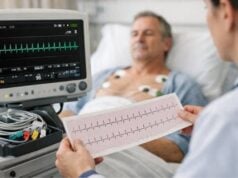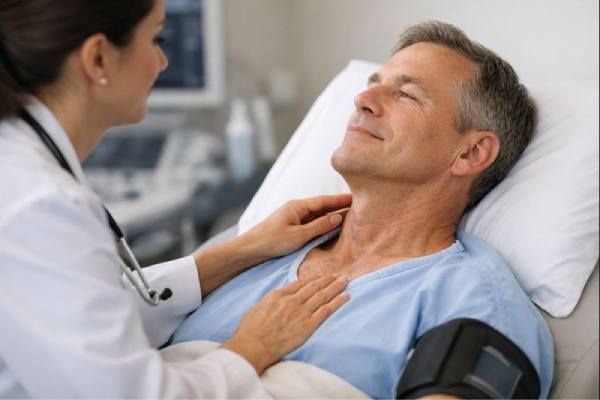
Jugular vein distention (JVD) means the neck veins look unusually full or raised. It is not a disease by itself—it is a visible clue that pressure is higher than it should be in the veins returning blood to the heart. Sometimes JVD is noticed by a clinician during an exam; other times a person spots it in the mirror when they are short of breath or lying back. The most important point is context: in a stable person, JVD can help confirm fluid overload or heart strain; in a suddenly ill person, it can signal a time-sensitive emergency. This guide explains what JVD reflects inside the body, the most common causes, what symptoms tend to travel with it, how clinicians confirm what’s going on, and what treatment and day-to-day management usually focus on.
Table of Contents
- What JVD means inside the body
- Common causes and who is at risk
- Symptoms that often come with JVD
- How clinicians check and confirm the cause
- Treatment: what improves JVD
- Long-term management and when to seek urgent care
What JVD means inside the body
Jugular vein distention is best understood as a “pressure gauge” you can sometimes see. The jugular veins—especially the internal jugular vein—carry blood from the head and neck back toward the right side of the heart. When pressure rises in the right atrium or in the large veins feeding it, that pressure can travel backward and make the neck veins look fuller.
Clinicians often talk about the jugular venous pulse (JVP), which is the subtle up-and-down movement of venous blood that mirrors events in the right side of the heart. In many people, the JVP is not easy to see. But when venous pressure is elevated, the column of blood rises higher in the neck and becomes more visible. That’s the practical reason JVD matters: it can hint at “too much volume,” “too much back-pressure,” or “blocked flow” on the way to the heart.
Why position matters
JVD is not judged while someone is sitting bolt upright or lying completely flat. The classic exam position is reclining with the head and chest elevated roughly 30–45 degrees. In that angle range, the veins are not artificially collapsed by gravity, and they are not artificially overfilled by being flat. Lighting, neck anatomy, and hydration can all change what is visible, which is why a single glance is rarely definitive.
JVD vs “prominent neck veins”
Not every visible neck vein is abnormal. Thin individuals can have visible veins that are normal. Anxiety, pain, or short-term breath-holding can also make veins stand out briefly. True JVD is more about a sustained, position-dependent rise in venous pressure, often accompanied by other signs of congestion.
What elevated venous pressure usually reflects
JVD most often points to one of these internal situations:
- The heart’s right side is struggling to accept or pump blood forward.
- Pressure is backing up from the lungs into the right heart.
- Fluid volume is higher than the circulation can handle.
- There is obstruction to venous return (less common, but important).
Because JVD is a sign, not a diagnosis, the next step is always the same: look for the “why” in symptoms, exam findings, and targeted testing.
Common causes and who is at risk
The causes of jugular vein distention cluster into a few major categories. Thinking in categories helps you understand why clinicians ask the questions they do and why certain tests come early.
1) Heart failure and fluid overload
A very common cause is heart failure, especially when the right side of the heart is under strain or when long-standing left-sided failure has led to backup pressure through the lungs. JVD can also appear with kidney failure, liver disease with significant fluid retention, or high salt intake combined with reduced ability to excrete fluid. In these situations, JVD is often part of a larger picture that includes swelling in the legs, weight gain from fluid, and shortness of breath.
