A jugular vein aneurysm is an uncommon bulge or widening in one of the large neck veins that return blood to the heart. Many people first notice it as a soft lump that becomes more obvious when coughing, straining, or holding a breath—then shrinks again at rest. That “comes and goes” pattern can be unsettling, but many jugular vein aneurysms are slow-growing and benign. The challenge is that a neck mass has a long list of possible causes, and a vein aneurysm can occasionally form a clot or press on nearby structures. Knowing what is typical—and what is not—helps you seek the right evaluation without delay. This article explains how jugular vein aneurysms form, who is most at risk, what symptoms matter, how doctors confirm the diagnosis, and what treatment and long-term management usually look like.
Table of Contents
- What is a jugular vein aneurysm?
- What causes it and who is at risk?
- Symptoms you may notice and possible complications
- How doctors confirm the diagnosis
- Treatment options and what to expect
- Living with it: monitoring, prevention, when to seek care
What is a jugular vein aneurysm?
A jugular vein aneurysm is an abnormal enlargement of a jugular vein in the neck. Doctors most often describe it in one of two ways:
- True venous aneurysm: the vein wall itself is stretched and enlarged.
- Pseudoaneurysm: a wall injury creates an outpouching that is not made of normal vein layers.
You may also hear phlebectasia, a term commonly used for a smooth, elongated widening—especially in children—rather than a rounded “saccular” bulge. In real life, the labels can overlap, and the important questions are practical ones: Which vein is involved, how big is it, is it changing, and is there clot inside?
Which jugular vein is involved?
There are three main jugular veins:
- Internal jugular vein (IJV): the deepest and largest; runs alongside the carotid artery.
- External jugular vein (EJV): closer to the skin; often easier to see when it enlarges.
- Anterior jugular vein: smaller; less commonly discussed, but it can also dilate.
An aneurysm can be saccular (a pouch on one side) or fusiform (the vein is widened in a more even, spindle-like way). This shape matters because it affects flow patterns and may influence clot risk and surgical planning.
Why it looks “dynamic”
A classic clue is that the swelling enlarges with actions that raise pressure in the chest and neck veins—coughing, straining, singing forcefully, or performing a Valsalva maneuver (bearing down). When pressure falls again, the bulge may soften or nearly disappear. That behavior helps distinguish it from many solid lumps, but it is not a diagnosis by itself.
Is it dangerous?
Many jugular vein aneurysms are stable and cause no medical harm. Still, “usually benign” is not the same as “always harmless.” Rarely, complications such as clot formation, pain, compression symptoms, or cosmetic distress lead to treatment. The safest approach is to confirm the diagnosis with appropriate imaging and then tailor follow-up to the individual risk profile.
What causes it and who is at risk?
Jugular vein aneurysms are rare, so there is no single “typical patient.” Instead, clinicians think in categories: congenital (present from development), acquired (developed later), and pressure-related (driven by flow and strain on the vein).
Congenital or developmental factors
In children, internal jugular phlebectasia is often considered a developmental condition. The vein wall may be more elastic or less supported by surrounding tissues, making it easier to balloon outward during coughing or crying. Many pediatric cases are right-sided, and many remain stable over time.
Certain inherited connective tissue patterns may also increase vein wall stretchiness. Most people with a jugular vein aneurysm do not have a known genetic syndrome, but clinicians still ask about:
- Easy bruising or unusually stretchy skin
- History of arterial aneurysms in the family
- Multiple hernias or very early varicose veins
This is less about labeling and more about choosing appropriate screening and follow-up.
Acquired causes in adults
In adults, the list broadens. A jugular vein aneurysm can develop after:
- Trauma to the neck (including blunt impact)
- Central venous catheterization or repeated venous access on that side
- Prior neck surgery or radiation that alters tissue support
- Local inflammation or infection affecting the vein wall (uncommon)
- Venous outflow obstruction downstream, which raises pressure upstream
Sometimes the trigger is not a single event but repeated strain over years—think chronic cough, heavy lifting, or occupations with frequent breath-holding. These factors do not “cause” an aneurysm in everyone, but they can make a vulnerable vein enlarge.
