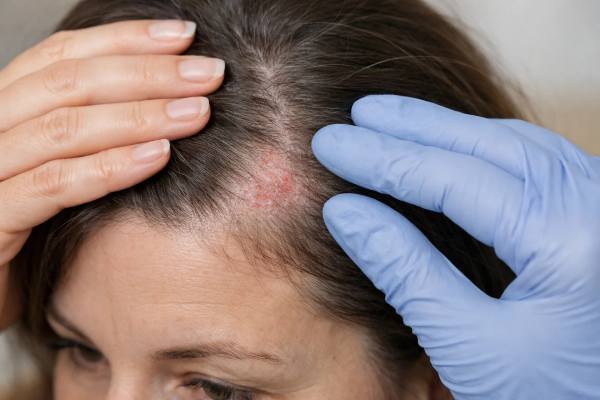
Lichen planopilaris is a form of inflammatory scarring hair loss that can be easy to miss at first. The earliest clues are often not bald patches but scalp symptoms: itching, burning, tenderness, and fine scale around the base of hairs. Because the condition can permanently damage follicles, timing matters. Early recognition and treatment can help calm inflammation and protect the hair that remains, even though areas that have already scarred usually do not fully regrow.
For many people, the hardest part is uncertainty. Lichen planopilaris can resemble other scalp disorders, and the treatment plan often needs adjustment over time rather than a single quick fix. This overview explains what the condition is, how it typically shows up, how doctors confirm the diagnosis, and which treatments are used to slow progression. It also covers realistic expectations, daily scalp care, and the signs that call for prompt dermatology review.
Essential Insights
- Early treatment can reduce active inflammation and help preserve follicles that have not yet scarred.
- The main goals are to ease itching, burning, and shedding while slowing or stopping further permanent hair loss.
- Regrowth is often limited in smooth, scarred areas, so treatment works best before follicular openings disappear.
- Many people need a combination plan, not one product, and response is usually judged over months rather than days.
- Monthly scalp photos in consistent lighting can make early spread easier to spot and discuss at follow-up visits.
Table of Contents
- What lichen planopilaris is
- Symptoms and early warning signs
- How diagnosis is confirmed
- Treatment options and expected results
- Daily care and trigger reduction
- Outlook and when to seek care
What lichen planopilaris is
Lichen planopilaris, often shortened to LPP, is a primary cicatricial alopecia. In plain language, that means it is a scarring hair-loss disorder in which inflammation targets the upper portion of the hair follicle. Over time, that inflammation can destroy the follicle and replace it with scar tissue. Once that happens, the follicle cannot reliably produce a normal hair again.
This is what makes LPP different from common non-scarring hair loss such as androgenetic hair loss or telogen effluvium. In non-scarring loss, follicles are still present, even if they are miniaturized or temporarily resting. In LPP, the core problem is damage to the follicle itself. That is why preserving unaffected follicles is the central goal.
LPP is uncommon, but it is one of the better-known causes of lymphocytic scarring alopecia. It tends to affect adults more often than children and can appear in any sex, though some related patterns are seen more often in women. The classic form usually causes irregular patches of hair loss on the crown, vertex, or parietal scalp. A related pattern, frontal fibrosing alopecia, is often considered a variant of LPP and more often affects the frontal hairline and eyebrows. A rarer variant, Graham-Little syndrome, combines scalp scarring alopecia with follicular papules on the body and hair loss in other regions.
The exact cause is still not fully settled. The leading view is that the immune system loses tolerance to part of the follicle, especially in a region important for hair regeneration. Genetics, autoimmunity, hormones, and environmental triggers may all play some role, but no single cause explains every case. This uncertainty matters because it explains why treatment is often individualized and why people can respond very differently to the same medication.
Another important point is that LPP is not simply “sensitive scalp” or routine shedding. It is an inflammatory disease, and signs of scalp inflammation should be taken seriously. Readers comparing symptoms with broader signs of scalp inflammation should remember that scarring disorders deserve faster evaluation than ordinary cosmetic scalp irritation.
The practical takeaway is straightforward: LPP is a condition in which delay can cost follicles. Treatment focuses on calming active inflammation, monitoring spread, and protecting hair that is still viable. Hair already lost in scarred areas may not come back, but a well-managed plan can still make a meaningful difference in symptoms, stability, and appearance.
