Platelet-rich plasma, or PRP, has become one of the most requested in-office hair treatments, yet it is also one of the most misunderstood. Many people arrive at a consultation hoping for a dramatic reversal of thinning after a few injections. Others assume it is little more than expensive hype. The truth sits in the middle. PRP can help certain patients, especially those with pattern thinning and still-active follicles, but it is not a cure, and it does not bring back hair in areas where follicles are no longer functioning. Its appeal is easy to understand: the treatment uses a concentrate made from your own blood, is minimally invasive, and can fit alongside medical therapy rather than replace it. What matters most is knowing what kind of improvement is realistic, how long it takes to see it, and which scalp patterns respond best. When you understand those details, PRP becomes easier to judge clearly and much harder to oversell.
Quick Overview
- PRP tends to improve hair density and reduce shedding more than it restores a fully bald area.
- The best candidates usually have early to moderate pattern thinning and follicles that are still producing fine or miniaturized hairs.
- Results are gradual and are often judged over 3 to 6 months rather than after a single session.
- Benefits vary because PRP preparation methods and treatment schedules are not yet fully standardized.
- A common starting plan is 3 to 4 sessions spaced about a month apart, followed by maintenance only if you are clearly improving.
Table of Contents
- How PRP works in the scalp
- What results usually look like
- Who benefits most from PRP
- Who should skip or reconsider PRP
- How many sessions and when
- PRP versus minoxidil finasteride and microneedling
How PRP works in the scalp
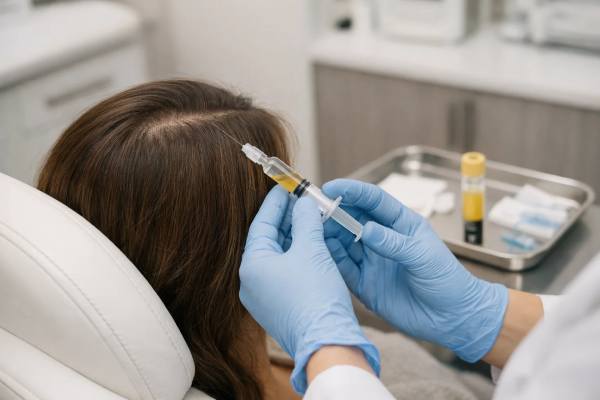
PRP is made by drawing a small amount of your blood, spinning it to concentrate platelets, and injecting that platelet-rich portion into areas of thinning on the scalp. Platelets are best known for helping blood clot, but they also release signaling proteins involved in repair, inflammation control, and tissue remodeling. In hair medicine, the idea is not that PRP creates brand-new follicles. The more realistic goal is that it helps weakened follicles function better, stay in growth mode longer, and produce stronger hairs than they were producing before.
That distinction matters. PRP works best when follicles are still alive but underperforming. In pattern hair loss, follicles often shrink over time and start producing finer, shorter hairs. PRP appears most useful during that stage, when the follicle is miniaturized rather than gone. Once an area has become smooth, shiny, and truly bare for a long time, there may not be enough viable follicular activity left for injections to do much. This is one reason people with early crown thinning or widening of the part often respond better than people hoping to refill an advanced, long-bald frontal scalp.
PRP also fits logically with the biology of the hair growth cycle. Hair does not grow continuously. Each follicle moves through growth, transition, rest, and shedding phases. PRP is thought to support a shift toward longer time in the active growth phase, which can translate into better density over time. That helps explain why results are gradual. A follicle has to respond, re-enter productive growth, and then grow a visible fiber. None of that happens overnight.
The evidence is strongest for androgenetic alopecia, also called male or female pattern hair loss. That is where most trials, reviews, and real-world treatment protocols are focused. PRP has also been studied in other hair disorders, but the data are far more mixed, and in some conditions standard medical therapy remains more dependable. Another key point is that PRP is not one perfectly standardized product. Platelet concentration, activation method, spin technique, injection depth, and session spacing vary across clinics and studies. That lack of uniformity helps explain why one patient may report impressive thickening while another sees only modest change. In other words, PRP is a real treatment, but it is also a variable one. The concept is biologically plausible and supported by growing evidence, yet the exact dose and protocol that work best are still being refined.
