Jugular vein thrombosis means a blood clot forms in one of the major neck veins that drain blood from the head back to the heart. It can happen for many reasons—from a recent IV line or device in the vein, to infection, to an underlying tendency for blood to clot. Some cases cause only localized neck pain and swelling. Others can become serious if the clot grows, becomes infected, or breaks off and travels to the lungs (pulmonary embolism, a clot that blocks lung blood flow).
Because the jugular veins sit close to the airway, nerves, and major arteries, symptoms can be confusing and easy to dismiss. The good news is that modern imaging can usually confirm the diagnosis quickly, and treatment often prevents complications. This guide explains what to watch for, how doctors confirm it, and what treatment and day-to-day management typically look like.
Table of Contents
- What it is and why it matters
- What causes jugular vein thrombosis?
- Risk factors and who gets it
- Symptoms, red flags, and complications
- How doctors diagnose it
- Treatment options and what to expect
- Management, prevention, and when to seek care
What it is and why it matters
The jugular veins are the main “drainage pipes” for blood leaving the brain, face, and neck. Most people have an internal jugular vein (deep, alongside the carotid artery) and an external jugular vein (more superficial, often visible in the neck). A thrombosis is a clot that forms inside a blood vessel. When it occurs in a jugular vein, it can block or slow blood flow and irritate the vessel wall, causing pain and swelling.
Jugular vein thrombosis is often discussed in two broad patterns:
- Device-related thrombosis: A central venous catheter, dialysis catheter, PICC, or other line can injure the lining of the vein and disturb flow, which encourages clot formation.
- Non-device-related thrombosis: The clot forms due to infection (including septic thrombophlebitis such as Lemierre syndrome), cancer, recent surgery/trauma, inflammatory disease, or inherited/acquired clotting tendencies.
Why it matters comes down to location and consequences:
- Neck anatomy is crowded. Swelling or inflammation around the vein can irritate nearby nerves and tissues, and pain may radiate to the jaw, ear, or shoulder.
- Clots can extend. A clot in the internal jugular vein can grow into the subclavian/brachiocephalic veins or (less commonly) toward venous sinuses in the head, depending on the underlying cause and anatomy.
- Pulmonary embolism is possible. Not every jugular clot leads to a lung clot, but the risk is real—especially when the thrombosis is part of a larger “upper-body DVT” pattern.
- Infection changes the urgency. If bacteria seed the clot, the problem is no longer only “blocked flow.” An infected clot can send septic emboli to the lungs or elsewhere, and it requires antibiotics and source control in addition to clot treatment.
A practical way to think about it: jugular vein thrombosis is not one single disease—it’s a final pathway that can result from very different triggers. Treatment and follow-up depend heavily on why it happened and whether infection or cancer is involved.
What causes jugular vein thrombosis?
A clot forms when the balance between blood flow, vessel lining health, and clotting tendency shifts in the wrong direction. Clinicians often organize the causes into three “buckets” (sometimes called Virchow’s triad): slowed flow, vessel injury, and increased clotting tendency. Jugular thrombosis usually involves more than one.
Common causes include:
1) Catheters and implanted devices
Anything placed in or near the vein can irritate the vessel lining and disrupt flow. Examples include:
- Central venous catheters (short-term or long-term)
- Dialysis catheters
- PICC or midline lines that end near the large chest/neck veins
- Pacemaker/defibrillator leads (more often in chest veins but can affect upstream flow)
2) Infection and inflammation
Infection can inflame the vessel wall and make blood “stickier.” A classic example is Lemierre syndrome, where a throat or oral infection leads to septic thrombophlebitis of the internal jugular vein. Other scenarios include:
- Deep neck infections or abscesses
- Dental infections with spread into neck spaces
- Severe skin/soft-tissue infection near the vein
- Systemic infections that increase clotting risk
3) Cancer and cancer treatments
Cancer can raise clot risk through tumor-related inflammation, compression of veins, and changes in clotting proteins. Chemotherapy and indwelling catheters add additional risk. Even when a catheter is the immediate trigger, the “why now?” often includes an underlying pro-thrombotic state.