Symptoms and early warning signs
The earliest stage of lichen planopilaris is often more symptomatic than it looks. Many people first notice itching, burning, stinging, tenderness, or a feeling that the scalp is sore to the touch. Some describe a tight, prickly sensation around specific patches rather than a diffuse itch across the whole scalp. That localized discomfort can be an important clue.
Visible changes may be subtle at first. Common early findings include redness around hair follicles, fine perifollicular scale, and hairs that seem easier to dislodge from active zones. The scalp may look slightly pink with a collar of scale around individual shafts. On close inspection, there may be a reduced density of hairs in a patchy pattern rather than uniform thinning. As inflammation continues, patches can widen and the skin can start to look smoother and shinier, with fewer visible follicular openings.
Typical symptoms and signs include:
- Itching, burning, pain, or tenderness of the scalp
- Patchy hair loss, often on the crown or top of the scalp
- Redness around follicles
- Scale or keratin casts that cling to the hair shaft
- A smooth or shiny look in more advanced areas
- Less visible follicular openings in affected patches
- Ongoing shedding from inflamed zones
One reason LPP is confusing is that it can overlap with other scalp problems. Dandruff, seborrheic dermatitis, contact dermatitis, psoriasis, bacterial folliculitis, discoid lupus, central centrifugal cicatricial alopecia, and even traction can share pieces of the picture. That is why a new itchy patch with visible thinning deserves more attention than a routine flaky scalp. If you are sorting through broader itchy scalp causes, note that persistent symptoms plus patchy loss or a shiny scar-like area raise the level of concern.
Classic LPP most often appears in irregular patches. Frontal fibrosing alopecia, the better-known variant, more often causes a band-like recession along the frontal or temporal hairline and may include eyebrow loss, facial papules, or loss of body hair. Both patterns can coexist. Some people mainly feel symptoms; others notice visual thinning first. The balance between symptoms and visible loss varies widely.
Advanced disease looks different from early disease. Once scarring is established, active redness and scale may lessen, but the loss becomes more permanent. That can create a false sense that the disease is “quiet” when the real question is whether the border of the patch is still inflamed and expanding.
The key early warning signs are not just hair loss itself, but inflammatory hair loss: scalp discomfort, follicular redness, perifollicular scale, and patches that seem to enlarge over time. New eyebrow thinning, a rapidly changing hairline, or bald areas that look smooth rather than fuzzy should prompt timely evaluation.
How diagnosis is confirmed
Diagnosing lichen planopilaris usually starts with pattern recognition, but confirmation often requires more than a quick visual exam. A dermatologist or hair-loss specialist will look at where the loss is happening, whether symptoms suggest active inflammation, and whether the scalp still shows normal follicular openings. The story matters too: when the symptoms began, how fast patches are spreading, whether eyebrows or body hair are involved, and what products, hairstyles, medications, or autoimmune issues may be relevant.
Trichoscopy, which is dermoscopy of the scalp and hair, is one of the most useful office tools. It allows the clinician to magnify the scalp and look for signs such as perifollicular scale, perifollicular redness, absent follicular openings, white scarred areas, and other inflammatory changes. Trichoscopy is especially helpful for finding the active edge of disease, which matters because that is usually the best place to sample if a biopsy is needed.
A scalp biopsy remains the most important confirmatory test when the diagnosis is uncertain, when several scarring alopecias are being considered, or when treatment decisions depend on a firm tissue diagnosis. In general, biopsy is taken from an active margin rather than the smoothest fully scarred center, because the active border is more likely to show the inflammatory pattern that defines the condition. If you want a clearer sense of what this test can show, scalp biopsy results often reveal whether the process is scarring, how much inflammation is present, and which type of alopecia pattern is most likely.
Laboratory tests do not diagnose LPP directly. There is no single blood test that confirms it. Labs may still be ordered to rule out mimics, investigate related autoimmune concerns, or check medication safety before treatment starts. In some cases, testing is tailored to symptoms, history, and planned drugs rather than done routinely for everyone.
Diagnosis usually brings together four pieces:
- Clinical pattern: patchy scarring alopecia on the scalp, or a frontal hairline and eyebrow pattern in the variant form.
