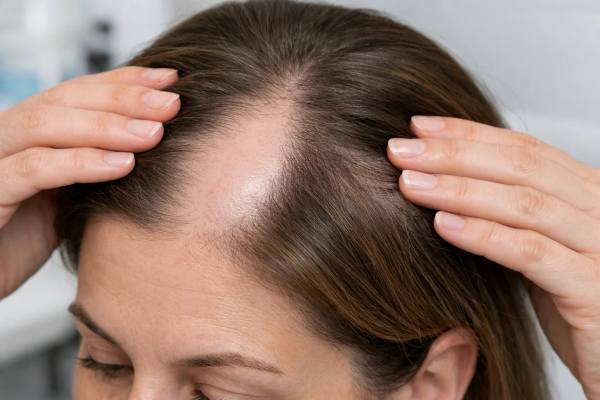
Hair loss in lupus is rarely just one thing. Some people notice sudden diffuse shedding during a flare. Others develop fragile, shortened hairs around the frontal hairline. And some face inflamed scalp plaques that slowly replace follicles with scar tissue. Those patterns can look similar at first, yet they do not carry the same meaning or the same chance of regrowth.
That is why the most important question is not simply, “Is lupus causing my hair loss?” It is, “What kind of lupus-related hair loss is this?” Non-scarring alopecia often improves once inflammation is controlled and the hair cycle resets. Scarring alopecia, most often from scalp discoid lupus, can become permanent if treatment is delayed.
A clear diagnosis makes the next steps much more practical. It helps you understand whether regrowth is likely, which signs suggest active scalp disease, when a biopsy is useful, and which treatments are meant to calm inflammation rather than merely stimulate growth.
Quick Overview
- Non-scarring lupus hair loss often regrows once disease activity and scalp inflammation are brought under control.
- Scarring alopecia from chronic cutaneous lupus can become permanent, so early recognition matters.
- Redness, scale, burning, tenderness, pigment change, and loss of follicle openings suggest active scalp disease rather than simple shedding.
- Topical anti-inflammatory treatment and systemic lupus control are often more important than hair-growth products alone.
- Prompt evaluation is especially useful when a patch is expanding or the scalp starts to look shiny, smooth, or scarred.
Table of Contents
- How Lupus Causes Hair Loss
- Scarring and Non-Scarring Alopecia Explained
- Symptoms That Point to Scalp Lupus
- How Doctors Confirm the Cause
- Treatment Options for Non-Scarring Hair Loss
- Treating Scarring Alopecia and Protecting Regrowth
How Lupus Causes Hair Loss
Lupus can affect hair through more than one pathway, which is why the term “lupus hair loss” is too broad to be useful on its own. In some cases, the problem is systemic inflammation. During a lupus flare, inflammatory signals can push more follicles out of their normal growth phase and into premature shedding. The result may be diffuse thinning across the scalp, increased hair in the shower, and a general drop in density rather than sharply outlined bald patches.
In other cases, the problem is direct inflammation in the scalp skin. Cutaneous lupus, especially chronic cutaneous lupus such as discoid lupus erythematosus, can target the follicular environment itself. When that inflammation stays active long enough, it can damage the follicle’s stem cell region and turn a potentially reversible problem into cicatricial, or scarring, alopecia. That is the dividing line that matters most: if the follicle is inflamed but still structurally intact, regrowth is often possible; if it has been destroyed and replaced by scar tissue, regrowth becomes much less likely.
Lupus-related hair loss can also be mixed. A person may have active systemic lupus with diffuse shedding at the same time that a few scalp plaques are creating localized scarring risk. That overlap is one reason lupus hair loss often feels confusing. It may not fit a single pattern, and what looks like one issue in the mirror may actually be two processes occurring together.
Another layer is that lupus does not exclude other causes of alopecia. Someone with lupus can also develop telogen effluvium after illness, medication-related shedding, iron deficiency, thyroid disease, or autoimmune patchy loss. Distinguishing these from lupus-specific changes is part of the workup, especially when the history includes fatigue, weight change, recent fever, medication shifts, or the broader pattern described in shedding versus lasting hair loss.
There is also a classic but often misunderstood finding called “lupus hair.” These are short, dry, fragile hairs, often around the frontal hairline. They may look broken or frayed, yet they reflect inflammatory disruption rather than simple cosmetic damage alone. Some people notice eyebrow thinning as well, while others describe hair that becomes harder to style long before it becomes visibly sparse.
