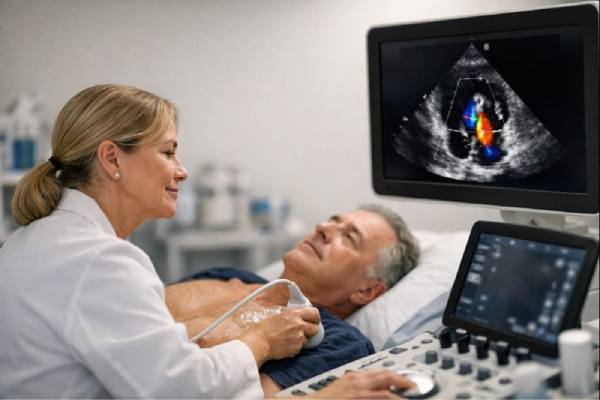
Insufficiency of the tricuspid valve—often called tricuspid regurgitation (blood leaks backward)—means the valve between the right upper and right lower chambers of the heart does not close tightly. When this happens, part of each heartbeat flows the wrong way, raising pressure in nearby veins and making the right side of the heart work harder.
Many people live for years with mild leakage and feel perfectly well. The condition becomes important when the leak is moderate-to-severe, because it can quietly enlarge the right side of the heart, reduce exercise capacity, and cause swelling, abdominal fullness, or rhythm problems. The most helpful mindset is “track trends, not just symptoms.” With modern ultrasound, MRI, and catheter-based repair options, clinicians can often treat the cause, protect the right heart, and improve quality of life—especially when care happens before advanced right-heart strain develops.
Table of Contents
- What it is and why it matters
- Causes and risk factors
- Symptoms and complications
- How it’s diagnosed
- Treatment options and what to expect
- Management, prevention, and when to seek care
What it is and why it matters
The tricuspid valve sits between the right atrium (upper chamber) and right ventricle (lower chamber). Its job is simple: open to let blood move forward, then close so blood does not leak backward when the ventricle pumps blood toward the lungs. In tricuspid valve insufficiency, the valve leaflets do not seal well, and blood slips back into the right atrium with each contraction.
What makes this condition unique is that it often reflects a bigger “right-sided” story. Many cases are functional, meaning the valve leaflets are not primarily damaged. Instead, the right ventricle or the valve ring stretches, pulling the leaflets apart like a doorframe that has widened. This is why tricuspid regurgitation commonly accompanies conditions that enlarge or strain the right ventricle—such as pulmonary hypertension, left-sided valve disease, or longstanding atrial fibrillation.
Over time, significant leakage can create a loop of worsening strain:
- The right ventricle handles extra volume each beat and gradually enlarges.
- Enlargement can worsen the leak, because the valve ring stretches further.
- Pressure backs up into veins, affecting the legs, liver, and abdomen.
- The right atrium may enlarge, raising the likelihood of rhythm problems.
A practical “why it matters” point: symptoms often appear late. Many people adapt slowly—walking a bit less, taking elevators, resting more—without realizing that the heart is compensating. Clinicians therefore pay close attention to objective markers such as right ventricular size and function, liver congestion, kidney function, and exercise testing results. In other words, the valve leak is not just a sound on a stethoscope; it can be a signal that the right side of the heart is being asked to do more than it can sustain long-term.
Another reason it matters is that treatment options have expanded. For years, many patients were managed only with diuretics because surgery was considered high risk, especially when tricuspid disease was “secondary.” Today, earlier referral to valve teams and less invasive catheter-based repairs are changing what is possible—particularly for people with severe symptoms who are not good candidates for open-heart surgery.
Causes and risk factors
Tricuspid valve insufficiency can be grouped into two broad categories: primary (the valve tissue itself is abnormal) and secondary/functional (the valve leaks because surrounding chambers or pressures distort it). Secondary causes are more common.
Common functional causes
- Right ventricular enlargement or pressure overload: Anything that increases pressure in the lung circulation (pulmonary hypertension) can enlarge the right ventricle and stretch the valve ring.
- Left-sided heart disease: Mitral or aortic valve problems and left-sided heart failure can raise pressures that eventually affect the right heart.
- Atrial fibrillation and atrial enlargement: In some people, the right atrium stretches enough to widen the tricuspid ring even without major right ventricular failure, producing “atrial functional” tricuspid regurgitation.
