Granulomatous pericarditis is inflammation of the pericardium—the sac around the heart—in which the body forms granulomas, or small clusters of immune cells. This pattern matters because it often points to a specific underlying cause, such as tuberculosis or sarcoidosis, rather than the more common “viral” pericarditis. In some people it behaves like a typical inflammatory episode with sharp chest pain; in others it builds quietly, leading to fluid around the heart or scarring that restricts heart filling.
The most helpful way to approach granulomatous pericarditis is to think in two tracks at once: treat the immediate pericardial inflammation and—just as important—identify what is driving the granulomas. That combination is what prevents relapse, long-term scarring, and dangerous complications.
Table of Contents
- What granulomatous pericarditis means for the heart
- Causes and risk factors that shape care
- Symptoms and complications you should not ignore
- How doctors diagnose it and find the cause
- Treatment options, from anti-inflammatory to cause-specific therapy
- Long-term management, prevention, and when to seek urgent help
What granulomatous pericarditis means for the heart
Granulomatous pericarditis is a diagnosis based on tissue pattern: the pericardium shows granulomas—organized collections of immune cells that form when the body is trying to contain something persistent (an infection, an inflammatory trigger, or an immune misfire). That tissue clue is powerful because it shifts the clinical question from “How do we calm this episode?” to “What is the deeper cause we must treat to prevent repeat injury?”
How the pericardium gets injured
In most inflammatory pericarditis, the pericardium becomes irritated, swollen, and painful, often after a virus. With granulomas, the immune response tends to be more structured and more durable. Over time, repeated inflammation can lead to:
- Pericardial effusion: fluid builds up in the sac around the heart. Small effusions may cause few symptoms; large or fast-growing effusions can compress the heart.
- Thickening and scarring: the pericardium can become rigid, limiting how the heart fills between beats.
- Adhesions and loculated fluid: fluid pockets may form that do not drain evenly, complicating procedures.
A key practical point: granulomatous inflammation can coexist with “standard” pericarditis findings (chest pain, ECG changes, elevated inflammatory markers). The difference is what the pattern suggests about cause and recurrence risk.
Why it can become constrictive
The heart needs room to expand as it fills. A healthy pericardium stretches slightly. When granulomatous inflammation persists, healing may lay down collagen and calcification. This can produce constrictive physiology, where the heart is squeezed by a stiff shell. Some people develop a reversible, “transient constrictive” stage that improves when inflammation is treated early. Others develop fixed constriction that may require surgery.
What makes this diagnosis high-stakes
Granulomatous pericarditis raises the likelihood of causes that require targeted therapy—especially tuberculosis in the right clinical setting. If the driver is missed, anti-inflammatory treatment alone may temporarily improve symptoms while the underlying process continues, increasing the risk of:
- recurrent effusions
- tamponade (dangerous pressure on the heart)
- chronic scarring and constriction
- systemic spread of an untreated infection
The good news is that when clinicians identify the cause early, many patients do very well—because treatment becomes specific rather than guesswork.
Causes and risk factors that shape care
Granulomatous pericarditis has a shorter list of likely causes than typical pericarditis. Clinicians usually group them into infectious and non-infectious categories, because the direction of treatment is very different. The central safety rule is simple: if an infection is plausible, it must be evaluated carefully before strong immune-suppressing therapy is started.
Infectious causes
In many parts of the world, tuberculosis (TB) is the most important infectious cause to consider. TB can involve the pericardium directly, or spread from nearby lymph nodes, lungs, or pleura. Granulomas with central necrosis on pathology raise suspicion, but clinical context still matters.
Other infections can also produce granulomatous patterns, especially in people with impaired immunity:
- Fungal infections (risk rises with transplant medications, chemotherapy, advanced HIV, or long-term steroids)
- Non-tuberculous mycobacteria (less common, but possible in specific exposure and immune settings)
- Less commonly, other chronic infections depending on geography and occupational exposure
Non-infectious inflammatory causes
These tend to be diagnosed by combining heart imaging with signs of disease elsewhere in the body:
- Sarcoidosis: granulomas can involve lungs, lymph nodes, skin, eyes, and sometimes the heart and pericardium. Pericardial involvement is uncommon, but it is well recognized.
- Autoimmune disease: rheumatoid arthritis, lupus, vasculitis, and related immune disorders can inflame the pericardium and occasionally produce granulomatous features.