4) Mechanical compression or trauma
Pressure on the vein—either sudden (trauma) or ongoing (anatomy or mass effect)—can slow flow and damage the lining. Examples:
- Neck injury or surgery
- Tumors or enlarged lymph nodes compressing venous outflow
- Rare anatomical causes that chronically narrow venous pathways
5) Systemic clotting tendency
This can be inherited (certain thrombophilias) or acquired, such as:
- Pregnancy/postpartum period
- Estrogen-containing birth control or hormone therapy
- Autoimmune disorders that increase clotting risk
- Severe dehydration, prolonged immobility, or critical illness
A helpful rule of thumb: if jugular vein thrombosis occurs without an obvious catheter, recent infection, or trauma, clinicians usually widen the search for hidden triggers—especially cancer, systemic inflammatory disease, or a significant clotting tendency—because management and recurrence risk depend on the underlying cause.
Risk factors and who gets it
Jugular vein thrombosis is uncommon compared with leg DVT, but certain situations make it much more likely. Understanding risk factors is not about blame—it’s about anticipating complications, deciding how aggressive treatment should be, and preventing recurrence.
High-impact risk factors (most strongly linked in real-world practice)
- A central venous catheter or dialysis catheter in the neck or upper chest region
Risk rises with longer dwell time, larger catheter size relative to vein size, multiple placement attempts, and catheter infection. - Active cancer (especially with chemotherapy, surgery, or long-term venous access)
Cancer-associated clots behave differently: recurrence risk is higher, and treatment often needs to be longer. - Recent serious infection in the throat/neck region
Fever, worsening throat pain, neck tenderness, and respiratory symptoms raise concern for septic thrombophlebitis. - Recent hospitalization or critical illness
Immobility, inflammation, dehydration, and multiple IV devices can combine to raise risk.
Moderate risk factors (often contributing, especially in combination)
- Major surgery or trauma, including head/neck procedures
- Pregnancy or the 6–12 weeks after delivery
- Estrogen exposure (combined hormonal contraception or certain hormone therapies)
- Previous blood clots (leg DVT, PE, or earlier upper-body clots)
- Known thrombophilia (inherited clotting disorders) or strong family history of early clots
- Autoimmune/inflammatory conditions that increase clotting tendency
- Smoking, especially with other risk factors present
Who gets it? Patterns by scenario
- Hospitalized or device-bearing patients: Often older, with multiple comorbidities and a catheter trigger. Symptoms may be subtle because pain can be masked by other illness.
- Otherwise healthy adolescents/young adults: When jugular thrombosis appears with severe sore throat, fever, and neck pain, clinicians consider Lemierre syndrome or deep neck infection.
- People with cancer: Clots may occur near ports, PICCs, or central lines, and can be the first clue that a device is irritating the vein.
Why risk profiling matters
Two people can have the same ultrasound finding but need different plans. A short, provoked clot after a temporary catheter removal may need limited-duration anticoagulation and monitoring. A clot in someone with active cancer or recurrent clots may require longer therapy, closer follow-up, and careful decisions about keeping or removing the catheter.
Symptoms, red flags, and complications
Symptoms vary widely. Some people feel a localized neck ache; others develop systemic illness. It often helps to think in three layers: local symptoms, infection features, and clot-travel/extension features.
