Granulomatous myocarditis is a rare form of myocarditis—inflammation of the heart muscle—in which the body forms granulomas, or small clusters of immune cells. These clusters can interfere with how the heart pumps and how electrical signals travel through it. Some people develop symptoms over weeks to months; others arrive suddenly with fainting, dangerous heart rhythms, or heart failure.
What makes this condition different is that treatment depends heavily on the cause. In many cases, granulomatous myocarditis is linked to inflammatory diseases such as cardiac sarcoidosis, but infections and certain immune disorders can also trigger it. Because the stakes can be high—and early symptoms can be subtle—timely diagnosis, careful rhythm monitoring, and a tailored treatment plan make a meaningful difference in recovery and long-term heart protection.
Table of Contents
- What granulomatous myocarditis does to the heart
- Causes and risk factors you should know
- Symptoms, red flags, and complications
- How it is diagnosed and confirmed
- Treatments that target inflammation and rhythm
- Monitoring, recovery, and when to seek care
What granulomatous myocarditis does to the heart
Granulomatous myocarditis means the heart muscle is inflamed in a specific pattern: immune cells gather into organized clusters (granulomas) within the myocardium and sometimes the heart’s conduction system. The heart then faces two problems at once—mechanical strain (how well it pumps) and electrical instability (how reliably it conducts impulses).
Why granulomas can be so disruptive
The heart is not built to tolerate “patchy islands” of inflammation. Granulomas can:
- Irritate or injure nearby muscle cells, weakening contraction
- Create scar over time, making the heart stiffer and less efficient
- Interrupt the pathways that carry electrical signals, causing slow heart rates or block
- Form an unstable border between healthy and inflamed tissue, which can trigger fast rhythms
This is why granulomatous myocarditis may show up as fainting or palpitations even before classic heart failure symptoms appear.
Two patterns clinicians watch for
Although real cases vary, many clinicians think in terms of two overlapping phases:
- Active inflammation: the immune process is “hot,” and symptoms can change quickly. This stage may respond best to targeted anti-inflammatory therapy when the cause is non-infectious.
- Residual scarring: even after inflammation settles, scar can remain. Scar is not “active disease,” but it can still create rhythm risk and reduced pumping reserve.
The distinction matters because imaging and treatment goals change. Inflammation-focused therapies aim to reduce immune activity; scar-focused management emphasizes rhythm protection and heart failure care.
How it differs from more common myocarditis
Many cases of myocarditis are lymphocytic (often post-viral). Granulomatous myocarditis is different because it often reflects a broader immune disorder (like sarcoidosis) or, less commonly, a chronic infection. It can also overlap with giant cell myocarditis, a related but typically more aggressive immune-mediated myocarditis that can progress rapidly and may require urgent, multi-drug immunosuppression.
Why early recognition helps
When granulomatous myocarditis is identified early, clinicians can do three things sooner:
- Search for the underlying cause (which directs therapy)
- Monitor rhythm risk closely (because conduction disease can emerge abruptly)
- Start heart-protective treatment before long-term scarring accumulates
That combination can lower the risk of sudden deterioration and improve the odds of durable recovery.
Causes and risk factors you should know
“Granulomatous myocarditis” describes what the tissue looks like under the microscope, not a single disease. The most important clinical step is identifying the driver behind the granulomas, because the right treatment for one cause can be harmful for another (for example, immunosuppression can worsen an untreated infection).
Common non-infectious causes
These are often the leading causes in many cardiology practices:
- Cardiac sarcoidosis: granulomas develop as part of a systemic inflammatory disease that often involves lungs and lymph nodes, but sometimes the heart is the main site.
- Autoimmune and inflammatory disorders: conditions that dysregulate immune signaling can involve the heart, sometimes alongside lung, skin, eye, or joint symptoms.
- Giant cell myocarditis spectrum: some cases show granulomatous features and behave aggressively, with rapid onset heart failure and malignant arrhythmias.
Infectious causes to consider
Infections can also produce granulomas, particularly when the immune system is trying to wall off a persistent organism. Examples include:
- Mycobacterial infections (such as tuberculosis)
- Fungal infections (more likely with immunosuppression or certain exposures)
- Other chronic infections depending on geography and immune status
Infection-related granulomatous myocarditis is uncommon, but it is critical to recognize because treatment centers on targeted antimicrobial therapy—and steroids may be used only in carefully selected situations under specialist guidance.
