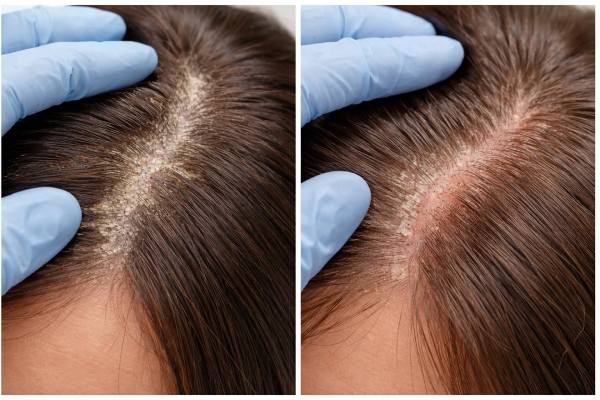
Perifollicular scaling sounds technical, but the finding itself is simple: scale gathers around the opening of individual hair follicles instead of sitting only as loose flakes across the scalp. That detail matters. It can show up in common conditions such as seborrheic dermatitis, but it can also appear in disorders where the follicle is being inflamed more deeply, including scarring alopecias like lichen planopilaris. In other words, the same visual clue can point to very different levels of urgency.
That is why the question is not only “Do I have scale?” but “What else is happening with it?” The pattern of redness, itch, pain, hair shedding, follicular loss, and scalp texture helps move the diagnosis in the right direction. This article explains what perifollicular scaling means, how seb derm and psoriasis usually differ, when scarring alopecia becomes the real concern, and how dermatologists sort these conditions apart before permanent damage occurs.
Quick Overview
- Perifollicular scaling is a clue, not a diagnosis, and it matters most when paired with the rest of the scalp exam.
- Seb derm usually causes greasy or yellowish scale with itch, while psoriasis more often brings thicker white scale and sharper redness.
- Scarring alopecia becomes more likely when scaling is paired with perifollicular redness, pain, smooth patches, or disappearing follicular openings.
- A close scalp exam and trichoscopy often narrow the answer quickly, but biopsy may be needed when permanent follicle damage is suspected.
- If scale is centered around follicles and comes with tenderness, burning, or patchy hair loss, treat it as a prompt for timely dermatology review.
Table of Contents
- What perifollicular scaling actually means
- Features that fit seb derm
- When psoriasis is more likely
- Red flags for scarring alopecia
- How dermatologists tell them apart
- What to do next and when to seek care
What perifollicular scaling actually means
Perifollicular scaling means that flakes or scale are concentrated around hair follicles, often forming a collar, sleeve, or cuff at the base of individual hairs. That is different from diffuse flaking, where loose scale sits broadly on the scalp surface without clearly centering on follicular openings. The distinction may sound subtle, but it can be diagnostically important because the follicle itself becomes part of the story.
In practical terms, perifollicular scale suggests that inflammation, keratin buildup, or altered oil and skin turnover is happening right where the hair exits the scalp. That can occur in relatively common inflammatory disorders such as seborrheic dermatitis. It can also appear in psoriasis. But it becomes especially meaningful when it is accompanied by perifollicular redness, pain, or loss of follicular openings, because those features raise concern for a scarring alopecia.
This is why perifollicular scaling should be treated as a sign, not a final label. The same visible clue may represent very different processes:
- In seborrheic dermatitis, it may reflect oil-rich inflammation and yeast-driven scaling around follicles.
- In psoriasis, it may appear alongside thicker, more adherent white scale and characteristic vascular patterns.
- In scarring alopecia, it may reflect active inflammation targeting the follicular unit itself.
Another reason the term matters is that patients often describe all scalp flaking with the same language: dandruff, buildup, dryness, or itch. Those words can miss the follicular pattern entirely. A scalp can look only mildly flaky in the mirror while trichoscopy shows that the scale is concentrated around follicular ostia, which may change the differential diagnosis.
Perifollicular scaling also does not always travel alone. It may appear with:
- Itching or burning
- Scalp tenderness
- Redness around follicles
- Hair shedding from inflamed zones
- Thick or greasy scale
- Smooth areas where follicular openings are harder to see
That last point is what makes careful observation so important. When follicles are still clearly visible and hair density is preserved, the problem may still sit in a reversible inflammatory range. When follicular openings start disappearing, the conversation shifts toward possible permanent damage.
A helpful mental model is to think of perifollicular scaling as a location marker. It tells you where the activity is happening, not why it is happening. The “why” comes from the rest of the exam: what the scale looks like, what the scalp feels like, how the hair is changing, and whether the follicle still appears structurally intact.