- Pacemaker or defibrillator leads: A lead crossing the tricuspid valve can interfere with leaflet closure or contribute to scarring and malcoaptation over time.
Primary (structural) causes
- Infective endocarditis: Infection can destroy leaflet tissue. Risk increases with intravenous drug use, long-term vascular access, and certain congenital heart conditions.
- Congenital valve disorders: Examples include Ebstein anomaly (a malformation of the tricuspid valve and right ventricle).
- Rheumatic disease: Less common for the tricuspid valve than for other valves, but possible.
- Trauma or injury: Rarely, blunt chest trauma can damage the valve.
- Carcinoid heart disease or infiltrative processes: These can cause stiff, retracted leaflets.
Risk factors for progression and symptoms
Two people can have a similar “grade” of leakage and feel very different. Factors that often predict faster progression or higher symptom burden include:
- Pulmonary hypertension (especially if longstanding).
- Chronic atrial fibrillation with enlarging atria.
- Coexisting valve disease (mitral regurgitation, aortic stenosis) or reduced left ventricular function.
- Kidney disease or liver congestion, which lowers tolerance for fluid shifts.
- Older age and frailty, which reduce physiologic reserve.
- Delayed diagnosis, because gradual limitation can be mistaken for “getting older.”
A useful clinical insight: many patients do not present because of shortness of breath first; they present because of swelling, abdominal bloating, early satiety, or repeated “fluid overload” episodes. Those symptoms reflect venous congestion—often the most direct downstream effect of a severely leaking tricuspid valve.
Symptoms and complications
Mild tricuspid regurgitation is common and often harmless. Symptoms typically appear when the leak becomes moderate-to-severe or when the underlying cause (like pulmonary hypertension or heart failure) worsens. Because the right side of the heart works at lower pressures than the left, the condition can smolder quietly for years.
Early symptoms (easy to overlook)
- Reduced stamina: You tire sooner on hills, stairs, or long walks.
- Breathlessness with sustained activity: Not necessarily sudden or dramatic—more like “I can’t keep up.”
- A sense of heaviness or fullness: Especially after meals or later in the day.
Congestion-focused symptoms (often the turning point)
As pressure backs up into the venous system, symptoms become more specific:
- Leg and ankle swelling that worsens by evening.
- Abdominal bloating or discomfort, sometimes with nausea or poor appetite.
- Rapid weight gain over days from fluid retention.
- Nocturia (urinating more at night) due to daytime fluid shifting back into circulation when lying down.
Rhythm and perfusion symptoms
Right atrial enlargement and strain can contribute to arrhythmias. People may notice:
- Palpitations (fluttering, racing, or irregular beats).
- Lightheadedness during episodes.
- Exercise intolerance out of proportion to lung findings.
Complications clinicians monitor
- Right ventricular dilation and dysfunction: The central complication. Once the right ventricle loses strength, recovery after intervention may be less complete.
- Worsening atrial fibrillation or flutter: Enlarged atria make rhythm stability harder.
- Liver congestion and injury: Chronic venous pressure can enlarge the liver and elevate liver enzymes; in advanced cases it can contribute to scarring.
- Kidney impairment: Congestion and reduced forward flow can lower kidney perfusion and make diuretic management challenging.
- Thromboembolism risk: Often tied to atrial fibrillation rather than the valve leak itself, but it matters because it changes medication decisions.
Symptoms that deserve urgent attention
Seek prompt medical evaluation if you develop:
- Fainting, chest pain, or severe breathlessness at rest.
- A fast, sustained heartbeat with dizziness or near-fainting.
- Fever plus new heart symptoms in someone with a device lead or prior valve disease.
- Rapidly worsening swelling or sudden marked abdominal distension.
A practical rule: if your shoes suddenly do not fit, your appetite drops because you feel “full,” or your walking range shrinks over a few weeks, it’s worth reassessing—even if you have lived with a murmur for years.
How it’s diagnosed
Diagnosis is a combination of clinical clues and imaging. The goal is not only to confirm a leaky valve, but to understand why it is leaking and what it is doing to the right heart, veins, liver, and lungs.
History and physical examination
Clinicians ask targeted questions about swelling patterns, abdominal fullness, exercise capacity, sleep position, palpitations, and prior heart procedures (including pacemakers/defibrillators). On exam, they may look for:
- Neck vein distension (a visible sign of higher venous pressure).
- A pulsatile liver or tenderness from congestion.
