Great saphenous vein thrombosis is a blood clot in the longest surface vein of the leg. It often shows up as a tender, red “cord” along the inner thigh or calf, but it can also be subtle—especially early on. Many people assume a surface-vein clot is harmless. In reality, the main concern is where the clot sits and how far it extends, because clots near the groin can sometimes reach deeper veins and raise the risk of a more serious clot. Deep vein thrombosis (DVT) means a clot in a deeper leg vein. The good news is that with timely evaluation and the right treatment plan, most people recover well and avoid complications. This guide explains what it is, why it happens, what it feels like, how it’s diagnosed, and how to manage it safely.
Table of Contents
- What is great saphenous vein thrombosis?
- What causes great saphenous vein thrombosis?
- Early symptoms and possible complications
- How is it diagnosed?
- Which treatments work best?
- Recovery, prevention, and when to seek care
What is great saphenous vein thrombosis?
The great saphenous vein runs from the inner ankle up the inner leg and thigh to the groin, where it connects with the deep veins. A clot in this vein is a type of superficial vein thrombosis (SVT), meaning it affects a vein closer to the skin rather than a deep vein.
Even though it’s “superficial,” it deserves careful attention for three reasons:
- Location matters more than size alone. A short clot that sits very close to the groin connection can be more concerning than a longer clot farther down the thigh or calf.
- The great saphenous vein is a common pathway toward deep veins. If a clot grows upward toward the groin, it may extend into the deep system.
- Symptoms don’t reliably predict risk. Some people have dramatic redness and pain with a low-risk clot, while others have mild symptoms with a clot close to the deep junction.
You may hear older terms like “superficial thrombophlebitis.” That phrase highlights the inflammation (redness, warmth, tenderness) that often travels with the clot. Clinically, many teams now prefer “superficial vein thrombosis” because the clot—not just inflammation—drives treatment decisions.
A helpful way to think about it: this condition lives on a spectrum. On one end are small, localized clots in a varicose vein that stay put and settle with supportive care. On the other end are clots that sit near the groin connection (the saphenofemoral junction) or occur alongside other clot risks (like cancer or recent surgery), where blood-thinning medicine can prevent extension.
Common “settings” where great saphenous vein thrombosis occurs include:
- In varicose veins, especially after long standing or heat exposure.
- After vein procedures (laser/ablation, sclerotherapy, phlebectomy) or catheter placement.
- After long travel or immobilization, especially with dehydration.
- During or after pregnancy, or with estrogen-containing medications.
The key takeaway: great saphenous vein thrombosis is often treatable, but it should be evaluated with the goal of answering two questions—Is there a deeper clot now? and Is this clot close enough to the deep system to need anticoagulation?
What causes great saphenous vein thrombosis?
A clot forms when blood flow slows, the vein lining becomes irritated or injured, or the blood becomes more prone to clotting. In the great saphenous vein, these factors often overlap.
Common underlying causes
- Varicose veins and venous reflux. Twisted, enlarged surface veins slow blood flow and make localized clotting more likely. This is one of the most frequent contributors.
- Recent procedures or trauma. Vein ablation, sclerotherapy, IV lines, or direct injury can irritate the vessel lining and trigger clot formation.
- Reduced movement. Long flights, bed rest, casting, or recovery after illness can slow circulation in the legs.
- Systemic inflammatory or pro-clot conditions. Some illnesses tilt the body toward clotting, especially during active inflammation.
Risk factors that raise the chance of extension or recurrence
These factors matter because they influence both the likelihood of complications and how aggressive treatment should be.
- History of clotting: prior DVT, pulmonary embolism, or previous SVT.
- Active cancer or current cancer therapy: cancer can increase clot risk through multiple pathways.
- Hormones: estrogen-containing birth control or hormone therapy can raise clot risk, especially with smoking or inherited risk.
- Pregnancy and the postpartum period: clot risk increases during pregnancy and remains elevated after delivery.
- Recent surgery: orthopedic and pelvic surgeries are classic triggers; even smaller procedures can matter when combined with other risks.
- Obesity: can increase venous pressure and inflammation and often coexists with reduced mobility.