Risk factors that shape management
Even more than “why it formed,” doctors focus on what raises the chance of complications:
- Aneurysm contains clot (thrombus) or has sluggish flow patterns
- Rapid growth over months rather than years
- Significant symptoms: pain, tenderness, swallowing discomfort, voice changes
- A history of blood clots, clotting disorders, or cancer
- Planned major surgery, pregnancy, or long travel where clot risk changes
A helpful way to think about risk is “structure + situation.” The structure is the aneurysm’s size, shape, and presence of clot. The situation is your overall clot risk and whether the aneurysm is exposed to repeated pressure spikes or injury. Treatment choices are usually built around both.
Symptoms you may notice and possible complications
Most people discover a jugular vein aneurysm because of appearance, not pain. The most common presentation is a soft, compressible neck swelling that enlarges with straining and becomes less visible at rest.
Common symptoms and signs
You may notice:
- A lump on one side of the neck that comes and goes
- Enlargement during coughing, laughing, singing, or exercise
- A “bag of worms” or balloon-like feeling under the skin
- Mild ache, pressure, or tenderness—especially if the area is bumped
- Cosmetic concern, especially if the swelling is prominent in photos or during speech
Some people feel a vague fullness when turning the head or wearing tight collars. Many have no symptoms at all beyond the visible swelling.
Less common symptoms that deserve attention
Although uncommon, symptoms can suggest pressure on nearby structures or an evolving complication:
- Trouble swallowing, a choking sensation, or frequent throat clearing
- Hoarseness or voice fatigue
- New headaches or facial swelling (possible venous outflow issues)
- Persistent, localized pain—especially if the mass feels firmer than usual
These symptoms do not automatically mean danger, but they do raise the urgency for evaluation.
Potential complications
Serious complications are rare, but they guide decision-making:
- Thrombosis (clot within the aneurysm): may cause new firmness, pain, or persistent swelling that no longer “deflates” as usual.
- Pulmonary embolism: very uncommon in jugular aneurysms, but theoretically possible if a clot forms and migrates.
- Compression effects: nearby nerves and airway structures sit in a tight neighborhood, especially around the internal jugular vein.
- Bleeding or rupture: extremely rare for low-pressure neck veins, but the risk may rise with trauma or if the aneurysm wall is abnormal.
What else can mimic it?
A dynamic neck mass has a wide differential diagnosis. Conditions that can look similar include:
- Laryngocele (air-filled pouch connected to the voice box)
- Enlarged lymph nodes or cysts that are not truly dynamic
- Vascular malformations or arteriovenous connections
- Thyroid-related masses (often lower in the neck and not compressible)
Because the neck contains vital structures, the safest assumption is: if it is new, changing, painful, firm, or associated with breathing/swallowing symptoms, it needs timely medical assessment.
How doctors confirm the diagnosis
Diagnosis usually combines a careful history, a focused exam, and imaging that demonstrates venous flow. The goal is to confirm that the mass is venous, identify which vein is involved, and assess features that affect risk (especially clot and outflow obstruction).
History and exam clues
Clinicians often ask:
- When was it first noticed, and has it changed recently?
- Does it enlarge with coughing, straining, or breath-holding?
- Any recent trauma, catheter placement, or neck procedures?
- Any symptoms of clotting (new pain, firmness) or infection (fever, redness)?
- Any personal history of blood clots, cancer, or clotting disorders?
On exam, a venous aneurysm is typically soft, nonpulsatile, and compressible. The clinician may observe it during gentle maneuvers that increase venous pressure—done carefully, not forcefully.