Local symptoms (from the clot and vein inflammation)
- Neck pain or tenderness, often on one side
- Swelling along the side of the neck or above the collarbone
- A firm, “cord-like” feeling (more typical with superficial veins)
- Pain that worsens when turning the head or swallowing
- Facial puffiness or fullness, especially in the morning (suggests impaired venous drainage)
- Headache or pressure sensation (can occur when drainage patterns change)
Symptoms that suggest infection (higher urgency)
- Fever or chills
- Recent or severe sore throat, dental pain, or ear pain
- Worsening fatigue, body aches, or a “toxic” feeling
- Redness or warmth over the neck (not always present)
- Cough, chest pain, or shortness of breath after a throat infection (can reflect septic emboli)
Symptoms that suggest extension or pulmonary embolism
- New shortness of breath, sharp chest pain, coughing blood, or unexplained rapid heart rate
- Arm swelling, heaviness, or bluish discoloration (suggesting extension into chest/arm veins)
- Dizziness, fainting, or low oxygen levels
Potential complications
- Pulmonary embolism (PE): A clot fragment travels to the lungs. This can range from mild to life-threatening.
- Post-thrombotic symptoms: Persistent discomfort, swelling, or heaviness in the neck/upper chest region due to scarring and altered flow.
- Septic emboli (in infected clots): In Lemierre-type illness, infected material can travel to the lungs, causing multiple small lung infections or abscesses.
- Clot progression: The clot can extend into larger central veins, making symptoms more extensive and treatment more complex.
- Bleeding from treatment: Anticoagulants reduce clot growth and recurrence but increase bleeding risk, especially in people with kidney disease, recent surgery, or certain medications.
When symptoms should be treated as urgent
Seek urgent evaluation if you have any combination of:
- Neck swelling/pain plus fever
- Neck swelling/pain plus shortness of breath or chest pain
- Rapidly worsening swelling, trouble swallowing, voice change, or breathing difficulty
- Neurologic red flags (severe headache unlike usual, confusion, focal weakness)
These combinations do not prove jugular thrombosis, but they justify prompt imaging and evaluation because the consequences of missing a serious clot or neck infection can be significant.
How doctors diagnose it
Diagnosis typically combines a careful history, a focused exam, and imaging that can actually “see” the clot. Because neck pain and swelling have many causes, clinicians aim to confirm three things: Is there a clot? Where is it? What caused it?
1) History and physical exam
Key questions usually include:
- Recent central line, PICC, dialysis catheter, or port placement
- Recent severe sore throat, dental infection, neck infection, or fever
- Cancer history or current chemotherapy
- Recent surgery, trauma, or prolonged immobility
- Prior DVT/PE, miscarriages, or strong family history of clots
- Medication review (especially estrogen therapy) and bleeding risks
On exam, clinicians look for unilateral neck swelling, tenderness along the vein path, visible superficial veins, facial swelling, arm swelling, fever, and lung findings.
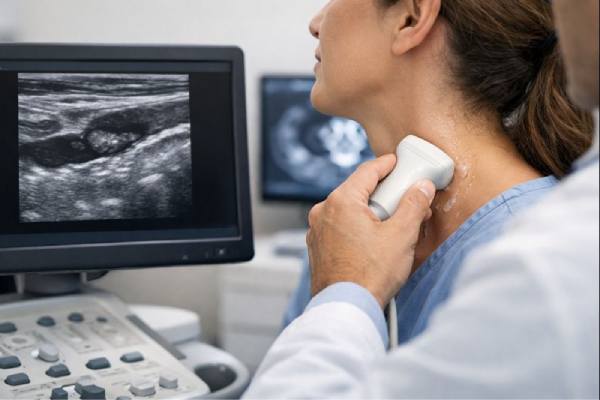
2) First-line imaging: ultrasound with Doppler
Ultrasound is often the first test because it is fast, noninvasive, and can be done at the bedside. Doppler assesses flow. Ultrasound is especially useful for:
- Internal jugular vein evaluation (many cases)
- External jugular or superficial clots
- Tracking changes over time
Limits: ultrasound can be less reliable for deep central veins behind the collarbone or chest structures, and in some patients the view is technically difficult.