What results usually look like
The most honest way to describe PRP results is this: they are usually visible as improvement, not transformation. Patients who respond often notice that shedding slows first. Hair may feel less fragile in the shower or on the brush before it looks dramatically fuller in the mirror. After that, the more meaningful changes tend to be a denser-looking part, a little more coverage at the crown, better blending of thin zones into thicker zones, and a stronger overall “fill” to the hair. What PRP does not usually do is turn a slick bald patch into a full head of dense hair.
Studies most often show improvement in hair density rather than dramatic jumps in shaft thickness. In practical terms, that means you may gain more visible coverage because more hairs are active or surviving, even if each single strand does not become dramatically thicker. In pooled research, average gains are often in the range of modest but real increases in hairs per square centimeter rather than a complete reset to baseline density from years earlier. That is exactly why standardized photographs, trichoscopy, or hair counts matter. Patients often evaluate progress emotionally and only from memory, which can distort the picture. The better approach is to compare the same area, under the same lighting, at the same angle, every few months.
The timeline also matters. Most patients will not know much after one treatment. Meaningful change is usually judged after a series, often around the 3- to 6-month mark. Some data suggest combination treatment with minoxidil can improve density more than minoxidil alone within that time window, but the certainty of that evidence is still limited. That does not mean the effect is imaginary. It means clinics should be careful not to promise a level of precision that the literature does not support.
A helpful way to think about response is in layers:
- Early response may look like less shedding and slightly better texture.
- Mid-course response may look like reduced scalp show-through at the part or crown.
- Stronger response may include visibly fuller styling and better photographic coverage.
- Poor response may mean little change despite correct treatment intervals.
This is also why expectations differ by pattern. A person with diffuse thinning across the mid-scalp may see a satisfying cosmetic improvement because small density gains spread across a broad area can look meaningful. Someone with deep temple recession or a long-standing bare crown may be disappointed because PRP does not reliably rebuild advanced loss. The treatment is best at improving what is still there. It is not best at replacing what is already gone. That single idea explains most of the success stories and most of the letdowns.
Who benefits most from PRP
The people who tend to benefit most from PRP usually share a few traits. First, they still have active follicles in the treatment area. Second, their hair loss pattern is one that PRP has been studied for most often, especially androgenetic alopecia. Third, they have expectations centered on improvement in density and maintenance, not a miracle reversal. When those pieces line up, PRP is often easier to justify.
In men, some of the best candidates are those with early to moderate thinning at the crown, mid-scalp, or frontal forelock rather than completely bare zones. These are often the same patients who are also weighing broader male pattern thinning options and want to add a procedure-based treatment without jumping straight to surgery. In women, PRP may be particularly useful for diffuse central thinning, widening of the part, and early female pattern hair loss where follicles are clearly weakened but still present. Because women often lose density in a more diffuse pattern rather than a sharply defined bald patch, even modest improvement can make the scalp look less exposed.
PRP also makes sense for patients who want an adjunct, not a replacement. Someone already using minoxidil or taking an appropriate medical therapy may use PRP to push for better density, slower shedding, or improved maintenance. Evidence increasingly suggests that multimodal treatment can outperform one standalone approach, even if the exact size of that advantage varies from study to study. Patients who do well are often the ones willing to treat PRP as part of a plan rather than as a single heroic intervention.
Other features can tilt the odds in a better direction:
- Earlier-stage thinning rather than very advanced loss.
- Noticeable miniaturized hairs rather than long-standing smooth baldness.
- A stable scalp without heavy inflammation, infection, or scarring.
- Willingness to complete an initial series instead of judging the treatment after one visit.
- Comfort with maintenance treatments if the first phase works.
Age may matter, but not in a simple yes-or-no way. Some recent clinical data suggest younger patients may trend toward better density gains, while older patients may need more sessions to reach a similar effect. That does not mean older adults cannot benefit. It means the pace and size of improvement may differ, and counseling should reflect that reality. The same is true for baseline hair caliber. If the follicles are still producing visible, although weaker, hairs, PRP has something to work with. If the area has progressed too far, the ceiling gets much lower.
