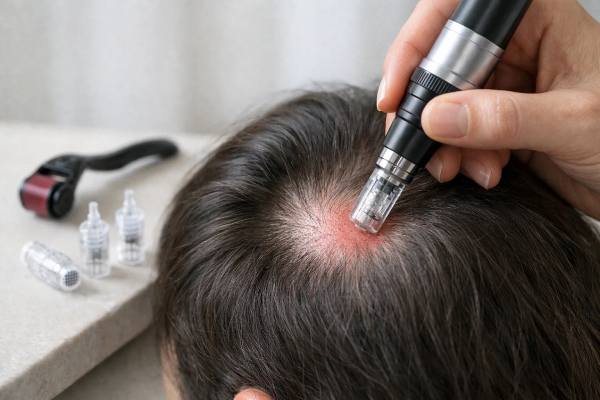
Microneedling has become one of the most discussed add-on treatments for thinning hair, but the real question is not whether tiny needles can help. It is how deep, how often, and how safely they should be used. Those details matter because scalp microneedling sits at a narrow line: too little stimulation may do very little, while too much depth or too-frequent treatment can turn a promising routine into unnecessary irritation.
The strongest evidence so far points to microneedling as an adjunct, especially for pattern hair loss, rather than a universal fix for every kind of shedding. It may help improve topical delivery, stimulate wound-healing signals linked to hair cycling, and support better results when paired with established therapies. But the studies do not support a single “perfect” needle length for everyone, and home use is not the same as in-office treatment.
This guide breaks down what current evidence suggests about needle length, session spacing, safety, aftercare, and when microneedling should be left to a clinician.
Core Points
- Microneedling appears most useful as an add-on for pattern hair loss, especially when paired with topical treatment.
- Shallower to moderate depths often perform as well as, or better than, more aggressive needling in current hair-loss studies.
- The goal is controlled stimulation, not heavy bleeding or daily trauma to the scalp.
- Redness and mild soreness are common, but persistent pain, pustules, crusting, or worsening scalp inflammation are warning signs.
- Home users should stay conservative with needle length and spacing, while deeper sessions belong in a supervised setting.
Table of Contents
- What microneedling can and cannot do
- Choosing needle length and depth
- How often sessions should be spaced
- Combining microneedling with other treatments
- Safety risks and common mistakes
- Who should avoid it and when to stop
What microneedling can and cannot do
Microneedling for hair growth works by creating controlled micro-injuries in the scalp. These tiny punctures appear to trigger wound-healing signals, growth-factor release, and changes in the local follicle environment. Just as important, they can improve the penetration of topical treatments applied as part of a broader regimen. That is why microneedling is usually discussed alongside minoxidil rather than as a fully stand-alone cure.
The best evidence is still in androgenetic alopecia, also called male and female pattern hair loss. In that setting, microneedling may improve hair count, diameter, and patient-rated improvement when it is added to established therapy. It does not have equally strong evidence for every other cause of thinning. If the main problem is sudden shedding, scarring alopecia, severe seborrheic dermatitis, or active scalp infection, microneedling may be the wrong first move.
That distinction matters because people often treat “hair loss” as one diagnosis. It is not. A patient with miniaturizing follicles and a patient with inflamed, tender, scaling scalp need very different plans. Microneedling tends to fit best when follicles are still present and the goal is to improve the response of a thinning scalp, not to revive fully scarred skin or bypass an untreated medical trigger. Readers comparing broader male pattern hair loss options will notice that microneedling is usually presented as an adjunctive procedure, not a replacement for first-line medical treatment.
It is also important to separate realistic outcomes from online hype. Microneedling can support hair regrowth, but it is rarely a one-session intervention. Most studies showing benefit used repeated sessions over at least 12 weeks, often longer. That means it behaves more like a structured program than a quick procedure. The payoff, when it happens, is typically gradual: better density, thicker-looking hair shafts, or improved response to topical therapy over months.
There are also limits built into the method itself. Needle length alone does not guarantee the same true penetration in every person. Device type, scalp thickness, pressure, angle, and operator technique all change what the follicle actually experiences. A 1.0 mm label on a box does not mean every puncture reaches exactly 1.0 mm into living scalp tissue. That is one reason the literature looks messy. Two studies may both say “1.5 mm,” yet the biological dose is not identical.