Risk factors that raise suspicion
You cannot “catch” granulomatous myocarditis from a single risk factor, but certain histories increase the chance clinicians will consider it earlier:
- Known systemic sarcoidosis or prior granulomatous disease
- Unexplained high-degree heart block or ventricular tachycardia, especially in a younger or middle-aged adult
- Recurrent fainting or near-fainting with abnormal ECG findings
- Autoimmune disease history (thyroid disease, inflammatory bowel disease, connective tissue disease)
- Immunosuppression (transplant medications, chemotherapy, long-term steroids) that increases risk for opportunistic infections
- Travel, occupational, or environmental exposures that raise infection likelihood (context matters)
Clues outside the heart that help find the cause
Because the heart is difficult to biopsy reliably, clinicians often look for safer tissue targets:
- Enlarged lymph nodes, lung changes, or skin lesions that can be sampled
- Eye inflammation, nerve symptoms, or unexplained cough that points toward systemic disease
- Fevers, night sweats, weight loss, or chronic fatigue that broadens the infectious and inflammatory differential
A practical takeaway: the “cause workup” is not a distraction—it is the core of safe care, because granulomatous myocarditis sits at the intersection of cardiology, infectious disease, and immunology.
Symptoms, red flags, and complications
Symptoms vary widely. Some people experience a slow buildup of fatigue and shortness of breath; others present abruptly with fainting or life-threatening arrhythmias. Many symptoms reflect either reduced pumping ability, electrical conduction problems, or both.
Common symptoms
Granulomatous myocarditis may cause:
- Palpitations or a racing heartbeat
- Dizziness, near-fainting, or fainting
- Shortness of breath with exertion or at rest
- Chest discomfort (not always “classic” chest pain)
- Unusual fatigue or reduced exercise tolerance
- Swelling in the legs, abdominal bloating, or rapid weight gain from fluid retention
Because conduction tissue can be involved, symptoms related to slow heart rhythm are especially important—fatigue that feels “sudden,” repeated lightheadedness, or blackouts without warning.
Red flags that deserve urgent evaluation
Seek urgent care (or emergency care, depending on severity) if you have:
- Fainting, especially with palpitations or chest discomfort
- New or worsening shortness of breath at rest
- A sustained rapid heartbeat, or a rapid heartbeat with dizziness
- New severe chest pressure, sweating, nausea, or marked weakness
- New neurologic symptoms such as one-sided weakness or speech trouble
In granulomatous myocarditis, a person can look “stable” and still be at risk for sudden rhythm changes, so clinicians take these red flags seriously.
Complications clinicians actively monitor
Major complications are driven by inflammation, scarring, or both:
- Conduction disease: first-degree block can progress to high-degree block, sometimes rapidly
- Ventricular arrhythmias: ventricular tachycardia can recur even after symptoms improve
- Heart failure: reduced ejection fraction or restrictive physiology from scarring
- Cardiogenic shock: uncommon overall, but more likely in aggressive immune-mediated forms
- Thromboembolism risk: severe heart dysfunction can raise clot risk in the heart chambers
- Sudden cardiac death risk: mainly tied to ventricular arrhythmias and scar burden
How symptoms change over time
Many patients experience “waves”—periods of improvement followed by flare-like setbacks. This can happen because inflammation fluctuates, medications are tapered, or a hidden trigger persists. A useful pattern to watch is trend rather than single days:
- You can do less week-by-week
- Your resting heart rate rises without explanation
- You develop repeated episodes of dizziness or palpitations
- Your weight increases by several kilograms over a short period with swelling and breathlessness
These patterns should prompt reassessment, because they can signal active inflammation, rhythm instability, or worsening heart function.
How it is diagnosed and confirmed
Diagnosis usually combines clinical suspicion, heart imaging, rhythm monitoring, and—when feasible—tissue confirmation. Because granulomatous myocarditis can be patchy, a single test rarely tells the whole story. Clinicians aim to confirm three things: inflammation is present, granulomatous disease is likely, and the underlying cause is identified as safely as possible.