If you are already noticing itch, tenderness, or shedding with scale at the root, broader signs of scalp inflammation can help you decide whether this is more than a cosmetic flake problem. Perifollicular scaling is not always dangerous, but it is rarely something to interpret in isolation.
Features that fit seb derm
Seborrheic dermatitis, often shortened to seb derm, is one of the most common explanations for scalp scale, and it can absolutely produce perifollicular scaling. In fact, in many clinical and trichoscopic studies, follicle-centered scale is a frequent feature of seb derm. What keeps it from being confused with more serious follicular disease is the rest of the pattern.
Seb derm typically favors oily, sebaceous areas and tends to create a scalp that feels itchy, greasy, and flaky rather than sharply painful. The scale is often yellowish-white or greasy rather than dry and powdery. Redness may be present, but it is often patchy and softer-edged than the classic plaques of psoriasis. Many people also have related involvement in other oil-rich areas such as the eyebrows, sides of the nose, beard region, or behind the ears.
Common clues pointing toward seb derm include:
- Greasy or yellowish scale
- Itch that fluctuates with stress, sweat, or skipped wash days
- A scalp that feels oily quickly after cleansing
- Flaking in the brows, beard, or folds around the nose
- Mild redness without clear smooth scarred patches
- Improvement with antifungal shampoos or more frequent washing
Perifollicular scale in seb derm often sits beside interfollicular scale rather than replacing it. In plain language, you may see scale around follicles and across the scalp at the same time. That mixed pattern is one reason people describe seb derm as “dandruff that keeps coming back.”
What seb derm usually does not do is erase follicular openings in a progressive way. It may cause temporary increased shedding because inflammation and scratching can disrupt normal cycling, but it does not usually cause classic permanent scarring alopecia on its own. That is an important distinction when a patient worries that every greasy flaky scalp condition is destroying follicles irreversibly.
Still, seb derm is not trivial. A chronically inflamed scalp can become very uncomfortable and can be confused with more serious disease. It can also overlap with psoriasis, creating the gray zone sometimes called sebopsoriasis. In those cases, the scalp may show traits of both conditions: oilier scale than classic psoriasis but more persistent redness and plaque-like areas than ordinary seb derm.
A useful clue is timing. Seb derm often worsens when washes are stretched too long, during stress, in colder seasons, or with heavy product use. It tends to improve with a targeted wash routine, especially shampoos built around antifungal or keratolytic ingredients. If you are already trying to sort out recurring flakes, the difference between dandruff and dry scalp often helps clarify why seb derm behaves differently from simple dryness.
The main trap is assuming that greasy scale always means a minor problem. Seb derm is common, but persistent follicle-centered scale that does not respond to a reasonable anti-dandruff plan deserves a closer look. The diagnosis may still be seb derm, but the scalp should earn that label by behaving like it.
When psoriasis is more likely
Psoriasis can also produce perifollicular scaling, but the overall picture often looks different from seb derm. The classic scalp psoriasis pattern features thicker, more adherent scale, a brighter inflammatory background, and more sharply demarcated plaques. Instead of greasy yellowish flakes, the scale tends to be drier, whiter, and more silvery. Patients often notice that the scalp sheds visible flakes onto clothing or that plaque edges feel more defined than ordinary dandruff.
The itch of psoriasis can be intense, but the dominant visual cues often matter more. A psoriasis-scalp exam may reveal plaques that extend just beyond the hairline, thicker scale that clings to the scalp surface, and associated psoriasis signs elsewhere, such as nail pitting, plaques on elbows or knees, or lesions in the ears. Some people have scalp-predominant disease, which can make diagnosis less obvious, but trichoscopy still often reveals a helpful vascular pattern.
Features that make psoriasis more likely include:
- Thick white or silver-white scale
- Sharper plaque borders
- Bright red or pink inflammatory background
- Scale that feels layered or adherent
- Nail changes or psoriasis elsewhere on the body
- A history of recurrent plaques rather than mainly greasy flares
On trichoscopy, psoriasis often shows regularly distributed red dots, glomerular vessels, or twisted red loops. These vascular clues can be extremely useful because they help separate psoriasis from seb derm, which more often shows thinner arborizing vessels and a yellower, oilier scale pattern. This is one reason dermatologists often reach for trichoscopy early when a red, flaky scalp is not clearly one condition or the other.
Psoriasis can sometimes coexist with hair shedding, especially when inflammation is severe or scratching is persistent. Long-standing severe scalp psoriasis can also, in rare cases, be associated with scarring change. That is not the usual course, but it is one reason a very inflamed scalp should not be trivialized just because psoriasis is often classified as a non-scarring disorder.
One of the more confusing patterns is sebopsoriasis, where the scalp carries features of both seb derm and psoriasis. In that overlap zone, the scale may be too greasy for textbook psoriasis yet too persistent and plaque-like for straightforward seb derm. The treatment plan may also reflect that overlap, using both scale-lifting and anti-inflammatory or antifungal strategies.