The practical takeaway is that microneedling can be useful, especially for patterned thinning, but it is not a magic workaround for poor diagnosis or unrealistic expectations. Used well, it can strengthen an evidence-based hair-loss plan. Used casually, it can create irritation without much benefit.
Choosing needle length and depth
Needle length is the most searched part of scalp microneedling, and it is also the most oversimplified. The evidence does not support one universal “best” number for every device, scalp, and treatment goal. What it does suggest is more nuanced: useful results have been reported across a wide range of depths, but deeper is not automatically better.
In published hair-loss studies, needle lengths have ranged from very short home-use depths around 0.25 mm to in-office protocols reaching 1.5 mm, 2.0 mm, or even 2.5 mm in some device-based studies. That sounds as if almost anything works, but the real pattern is narrower than it looks. A recent meta-analysis found that microneedling combined with minoxidil improved outcomes overall, yet subgroup analysis did not show a statistically significant hair-count advantage for depths above 1 mm compared with 1 mm or less. In other words, the pooled evidence does not prove that more depth produces more hair.
A useful head-to-head study compared 0.6 mm with 1.2 mm microneedling, both paired with minoxidil. The 0.6 mm group performed better than minoxidil alone and tended to outperform the 1.2 mm group on key measures. That is not the same as proving 0.6 mm is always optimal, but it does challenge the common belief that aggressive needling is the most effective route.
A practical way to think about depth is by treatment setting:
- Very short needles, around 0.25 mm: mostly useful for enhancing topical penetration, with limited evidence for strong stand-alone hair effects.
- Shallow to moderate depths, roughly 0.5 to 1.0 mm: often the most balanced range for hair-focused protocols, especially when paired with minoxidil.
- Deeper treatments, around 1.25 to 1.5 mm and above: usually reserved for in-office work, where pain, pinpoint bleeding, and downtime are more acceptable and technique is controlled.
Device choice changes how those depths behave. A pen-style device tends to puncture more vertically and consistently. A roller enters at changing angles as it moves across the curved scalp, which may create more drag and a less uniform injury pattern. That does not make rollers useless, but it helps explain why “needle length” and “biologic effect” are not the same thing.
The safest evidence-based interpretation is this: for hair growth, the goal is controlled stimulation, not maximal trauma. Current studies support shallow-to-moderate depths as credible options, especially when the target is androgenetic alopecia and the plan includes topical therapy. Depth should match the setting, the device, the patient’s tolerance, and the reason microneedling is being used.
One more point often gets missed. Needle length is not a scorecard. Better treatment is not the treatment that looks most dramatic. A session that causes excessive pain, diffuse bleeding, or a week of inflammation is not automatically more therapeutic than a calmer, well-spaced protocol.
How often sessions should be spaced
Frequency is where many home routines go wrong. Once people hear that microneedling may stimulate hair growth, they assume that more sessions should create faster results. The evidence does not support that. Scalp tissue needs recovery time, and repeated trauma without enough healing can shift the balance from useful stimulation to chronic irritation.
Clinical studies in androgenetic alopecia have used schedules ranging from twice weekly to once monthly. That is a very broad range, and it reflects how variable the protocols are. Shorter needles in home-use or topical-delivery studies have sometimes been used more often. Longer needles in office-style studies are usually spaced out, often weekly, every two weeks, or every four weeks. That pattern makes biological sense: the deeper the injury, the longer the scalp generally needs to calm down.
The most practical frequency rule is to match spacing to depth.
- Shorter, more superficial needling: may be done more often, though evidence for dramatic hair gains at very short lengths is limited.
- Moderate depths: commonly fit weekly or every-other-week schedules in studies.
- Deeper sessions: are usually spaced every two to four weeks, sometimes longer.
One review of the hair-loss literature found an interesting trend: longer overall treatment duration and lower session frequency appeared to be associated with better total-hair-count improvement. That should not be read as “monthly is always better than weekly,” but it does support a useful mindset. Patience matters more than intensity. A measured protocol continued long enough may beat a very aggressive plan that is hard to tolerate or easy to abandon.
Time horizon matters just as much as spacing. Hair changes slowly. Even when a protocol is working, visible improvement often takes at least 3 months, and fuller assessment commonly takes 4 to 6 months. That means evaluating a session schedule after two or three weeks is usually too early. What matters is whether the scalp is tolerating treatment and whether the plan can be maintained long enough to judge results honestly.
At home, conservative scheduling is especially important. One small home-use study used 0.25 mm needling twice weekly for 6 months and found mild tolerability with limited statistical improvement. That does not mean home use is pointless. It does mean that frequent superficial needling is not a guaranteed shortcut.
