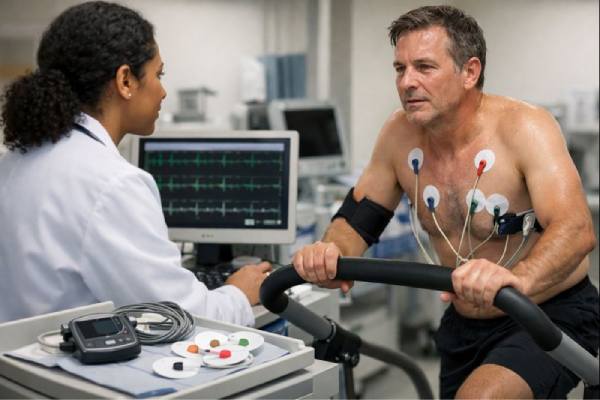
Exercise is supposed to make the heart stronger and steadier. But in some people, physical effort can uncover a rhythm problem—or briefly push a normal rhythm into an abnormal one. Exercise-induced arrhythmia means an irregular heartbeat that starts, worsens, or becomes noticeable during activity or recovery. It can feel like fluttering, pounding, skipped beats, or sudden racing, and it may happen in both athletes and non-athletes.
Most episodes are harmless and related to dehydration, stimulants, poor sleep, or stress. Still, a smaller group signals an underlying heart condition that needs careful evaluation—especially when symptoms include chest pain, fainting, or shortness of breath out of proportion to effort. This guide explains what exercise-induced arrhythmia is, what triggers it, how clinicians diagnose it, and how treatment and safe return to exercise are planned.
Table of Contents
- What exercise-induced arrhythmia means
- Why exercise can trigger rhythm changes
- Who is at higher risk
- Symptoms, red flags, and complications
- How doctors diagnose it
- Treatment and return to exercise
What exercise-induced arrhythmia means
An arrhythmia is any heartbeat that is too fast, too slow, or irregular. When it is “exercise-induced,” it appears during exertion (walking uphill, lifting, running, cycling) or in the minutes after stopping—an important window because some rhythm issues show up in recovery rather than at peak effort.
Not all exercise-related palpitations are dangerous. Many people experience occasional extra beats, especially when they are tired, dehydrated, or anxious. Others notice a “thump” after a skipped beat. These can be benign, but context matters: the same sensation can also come from rhythms that deserve treatment.
Common rhythm patterns linked with exercise include:
- Sinus tachycardia: a normal increase in heart rate with effort, sometimes felt as pounding.
- Premature beats: early beats from the atria or ventricles that can feel like flutters or “skips.”
- Supraventricular tachycardia (SVT): a sudden, fast rhythm that often starts and stops abruptly.
- Atrial fibrillation or flutter: rapid, irregular rhythms from the upper chambers, sometimes triggered by endurance training or illness.
- Ventricular tachycardia (VT): a fast rhythm from the lower chambers; risk depends on the cause and the person’s heart structure.
- Exercise-related bradycardia issues: less common during exercise itself, but some people have abnormal slowing or pauses during recovery.
A helpful way to think about it is: exercise can act like a “stress test” for the electrical system. If the wiring is healthy, the heart speeds up smoothly and settles back down. If there is irritability, scarring, inflammation, inherited electrical instability, or a supply-demand problem, exercise may expose it.
Even when the episode is brief, it still matters because it can guide decisions about training intensity, medication safety, and whether additional testing is needed before returning to vigorous activity.
Why exercise can trigger rhythm changes
Exercise changes the body in predictable ways: heart rate rises, adrenaline increases, breathing deepens, and fluid shifts occur. Any of these can make the heart more “excitable,” especially in a vulnerable setting.
Key triggers and mechanisms include:
- Adrenaline surge and rapid heart-rate transitions. Sudden starts (sprints, heavy sets without warm-up) and abrupt stops can provoke rhythm problems. The shift from high adrenaline to recovery can be a trigger point.