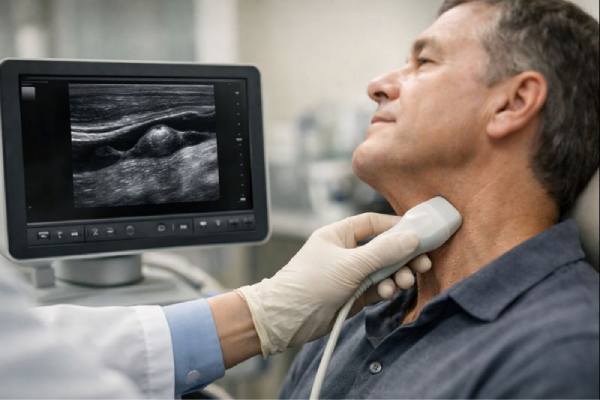
First-line test: duplex ultrasound
Duplex ultrasound with color Doppler is usually the first test because it can:
- Confirm venous blood flow within the mass
- Show the aneurysm’s size and shape
- Detect internal clot or sluggish “swirling” flow
- Assess nearby veins for obstruction or narrowing
Ultrasound can often be performed while you perform a light Valsalva maneuver, which helps demonstrate the dynamic enlargement.
When CT or MRI is useful
If ultrasound is inconclusive—or if the aneurysm is deep, large, or close to important structures—clinicians may use:
- CT venography: detailed anatomy and surrounding structures; helpful for surgical planning.
- MR venography: strong soft-tissue detail without ionizing radiation; often preferred when repeated imaging is expected.
These studies also help rule out alternative diagnoses and identify venous outflow problems, such as compression or narrowing downstream.
Key details doctors document
A thorough report usually describes:
- Which jugular vein is affected (internal vs external)
- Saccular vs fusiform shape
- Maximum diameter at rest and with strain
- Presence or absence of thrombus
- Evidence of venous obstruction or collateral veins
- Relationship to nearby arteries, nerves, and airway structures
If the diagnosis is confirmed and the aneurysm is uncomplicated, many patients move into a monitoring plan rather than immediate intervention. If there is clot, rapid change, or significant symptoms, referral to vascular surgery (and sometimes ENT or radiology) is common.
Treatment options and what to expect
Treatment depends less on the name of the condition and more on risk and goals: safety, symptom relief, and cosmetic preference. Because jugular vein aneurysms are rare, there is no single universal protocol, but most care follows a practical decision pathway.
Observation and follow-up
For an asymptomatic, nonthrombosed jugular vein aneurysm, watchful waiting is often reasonable. A typical monitoring plan may include:
- Baseline duplex ultrasound to document size and flow.
- Repeat ultrasound in about 6–12 months to confirm stability.
- Longer intervals if stable, with earlier recheck if symptoms change.
Observation is most appropriate when the aneurysm is soft, stable, and not causing pain or functional problems. Many people choose this route once they understand the condition and have clear “return precautions.”
When surgery is considered
Surgery is more likely when there is:
- Persistent pain or tenderness
- Thrombosis or suspected embolic risk
- Rapid growth or concerning imaging features
- Compression symptoms (swallowing, voice, airway discomfort)
- Significant cosmetic distress affecting quality of life
The approach depends on the vein and anatomy. Common open surgical strategies include excision of the aneurysm with:
- Ligation (tying off the vein) in selected cases, more often for external jugular lesions
- Reconstruction or repair to preserve venous flow, especially for internal jugular involvement when anatomy or patient factors make preservation preferable
For internal jugular aneurysms, surgeons may favor techniques that maintain patency when feasible, particularly on the dominant drainage side or in patients with limited venous alternatives.
Anticoagulation and clot management
If imaging shows thrombosis, clinicians evaluate the broader clot risk picture: symptoms, clot extent, prior clot history, and any downstream obstruction. Anticoagulation decisions are individualized. In some cases, clot plus symptoms pushes management toward surgery; in others, careful anticoagulation and follow-up imaging may be chosen first.