- Leg edema and sometimes fluid in the abdomen.
- A heart murmur that may intensify with inhalation (a helpful clue for right-sided murmurs), though murmur intensity does not reliably measure severity.
First-line testing
- Transthoracic echocardiogram (TTE): The cornerstone test. It estimates regurgitation severity, evaluates valve anatomy, measures right ventricular size/function, and assesses pulmonary pressures and other valves.
- Electrocardiogram (ECG): Looks for atrial fibrillation, conduction delays, or right-sided strain patterns.
- Basic labs: Often include kidney function, liver enzymes, electrolytes, and sometimes natriuretic peptides to help assess congestion and heart strain.
Advanced evaluation (when detail matters)
- Transesophageal echocardiogram (TEE): Provides sharper images when TTE windows are limited and is often used when planning interventions.
- Cardiac MRI: Especially useful to quantify right ventricular volumes and function with high accuracy, and to track changes over time.
- Right-heart catheterization: Measures pressures directly when pulmonary hypertension is suspected or when symptoms do not match noninvasive findings.
- Exercise testing: A treadmill or cardiopulmonary exercise test can reveal hidden limitation and provide objective baselines.
How “severity” is interpreted in practice
Clinicians typically integrate multiple domains rather than relying on one measurement:
- Imaging-based severity (mild, moderate, severe; some centers also recognize “massive” or “torrential” categories for advanced cases).
- Right ventricular size and function trends.
- Degree of venous congestion (clinical and lab markers).
- Rhythm status (especially atrial fibrillation burden).
- The root cause (functional vs primary; device lead involvement; pulmonary hypertension).
An important, patient-centered point: diagnosis is not just “you have a leaky valve.” The real question is whether the leak is driving right-heart remodeling and congestion—and whether treating the cause or the valve would change your daily life and long-term risk.
Treatment options and what to expect
Treatment depends on three things: the cause of the leak, the severity, and the condition of the right ventricle. For many people, the earliest and most effective “treatment” is addressing the driver—such as pulmonary hypertension, atrial fibrillation, left-sided valve disease, or device lead issues—before the right ventricle becomes significantly weakened.
Medical management (symptom control and stabilization)
Medications do not “seal” the valve, but they can reduce the consequences:
- Diuretics help remove excess fluid and ease swelling and abdominal congestion. Many patients do best with a structured plan (daily weights, a target weight range, and clear instructions for when to adjust doses).
- Treating atrial fibrillation (rate or rhythm control) can reduce symptoms and limit atrial enlargement in some cases.
- Managing pulmonary hypertension (when present) may reduce right ventricular strain.
- Optimizing left-sided heart disease can lower downstream pressures that worsen tricuspid leakage.
Medical therapy is often the first step, but it can become a “treadmill” if the underlying valve leak is severe—higher diuretic doses may be needed over time, and kidney function can limit how aggressively fluid can be removed.
Procedural and surgical options
- Tricuspid valve repair (surgical):
Often preferred over replacement when feasible, especially in functional regurgitation. Repair commonly involves tightening the valve ring (annuloplasty) and addressing leaflet tethering. - Tricuspid valve replacement (surgical):
Considered when repair is unlikely to be durable or when valve tissue is significantly damaged (for example, from endocarditis). Choice of prosthesis depends on age, bleeding risk, and comorbidities. - Transcatheter (minimally invasive) interventions:
These have expanded rapidly and may include:
- Edge-to-edge repair (clipping leaflets to improve closure) for selected anatomies.
- Annuloplasty devices to reduce ring size.
- Valve replacement approaches in carefully chosen cases or trial settings, depending on anatomy and availability.
When is intervention considered?
Teams typically look for a combination of:
- Severe regurgitation and meaningful symptoms (fatigue, swelling, reduced walking distance).
- Evidence of progressive right ventricular enlargement or declining function.
- Recurrent heart-failure admissions or escalating diuretic needs.
- Significant liver congestion, worsening kidney function related to congestion, or difficult-to-control atrial fibrillation.
- The opportunity to treat the tricuspid valve while addressing another valve surgically (a common, important scenario).
What outcomes to expect
Many patients experience:
- Improved swelling and abdominal comfort within weeks when congestion decreases.
- Better stamina over months as forward flow improves and rhythm stabilizes.
- Ongoing need for follow-up, because right-heart conditions can persist and device-based repairs may require surveillance.