- Inherited or acquired clotting tendencies: examples include factor V Leiden or antiphospholipid syndrome. Testing is not routine for everyone, but it may be considered when clots are unprovoked, recurrent, or occur at a young age.
A practical “why now?” checklist
If you’re trying to make sense of a new diagnosis, it often helps to look back over the prior 6–8 weeks and ask:
- Was there a vein procedure, IV line, injury, or infection?
- Were you less active than usual (travel, illness, work constraints)?
- Did you start or change hormones?
- Are there new red flags such as unexplained weight loss, night sweats, or persistent fatigue that might warrant broader evaluation?
Sometimes, no clear trigger appears. When that happens, clinicians focus on confirming the clot’s location, checking for a deeper clot, and deciding whether prevention of extension (with anticoagulation) is the safest path.
A final point that surprises many people: antibiotics are usually not needed unless there are signs of skin infection (fever, spreading redness beyond the vein track, pus, or rapidly worsening pain). Most redness in this condition is inflammation related to clotting, not infection.
Early symptoms and possible complications
Great saphenous vein thrombosis often announces itself in a very “local” way—right where the vein runs. But complications can involve the deeper circulation and the lungs, which is why symptom awareness matters.
Common symptoms
Many people notice one or more of the following along the inner calf, knee, or thigh:
- Tenderness or burning pain along a line, worse when standing or walking
- Redness and warmth over a visible vein
- A firm, rope-like cord that feels thickened under the skin
- Localized swelling near the inflamed segment
- Itching or skin sensitivity over the vein track (less common)
Symptoms often peak over a few days and then slowly improve. The firm cord can take longer to soften—sometimes weeks.
When symptoms suggest a deeper clot
A superficial clot can coexist with a deep vein clot, or it can extend into deeper veins. Seek prompt evaluation if you have:
- Whole-leg swelling (not just a small area around the vein)
- New calf tightness or cramping that does not match the visible superficial track
- Pain deep in the calf rather than right under the skin
- Marked swelling of the thigh, especially if the clot is high in the inner thigh
These symptoms do not prove a deep clot, but they raise suspicion.
Signs of pulmonary embolism
A clot that reaches deeper veins can break off and travel to the lungs. Go to urgent or emergency care for:
- New shortness of breath, especially at rest
- Chest pain that worsens with deep breathing
- Coughing up blood
- Fast heart rate, fainting, or sudden severe weakness
Other complications to know
- Extension toward the groin connection. The closer the clot is to the deep-vein junction, the more carefully clinicians treat it.
- Recurrence. People with varicose veins, prior clots, or ongoing risk factors can have repeat episodes.
- Persistent discomfort and skin changes. Most recover fully, but a subset develops lingering tenderness, firmness, or discoloration along the vein.
- Post-procedure thrombosis. After vein ablation, a clot can form near the treated junction. This is managed with imaging-based risk assessment and, sometimes, anticoagulation.
A realistic timeline
While every case is different, a common pattern looks like this:
- Days 1–7: pain, redness, and a firm cord are most noticeable.
- Weeks 2–4: tenderness decreases; the cord remains but slowly softens.
- Weeks 4–8: most day-to-day symptoms resolve; some firmness may persist.
If pain or swelling worsens after initial improvement, it’s a reason to re-check—especially if the original clot was near the groin or if you were not placed on anticoagulation.
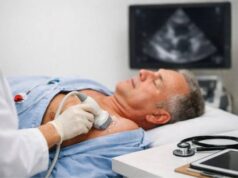
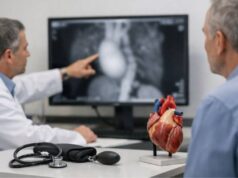
How is it diagnosed?
Diagnosis starts with a clinical exam, but imaging often provides the details that guide treatment decisions. The goal is not just to confirm a superficial clot—it’s to map its length and distance from the deep system, and to look for a deep clot that might be present without obvious symptoms.
Clinical assessment
A clinician typically asks about:
- Where the pain started and how it changed over time
- Recent travel, immobility, surgery, injury, or vein procedures
- Hormone use, pregnancy status, and past clot history
- Cancer history, recent infection, or inflammatory disease
- Bleeding risks (prior bleeding, stomach ulcers, liver disease, certain medications)
On exam, they look for a tender cord, localized warmth, and swelling patterns.