First-line tests most patients receive
Common starting points include:
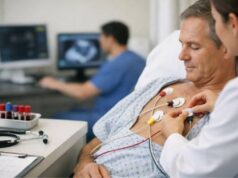
- ECG and continuous rhythm monitoring: looks for heart block, ventricular ectopy, or sustained arrhythmias
- Blood tests: cardiac troponin can be elevated with active injury; BNP/NT-proBNP helps assess heart strain
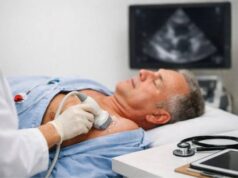
- Echocardiogram: assesses pumping function, wall motion changes, valve function, and pericardial effusion
- Chest imaging and basic labs: helpful when systemic disease is suspected (lungs, lymph nodes, inflammatory markers)
These tests often show that “something is wrong,” but they are not specific enough to define the cause.
Advanced imaging that refines the diagnosis
Many centers rely on two advanced approaches:
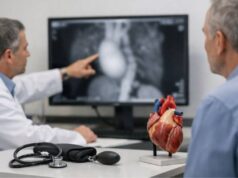
- Cardiac MRI: can detect edema (active inflammation) and late gadolinium enhancement (scar or active injury patterns). Certain distributions raise suspicion for granulomatous processes.
- FDG-PET (often combined with perfusion imaging): highlights metabolically active inflammation and can detect extracardiac targets for biopsy. PET is also useful for tracking response to therapy over time.
Clinicians often pair these tests: MRI helps define scar pattern and anatomy; PET helps define active inflammation and treatment response.
Biopsy: the gold standard with real limitations
- Endomyocardial biopsy can confirm granulomas, giant cells, or other diagnostic features, but sampling error is common because disease can be patchy.
- Some centers use electroanatomic mapping–guided biopsy to target abnormal areas and improve yield.
- When available, biopsy specimens may undergo specialized staining and molecular testing to assess for infectious organisms.
Because biopsy carries procedural risk and may miss the lesion, many teams pursue extracardiac biopsy first when a safe target exists (for example, lymph nodes or lung tissue).
Finding the cause safely
Clinicians often coordinate cardiology, electrophysiology, pulmonology, rheumatology, and infectious disease to answer:
- Is this most consistent with sarcoidosis, a different autoimmune process, or infection?
- Is immunosuppression safe to start now, or must infection be ruled out first?
- What objective markers will be used to judge improvement (symptoms, rhythm burden, imaging activity, function)?
A clear diagnostic plan is as important as the diagnosis itself, because it determines both safety and long-term outcomes.
Treatments that target inflammation and rhythm
Treatment is usually “two-track”: control inflammation when appropriate and protect the heart from rhythm and heart failure complications. The exact plan depends on whether the cause is non-infectious (often treated with immunosuppression) or infectious (treated with organism-specific therapy, sometimes with carefully selected adjunctive anti-inflammatory treatment).
Anti-inflammatory treatment when the cause is non-infectious
For cardiac sarcoidosis and related immune-driven granulomatous myocarditis, clinicians often use a tiered approach:
- Corticosteroids as first-line therapy: dosing varies, but many regimens start with a higher daily dose (often in the range of prednisone 0.5–1 mg/kg/day) followed by a slow taper over months, guided by symptoms, imaging, and rhythm burden.
- Steroid-sparing immunosuppressants: added when disease is severe, relapses during taper, or steroid side effects are significant. Choices depend on patient factors, infection risk, and organ function.
- Escalation for aggressive disease: in fulminant or giant cell–spectrum cases, teams may use high-intensity regimens early (sometimes including short-course IV steroids such as methylprednisolone 500–1,000 mg/day for 3 days) plus combination immunosuppression in specialized settings.
The key principle is balance: suppress harmful inflammation while minimizing infection risk and medication toxicity.
Treating infectious causes
If infection is suspected or confirmed, treatment centers on targeted antimicrobial therapy directed by cultures, pathology, and specialist input. For example:
- Tuberculosis-related disease typically requires multi-drug therapy over many months.
- Fungal causes require prolonged antifungal treatment, often with close drug-level and toxicity monitoring.
In these cases, immunosuppression is approached cautiously and usually only with coordinated infectious disease oversight.