2) Lung-related pressure overload
Conditions that raise pressure in the pulmonary arteries can overload the right ventricle and raise right-sided pressures. Pulmonary hypertension can be primary, but it also develops secondary to lung disease (such as COPD), sleep apnea, chronic blood clots in the lungs, or left-heart disease. Over time, the right heart may enlarge and weaken, and JVD becomes one of the visible clues.
3) Valve and rhythm problems
Tricuspid regurgitation (a leaky valve between the right atrium and right ventricle) can produce prominent neck vein pulsations and JVD. Some rhythm issues can also contribute to venous congestion by reducing effective forward flow or altering filling.
4) Obstructive emergencies
Some causes require urgent action because they block normal filling of the heart or impede venous return:
- Cardiac tamponade (fluid under pressure around the heart)
- Tension pneumothorax (air under pressure compressing lung and major veins)
- Massive pulmonary embolism (large clot burden raising right-heart pressure)
In these cases, JVD may appear alongside low blood pressure, severe breathlessness, or sudden collapse.
5) Venous flow obstruction
Less commonly, a blockage in major veins (such as superior vena cava obstruction) can cause neck and facial swelling and distended neck veins. Cancer, clot related to indwelling catheters, or scarring can be contributors.
Who is more likely to develop JVD?
Risk rises in people with heart failure, pulmonary hypertension, chronic lung disease, sleep apnea, chronic kidney disease, significant valve disease, a history of blood clots, active cancer, or long-term central venous access. Risk also increases during episodes of acute illness that change fluid balance, oxygen levels, or clot risk.
Symptoms that often come with JVD
JVD itself usually does not hurt. People rarely “feel” elevated venous pressure in the neck. What they notice instead are symptoms from the underlying problem, plus the visual change in the neck veins. That’s why it helps to focus on the full pattern rather than the vein appearance alone.
Common symptoms when JVD is due to congestion
When JVD is part of fluid overload or heart failure, symptoms often include:
- Shortness of breath with activity, and sometimes at rest
- Needing extra pillows to sleep comfortably or waking up gasping
- Rapid weight gain over days from fluid retention
- Swollen ankles or legs, or swelling that worsens by evening
- Fatigue, reduced exercise tolerance, and a “heavy” feeling in the body
- Abdominal fullness, reduced appetite, or nausea from liver congestion
People may also notice a persistent cough, wheezing, or decreased urination when fluid is building up.
Symptoms that suggest lung-pressure strain
When right-heart strain is driven by lung disease or pulmonary hypertension, symptoms can center on breathing and circulation:
- Breathlessness out of proportion to activity
- Lightheadedness or fainting with exertion (a higher-risk sign)
- Chest tightness or pressure
- Bluish lips or fingertips in advanced disease
- Swelling and abdominal bloating as right-heart failure progresses
Clues that point toward urgent causes
JVD becomes more concerning when it appears with sudden, severe symptoms, especially if the person is deteriorating quickly. Warning patterns include:
- Sudden severe shortness of breath, chest pain, or collapse
- Very low blood pressure, confusion, or clammy skin
- One-sided absent breath sounds or severe chest trauma symptoms
- Rapidly worsening breathing difficulty after a procedure or mechanical ventilation
- Sharp chest pain and breathlessness with risk factors for blood clots
These patterns raise concern for obstructive emergencies like tension pneumothorax, cardiac tamponade, or massive pulmonary embolism.
Complications are about the cause
JVD can be a marker that the body is under hemodynamic stress. The potential complications depend on what is driving the pressure:
- Worsening heart failure with fluid in the lungs and low oxygen
- Kidney injury from poor perfusion and congestion
- Liver congestion and fluid in the abdomen (ascites) in advanced right-heart failure
- Dangerous low blood pressure and organ hypoperfusion in obstructive shock
- Arrhythmias that further destabilize circulation
The practical takeaway is simple: JVD is most meaningful when you pair it with symptoms, speed of onset, and overall stability.
How clinicians check and confirm the cause
Clinicians do not diagnose “jugular vein distention” and stop. They use it as a sign to estimate venous pressure and to narrow down causes. Confirmation usually involves a structured exam plus tests that match the suspected category (heart, lungs, fluid balance, or venous obstruction).