The best candidate, then, is not the person with the most hair loss. It is the person with the most salvageable hair. That is an important difference, and it is one of the main reasons good consultations focus on scalp findings, not just patient frustration.
Who should skip or reconsider PRP
PRP is often marketed as broadly suitable because it uses your own blood, but that can create a false sense that almost anyone with thinning is a good candidate. In reality, there are several situations where PRP is less likely to help, should be postponed, or needs more careful medical review before going ahead.
The clearest poor candidates are people with long-standing, smooth bald areas where follicles are likely no longer active. PRP may still be offered in these settings, but the expected payoff is low. The same caution applies to certain scarring alopecias, where inflammation destroys the follicle and replacement tissue forms. In those cases, management is usually centered on diagnosis and disease control first, not cosmetic stimulation alone. Patients with untreated rapid shedding also need a pause rather than an injection reflex. If the true driver is iron deficiency, thyroid disease, recent weight loss, illness, medication change, or severe stress, PRP may distract from the real cause instead of addressing it.
The scalp itself matters too. A calm, intact surface gives any regenerative treatment a better chance. If the scalp is inflamed, painful, infected, or covered in active dermatitis, it is wiser to stabilize that first and improve the follicle environment before considering injections. Tenderness, burning, pustules, or scaly active plaques should not be brushed aside as minor details during a cosmetic consult.
There are also practical reasons to reconsider PRP:
- You cannot commit to the initial series and only want one session.
- You are unwilling to use other evidence-based treatments when they are appropriate.
- You expect PRP to restore a dense juvenile hairline.
- You have severe needle anxiety or low tolerance for repeated scalp injections.
- You are taking medications or have platelet or bleeding issues that require physician review.
Side effects are usually mild, but they are not nonexistent. Temporary pain, scalp tenderness, pinpoint bleeding, mild swelling, tightness, and short-lived headache are common enough that patients should hear about them plainly. Serious complications are uncommon when the procedure is done correctly, but technique still matters. This is one reason PRP should not be chosen purely by marketing language, package pricing, or social media photos.
Pregnancy is another situation where clinics often become more conservative. Because PRP for hair loss is elective, many providers prefer to defer until after pregnancy even though the material is autologous. That kind of caution is reasonable. The same applies when hair loss is clearly unstable or the diagnosis is uncertain. In those settings, the smarter move is often better evaluation, not faster treatment. PRP tends to disappoint most when it is used to avoid diagnosis, avoid realistic counseling, or avoid the harder discussion that a different therapy may be better suited to the pattern in front of you.
How many sessions and when
One of the biggest reasons PRP gets misjudged is timing. Patients often expect a straight line from first injection to visible regrowth, but hair biology does not work that way. Most clinics use a loading phase first, then a maintenance phase only if there is a clear response. A common starting plan is three monthly sessions or three to four sessions spaced roughly every 2 to 4 weeks. That structure matches much of the published literature, even though protocols still vary from study to study.
The goal of the first phase is not to deliver a miracle at session one. It is to create enough repeated stimulation for a fair trial. By the end of that initial series, some patients notice less shedding or a slightly healthier feel to the hair. More visible density changes are often judged later, typically by the 3- to 6-month mark. If there is clear improvement, maintenance may then be offered every few months, sometimes every 3 to 6 months, and in some settings even less often once results stabilize. Age, baseline thinning, concurrent medical therapy, and how quickly the benefit fades can all influence that schedule.
A more useful question than “How many sessions does PRP require?” is “When should I decide whether it is working?” The answer is usually after the loading phase plus enough time for the hair cycle to show it. In practice, that means you need both treatments and patience. Judging PRP after one month is usually too early. Judging it after a full series with standardized photos is much more reasonable.
A good treatment plan also avoids chaos. If you start PRP, stop minoxidil, begin supplements, switch shampoos, and change your styling routine all in the same two weeks, it becomes difficult to know what is helping or hurting. Patients often do better when the rest of the regimen is kept stable. If you are already using topical therapy, maintaining a consistent minoxidil routine makes response easier to interpret than repeatedly stopping and restarting.