Compression ultrasound: the main test
Compression ultrasound is the workhorse test because it can:
- Confirm SVT and identify the affected segment of the great saphenous vein
- Measure how close the clot is to the groin connection
- Check for deep vein thrombosis in the leg
- Identify extension into connecting veins or the deep system
Because ultrasound findings drive treatment, it’s reasonable to ask your clinician whether the report includes:
- The clot’s most proximal point (how high it reaches)
- Whether it is within a “high-risk” distance to the deep junction
- Whether there is any deep clot at the same time
Blood tests: sometimes helpful, often not decisive
Routine blood work may be used to evaluate overall health or bleeding risk before anticoagulation. A D-dimer test can be elevated in many conditions, including superficial clots and inflammation, so it is not a stand-alone answer.
When to consider evaluating for broader causes
Not everyone needs a “full clotting workup,” but clinicians may consider additional evaluation when:
- The clot appears unprovoked (no clear trigger like varicose veins, travel, or a procedure)
- There are recurrent episodes
- The patient is young for a first clot, especially without risk factors
- There is a strong family history
- The clot occurs in unusual sites or alongside autoimmune symptoms
This evaluation might include targeted testing for inherited clotting risks or antiphospholipid syndrome, as well as age-appropriate cancer screening if there is no obvious explanation.
Follow-up imaging
If you are not placed on anticoagulation, clinicians may recommend a repeat ultrasound—often within about 7–10 days—to ensure the clot is not extending. If you are treated with anticoagulation, follow-up imaging is more individualized and often guided by symptom course rather than routine “proof of clot disappearance,” since residual clot can linger even after risk has passed.
Which treatments work best?
Treatment depends on risk level. The most important factors are: whether a deep clot is present, how close the clot is to the deep junction, how long the clot is, and whether you have strong clotting risk factors (like active cancer).
Supportive care for lower-risk cases
For smaller clots that are clearly away from the deep junction and in people without major risk factors, clinicians may recommend a symptom-first approach:
- Walking and gentle activity (avoid prolonged bed rest)
- Leg elevation when resting
- Warm or cool compresses (choose what feels best)
- Anti-inflammatory pain relief (topical or oral NSAIDs if safe for you)
- Compression stockings if comfortable and appropriate for your circulation
Supportive care works best when paired with a clear plan for follow-up—especially if symptoms worsen or if the clot is near the thigh.
Anticoagulation (blood thinners): when it’s recommended
Anticoagulation aims to prevent extension into deeper veins and reduce the risk of pulmonary embolism. It is commonly used when:
- The clot is longer or involves a substantial segment of the great saphenous vein
- The clot sits near the deep junction (higher-risk anatomy)
- You have strong risk factors (active cancer, prior DVT/PE, major recent surgery, pregnancy/postpartum)
- Ultrasound shows progression or a deep clot at the same time
In many standard-risk cases of superficial vein thrombosis in the legs, clinicians use a prophylactic-dose anticoagulant for about 45 days. Common options include:
- Fondaparinux 2.5 mg once daily (injection)
- A low-molecular-weight heparin option (injection)
- In selected patients, a direct oral anticoagulant regimen may be used based on local practice and patient factors
If the clot is extremely close to the deep system or deep clot is present, clinicians may treat it more like a DVT, often using therapeutic-dose anticoagulation and a longer duration (commonly around 3 months), individualized to the situation.
What to expect once treatment starts
- Pain and redness usually improve within several days to two weeks.
- The firm cord can persist longer even when the risk has dropped; this does not automatically mean treatment failed.
- If you start anticoagulation, your clinician will review bleeding precautions and medication interactions.
When procedures are part of care
Surgery is not the first-line treatment for most acute cases, but procedures can matter in the bigger plan:
- If varicose veins drive recurrent episodes, vein treatment (ablation, phlebectomy, or other approaches) may reduce future risk after the acute phase settles.
- If symptoms persist or episodes recur, a vascular specialist may discuss longer-term strategies to address reflux and vein anatomy.
Medication safety notes
- Avoid combining multiple NSAIDs (for example, ibuprofen plus naproxen).