Bedside exam: looking for a pattern
A careful exam often includes:
- Positioning the person at an angle and identifying the highest point of venous pulsation
- Listening to the heart and lungs for signs of fluid overload or valve disease
- Checking for leg swelling, abdominal swelling, and liver tenderness
- Measuring blood pressure, heart rate, oxygen level, and breathing effort
Clinicians may also use the abdominojugular reflux test (sometimes called hepatojugular reflux). Gentle pressure on the abdomen briefly increases venous return; if the neck veins remain elevated rather than settling, it supports the idea of limited right-heart reserve or congestion.
Point-of-care ultrasound is increasingly important
Because neck anatomy and lighting can make visual JVP estimates challenging, many settings now use bedside ultrasound to assess venous congestion. Ultrasound can help clinicians:
- Identify the internal jugular vein and observe distention more precisely
- Compare findings with other congestion markers (for example, ultrasound findings in the lungs or inferior vena cava)
- Track changes after treatment (such as after diuretics)
Ultrasound does not replace clinical judgment, but it can improve confidence when the exam is difficult.
Tests commonly used to find the cause
Depending on the situation, clinicians may order:
- ECG to look for rhythm problems or strain patterns
- Chest imaging to evaluate fluid in the lungs, enlarged heart silhouette, or lung pathology
- Echocardiogram to assess heart pumping, valve function, and pericardial fluid
- Blood tests for kidney function, liver congestion markers, anemia, and electrolytes
- Natriuretic peptides in suspected heart failure
- Tests for clot evaluation when pulmonary embolism is suspected (chosen based on risk assessment)
- CT or venography when major venous obstruction is a concern
In complex cases—especially pulmonary hypertension—right heart catheterization may be used to measure pressures directly and guide therapy.
Why self-diagnosis is risky
People sometimes try to check for JVD at home. The problem is that neck vein visibility is variable, and serious conditions can be missed or misinterpreted. If you notice new neck vein distention along with breathlessness, chest symptoms, fainting, leg swelling, or rapid decline, the safer move is medical evaluation rather than repeated mirror checks.
Treatment: what improves JVD
There is no single treatment for JVD because JVD is a sign of elevated venous pressure, not the root problem. Treatment works when it lowers the pressure that is distending the jugular veins—either by reducing excess fluid, improving heart function, relieving obstruction, or urgently reversing an obstructive emergency.
If heart failure or fluid overload is the cause
Treatment often includes:
- Diuretics to remove excess fluid and reduce venous congestion
- Adjusting long-term heart failure medications that support heart function and remodeling
- Managing triggers such as infection, uncontrolled blood pressure, anemia, thyroid disease, or medication-related fluid retention
In acute decompensation, clinicians may use intravenous diuretics, oxygen support, and close monitoring. When the underlying circulation improves, JVD typically decreases along with leg swelling and breathing symptoms.
If pulmonary hypertension or lung disease is driving right-heart strain
The priority is treating the cause of elevated lung pressures. That may involve:
- Targeted pulmonary hypertension therapies in appropriate patients
- Optimizing oxygen levels and treating underlying lung disease
- Addressing sleep apnea with effective therapy
- Managing fluid carefully to reduce right-heart workload
Because these conditions can be complex, care often involves specialist follow-up and structured monitoring.
If a valve problem is central
For tricuspid regurgitation or other significant valve disease, treatment may include diuretics for symptom control and, in selected cases, interventional or surgical repair. The aim is to reduce backward flow and improve forward circulation.
If the cause is an emergency obstruction
Some causes of JVD require immediate action:
- Cardiac tamponade is treated by urgent drainage of the pericardial space.
- Tension pneumothorax is treated with immediate decompression to relieve pressure and restore venous return.
- Massive pulmonary embolism is treated with rapid stabilization and clot-directed therapy when indicated.
In these situations, JVD is not the target—it is one of the signs that helps clinicians recognize obstructive shock and act quickly.