A useful decision framework is simple:
- Start with the least aggressive frequency that fits the chosen depth.
- Watch how long redness, tenderness, and flaking last after each session.
- Do not repeat a session while the scalp still feels actively irritated.
- Judge results over months, not days.
The best schedule is usually the one the scalp can recover from, not the one that looks most ambitious on paper. In hair restoration, steady, tolerable repetition tends to outperform bursts of over-treatment.
Combining microneedling with other treatments
Microneedling tends to look strongest when it is not used alone. Most of the better hair-loss studies pair it with topical minoxidil, and the combined approach usually outperforms minoxidil by itself on hair count and, in some analyses, hair diameter. That does not mean microneedling has no independent effect. It means the clearest evidence today is for microneedling as a booster rather than as a solo cornerstone.
Why might the combination work better? Two reasons are plausible. First, microneedling may stimulate growth-related signaling through the controlled wound-healing response. Second, it can improve the penetration of topical agents through the outer scalp barrier. For a patient already using minoxidil, that combination may make the scalp more responsive over time.
Still, combining treatments adds a timing question: when should topicals be applied around the session? The literature is not perfectly standardized, and studies vary. The safer practical principle is to follow the instructions tied to the specific depth and device being used. The deeper the treatment, the less sense it makes to improvise with multiple active products immediately afterward. Channels that can improve delivery can also increase irritation. That matters especially with alcohol-heavy solutions, fragranced serums, and strong over-the-counter actives.
For patients already navigating a minoxidil plan, it helps to understand common minoxidil routine mistakes before layering microneedling on top. A good routine is easier to judge when only one major variable changes at a time.
Microneedling is also discussed alongside platelet-rich plasma, growth-factor solutions, and certain device-based treatments. Some studies suggest combination benefit, but the evidence becomes harder to compare because the protocols vary so much. PRP plus microneedling is a common pairing in clinics, yet the gain from adding both together depends heavily on who is being treated, how advanced the thinning is, and whether a strong medical foundation is already in place. The same logic applies to topical peptides, growth-factor cocktails, and other add-ons: the scalp does not necessarily benefit from every trending serum simply because the barrier is temporarily more open.
A grounded combination plan usually follows a few principles:
- Keep the diagnosis clear.
- Anchor the routine in proven treatments first.
- Add microneedling for a defined reason, not as a reflex.
- Avoid stacking several irritants in the same window.
- Reassess after a meaningful treatment interval.
One original but useful way to frame it is this: microneedling often improves the “delivery environment” and the “repair signal,” but it does not replace the medication doing the long-term biochemical work. That is why it fits so naturally with minoxidil and less convincingly with product overload. The scalp usually responds better to one smart combination than to five half-tested add-ons.
Safety risks and common mistakes
Microneedling is generally described as minimally invasive, but “minimally invasive” does not mean risk-free. In hair-loss studies, serious adverse events have been uncommon, and the most common problems have been mild and temporary: pain, redness, scalp irritation, and short-lived tenderness. That reassuring safety pattern is real. It is also closely tied to proper patient selection, sterile equipment, and reasonable technique.
Most complications start with one of three mistakes: too much depth, too little recovery time, or poor hygiene. Those errors are far more common in self-directed routines than in supervised treatment. A scalp that stays red, sore, or crusted for days is not showing toughness. It is showing that the treatment may have overshot its useful range.
Common warning signs after microneedling include:
- Redness that does not steadily improve
- Burning rather than simple soreness
- Pustules, yellow crust, or oozing
- Increasing tenderness after the first day
- Flare of dandruff, dermatitis, or folliculitis
- Patchy breakage from rough device drag through long hair
Pain level can be informative too. One depth-comparison study found that the deeper setting caused more pain. That matters because tolerability affects adherence, and it may also signal that deeper is not buying a better risk-benefit tradeoff for that patient.
At-home users should be especially careful about scalp preparation and device care. Dirty needles, shared devices, and casual “disinfection” create preventable infection risk. Even when outright infection does not occur, repeated barrier disruption on an already inflamed scalp can worsen itch, flaking, and shedding. If the scalp already shows signs of active inflammation, adding needling before the underlying problem is controlled is usually a poor idea.