- Post-surgical or post-radiation inflammatory states: these usually cause non-granulomatous pericarditis, but complex immune healing responses can confuse the picture, especially if tissue sampling is limited.
Risk factors that raise suspicion in real life
Doctors weigh risk factors heavily because granulomatous pericarditis is uncommon and tests can be imperfect. Examples include:
- TB exposure, prior TB, living in or travel to TB-endemic regions, or close contact with TB
- Immunosuppression (transplant, biologic therapies, chemotherapy, advanced HIV)
- Unexplained weight loss, night sweats, prolonged fever, or chronic cough
- Known sarcoidosis or suggestive findings such as enlarged hilar lymph nodes
- Recurrent or persistent pericardial effusion that does not behave like typical “viral” pericarditis
- Early signs of constriction or effusive-constrictive physiology
A useful insight: granulomatous pericarditis is often suspected not because of a single symptom, but because the course is “stubborn”—symptoms recur, fluid returns, or constrictive features appear despite standard therapy.
Symptoms and complications you should not ignore
Granulomatous pericarditis can feel like classic pericarditis, but it is more likely to come with fluid, recurrence, and longer-lasting inflammation. Symptoms are shaped by three factors: inflammation, fluid volume and speed of accumulation, and whether scarring has begun to restrict the heart.
Common symptoms
Many people report a mix of these:
- Sharp or stabbing chest pain, often worse with deep breathing or lying flat and better when sitting forward
- Shortness of breath, especially when lying down or with exertion
- Low-grade fever and fatigue
- A dry cough or chest “heaviness” (sometimes from associated pleural or lung involvement)
- Reduced exercise tolerance that worsens over weeks
When TB is the cause, people may also report weight loss, drenching night sweats, or prolonged fevers. When sarcoidosis is the driver, symptoms outside the heart (cough, skin lesions, eye irritation) can be important clues.
Signs of pericardial effusion and tamponade
Fluid around the heart can be mild or life-threatening. Seek urgent evaluation if you develop:
- Rapidly worsening breathlessness
- Chest pressure rather than sharp pain
- Lightheadedness or fainting
- A sense of extreme weakness or “impending collapse”
A practical detail: a slowly growing effusion can become very large before symptoms are dramatic, while a fast-growing effusion can cause tamponade even when fluid volume is modest. The rate matters as much as the amount.
Complications clinicians watch for
Granulomatous pericarditis is associated with complications that shape long-term care:
- Recurrent pericarditis: symptoms return during tapering of treatment or after incomplete cause control.
- Effusive-constrictive pericarditis: fluid and constriction occur together, so drainage alone does not fully relieve pressure.
- Constrictive pericarditis: scarring limits filling, causing swelling, abdominal distention, and exertional breathlessness.
- Arrhythmias and myocardial involvement: less common than in myocarditis, but possible, especially in systemic inflammatory diseases that also involve the heart muscle.
How constriction can present (often missed early)
Constrictive symptoms can resemble liver or kidney problems, which is why they are sometimes overlooked. Watch for:
- Progressive leg swelling and rapid weight gain
- Abdominal swelling or fullness after small meals
- Shortness of breath that is out of proportion to chest pain
- Fatigue with minimal exertion
When these symptoms develop after a prolonged pericarditis course—particularly with persistent inflammation or a known TB/sarcoid context—clinicians evaluate for constriction early, because timely treatment can sometimes prevent permanent scarring.
How doctors diagnose it and find the cause
Diagnosis has two layers: confirming pericardial disease severity (inflammation, fluid, constriction) and identifying the underlying cause of the granulomas. Because tissue sampling of the pericardium is not always straightforward, clinicians often build a diagnosis using a combination of imaging, fluid analysis, and targeted biopsies from safer sites when available.
Initial evaluation
Most patients start with:
- History and exam: pain pattern, TB exposure, systemic symptoms, autoimmune history, immunosuppression, and signs of fluid overload.
- ECG and blood tests: inflammatory markers may be elevated; troponin is checked to assess for associated myocardial injury.
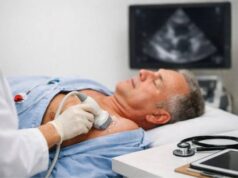
- Echocardiography: the first-line test to assess effusion size, tamponade physiology, and constrictive features.