If venous return is physically blocked
When superior vena cava obstruction or major venous thrombosis is suspected, treatment depends on cause and may include anticoagulation, stenting, cancer-directed therapy, or catheter management.
A useful way to think about treatment is: JVD improves when right-sided filling pressures fall. The correct strategy depends on why those pressures rose in the first place.
Long-term management and when to seek urgent care
Long-term management is about preventing the underlying condition from flaring and having a clear plan for changes. For many people, JVD enters the conversation after a diagnosis like heart failure or pulmonary hypertension is already established. In that setting, JVD becomes a monitoring clue alongside symptoms, weight, swelling, exercise tolerance, and vital signs.
Daily and weekly habits that reduce congestion risk
Depending on the diagnosis, clinicians commonly recommend:
- Taking medications consistently and refilling early to avoid missed doses
- Tracking symptoms and functional capacity (for example, what activities trigger breathlessness)
- Monitoring weight trends when fluid retention is a known issue
- Following a heart-healthy eating pattern and moderating sodium intake when advised
- Limiting alcohol and avoiding tobacco
- Keeping vaccinations current to reduce infection-related decompensation
- Treating sleep apnea and controlling blood pressure and diabetes when present
Some medications can worsen fluid retention or strain kidney function in susceptible people. Nonsteroidal anti-inflammatory drugs (NSAIDs) are a common example. It’s worth asking your clinician which over-the-counter drugs are safest for you.
What to do when symptoms change
If you have a condition associated with congestion, the most useful question is not “Are my neck veins bigger today?” It is “Is my breathing, swelling, weight, or stamina changing compared with my baseline?” A practical response plan often includes early contact with your care team when you notice:
- Worsening shortness of breath, especially at night
- Swelling that is spreading or becoming tight and painful
- A rapid upward weight trend over several days
- Reduced urine output with increasing swelling
- New palpitations, dizziness, or near-fainting
Early action can prevent hospitalization in many cases of fluid overload.
When to seek urgent or emergency care
Seek urgent medical care if JVD appears with, or you develop, any of the following:
- Sudden severe shortness of breath, chest pain, or collapse
- Fainting, seizure-like episodes, or severe lightheadedness
- Confusion, blue discoloration of lips, or very low oxygen readings
- Severe one-sided chest symptoms, especially after trauma or procedures
- Coughing blood, or symptoms suggestive of a blood clot
- Rapidly worsening swelling of the face and neck, especially with trouble breathing
These symptoms can indicate time-sensitive conditions where minutes matter.
Outlook depends on the cause
JVD caused by a reversible trigger—such as medication-related fluid retention or a treatable exacerbation—may resolve quickly with appropriate care. JVD linked to chronic heart or lung disease may come and go with disease control. The best long-term outcomes usually come from a clear diagnosis, consistent follow-up, and an action plan that treats early congestion before it becomes a crisis.
References
- 2022 AHA/ACC/HFSA Guideline for the Management of Heart Failure: A Report of the American College of Cardiology/American Heart Association Joint Committee on Clinical Practice Guidelines 2022 (Guideline)
- 2022 ESC/ERS Guidelines for the diagnosis and treatment of pulmonary hypertension 2022 (Guideline)
- Accuracy of Ultrasound Jugular Venous Pressure Height in Predicting Central Venous Congestion 2022 (Clinical Study)
- Tension Pneumothorax – StatPearls – NCBI Bookshelf 2025 (Clinical Review)
- Pericardial Tamponade in Trauma: A Systematic Review of Diagnosis, Emergency Management, and Surgical Outcomes 2025 (Systematic Review)
Disclaimer
This article is for general educational purposes and does not provide medical advice, diagnosis, or treatment. Jugular vein distention is a clinical sign that can be associated with serious heart, lung, and circulatory conditions. If you have new or worsening shortness of breath, chest pain, fainting, confusion, rapid swelling, or any sudden decline—especially with visibly distended neck veins—seek urgent medical evaluation. In an emergency (collapse, severe breathing difficulty, or suspected cardiac arrest), call emergency services immediately.
If you found this guide helpful, please share it on Facebook, X (formerly Twitter), or any platform you prefer, and follow us on social media. Your support through sharing helps our team continue producing reliable, practical health content.