Psoriasis also deserves extra consideration when scalp symptoms are accompanied by discomfort elsewhere. Joint pain, nail changes, or plaques on classic body sites strengthen the case. So does a family history. By contrast, isolated greasy itching that rises and falls with wash frequency leans more toward seb derm.
If hair loss becomes part of the picture, it helps to understand how scalp psoriasis can affect hair shedding without immediately assuming permanent follicle destruction. Psoriasis can definitely disrupt the hair environment, but the bigger diagnostic question is whether the follicle openings remain present and whether the scale is part of a broader plaque pattern rather than a targeted follicular attack.
Red flags for scarring alopecia
Perifollicular scaling becomes more concerning when the scalp stops behaving like a flaky inflammatory surface disorder and starts behaving like a follicular destruction process. That is the point where scarring alopecia enters the differential. Among the scarring causes, lichen planopilaris is one of the most important because perifollicular scaling is one of its most characteristic active features.
In scarring alopecia, the problem is not only scale. It is inflammation aimed at the follicle itself, especially the region responsible for regeneration. Over time, that inflammation can replace follicles with scar tissue. Once a follicle is truly scarred, meaningful regrowth is limited. That is why early recognition matters so much more here than it does with ordinary dandruff.
Signs that push perifollicular scaling into a higher-risk category include:
- Burning, stinging, pain, or tenderness
- Perifollicular redness around active hairs
- Patchy hair loss rather than only diffuse flaking
- Smooth or shiny areas
- Fewer visible follicular openings
- Hair loss at the edges of an active red, scaly patch
- Eyebrow loss or a changing frontal hairline in some variants
Lichen planopilaris is the classic example, but it is not the only scarring condition in the differential. Discoid lupus erythematosus, central centrifugal cicatricial alopecia, and other inflammatory cicatricial alopecias can also alter follicular openings and cause persistent scalp change. The exact pattern differs, which is why diagnosis should not be made from one symptom alone.
What makes scarring alopecia different from seb derm or routine psoriasis is the texture of progression. Patients often describe a sore scalp, burning, or tenderness rather than only itch. The patches may look less like broad flaky zones and more like irregular areas where the hair density is thinning and the skin begins to look smoother. On trichoscopy, the warning signs include absent follicular openings, perifollicular erythema, tubular casts, white scar-like areas, and other signs of follicular damage.
This is where a reader needs to slow down. Not every follicle-centered scale pattern is a scarring alopecia. But once follicular openings seem reduced or the scalp feels painful, the threshold for medical review should drop. It becomes much more important to think in terms of protecting follicles rather than simply controlling flakes.
For readers who want a deeper picture of the best-known example in this group, a focused lichen planopilaris overview can help explain why the same scale that looks minor in one patient can carry more urgency in another. The practical difference is permanence. Seb derm can be annoying and chronic. Active scarring alopecia can be chronic and cumulative.
A useful rule is this: itch and grease suggest common inflammatory scale; pain, follicular loss, and shiny patches suggest the need to rule out scarring disease quickly.
How dermatologists tell them apart
Dermatologists rarely diagnose perifollicular scaling from the scale alone. They build the answer from pattern, symptoms, trichoscopy, and sometimes biopsy. This layered approach matters because seb derm, psoriasis, and scarring alopecia can overlap enough that a quick glance may be misleading.
The first step is a careful history. The clinician will usually ask when the problem started, whether the main symptom is itch or pain, how fast it is changing, whether there is visible shedding or patchy thinning, and whether other body sites are involved. Red flaky eyebrows or beard areas support seb derm. Nail pitting or plaques elsewhere support psoriasis. Burning pain, scalp tenderness, or patchy scarring loss raise concern for lichen planopilaris or another cicatricial alopecia.
The next step is direct scalp examination. Doctors look for:
- The quality of the scale: greasy, dry, thick, thin, yellow, or silvery
- The distribution: diffuse, patchy, plaque-like, frontal, vertex, or perifollicular
- The presence or absence of follicular openings
- Signs of scratching, crusting, pustules, or product irritation
- Hair density changes and whether the scalp surface appears smooth
Trichoscopy is often the turning point. This magnified scalp exam can show details that are easy to miss with the naked eye. In psoriasis, regularly distributed red dots or twisted loops often stand out. In seb derm, thin arborizing vessels and yellowish-white scale are more typical. In lichen planopilaris, perifollicular scale with erythema, tubular casts, and loss of follicular openings can point toward active scarring alopecia.