Before beginning, ask how progress will be measured. The strongest clinics do not rely only on casual mirror impressions. They use:
- Baseline photos with consistent lighting and part placement.
- A clearly defined treatment area.
- Follow-up images at set intervals.
- Objective counts or trichoscopy when available.
- A stated reassessment point.
That structure helps prevent two common problems: continuing ineffective sessions for too long, and quitting a potentially useful treatment too early. PRP works best when it is treated like a monitored medical procedure, not a beauty service bought in bundles and judged by hope alone.
PRP versus minoxidil finasteride and microneedling
PRP often enters the conversation when patients are deciding whether they want a procedure, a home treatment, a prescription, or some combination of the three. The answer depends less on trendiness than on mechanism, convenience, tolerance, and stage of hair loss.
Minoxidil remains one of the most practical first-line tools because it is noninvasive, accessible, and backed by years of use. It is especially useful when patients are willing to apply it consistently and accept that stopping usually means losing the benefit. PRP differs in a few important ways: it is office-based, involves injections, and does not require daily application, but it costs more and depends heavily on clinic technique. For some patients, that trade-off is appealing. For others, it makes far less sense than simply using a strong home regimen well.
Finasteride addresses a different part of the problem. In androgen-driven hair loss, it targets the hormonal pathway that causes progressive follicle miniaturization. That means it often plays a stronger role in maintenance of male pattern loss than PRP alone, because it addresses the disease mechanism more directly. PRP can still be useful, but often as an adjunct rather than a substitute. Patients who refuse every medical option and place all hope on PRP are sometimes setting themselves up for a softer result than they expect.
Microneedling occupies a middle space. It is procedure-based like PRP, but it works through controlled injury and remodeling rather than platelet concentrate alone. Some data suggest combination approaches may perform better than monotherapy, and PRP paired with minoxidil or microneedling can produce better density outcomes than a single treatment in selected patients. That said, the studies are heterogeneous, and not every combination result is equally strong. The broad pattern is encouraging, but the exact size of benefit is still hard to pin down because protocols differ so much.
For advanced loss, the comparison changes again. PRP is not a replacement for hair transplantation when the problem is simply lack of enough functioning follicles. In that setting, patients exploring transplant candidacy and recovery are often asking a better question than patients trying to force PRP into a job it cannot reliably do. PRP may still have a role around the edges of treatment plans, but it is not the same category of solution.
A practical way to compare the main options is this:
- Minoxidil is convenient and evidence-based, but requires consistency.
- Finasteride targets androgen-driven progression more directly, but is not suitable for everyone.
- PRP can improve density and shedding in the right candidate, but requires office sessions and realistic goals.
- Microneedling may add benefit, especially in combination plans, but also requires structure and technique.
The best plan is often not choosing one camp forever. It is choosing the combination that fits the diagnosis, the stage of thinning, and the kind of maintenance you can actually sustain.
References
- The role of platelet-rich plasma in androgenetic alopecia: A systematic review 2024 (Systematic Review)
- Effectiveness of platelet‐rich plasma in treating female hair loss: A systematic review and meta‐analysis of randomized controlled trials 2024 (Systematic Review)
- The additive value of platelet-rich plasma to topical Minoxidil in the treatment of androgenetic alopecia: A systematic review and meta-analysis 2024 (Systematic Review)
- Treatment of Androgenetic Alopecia: Current Guidance and Unmet Needs 2023 (Review)
- Impact of Age on Response to Platelet-Rich Plasma Therapy 2025
Disclaimer
This article is for educational purposes only and is not a substitute for medical advice, diagnosis, or treatment. PRP for hair loss should be considered only after an appropriate evaluation of the cause and pattern of thinning. A dermatologist or qualified hair-loss specialist should assess rapid shedding, scalp pain, inflammation, patchy loss, scarring signs, or long-standing progression before any procedure is started.
If you found this article useful, please consider sharing it on Facebook, X, or another platform that helps others find reliable hair and scalp health information.