The key insight is that lupus does not cause one signature hairstyle or one universal pattern of balding. It causes a spectrum. The practical approach is to ask three questions early: Is the loss diffuse or patchy? Is the scalp inflamed? Are follicles still present? Those answers guide both the diagnosis and the odds of regrowth far better than the word “lupus” by itself.
Scarring and Non-Scarring Alopecia Explained
The difference between scarring and non-scarring alopecia is not just academic. It changes how quickly treatment is needed, what regrowth to expect, and how a dermatologist interprets the scalp exam. In lupus, both types can occur.
Non-scarring alopecia means the follicles are still there. The hair may shed, miniaturize, or look sparse, but the basic follicular openings remain. In lupus, non-scarring patterns often include diffuse thinning, increased shedding during active systemic disease, patchy nonscarring loss, and frontal short hairs known as lupus hair. These forms can look dramatic, but they are usually more reversible. Once inflammation settles and the hair cycle normalizes, many patients regain density over time.
Scarring alopecia is different. Here, chronic inflammation destroys the follicle and replaces it with fibrous tissue. The most important lupus-related cause is scalp discoid lupus erythematosus. Early lesions may be red or violaceous, scaly, and plugged around follicles. Later, the area may become smooth, shiny, pale, or dyspigmented, with fewer visible follicle openings. At that stage, some of the loss is no longer temporary.
A simple way to compare the two is this:
- Non-scarring lupus alopecia tends to preserve follicle openings and has a better chance of regrowth.
- Scarring lupus alopecia gradually erases those openings and can leave permanent gaps if treatment is delayed.
- Mixed presentations can occur, especially when diffuse shedding sits beside one or two inflamed scalp plaques.
The patchy forms create the most confusion. Some nonscarring lupus patches can resemble alopecia areata, while early discoid lupus can be mistaken for dandruff, eczema, or a minor irritated spot. That is why the scalp surface matters so much. Smooth skin without inflammation may suggest one process; scale, follicular plugging, dyspigmentation, and tenderness point in another direction.
Location can help, but it is not enough on its own. Scalp discoid lupus often affects sun-exposed areas and may spread slowly at the edges. Diffuse lupus-related shedding, by contrast, usually feels more global and may line up with a systemic flare or other illness. Yet there is enough overlap that diagnosis should never rely on pattern alone.
For patients, the most important takeaway is this: non-scarring hair loss asks, “How do we calm the disease and help the hair cycle recover?” Scarring alopecia asks, “How much inflammation is still active, and how do we stop further follicle loss now?” The first is often about regrowth. The second is about preservation, with regrowth possible only in areas where follicles have not been fully destroyed.
Symptoms That Point to Scalp Lupus
Scalp lupus is easier to recognize when you stop looking only at the hair and start looking at the scalp itself. Hair loss caused by lupus often comes with surface clues that ordinary shedding does not. Those clues can be subtle at first, which is why many people spend months treating the wrong problem.
In non-scarring lupus alopecia, the main complaint may be increased shedding, overall thinning, or hair that suddenly feels less dense. The scalp may look relatively normal or only mildly inflamed. Some patients notice more hair fall during washing, a broader part line, or temple and frontal hairs that stay short and wispy. Those front hairs may seem fragile, uneven, and difficult to smooth back. That pattern is especially suggestive when it appears alongside other signs of lupus activity.
Scarring lupus alopecia usually looks more inflammatory. Common warning signs include:
- persistent redness or dusky discoloration,
- adherent scale,
- follicular plugs,
- burning, stinging, or tenderness,
- lighter or darker skin after inflammation,
- patches that slowly become smoother and shinier.
These changes matter because they suggest the follicle is under direct attack. Once the scalp starts losing visible follicular openings, the window for easy regrowth narrows.
Symptoms can also evolve over time. Early discoid lupus may itch or burn and look only mildly scaly. Later, the center of the patch may flatten and scar while the border remains active. That combination of quiet center and inflamed edge is one reason a lesion can be mistaken for an old scar when it is actually still progressing.
Photosensitivity is another clue. If scalp patches or hair loss worsen after sun exposure, lupus should stay on the list. On the scalp, ultraviolet exposure is easy to overlook, especially along the part line, frontal hairline, or areas where density has already decreased. Because inflammation can hide under the hair for a long time, subtle tenderness or an unusual warm, irritated feeling may be more informative than dramatic redness.