Echocardiography is especially useful because it can be repeated frequently and shows how the heart is functioning in real time.
Imaging that adds crucial detail
When the course is complex, clinicians often use:
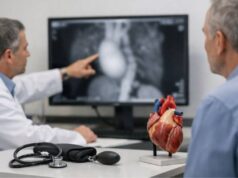
- Cardiac MRI: can show pericardial thickening, edema (active inflammation), and enhancement patterns that support an inflammatory process.
- CT scan: helps define pericardial thickness and calcification, and can identify lymph nodes or lung findings that suggest TB or sarcoidosis.
- FDG-PET (in selected cases): can reveal active inflammatory targets outside the heart that are safer to biopsy and can help track treatment response.
A useful insight: in granulomatous pericarditis, imaging is not just “confirmatory.” It helps decide whether the illness is mainly inflammatory (more reversible) or mainly scarred (less reversible), which changes both urgency and treatment goals.
Pericardiocentesis and fluid testing
If there is a moderate-to-large effusion, especially with symptoms, clinicians may drain fluid for diagnosis and relief. Fluid analysis may include:
- cell count and differential
- bacterial, mycobacterial, and fungal cultures (culture can take weeks for TB)
- tests that estimate TB likelihood (commonly including adenosine deaminase in many settings)
- cytology when malignancy is a concern
Because no single test is perfect, doctors often interpret fluid results alongside imaging and epidemiologic risk.
Biopsy and pathology
- Pericardial biopsy can confirm granulomas and may identify organisms with special staining or molecular testing.
- If a safer target exists (enlarged lymph nodes, lung lesions, skin lesions), clinicians may biopsy that site first to reduce procedural risk and improve yield.
In practice, the best diagnostic strategies are “layered”: start with echo and labs, add advanced imaging when needed, drain and test fluid when appropriate, and pursue biopsy in a targeted, safety-first way.
Treatment options, from anti-inflammatory to cause-specific therapy
Treatment works best when it addresses both the pericardial inflammation and the root cause of granuloma formation. The exact plan depends on whether an infection is driving the process, whether an autoimmune condition is active, and whether the pericardium is already becoming scarred and restrictive.
1) Stabilize urgent complications first
If tamponade is present or strongly suspected, urgent drainage and hemodynamic support come first. Similarly, if constrictive physiology is causing severe fluid overload, clinicians may use diuretics cautiously while clarifying whether the constriction is transient (inflammatory) or fixed (scarred).
2) Treat inflammation safely
For inflammatory pericarditis symptoms (pain, fever, elevated inflammatory markers), clinicians often use a familiar foundation:
- NSAIDs (such as ibuprofen or indomethacin) for pain and inflammation when kidney function and bleeding risk allow
- Colchicine to reduce relapse risk, often used for at least 3 months in acute pericarditis and longer in recurrent disease, tailored to tolerance and kidney function
- Corticosteroids when first-line therapy fails, when NSAIDs are contraindicated, or when a systemic inflammatory cause is likely
However, granulomatous pericarditis adds a crucial twist: steroids can be essential for sarcoidosis and some autoimmune causes, but they can be risky if an untreated infection is present. Many teams avoid starting high-dose steroids until TB and other infections are reasonably assessed, unless the clinical situation is life-threatening and requires immediate action.
3) Cause-specific therapy
- Tuberculous pericarditis: treatment centers on standard multi-drug anti-TB therapy for a full course (commonly at least 6 months, sometimes longer depending on response and local protocols). In selected patients, steroids may be added to reduce inflammation and complications, but decisions depend on HIV status, severity, and bleeding/infection risk profile.
- Sarcoidosis-related pericarditis: corticosteroids are commonly first-line. If relapse occurs during taper or side effects are significant, clinicians may add steroid-sparing therapy.
- Fungal or other opportunistic infections: prolonged targeted antimicrobial therapy is required, often with careful monitoring for drug interactions—particularly because many antifungals interact with heart and immune medications.
4) When surgery enters the discussion
If constrictive pericarditis becomes fixed and severely symptomatic, pericardiectomy (surgical removal of the pericardium) may be considered. This is a major operation, and outcomes depend on cause, timing, and surgical expertise. In many patients, the best results occur when surgery is performed before advanced organ congestion and malnutrition develop.