- Dehydration and electrolyte shifts. Sweating reduces plasma volume and can concentrate electrolytes. Even mild dehydration can raise heart rate, increase perceived exertion, and promote extra beats. Low potassium or magnesium—whether from sweat, diet, or medications—can increase susceptibility.
- Stimulants and “stacking” effects. Caffeine, nicotine, pre-workout supplements, decongestants, and some weight-loss products can increase heart rate and trigger palpitations, especially when combined with poor sleep or dehydration.
- Overreaching and inadequate recovery. Training hard without rest can elevate stress hormones and increase baseline heart irritability. Illness, travel, and heat amplify the effect.
- Underlying heart structure or scarring. Prior myocarditis (heart muscle inflammation), cardiomyopathy, or small areas of scar can act as a focus for abnormal rhythms—sometimes only under load.
- Inherited rhythm conditions. Some genetic disorders are specifically triggered by exertion or emotion, where adrenaline acts as a “switch” for dangerous rhythms.
- Ischemia (reduced blood supply). In people with coronary disease, exertion can trigger rhythm changes because the heart muscle is under-supplied at higher demand.
Notably, the same symptom can have very different meaning depending on timing and pattern. For example, scattered extra beats that disappear as you warm up often point to a benign pattern, while increasing ectopy with intensity, complex runs, or symptoms like dizziness raise concern.
A practical takeaway: clinicians care as much about the story as the rhythm itself—what activity triggered it, whether it starts suddenly or ramps up, whether it happens during peak effort or recovery, and whether there are warning symptoms. Those details often determine how urgent the work-up should be and how conservative return-to-play decisions need to be.
Who is at higher risk
Exercise-induced arrhythmia can happen to anyone, but the likelihood and the level of concern rise with certain risk profiles. Some risks increase the chance of benign palpitations; others increase the chance of clinically important arrhythmias.
Higher-risk groups and situations include:
- History of fainting during exercise or near-fainting with palpitations.
- Known heart disease (prior heart attack, cardiomyopathy, valve disease, congenital heart disease).
- Prior myocarditis or unexplained chest illness followed by reduced exercise tolerance.
- Family history of sudden cardiac death (especially under age 50) or known inherited rhythm disorders.
- Use of stimulants or performance-enhancing drugs. This includes high-dose caffeine, certain fat burners, anabolic agents, and some “natural” products with hidden stimulants.
- Electrolyte vulnerability: people on diuretics, those with vomiting/diarrhea, eating disorders, or very low-calorie dieting.
- Sleep deprivation and high stress—common but underestimated contributors.
- Endurance athletes and long-term high-volume training. Many endurance athletes are healthy, yet long-term high loads can be associated with atrial rhythm issues in some individuals, and it can complicate interpretation of findings like resting bradycardia or enlarged chambers.
- Uncontrolled high blood pressure or poorly managed thyroid disease, both of which increase arrhythmia risk.
- Anemia or iron deficiency. These raise heart rate for a given workload and can worsen palpitations and breathlessness.
- Age and cardiometabolic factors. Risk increases with age, diabetes, smoking, and high cholesterol because coronary disease becomes more likely.
Risk is not only about who you are; it is also about the pattern of episodes. Clinicians become more concerned when arrhythmias:
- Worsen with increasing intensity rather than fade as you warm up
- Occur with chest pressure, marked shortness of breath, confusion, or collapse
- Are new and clearly different from a person’s typical “normal” exercise response
- Occur in clusters after illness, especially viral illness
A useful mindset is to separate trigger risk (sleep, heat, dehydration, stimulants) from substrate risk (the underlying heart’s structure and electrical stability). The goal of evaluation is to identify substrate risk and reduce trigger risk—so people can exercise safely, not fearfully.
Symptoms, red flags, and complications
Exercise-induced arrhythmia can be obvious or subtle. Some people feel a dramatic, sudden “flip” into a fast rhythm; others only notice fatigue, breathlessness, or an unusual drop in performance.