Another common mistake is judging success by bleeding. Pinpoint bleeding appears in some clinical protocols, especially at deeper in-office depths, but it is not a required home benchmark. Chasing blood as proof of effectiveness encourages overtreatment. For many hair-focused routines, mild erythema and controlled stimulation are enough.
Aftercare deserves more respect than it gets. The basic goals are simple:
- Keep the scalp clean.
- Avoid touching it unnecessarily.
- Do not layer irritating products onto freshly needled skin.
- Skip aggressive heat styling the same day.
- Avoid sun exposure on a tender scalp.
A final safety insight is worth stating plainly: not every problem after microneedling is “purging” or a normal adjustment phase. Hair-loss communities sometimes normalize too much discomfort. If the scalp becomes more inflamed, more painful, or more reactive over repeated sessions, the protocol needs to change. Hair growth should not depend on pushing through obvious tissue stress.
Who should avoid it and when to stop
Microneedling is not appropriate for every thinning scalp. The most important reason to pause is diagnostic uncertainty. If a person does not know whether the problem is pattern hair loss, shedding from a medical trigger, psoriasis, seborrheic dermatitis, alopecia areata, or a scarring alopecia, microneedling should not be the first experiment. The same procedure can be helpful in one setting and counterproductive in another.
People who should be especially cautious include those with:
- Active scalp infection or pustules
- Open wounds, raw skin, or recent chemical irritation
- Moderate to severe eczema or psoriasis on the scalp
- Strong keloid tendency or abnormal scar history
- Significant bleeding tendency or anticoagulant use
- Immunosuppression
- Pregnancy, unless a clinician specifically advises otherwise
- Scalp pain, burning, or rapid inflammatory hair loss without a diagnosis
These are not small details. A needling device used on an infected or highly inflamed scalp can intensify problems that were never mechanical to begin with. It is also wise to avoid self-treatment when shedding is sudden, diffuse, and recent. In that setting, the first priority is often finding the trigger, not trying to mechanically stimulate the scalp.
Knowing when to stop matters just as much as knowing when to start. Stop microneedling and seek evaluation if you develop persistent swelling, spreading redness, crusting, pus, worsening pain, fever, or a marked increase in scalp sensitivity. Also stop if each session leaves the scalp more reactive than the one before. Improvement should look like better tolerance and gradual benefit over time, not escalating irritation.
There is also a softer stop point: lack of meaningful benefit despite good technique and enough time. If a well-planned routine has gone on for several months with no visible improvement and no clear enhancement of a broader treatment plan, it may not be the right tool for that person. Persistence is useful in hair care, but endless escalation is not.
A reasonable clinician-guided path often looks like this:
- Confirm the diagnosis.
- Decide whether microneedling is being used for stimulation, topical delivery, or both.
- Choose a depth and schedule that match the setting.
- Monitor tolerance closely for several sessions.
- Reassess after a true trial, not after one treatment.
If the diagnosis is unclear or the scalp is symptomatic, the safer move is to step back and get expert review. That is especially true when the pattern, symptoms, or pace of loss suggest something beyond routine thinning. In those cases, the threshold for when hair loss needs a dermatologist should be low.
The bottom line is measured rather than dramatic. Microneedling can be a worthwhile part of a hair-growth strategy, but only when the scalp is the right scalp, the depth is sensible, the schedule is realistic, and safety stays in the foreground.
References
- Evaluating the efficacy and safety of combined microneedling therapy versus topical Minoxidil in androgenetic alopecia: a systematic review and meta-analysis 2025 (Systematic Review)
- Efficacy and safety of combined microneedling therapy for androgenic alopecia: A systematic review and meta-analysis of randomized clinical trials 2024 (Systematic Review)
- Microneedling for Hair Loss 2022 (Review)
- Microneedling in androgenetic alopecia; comparing two different depths of microneedles 2021 (Randomized Study)
- Usefulness of home-use microneedle devices in the treatment of pattern hair loss 2021 (Randomized Study)
Disclaimer
This article is for educational purposes only and is not a substitute for medical advice, diagnosis, or treatment. Microneedling for hair loss is not appropriate for every scalp condition, and the safest depth and schedule depend on your diagnosis, skin tolerance, device, medications, and medical history. Seek professional evaluation if hair loss is sudden, painful, inflamed, scar-like, or associated with scaling, pustules, or rapid progression.
If you found this article helpful, please share it on Facebook, X, or another platform you trust so others looking for clear guidance on microneedling depth, frequency, and safety can find it.