Biopsy becomes more important when the diagnosis remains uncertain or when scarring alopecia is suspected. A biopsy is usually taken from an active edge rather than a fully smooth scarred center, because the active border is more likely to capture the inflammatory process that explains the disease. If you are wondering what that test can clarify, what a scalp biopsy can show often includes whether follicles are being scarred, what type of inflammatory infiltrate is present, and whether the process is more compatible with lupus, lichen planopilaris, or another diagnosis.
The diagnostic sequence often works like this:
- Identify the scale pattern and symptom profile.
- Look for clues elsewhere on the skin, nails, brows, or face.
- Use trichoscopy to examine vessels, scale distribution, and follicular openings.
- Reserve biopsy for doubtful cases or suspected scarring disease.
One original but useful way to frame it is that diagnosis moves from surface clues to follicular clues. Seb derm and psoriasis often declare themselves at the surface first. Scarring alopecia often declares itself at the follicle.
This is also why repeated self-treatment can muddy the picture. Strong steroids, exfoliants, oils, and medicated shampoos may partially suppress scale without resolving the underlying diagnosis. By the time a patient is finally examined, the scalp may look altered but not clarified. That is another reason persistent perifollicular scaling deserves assessment before months of trial-and-error blur the pattern.
What to do next and when to seek care
If you notice perifollicular scaling, the next step is not to panic. It is to assess the company it keeps. A mildly itchy oily scalp that improves with anti-dandruff shampoo sits in a very different category from a sore scalp with follicular redness and patchy hair loss. The safest and most useful response is to match urgency to the rest of the picture.
A reasonable self-check includes these questions:
- Is the main symptom itch, or is there pain and burning too?
- Is the scale greasy and diffuse, or thick and sharply plaque-like?
- Are you seeing increased shedding or actual patchy thinning?
- Do the follicles still look visible, or does the scalp appear smoother in spots?
- Are the eyebrows, beard, ears, or nails involved?
- Have you already tried a sensible treatment plan for several weeks without improvement?
If the pattern looks more like simple seb derm, first-line care often means more consistent washing and evidence-based medicated shampoos rather than endless product rotation. If it looks more psoriatic, especially with plaque-like scale or body signs, evaluation is worthwhile because scalp psoriasis often needs a more targeted plan. If pain, tenderness, smooth patches, or disappearing follicular openings are present, the priority is ruling out scarring alopecia.
What should you avoid while sorting it out?
- Picking at follicle-centered scale
- Scratching until the scalp becomes raw
- Repeated harsh exfoliation
- Heavy oils on an inflamed scalp
- Frequent product switching that makes the scalp harder to read
- Assuming all flakes are dandruff
It also helps to document the scalp with photos in consistent lighting. This is especially useful when you are trying to determine whether there is true progression or just day-to-day fluctuation in scale. Photos can reveal whether a red patch is enlarging, whether density is changing, and whether a hairline or crown is shifting over time.
Seek medical care sooner rather than later if there is tenderness, burning, patchy loss, eyebrow thinning, scalp pain, or areas that look smooth and shiny. Those signs move perifollicular scaling out of the “annoying” category and closer to the “protect follicles now” category. The same is true if ordinary dandruff products have failed and the scalp keeps returning to the same inflamed state.
For people trying to decide whether the situation has crossed that line, guidance on when hair loss needs a dermatologist becomes especially relevant when scale is centered around follicles rather than scattered loosely on the surface.
The bottom line is that perifollicular scaling is worth respecting. Sometimes it points to seb derm. Sometimes it points to psoriasis. And sometimes it is one of the earliest visible signs that the follicle itself is under threat. The difference is not in the word “scale.” It is in the pattern around it.
References
- A comprehensive literature review and an international expert consensus on the management of scalp seborrheic dermatitis in adults 2024 (Expert Consensus)
- Differential diagnosis of red scalp: the importance of trichoscopy 2024 (Review)
- Clinical and trichoscopic features in various forms of scalp psoriasis 2021 (Clinical Study)
- Trichoscopic Features of Lichen Planopilaris versus Frontal Fibrosing Alopecia: A Systematic Review 2025 (Systematic Review)
- A Practical Approach to the Diagnosis and Management of Classic Lichen Planopilaris 2021 (Review)
Disclaimer
This article is for educational purposes only and is not a diagnosis or a substitute for care from a dermatologist or other qualified clinician. Perifollicular scaling can occur in common inflammatory scalp conditions, but it can also be a sign of disease affecting the hair follicle more directly. Prompt medical assessment is important when scaling is accompanied by pain, burning, patchy hair loss, eyebrow loss, or smooth areas that suggest scarring.
If this article helped you, please share it on Facebook, X, or another platform you prefer so others can find clear guidance on perifollicular scaling and its most important causes.