Common symptoms include:
- Palpitations: fluttering, pounding, skipped beats, or a rapid “buzzing” heartbeat
- Lightheadedness or dizziness, especially when stopping suddenly
- Shortness of breath that feels out of proportion to effort
- Chest tightness, pressure, or pain during exertion
- Unusual fatigue or reduced exercise capacity
- Anxiety sensations that follow the rhythm change (not necessarily the cause)
Red flags that should prompt urgent evaluation (same day or emergency care depending on severity) include:
- Fainting during exercise or collapsing without a clear explanation
- Chest pain with sweating, nausea, or radiation to arm/jaw/back
- Severe shortness of breath or wheezing not typical for you
- Palpitations with confusion, gray-out vision, or inability to stand
- Sustained rapid heart rate that does not settle with rest in a reasonable time
- New neurologic symptoms (one-sided weakness, speech difficulty), which can signal stroke risk if atrial fibrillation is involved
Potential complications depend on the rhythm type and the person’s baseline heart health:
- Reduced performance and injury risk from dizziness or poor coordination
- Worsening heart function in those with frequent uncontrolled rapid rhythms over time
- Blood clots and stroke risk in persistent atrial fibrillation or flutter (risk varies by age and other factors)
- Sudden cardiac arrest, rare but critical—more likely when dangerous ventricular rhythms occur in a susceptible heart
One often-missed complication is behavioral: people may stop exercising entirely out of fear. That can worsen blood pressure, weight, sleep, mood, and long-term cardiovascular risk. A careful, structured plan can usually keep people active while the cause is clarified.
If possible, capture details during an episode:
- What were you doing (pace, incline, weight, temperature)?
- Did it start suddenly or gradually?
- What did your wearable show (rate, irregularity)?
- How long did it last, and what ended it?
- Were there warning symptoms (chest pain, dizziness, breathlessness)?
This “episode profile” often shortens the diagnostic process and improves treatment targeting.
How doctors diagnose it
Diagnosis aims to answer two questions: What rhythm is happening? and Is it dangerous in this person? That second question depends on heart structure, triggers, and the exact circumstances of exercise.
A typical evaluation includes:
- Detailed history and medication/supplement review. Clinicians will ask about caffeine dose, pre-workouts, decongestants, recreational drugs, and performance enhancers, plus sleep, stress, recent illness, and hydration habits.
- Physical exam and resting ECG. This can show baseline conduction patterns, prior silent injury clues, or signs of inherited electrical syndromes.
- Blood tests when appropriate. Common checks include thyroid function, electrolytes, kidney function, and sometimes iron studies if fatigue is prominent.
- Ambulatory rhythm monitoring. Options range from 24–48 hour Holter monitors to 1–2 week patches, event monitors, or wearable-based recordings. The goal is to catch the rhythm during symptoms.
- Exercise testing (treadmill or bike). This is often central for exercise-induced symptoms because it reproduces the trigger, documents the rhythm at onset, and reveals whether the issue appears during effort or recovery.
- Echocardiogram. Ultrasound assesses chamber size, pumping function, valve disease, and wall thickness—key for determining whether the heart is structurally normal.
- Cardiac MRI in selected cases. MRI can detect scar or inflammation patterns that are not visible on ultrasound, and it can be especially useful when ventricular arrhythmias, myocarditis history, or unexplained symptoms are present.
- Coronary evaluation when indicated. In older individuals or those with risk factors and exertional chest symptoms, clinicians may evaluate for coronary disease using stress imaging or CT-based methods.
Interpretation is nuanced, especially in trained athletes. Athletic remodeling can produce slower resting heart rates, larger chambers, and ECG changes that look abnormal in sedentary people but are normal in athletes. That is why sports cardiology–aware interpretation matters.