- Symptoms: itching, burning, tenderness, or increased shedding in active areas.
- Trichoscopy findings: perifollicular scale, erythema, and loss of follicular openings.
- Histology when needed: biopsy evidence of a lymphocytic scarring alopecia with a lichenoid pattern.
Follow-up is part of diagnosis too. Doctors often compare serial photographs, symptom scores, and the amount of redness or scale over time. That is because LPP is not only about naming the condition; it is about deciding whether it is active right now. A stable scarred patch and a quietly expanding inflammatory border are not the same clinical problem, and they do not call for the same urgency or treatment intensity.
Treatment options and expected results
Treatment for lichen planopilaris is aimed at disease control, not a guaranteed cosmetic reset. The realistic goals are to reduce symptoms, decrease inflammatory signs such as redness and scale, and slow or stop further permanent loss. Regrowth can happen in less-damaged follicles, but smooth scarred skin usually has limited capacity to recover dense hair.
Most treatment plans combine local anti-inflammatory therapy with longer-term monitoring. Common first steps include potent topical corticosteroids and corticosteroid injections into active areas. These approaches try to suppress inflammation where it is happening most. They can be useful for patches with perifollicular redness, scale, pain, or recent spread. Topical calcineurin inhibitors are sometimes used in selected cases, especially when steroid burden needs to be reduced.
When disease is more active, symptomatic, or extensive, doctors often add a systemic medication. Hydroxychloroquine is a frequent early systemic choice because it can help reduce inflammatory activity over time. Other oral options used in selected patients include doxycycline, mycophenolate, methotrexate, cyclosporine, short courses of oral corticosteroids, and sometimes pioglitazone or retinoid-based therapy in related patterns. The choice depends on disease severity, speed of progression, coexisting conditions, pregnancy planning, lab risk, and how aggressive treatment needs to be.
A few practical points matter:
- Improvement is often judged over months, not weeks.
- Symptom relief may come before visible stabilization.
- Some drugs are used off label and need bloodwork or other monitoring.
- Treatment may need to change if control is incomplete or side effects limit use.
Hair-growth support is often added alongside anti-inflammatory treatment. Topical or oral minoxidil does not treat the scarring process itself, but it can help maximize the output of follicles that are still functioning. That is why it is commonly included as an adjunct, especially when LPP overlaps with pattern hair loss. Readers comparing options can review how minoxidil works for hair loss while keeping in mind that LPP still requires inflammation control.
Newer therapies are being explored, including JAK inhibitors in selected difficult cases, but the evidence remains limited compared with better-established treatments. This is an area of active interest rather than a settled first-line standard.
Expectations should be specific. A good response may mean less itching, less burning, less perifollicular scale, and no obvious expansion of patches over several visits. It may not mean full regrowth. That distinction can be emotionally difficult, but it is one of the most important parts of informed care. In LPP, preserving hair today is often the best route to a better-looking scalp six or twelve months later.
Daily care and trigger reduction
Medical treatment does most of the heavy lifting in lichen planopilaris, but daily scalp habits still matter. The goal of self-care is not to cure the disease at home. It is to reduce added irritation, make symptoms easier to tolerate, and protect the scalp barrier while prescription treatment is doing its job.
A gentle routine is usually best. Use a mild shampoo suited to your scalp type and wash often enough to remove sweat, oil, and product buildup without scrubbing aggressively. There is no evidence that ordinary washing causes LPP, but harsh manipulation can make an inflamed scalp feel worse. Fingernails, stiff brushes, gritty exfoliants, and vigorous massage are common triggers for soreness in active areas.
Helpful day-to-day habits include:
- Keep shampooing gentle and thorough rather than forceful.
- Avoid picking at scale or scratching active patches.
- Limit high-heat tools if the scalp feels tender or inflamed.
- Avoid tight hairstyles that add traction to already stressed follicles.
- Be cautious with dyes, relaxers, and other strong chemical processes during flares.
- Use fragrance-light products if the scalp is reactive.
Sun protection matters too, especially if the scalp is more visible because of thinning. Inflamed or scarred skin can be more sensitive, and sun exposure may worsen discomfort. A hat with breathable fabric is often the simplest choice. For readers building a broader routine, scalp sun protection with hats and SPF becomes more important as hair density decreases.