- If on anticoagulation, ask before using aspirin, NSAIDs, herbal supplements, or alcohol in higher amounts, since bleeding risk can rise.
- Tell your clinician about kidney disease, liver disease, prior ulcers, heavy periods, or recent bleeding—these can change the safest medication choice.
Recovery, prevention, and when to seek care
Recovery is usually steady, but good management is more than “wait it out.” The aim is to protect you during the higher-risk window, reduce symptoms, and prevent recurrence.
A practical recovery plan
Most people do well with a few consistent habits:
- Move every hour while awake. A 3–5 minute walk around the house or workplace is often enough to keep blood moving.
- Elevate the leg above heart level when resting, especially in the first week.
- Use compression thoughtfully. If you tolerate stockings, aim for daytime use and remove them at night. If stockings worsen pain or cause numbness, stop and ask for guidance.
- Hydrate consistently. Dehydration can worsen blood viscosity and leg symptoms, especially during travel.
- Track your symptoms. A simple daily note—pain (0–10), swelling, redness area, walking tolerance—helps you notice improvement or early warning signs.
Preventing future episodes
Prevention depends on your “why,” but these strategies commonly help:
- Address varicose veins and reflux if they are significant contributors, particularly with recurrent SVT.
- Plan for travel and immobilization. For flights or car rides over 4 hours:
- Stand and walk every 60–90 minutes when possible.
- Do ankle pumps and calf squeezes while seated.
- Wear compression stockings if recommended.
- Review hormones. If estrogen-containing therapy likely contributed, ask about non-estrogen alternatives.
- Manage weight and strength. Even modest weight reduction and calf-strength work (like heel raises) can improve venous return over time.
- Know your personal risk periods. Surgery, postpartum weeks, cancer treatment, and severe illness are times when your clinician may recommend extra prevention steps.
Follow-up you should not skip
- If you were not treated with anticoagulation, follow the plan for repeat ultrasound or re-evaluation if symptoms expand.
- If you were treated, schedule follow-up to review:
- Whether symptoms fit the expected timeline
- Bleeding or bruising concerns
- Whether ongoing risks require a longer plan (especially with cancer or recurrent SVT)
When to seek urgent care
Seek same-day evaluation (urgent care or emergency care depending on severity) for:
- New or worsening shortness of breath
- Chest pain with breathing, fainting, or coughing blood
- Rapidly increasing leg swelling, especially whole-leg swelling
- Severe pain with skin color change, numbness, or a cold foot
- Fever with spreading redness or drainage (possible infection)
The outlook
Most people recover fully, particularly when the clot is found early and managed based on location and risk factors. Recurrence is possible, especially with untreated varicose veins or ongoing systemic risks. The most effective long-term approach is a combination of:
- targeted anticoagulation when appropriate,
- symptom control that keeps you mobile,
- and addressing the underlying drivers (vein disease, hormones, or systemic clot risks).
References
- Treatment of Superficial Vein Thrombosis: Recent Advances, Unmet Needs and Future Directions 2024 (Review)
- Superficial Thrombophlebitis, Superficial Vein Thrombosis 2023 (Guideline)
- Editor’s Choice – European Society for Vascular Surgery (ESVS) 2021 Clinical Practice Guidelines on the Management of Venous Thrombosis 2021 (Guideline)
- Management and outcomes of superficial vein thrombosis: a single-center retrospective study 2023 (Observational Study)
- A systematic review and meta-analysis for the association between duration of anticoagulation therapy and the risk of venous thromboembolism in patients with lower limb superficial venous thrombosis 2024 (Systematic Review)
Disclaimer
This article is for educational purposes only and does not replace personalized medical care. Great saphenous vein thrombosis can range from low-risk to urgent depending on clot location, extension, and personal risk factors. If you have new leg swelling, chest pain, shortness of breath, fainting, or rapidly worsening symptoms, seek emergency care. Always talk with a licensed clinician before starting, stopping, or changing any medication—especially anticoagulants, anti-inflammatory drugs, or hormone therapy.
If you found this article helpful, please consider sharing it on Facebook, X (formerly Twitter), or any platform you prefer, and follow us on social media. Your support through sharing helps our team keep producing high-quality health content.