3) CT or MR venography when detail matters
If ultrasound is unclear—or if doctors need a better map—CT venography or MR venography may be used. These are helpful when:
- There is suspicion of clot extension into chest veins
- A deep neck infection, abscess, or mass is also suspected
- Symptoms are severe but ultrasound is negative or incomplete
4) Lab tests: supportive, not definitive
Blood tests do not diagnose jugular thrombosis on their own, but they guide safety and cause-finding:
- CBC (anemia, platelet level, infection clues)
- Kidney and liver tests (affect anticoagulant choice and dosing)
- Inflammatory markers when infection is suspected
- Blood cultures if septic thrombophlebitis is possible
- D-dimer may be used in selected contexts, but it is less helpful in hospitalized patients, after surgery, or with infection because it can be elevated for many reasons.
5) Finding the cause: targeted, not “everything at once”
A focused cause evaluation is common:
- If the clot is provoked by a catheter, attention goes to catheter position, function, and infection.
- If infection is likely, clinicians look for the source (throat, teeth, neck spaces) and treat rapidly.
- If unprovoked, clinicians consider cancer screening appropriate to age and risk, and sometimes clotting tendency testing—often delayed until after the acute phase because illness and anticoagulants can skew results.
The goal is not just naming the clot. It’s building a plan that prevents progression, treats the trigger, and reduces recurrence risk.
Treatment options and what to expect
Treatment depends on whether the clot is sterile (not infected) or septic (infected), whether a device is involved, and whether the clot has extended or caused complications like PE. Most treatment plans include some combination of anticoagulation, source control, and monitoring.
1) Anticoagulation (blood thinners)
For many patients, anticoagulation is the main therapy because it helps prevent clot growth, lowers the chance of new clots, and allows the body to gradually break down the clot.
Common approaches include:
- Heparin-based therapy (unfractionated heparin in hospital or low-molecular-weight heparin injections)
- Direct oral anticoagulants (DOACs) such as factor Xa inhibitors, when appropriate
- Warfarin in selected scenarios (for example, when DOACs are unsuitable)
Duration is individualized. Many clinicians treat jugular/upper-body thrombosis for at least 3 months when it behaves like an upper-extremity DVT, especially if the trigger is not immediately reversible. Shorter courses may be considered in select low-risk, clearly provoked cases, while longer treatment may be recommended when cancer, recurrence, or persistent risk factors are present. Follow-up imaging may be used to support stopping decisions, especially if symptoms persist.
2) What about the catheter or device?
If a catheter triggered the clot, the next steps depend on whether it is:
- Infected or malfunctioning: removal is often favored.
- Working well and not infected: it may be kept in place while anticoagulation treats the clot, particularly if access is essential (for example, chemotherapy or dialysis). The decision is weighed against clot burden and infection risk.
3) Antibiotics and source control (when infection is involved)
If clinicians suspect septic thrombophlebitis (for example, Lemierre syndrome), antibiotics are urgent and typically start before culture results return. Treatment often includes:
- Broad coverage initially, then narrowing once cultures and source are clearer
- A longer antibiotic course than a simple throat infection, because infected clots and deep spaces can be hard to sterilize
- Drainage of abscesses or treatment of dental/ENT sources when present
The role of anticoagulation in septic jugular thrombosis can be more nuanced, but many teams use anticoagulation when the clot is extensive, progressing, or associated with embolic complications—balancing bleeding risk and the individual clinical picture.
4) Thrombolysis, thrombectomy, or procedures
These are not routine. They may be considered if there is:
- Severe symptoms from major central vein obstruction
- Threatened limb/organ drainage
- Failure of standard therapy in carefully selected cases
Because bleeding risk is higher, procedural options are typically reserved for specific situations and performed by specialist teams.
5) What patients usually feel during recovery
- Pain and tenderness often improve over days to a few weeks.
- Swelling can take longer, especially if the clot was large or extended into central veins.
- Some people feel “normal” quickly, while others need gradual return to activity.
A good treatment plan includes not only the right medication, but also clear instructions on bleeding precautions, follow-up timing, and what symptoms should trigger urgent re-check.
