is individualized rather than “one-size-fits-all.”
4) Procedures when disease is focal and treatable
When graft vasculopathy produces discrete, high-grade lesions—most commonly discussed in heart transplant coronary disease—interventions may include angioplasty and stenting. Limits are important:
- Diffuse disease may not be stentable in a durable way
- Small-vessel disease may drive symptoms even when large vessels look mild
- Restenosis risk can be higher than in typical atherosclerosis
5) Advanced options
If graft function declines despite maximal therapy, teams may consider advanced supportive care, mechanical support in selected heart cases, or evaluation for retransplantation when appropriate.
What to expect overall: the goal is often a measurable stabilization—slower decline on imaging and function tests, fewer events, and longer graft survival—rather than a quick “cure.”
Long-term management, prevention, and when to seek care
Long-term success with graft vasculopathy prevention is built on consistent routines. Many patients do best when the plan is concrete, trackable, and realistic—because the biggest risk is often quiet drift rather than a single dramatic event.
Daily and weekly habits that protect graft vessels
- Take immunosuppression on schedule, every day. If you miss a dose, follow your transplant team’s instructions rather than improvising.
- Track a small set of home data: weight, blood pressure, heart rate, and (if relevant) blood sugar. Trends are more important than single readings.
- Move consistently: aim for at least 150 minutes/week of moderate activity when cleared, divided across the week. For many people, brisk walking 25–30 minutes most days is a realistic baseline.
- Eat for vessel health: prioritize vegetables, legumes, whole grains, lean proteins, and unsalted nuts; limit processed foods high in salt, sugar, and refined carbs.
- Avoid nicotine in all forms. If quitting is difficult, ask for a structured cessation plan—support improves success rates.
- Prevent infections: follow vaccine recommendations and practical precautions during high-risk seasons, because infections can trigger inflammatory stress on vessels.
Medication and supplement safety
Transplant medications can interact with common over-the-counter drugs and supplements. A simple rule: do not start new supplements, herbals, or “detox” products without checking first. Many problems that look like “progression” are actually medication-level instability caused by interactions.
Surveillance that makes sense
Ask your team what your center uses for:
- Routine screening intervals
- Triggers for earlier testing (rejection episode, antibody changes, functional decline)
- The single most important “marker” they want you to watch at home
This turns surveillance into a partnership instead of a series of scary tests.
When to seek urgent help
Seek emergency care for:
- Severe shortness of breath at rest, fainting, or new confusion
- Sudden chest pressure with sweating, nausea, or weakness
- New one-sided weakness, speech trouble, or severe dizziness
- Rapidly worsening swelling, especially with breathlessness
- Any sudden, dramatic change your transplant team has warned you about for your specific organ
Contact your transplant team promptly (same day) for:
- New or steadily worsening exercise intolerance or fatigue
- Palpitations that are new, frequent, or associated with dizziness
- Persistent fever or signs of infection
- Noticeable trends in home readings (weight gain, rising blood pressure)
- Any repeated missed doses or medication access problems
The long game is steady: keep immune activity quiet, keep vascular risks controlled, and catch early changes before they become irreversible.
References
- ISHLT Guidelines for the Care of Heart Transplant Recipients 2022 (Guideline) ([Default][1])
- Cardiac Allograft Vasculopathy: A Focus on Advances in Diagnosis and Management 2025 (Review) ([PMC][2])
- Cardiac Allograft Vasculopathy: Challenges and Advances in Invasive and Non-Invasive Diagnostic Modalities 2024 (Review) ([PMC][3])
- Chronic Rejection After Kidney Transplantation 2024 (Review) ([PMC][4])
Disclaimer
This article is for educational purposes and does not replace personalized medical advice, diagnosis, or treatment. Graft vasculopathy can progress without obvious symptoms, and the right evaluation depends on your transplanted organ, your immunosuppression regimen, and your overall health. If you have a transplant and develop new chest discomfort, severe shortness of breath, fainting, sudden weakness, rapidly worsening swelling, a sharp drop in urine output, or signs of infection, seek urgent medical care and contact your transplant team. Never start, stop, or change immunosuppressive, antiplatelet, or anticoagulant medications—or supplements—without guidance from your transplant clinicians, because both rejection and bleeding/clot risks must be balanced carefully.
If you found this article helpful, please consider sharing it on Facebook, X (formerly Twitter), or any platform you prefer, and follow us on social media. Your support through sharing helps our team continue producing reliable, patient-centered health content.