Endovascular options
Minimally invasive or endovascular treatments have been reported in select venous aneurysms, but for jugular vein aneurysms they are less common than open approaches. They may be considered when anatomy is favorable, surgical risk is high, or the lesion is difficult to access—usually after multidisciplinary review.
What recovery typically involves
After surgery, patients generally have:
- Short-term activity limits to reduce neck strain
- Wound care and monitoring for swelling or infection
- Follow-up imaging if reconstruction was performed or if clot risk was part of the concern
Most outcomes are good when the condition is properly characterized and the plan matches the patient’s risk profile and goals.
Living with it: monitoring, prevention, when to seek care
If you are living with a jugular vein aneurysm, the main tasks are straightforward: keep follow-up consistent, reduce preventable risk, and respond quickly to meaningful changes.
Monitoring that is actually useful
Monitoring works best when it is measurable. Consider keeping a simple log:
- Date you notice visible change (photos can help, taken at similar angles)
- New symptoms: pain, firmness, swallowing or voice changes
- Triggers that worsen it (heavy lifting, coughing spells)
- Results of imaging and the plan for next follow-up
If your clinician recommends ultrasound surveillance, try to use the same facility when possible so measurements are comparable.
Risk reduction in daily life
There is no proven lifestyle “cure,” but you can reduce avoidable strain and clot risk:
- Treat chronic cough, uncontrolled asthma, or reflux that drives frequent coughing.
- Avoid repeated heavy breath-holding during lifting; exhale through effort instead.
- Stay well-hydrated during long travel and take walking breaks to reduce overall clot risk.
- Discuss estrogen-containing contraception or hormone therapy with your clinician if you have other clot risks.
- Protect the area from direct trauma if the aneurysm is superficial and prominent.
If you have a known clotting disorder or a strong personal history of clots, ask directly how that changes your monitoring plan.
Prognosis
Many jugular vein aneurysms remain stable for years and never cause serious problems. When intervention is needed, it is often for symptoms or cosmetic impact rather than emergency risk. Prognosis is generally favorable when clot is absent and imaging confirms uncomplicated anatomy.
When to seek urgent evaluation
Seek prompt medical care if you develop:
- Sudden swelling that does not reduce at rest
- New firmness, redness, warmth, or escalating pain over the mass
- Shortness of breath, chest pain, coughing blood, or fainting
- New neurologic symptoms (severe headache, one-sided weakness)
- Trouble breathing, stridor, or rapidly worsening swallowing difficulty
Even if these turn out not to be related, they warrant urgent assessment.
How to prepare for appointments
Bring:
- A timeline of when it started and how it changed
- Any photos showing enlargement with strain (if safe and comfortable)
- A list of prior procedures (central lines, neck surgery, trauma)
- Your clot risk history (prior DVT/PE, miscarriages, family history)
That information helps your clinician decide whether observation is enough or whether further imaging, specialist referral, or treatment is the safer next step.
References
- Comprehensive review with pooled analysis on external and internal jugular vein aneurysm 2021 (Systematic Review)
- Management of external jugular vein aneurysm: a systematic review 2022 (Systematic Review)
- Internal jugular vein phlebectasia: A systematic review of therapeutic approaches in Pediatrics 2023 (Systematic Review)
- Surgical management of venous aneurysms 2021 (Clinical Study)
- Superficial venous aneurysms: a case-based review 2025 (Review)
Disclaimer
This article is for general educational purposes and does not provide medical advice, diagnosis, or treatment. A neck mass—especially one that is new, enlarging, painful, firm, or associated with breathing, swallowing, voice changes, fever, or chest symptoms—should be assessed by a qualified clinician. If you develop sudden persistent neck swelling, signs of infection, or symptoms that could suggest a blood clot or pulmonary embolism, seek urgent medical care.
If you found this guide useful, please share it on Facebook, X (formerly Twitter), or any platform you prefer, and follow us on social media. Your support through sharing helps our team continue producing careful, practical health content.