Management, prevention, and when to seek care
After the initial diagnosis and treatment plan, day-to-day management focuses on three goals: stay safe on therapy, support recovery, and reduce recurrence risk.
1) Living safely with anticoagulation
Practical habits that reduce bleeding risk:
- Take the medication at the same time daily (set a phone reminder).
- Avoid “doubling up” if you miss a dose—follow the plan your clinician gave you.
- Ask before using NSAIDs (like ibuprofen or naproxen) or herbal supplements that can raise bleeding risk.
- Use a soft toothbrush and electric razor if you bruise easily.
- Get urgent care for heavy or persistent bleeding, black stools, vomiting blood, sudden severe headache, or a major fall/head injury.
If you are on warfarin, stable vitamin K intake and INR monitoring are key. If you are on a DOAC, kidney function and drug interactions matter.
2) Activity, posture, and symptom control
Most people do not need strict bed rest. In fact, gentle movement often helps circulation and recovery.
- Resume light activity as symptoms allow, then gradually increase.
- Avoid prolonged neck compression (tight collars, heavy straps) while symptoms are active.
- Use warm compresses for comfort if advised, and consider acetaminophen for pain unless told otherwise.
3) Follow-up and monitoring
Follow-up usually includes:
- A check-in within days to weeks to confirm symptom improvement and medication tolerance
- Repeat imaging when symptoms persist, when decisions about stopping anticoagulation are approaching, or when the initial clot was extensive
- Review of the triggering factor (catheter plan, infection resolution, cancer therapy plan)
4) Prevention strategies (based on cause)
- If a catheter was involved: ensure meticulous line care, confirm appropriate catheter size and position, and remove lines that are no longer needed.
- If infection triggered it: treat throat/dental infections promptly, and seek care if fever and neck pain worsen rather than improve.
- If clotting tendency is a concern: manage modifiable risks—smoking cessation, staying hydrated during travel/illness, moving regularly on long trips, and reviewing hormone therapy options.
- If cancer is present: coordinate clot prevention with oncology/hematology teams; recurrence risk and bleeding risk both matter.
5) When to seek care urgently
Call emergency services or seek urgent evaluation if you develop:
- Sudden shortness of breath, chest pain, coughing blood, or fainting
- Rapidly worsening neck swelling, trouble swallowing, voice change, or breathing difficulty
- High fever, shaking chills, confusion, or severe worsening fatigue
- New major arm swelling or bluish discoloration
- Signs of serious bleeding while on anticoagulation
A final, helpful mindset
Think of jugular vein thrombosis as a “signal event.” The clot is treatable, but the larger win is understanding why it happened—so you can match the intensity of treatment and prevention to your personal risk.
References
- Internal Jugular Vein Thrombosis: A Bicentric Cohort Study – PubMed 2025
- A Comprehensive Review of Catheter-Related Thrombosis – PMC 2024 (Review)
- 2022 international clinical practice guidelines for the treatment and prophylaxis of venous thromboembolism in patients with cancer, including patients with COVID-19 – PMC 2022 (Guideline)
- Internal Jugular Vein Thrombosis – StatPearls – NCBI Bookshelf 2023
- Management of Lemierre Syndrome – PubMed 2021 (Review)
Disclaimer
This article is for educational purposes only and is not a substitute for individualized medical advice, diagnosis, or treatment. Jugular vein thrombosis can be associated with serious conditions, including infection and pulmonary embolism, and needs timely evaluation by a qualified clinician. If you have symptoms such as neck swelling with fever, chest pain, shortness of breath, fainting, or signs of significant bleeding while on blood thinners, seek urgent medical care immediately. Never start, stop, or change anticoagulant or antibiotic therapy without guidance from your healthcare team.
If you found this guide helpful, please consider sharing it on Facebook, X (formerly Twitter), or any platform you prefer—and following us on social media. Your support through sharing helps our team keep producing clear, trustworthy health content.