What “success” looks like
In granulomatous pericarditis, success is measured by more than pain relief:
- stable or shrinking effusion
- normalization of inflammation markers (when tracked)
- improved functional capacity
- no progression to constriction
- no relapse during careful medication tapering
A thoughtful plan emphasizes durability: the goal is not just feeling better this month, but preventing the next flare and protecting long-term heart filling.
Long-term management, prevention, and when to seek urgent help
Long-term management is about preventing recurrence, monitoring for constriction, and supporting recovery without exposing patients to avoidable medication harms. Because granulomatous pericarditis often reflects a systemic condition, follow-up commonly involves more than one specialty.
Monitoring that catches problems early
Clinicians often track progress with:
- Repeat echocardiography to monitor effusion size and filling patterns
- In selected cases, repeat MRI, CT, or PET to judge inflammation versus scarring
- Symptom trends: exertional breathlessness, swelling, abdominal fullness, and the ability to lie flat comfortably
- Medication safety labs when on long courses of anti-TB therapy, steroids, or immunosuppressive drugs
A practical habit that helps many patients: track weight and swelling. A gain of several kilograms over a short time—especially with leg swelling or abdominal distention—can be an early sign of worsening constriction or fluid retention.
Reducing relapse risk in daily life
These steps do not replace medical therapy, but they support stability:
- Take medications exactly as prescribed, especially long courses like anti-TB therapy
- Avoid abrupt steroid stopping; tapering should be planned and slow when used
- Limit alcohol if it worsens sleep, blood pressure, or medication adherence
- Prioritize sleep and gentle activity as tolerated; deconditioning can mimic “worsening heart disease”
- Discuss drug interactions before starting supplements or over-the-counter products
If TB was involved, public health measures (contact evaluation, adherence support) are part of prevention for both the patient and household.
Special considerations with immunosuppression
If steroids or other immunosuppressants are used, infection prevention becomes part of the treatment plan:
- report fevers, persistent cough, new shortness of breath, or urinary symptoms promptly
- ask which vaccines are appropriate for your situation and timing
- avoid exposure to known infectious risks when possible
A common real-world problem is “treating the pericarditis but losing the patient to side effects.” A good plan actively prevents complications such as stomach irritation from NSAIDs, glucose spikes from steroids, and drug interactions during anti-infective therapy.
When to seek urgent or emergency care
Seek emergency care now if you have:
- severe or rapidly worsening shortness of breath
- fainting, near-fainting, or extreme weakness
- chest pressure with sweating, nausea, or confusion
- signs of shock (cold clammy skin, very low blood pressure, collapse)
Contact your clinician promptly (same day) if you notice:
- increasing breathlessness or inability to lie flat
- rapid weight gain with swelling of legs or abdomen
- persistent fever or night sweats during treatment
- recurrence of sharp chest pain after initial improvement
The long-term goal is steady recovery with fewer surprises: control the driver of granulomas, reduce pericardial inflammation, and watch closely for early constrictive changes when they are most treatable.
References
- 2025 ESC Guidelines for the management of myocarditis and pericarditis 2025 (Guideline)
- Update on the diagnosis and treatment of pericardial diseases: a position paper of the Italian Society of Cardiology in collaboration with the study group on cardiomyopathies and pericardial diseases – PMC 2024 (Position Paper)
- Pericardial Diseases: International Position Statement on New Concepts and Advances in Multimodality Cardiac Imaging – PMC 2024 (Position Statement)
- Tuberculous Pericarditis-Own Experiences and Recent Recommendations – PubMed 2022 (Review)
- Pericardial Involvement in Sarcoidosis – PubMed 2022 (Systematic Review)
Disclaimer
This article is for educational purposes and does not replace medical advice, diagnosis, or treatment. Granulomatous pericarditis can lead to serious complications such as cardiac tamponade and constrictive pericarditis, and safe treatment depends on identifying the underlying cause (including ruling out infections like tuberculosis when appropriate). If you have severe or rapidly worsening shortness of breath, fainting, extreme weakness, chest pressure with sweating or confusion, or sudden worsening swelling, seek emergency care. Never start, stop, or change anti-tuberculosis therapy, corticosteroids, NSAIDs, colchicine, or immunosuppressive medications without guidance from a qualified clinician.
If you found this article helpful, please share it on Facebook, X (formerly Twitter), or any platform you prefer, and follow us on social media. Your support through sharing helps our team continue producing clear, reliable health content.