Still, none of these signs is exclusive to lupus. Seborrheic dermatitis, psoriasis, lichen planopilaris, fungal infection, and contact reactions can all cause visible scalp inflammation. That is why readers who are tracking signs of scalp inflammation should treat them as reasons for evaluation, not as proof of one diagnosis.
A useful rule is to worry less about the number of hairs you lose on a given day and more about the behavior of the scalp. Hair that sheds from a calm scalp may still regrow. Hair loss from a painful, scaly, expanding, or shiny patch deserves faster attention. In lupus, that distinction often tells you whether the problem is likely to be reversible shedding, active follicular damage, or a combination of both.
How Doctors Confirm the Cause
Diagnosing lupus hair loss starts with the pattern, but it should not end there. A dermatologist usually combines history, scalp examination, trichoscopy, and selected tests to decide whether the loss is non-scarring, scarring, or partly both. The goal is not just to label the condition. It is to identify whether there is active inflammation that can still be stopped.
The history often reveals the first clue. Diffuse shedding after a lupus flare suggests one pathway. Slowly enlarging plaques with scale, color change, or tenderness suggest another. Timing matters too. Hair loss that accelerates with fevers, medication changes, recent hospitalization, or nutritional restriction may have a second driver layered on top of lupus.
The exam then focuses on the scalp surface. Dermatologists look for follicular openings, perifollicular scale, keratotic plugs, redness, dyspigmentation, broken hairs, and the shape of the patch border. Trichoscopy, a magnified scalp exam, helps show features that are hard to see with the naked eye. It can support lupus as the cause and help distinguish it from lichen planopilaris, psoriasis, alopecia areata, and other inflammatory disorders.
A practical workup often includes these steps:
- Careful review of lupus history, disease activity, medications, and flare pattern.
- Scalp and hair exam to decide whether the alopecia is diffuse, patchy, inflammatory, or scarring.
- Trichoscopy to assess follicular openings, plugs, vessels, scale, and shaft changes.
- Blood testing when the history suggests additional contributors such as anemia, thyroid disease, or nutritional deficiency.
- Scalp biopsy when the diagnosis is uncertain, when scarring alopecia is suspected, or when more than one diagnosis is possible.
Biopsy is especially important in patchy inflammatory cases. It is often taken from an active border rather than from the oldest scarred center, because that is where the tissue is most likely to show the process clearly. If you want a clearer sense of what clinicians learn from that test, this guide to scalp biopsy findings in hair loss provides useful background.
Laboratory tests can support the bigger picture, but they do not replace scalp evaluation. Lupus-related hair loss may coexist with low ferritin, thyroid dysfunction, or medication effects, and those factors can worsen recovery if they are missed. Even so, blood work alone cannot tell whether follicles are being scarred.
The most helpful mindset is to treat lupus alopecia as a diagnosis that deserves precision. A person with active scalp discoid lupus needs a different level of urgency than someone with diffuse shedding during a flare. Both need care, but only one is at high risk of permanent follicle loss. Good diagnosis is what prevents reversible thinning from being undertreated and irreversible scarring from being recognized too late.
Treatment Options for Non-Scarring Hair Loss
When lupus hair loss is non-scarring, the treatment goal is straightforward: reduce inflammation, control the underlying disease, and give follicles a chance to return to normal cycling. That usually means the best “hair treatment” is not a cosmetic product at all, but effective lupus management.
If the hair loss is tied to active systemic lupus, regrowth often depends on bringing the overall disease under control. Hydroxychloroquine is a common foundation because it can help both skin and systemic disease, though it is not an instant fix. Some patients also need a short course of corticosteroids to calm a flare while slower treatments take effect. In others, treatment is adjusted with steroid-sparing agents chosen by the dermatologist or rheumatologist based on the broader lupus picture.
When the scalp itself shows inflammatory activity but follicles are still preserved, topical treatment becomes more important. High-potency topical corticosteroids are often used for short periods on the scalp. Calcineurin inhibitors may be used in selected areas, especially when steroid exposure needs to be limited. These treatments are not meant to “grow hair” directly. They are meant to lower the inflammation that is interrupting normal growth.
Adjuncts can still help. Topical minoxidil is sometimes added to support density and speed visible recovery once disease control is underway. It is best thought of as supportive, not primary. If active lupus is left untreated, growth stimulants alone rarely solve the problem.
Daily care matters more than many people expect. Helpful habits include:
- avoiding tight styles on already inflamed areas,
- minimizing hot tools during active shedding,
- washing gently but regularly so scale and product buildup do not obscure the scalp,
- protecting the scalp from ultraviolet exposure with hats, shade, and appropriate scalp-safe protection.