A useful way to think about success: the goal is often fewer “fluid crises,” less daily limitation, and protecting the right ventricle—sometimes even more than achieving a perfect-looking valve on imaging.
Management, prevention, and when to seek care
Living well with tricuspid valve insufficiency is about controlling congestion, supporting the right heart, and watching for changes early enough to act. Many patients do best with a simple, repeatable routine that reduces guesswork.
Daily habits that make a real difference
- Track weight and swelling patterns: Weigh yourself at the same time each morning. A short trend (for example, several pounds gained over a few days) often matters more than any single number.
- Follow a practical sodium plan: You do not need perfection, but consistent moderation helps diuretics work better. Processed foods and restaurant meals are the most common “hidden sodium” sources.
- Balance fluids thoughtfully: Your clinician may recommend a fluid goal if you retain fluid easily. The aim is steady intake—not big swings.
- Move daily within your safe range: Gentle aerobic activity (walking, cycling, water exercise) supports circulation and conditioning. If you become dizzy, markedly breathless, or unusually fatigued, scale down and report the change.
- Protect sleep and treat anemia: Poor sleep and low iron can amplify fatigue and shortness of breath, making heart symptoms feel worse than the valve alone would predict.
Preventing common setbacks
- Medication consistency: Missing diuretics or heart rhythm medications often leads to a predictable spiral: fluid retention, worse sleep, less activity, then more congestion.
- Vaccinations and infection prevention: Respiratory infections can destabilize heart failure symptoms. Keep routine vaccines up to date per local guidance.
- Device awareness: If you have a pacemaker/defibrillator, report new palpitations or changes in exercise tolerance. Lead-related valve issues may be subtle and benefit from specialist review.
Follow-up planning (what “good monitoring” looks like)
Many clinicians tailor follow-up to severity:
- Mild disease may need periodic reassessment only.
- Moderate-to-severe disease often warrants regular imaging, lab monitoring (kidney/liver), and rhythm evaluation, especially if symptoms or diuretic needs are changing.
A helpful self-advocacy tip: ask what your “watch markers” are—right ventricular size/function, pulmonary pressures, liver tests, arrhythmia burden—and what change would trigger a new plan.
When to contact a clinician promptly
Reach out within days if you notice:
- Increasing leg swelling, abdominal bloating, or reduced appetite.
- Rapid weight gain or needing higher diuretic doses to stay comfortable.
- New palpitations, irregular heartbeat, or reduced walking tolerance.
- New confusion, marked fatigue, or reduced urination (possible signs of worsening perfusion or kidney stress).
Seek urgent care for:
- Fainting, severe breathlessness at rest, chest pain, or a sustained racing heart with dizziness.
- Fever with chills plus new heart symptoms, especially in people with device leads or prior endocarditis history.
The overall goal is simple: keep the right heart from being silently overworked. With consistent monitoring and timely referral to a valve team when severity increases, many patients avoid repeated hospitalizations and maintain a stable, active life.
References
- 2025 ESC/EACTS Guidelines for the management of valvular heart disease 2025 (Guideline)
- 2020 ACC/AHA Guideline for the Management of Patients With Valvular Heart Disease: A Report of the American College of Cardiology/American Heart Association Joint Committee on Clinical Practice Guidelines 2021 (Guideline)
- Two-Year Outcomes of Transcatheter Edge-to-Edge Repair for Severe Tricuspid Regurgitation: The TRILUMINATE Pivotal Randomized Controlled Trial 2025 (RCT)
- Tricuspid Regurgitation: A Review of Current Interventional and Medical Management 2024 (Review)
Disclaimer
This article is for educational purposes only and does not provide medical advice, diagnosis, or treatment. Tricuspid valve insufficiency can range from mild and stable to severe and life-altering, depending on the cause, the degree of leakage, and the condition of the right side of the heart. If you have worsening swelling, shortness of breath, fainting, chest pain, a sustained rapid heartbeat, or fever with new heart symptoms—especially if you have a cardiac device or known valve disease—seek medical care promptly. Decisions about medications, activity level, imaging frequency, and whether to pursue surgical or transcatheter intervention should be made with a qualified clinician who knows your history and test results.
If you found this guide helpful, please share it on Facebook, X (formerly Twitter), or any platform you prefer, and follow us on social media. Your support through sharing helps our team continue producing high-quality health content.