Heart failure and rhythm protection
Even when inflammation improves, supportive cardiac care remains essential:
- Guideline-directed heart failure therapy when pumping function is reduced
- Antiarrhythmic strategies for recurrent ventricular tachycardia (medication, catheter ablation in selected cases)
- Device therapy: pacemaker for high-degree block; ICD consideration for sustained ventricular arrhythmias, high-risk scar patterns, or persistently reduced ejection fraction
- Temporary mechanical circulatory support for cardiogenic shock in severe cases
What “response” looks like
Clinicians typically define improvement using objective markers:
- Fewer arrhythmia episodes on monitoring
- Improved symptoms and exercise tolerance
- Stabilized or improved ejection fraction
- Reduced inflammatory activity on PET (when used)
- A safer taper plan without relapse
Treatment often continues for many months, and follow-up is deliberate—because relapse risk is real, especially during dose reductions.
Monitoring, recovery, and when to seek care
Recovery from granulomatous myocarditis is rarely a straight line. Many patients do well when care focuses on three practical goals: prevent sudden rhythm events, track inflammation objectively, and support a gradual return to activity without provoking setbacks.
Monitoring that protects you between visits
Your team may recommend a tailored set of tools depending on severity:
- Rhythm monitoring: periodic Holter monitors, event monitors, or device interrogations (if you have a pacemaker/ICD) to quantify arrhythmia burden
- Repeat imaging: cardiac MRI and/or FDG-PET at planned intervals to distinguish active inflammation from stable scar
- Lab trends: biomarkers for heart strain and medication safety (liver, kidney, blood counts), especially during immunosuppressive therapy
At home, simple tracking can be surprisingly useful:
- Daily or near-daily weight during active disease
- Blood pressure and resting heart rate trends
- A symptom log for palpitations, dizziness, exertional limits, and sleep quality
Medication safety and infection prevention
If you are on immunosuppressive therapy, prevention becomes part of treatment:
- Report fevers, persistent cough, painful urination, or skin infections early.
- Avoid starting new supplements or over-the-counter drugs without checking first; drug interactions can destabilize therapy.
- Ask your clinician which vaccines are appropriate for your situation and timing.
A practical insight: many “relapses” are first noticed as increasing arrhythmias or unexplained fatigue, not dramatic chest symptoms.
Exercise and return to normal life
Because myocarditis can carry exercise-related rhythm risk during active inflammation, clinicians often advise:
- Restrict vigorous activity during the acute/active phase
- Reintroduce moderate activity gradually after stabilization, guided by imaging, rhythm monitoring, and symptoms
- Use cardiac rehabilitation when available, especially if you had heart failure or deconditioning
A common target for long-term health—once cleared—resembles standard cardiovascular goals (about 150 minutes/week of moderate activity), but the pace to get there should be individualized.
When to seek urgent care
Seek emergency care for:
- Fainting, near-fainting with palpitations, or new severe dizziness
- Severe shortness of breath at rest or rapidly worsening swelling
- Sustained rapid heartbeat, chest pressure, or new confusion
- New neurologic symptoms (weakness, speech difficulty)
Contact your clinician promptly for:
- Increasing palpitations, especially if they cluster or wake you from sleep
- New exercise intolerance that persists for more than a few days
- Signs of infection while on immune-suppressing treatment
- Medication side effects that make adherence difficult
With the right surveillance and a cause-specific treatment plan, many patients stabilize and regain a good quality of life—even if they need long-term rhythm follow-up.
References
- Diagnosis and Management of Cardiac Sarcoidosis: A Scientific Statement From the American Heart Association 2024 (Guideline/Statement)
- 2024 ACC Expert Consensus Decision Pathway on Strategies and Criteria for the Diagnosis and Management of Myocarditis: A Report of the American College of Cardiology Solution Set Oversight Committee 2025 (Guideline)
- Management of Patients With Giant Cell Myocarditis: JACC Review Topic of the Week 2021 (Review)
- Cardiac Sarcoidosis: A Comprehensive Clinical Review 2024 (Review)
Disclaimer
This article is for educational purposes and does not replace medical advice, diagnosis, or treatment. Granulomatous myocarditis can involve dangerous heart rhythm problems and heart failure, and the safest evaluation depends on your symptoms, medical history, and test results. If you have fainting, severe shortness of breath, chest pressure, a sustained rapid heartbeat, new confusion, or stroke-like symptoms, seek emergency care. Never start, stop, or change steroids, immunosuppressive drugs, antiarrhythmics, or heart medicines without guidance from a qualified clinician, because both undertreatment and overtreatment can cause harm.
If you found this article helpful, please share it on Facebook, X (formerly Twitter), or any platform you prefer, and follow us on social media. Your support through sharing helps our team keep producing clear, reliable health content.