That last point is especially important in cutaneous lupus. Photoprotection is part of treatment, not an optional extra, and practical strategies for protecting the scalp from sun damage can make a real difference.
Patients also need realistic timing. Even when treatment is working, hair regrowth lags behind inflammation control. Shedding may settle first. Density improves later. Visible recovery often unfolds over months, not weeks. This is one reason people sometimes stop helpful treatment too early.
It is also worth checking for overlapping factors. Lupus patients can still have low iron stores, thyroid disease, stress-related shedding, or medication-related loss. Those issues do not replace the lupus diagnosis, but they can slow regrowth if ignored.
The encouraging part is that non-scarring lupus alopecia usually offers a meaningful chance of recovery. The caveat is that recovery depends less on finding the perfect hair product and more on matching treatment to disease activity, scalp findings, and the patient’s broader lupus plan.
Treating Scarring Alopecia and Protecting Regrowth
Scarring alopecia from lupus demands a different conversation. Here, the priority is not simply to regrow hair. It is to stop active inflammation before more follicles are lost. This is why scalp discoid lupus is treated with more urgency than diffuse non-scarring shedding, even when the affected area looks smaller.
Treatment usually begins with anti-inflammatory therapy directed at the scalp lesion itself and, when needed, systemic treatment to control the broader disease. Topical corticosteroids and intralesional steroid injections are commonly used for active plaques. Hydroxychloroquine is often the systemic anchor. If response is incomplete or the disease is more aggressive, clinicians may escalate to other systemic options such as methotrexate, mycophenolate, retinoids, dapsone, or other immunomodulatory treatment chosen according to the patient’s skin and systemic disease pattern. In patients with broader lupus activity, rheumatology-directed therapies may also change the scalp outcome indirectly by reducing disease activity overall.
The hardest part of counseling is explaining regrowth honestly. Active, inflamed edges may still contain salvageable follicles, so some recovery can happen if treatment begins early enough. Fully scarred, smooth, shiny areas usually do not regrow meaningful hair because the follicle structure has already been lost. That does not mean treatment has failed. It may have successfully prevented the scar from expanding.
Monitoring is therefore crucial. A patch that looks “quiet” at a glance may still be smoldering at the border. Follow-up visits help determine whether redness, scale, tenderness, and perifollicular activity are improving. If they are not, treatment often needs to be adjusted rather than simply continued unchanged.
Cosmetic support also deserves a place in the plan. For stable areas of loss, patients may benefit from:
- strategic haircuts and part changes,
- color-matched camouflage powders or fibers,
- scalp-friendly styling that avoids tension,
- partial hairpieces, toppers, or wigs when coverage is more substantial.
For many people, guides on wigs and toppers for hair loss become just as practical as medication discussions.
Hair transplantation is usually not a first-line answer. In active scarring alopecia, transplanting into an inflamed scalp risks poor survival and further disappointment. It is generally considered only after prolonged disease quiet and specialist confirmation that the process is truly inactive.
The core message is clear: in scarring lupus alopecia, success means preserving follicles before they disappear. Early treatment can save hair that has not yet scarred. Later treatment can still stop progression and reduce symptoms, but it cannot reliably recreate follicles that are already gone. That is why any patch with scale, pain, pigment change, or a smooth shiny center deserves prompt specialist assessment.
References
- Non-scarring alopecia of lupus erythematosus: A comprehensive review 2023 (Review)
- Cutaneous Lupus Erythematosus: An Update on Pathogenesis and Future Therapeutic Directions 2023 (Review)
- Trichoscopic Features of Scalp Discoid Lupus Erythematosus versus Lichen Planopilaris: A Systematic Review 2024 (Systematic Review)
- British Association of Dermatologists guidelines for the management of people with cutaneous lupus erythematosus 2021 2021 (Guideline)
- Recent Insight on the Management of Lupus Erythematosus Alopecia 2021 (Review)
Disclaimer
This article is for educational purposes only and does not replace medical advice, diagnosis, or treatment. Lupus-related hair loss can overlap with other causes of alopecia, and scarring forms may become permanent if evaluation is delayed. If you have expanding patches, scalp pain, redness, scale, or sudden diffuse shedding with other lupus symptoms, seek assessment from a dermatologist or rheumatologist.
If you found this article helpful, please share it on Facebook, X, or your preferred platform so others dealing with lupus hair loss can find clear, practical information.