Monthly documentation can be surprisingly useful. Take photos of the same regions in the same lighting, with hair parted the same way each time. This can reveal subtle progression that is easy to miss day to day. It also gives your clinician a more reliable way to compare change than memory alone.
Supportive styling options are worth considering early, not only after major loss. Camouflage powders, fibers, strategic part changes, toppers, wigs, and careful haircut adjustments can reduce visual contrast and improve confidence while treatment is underway. These do not interfere with medical management when used thoughtfully.
What should you avoid? The short answer is anything that repeatedly inflames the scalp or makes it harder to judge disease activity. That includes frequent product switching, self-prescribed harsh actives, repeated scalp “detox” treatments, and internet remedies that promise regrowth in scarred areas. In LPP, a calmer scalp is usually a better scalp. Self-care works best when it is boring, consistent, and easy to maintain.
The most useful home mindset is this: reduce extra friction, protect the skin, and let treatment be measurable. Routine, not experimentation, usually gives the clearest path forward.
Outlook and when to seek care
The course of lichen planopilaris is variable. Some people have a relatively limited area that stabilizes with treatment, while others have persistent activity that requires several medication changes. The disease can wax and wane, which is one reason follow-up matters even after symptoms improve. A quieter scalp is encouraging, but stability should be confirmed over time rather than assumed after a short calm period.
In general, prognosis depends on how early the condition is recognized, how active the inflammation is, and how much irreversible scarring has already occurred. That is why the best outcomes usually come from early identification of active disease rather than waiting for larger smooth patches to appear. Areas that still have visible follicular openings are more likely to respond cosmetically than areas that look shiny and scarred.
Follow-up visits typically focus on a few practical questions:
- Are itching, burning, or tenderness improving?
- Is there still perifollicular redness or scale?
- Are the borders of patches stable on exam and photos?
- Are eyebrows, hairline, or other body sites changing?
- Is the current medication effective and well tolerated?
It is also common for LPP to overlap with other forms of hair loss, especially pattern thinning. When that happens, treatment may need to address both the inflammatory scarring component and the non-scarring component at the same time. That overlap is one reason a personalized plan matters more than a one-size-fits-all checklist.
Seek prompt specialist care if you notice a painful or burning scalp with patchy thinning, rapidly increasing hairline recession, new eyebrow loss, a shiny bald patch, or hair loss that continues despite basic scalp treatment. A faster appointment is especially important when symptoms are active right now, because active inflammation offers the clearest target for diagnosis and early control. If you are unsure about timing, signs that help define when to see a dermatologist for hair loss become more urgent when scarring is on the differential.
The emotional side should not be minimized. Permanent hair loss can change how a person feels in social settings, at work, and in daily routines. Even when the medical plan is solid, the adjustment can be hard. Cosmetic support, counseling, or a support community can be a useful part of care rather than an afterthought.
The bottom line is hopeful but honest: LPP is a chronic inflammatory scarring alopecia, yet it is treatable in the sense that activity can often be reduced and progression can often be slowed. The earlier that process begins, the more hair there is to protect.
References
- A Practical Approach to the Diagnosis and Management of Classic Lichen Planopilaris 2021 (Review)
- Lichen planopilaris and frontal fibrosing alopecia: review and update of diagnostic and therapeutic features 2022 (Review)
- Treatment of Lichen Planopilaris and Frontal Fibrosing Alopecia: A Retrospective, Real-Life Analysis in a Tertiary Center in Germany 2024 (Retrospective Study)
- JAK Inhibitors in the Treatment of Lichen Planopilaris 2024 (Review)
- Systemic Treatments for Lichen Planopilaris and Frontal Fibrosing Alopecia: A Retrospective Study of 315 Patients 2025 (Retrospective Study)
Disclaimer
This article is for educational purposes only and is not a medical diagnosis or a substitute for personal care from a dermatologist or other qualified clinician. Lichen planopilaris is a scarring hair-loss disorder, and delaying evaluation can affect outcomes. A new or worsening painful, itchy, burning, or patchy scalp condition should be assessed by a medical professional, especially if hair loss appears permanent or the skin looks smooth and scarred.
If this article helped you, please consider sharing it on Facebook, X, or another platform you trust so more readers can find it.