Many people also ask about wearables. They can be helpful for timing and pattern recognition, but they are not a complete diagnostic tool. A clean-looking wearable tracing does not always rule out a clinically significant rhythm, and a “warning” does not always mean danger. The best use is to bring recordings to your clinician to guide formal monitoring.
A clear diagnosis usually emerges from matching symptoms to a documented rhythm and then layering in structural evaluation. Once those pieces are known, a safe treatment and exercise plan becomes much more straightforward.
Treatment and return to exercise
Treatment is individualized because “exercise-induced arrhythmia” is not one condition. The plan depends on the rhythm type, symptom burden, and whether there is underlying heart disease. In many cases, the goal is not to stop exercise—it is to make exercise safer and more predictable.
Common treatment components include:
1) Trigger control (often the fastest win)
- Hydration: aim for pale-yellow urine and adjust fluid intake for heat and duration.
- Heat strategy: reduce intensity in high heat/humidity; use cooling and longer warm-ups.
- Stimulant audit: reduce or remove pre-workouts, high-dose caffeine, nicotine, and decongestants.
- Sleep and recovery: prioritize consistent sleep; build rest days into training cycles.
- Illness rule: avoid intense training during fever, chest infections, or “viral-with-chest” symptoms.
2) Rhythm-specific therapy
- For SVT, vagal maneuvers may help some episodes, and catheter ablation can be highly effective for many SVT types.
- For atrial fibrillation/flutter, options include rate control, rhythm-control medications, ablation, and stroke-prevention decisions based on individual risk factors.
- For frequent premature beats, treatment ranges from reassurance to medications or ablation when symptoms are severe or when the burden is high and affects heart function.
- For ventricular arrhythmias, the focus is identifying the cause (scar, cardiomyopathy, inherited syndromes, myocarditis) and tailoring therapy, which may include medication, ablation, and in selected cases implantable defibrillator strategies.
3) A structured return-to-exercise plan
A typical graded approach includes:
- Start below the intensity that provokes symptoms.
- Increase duration first, then intensity, in small steps (for example, weekly adjustments rather than daily jumps).
- Include a 5–10 minute warm-up and cool-down to reduce abrupt adrenaline swings.
- Re-test (symptoms, monitor, or formal exercise test) before returning to maximal effort if the initial episodes were concerning.
When to stop and seek care during a workout
Stop exercising and seek medical advice urgently if you develop chest pain, fainting, near-fainting, severe breathlessness, or sustained rapid palpitations that do not improve with rest.
With the right diagnosis and plan, many people—including competitive athletes—return to meaningful training. The key is not guesswork. Document the rhythm, clarify the risk, address triggers, and then rebuild fitness with clear guardrails.
References
- 2024 HRS expert consensus statement on arrhythmias in the athlete: Evaluation, treatment, and return to play 2024 (Guideline/Consensus)
- 2020 ESC Guidelines on sports cardiology and exercise in patients with cardiovascular disease 2021 (Guideline)
- Ventricular arrhythmias in association with athletic cardiac remodelling 2024 (Review)
- Prognostic implications of stress test-induced arrhythmias: a systematic review and meta-analysis 2025 (Systematic Review/Meta-Analysis)
Disclaimer
This article is for educational purposes and is not a substitute for personalized medical care. Exercise-related palpitations can range from benign to urgent. If you have chest pain, fainting, severe shortness of breath, new neurologic symptoms, or sustained rapid heartbeats—especially during or right after exercise—seek emergency care. If you have recurrent symptoms, a family history of sudden cardiac death, or known heart disease, talk with a qualified clinician before returning to vigorous training. Medication changes and supplement use should be discussed with a healthcare professional, because some products can worsen arrhythmias or interact with prescriptions.
If you found this article helpful, please consider sharing it on Facebook, X (formerly Twitter), or any platform you prefer, and follow us on social media. Your support through sharing helps our team continue producing high-quality, trustworthy health content.






