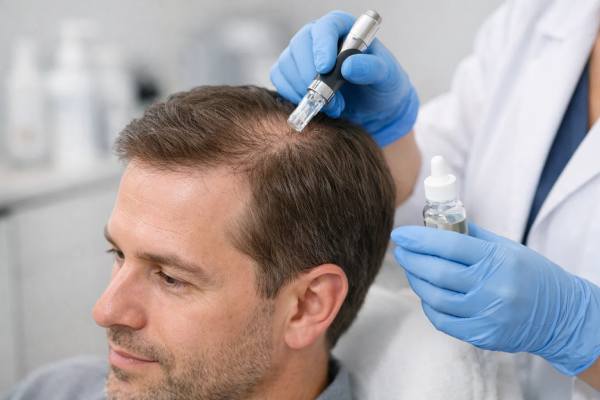
Hair-loss treatment is full of big promises, but exosome therapy stands out because it sounds both futuristic and biologically precise. Instead of transplanting cells, it uses tiny extracellular vesicles that carry signaling molecules such as proteins, lipids, and genetic material. The idea is that these messengers may nudge the scalp toward a more growth-friendly state by calming inflammation, supporting dermal papilla cells, and extending active growth phases in vulnerable follicles.
That is the promise. The reality is more complicated. Exosome therapy for hair loss is still early, protocols vary widely, and many clinics market it long before the science has settled. Some products are injected, others are paired with microneedling, and some may not be well-characterized exosomes at all. Early human studies are encouraging, especially for androgenetic alopecia, but they are still small and uneven.
For readers trying to separate innovation from hype, the key question is not whether exosomes are interesting. They are. The key question is whether the product, clinic, and evidence are strong enough to justify the risk and cost right now.
Essential Insights
- Early studies suggest exosome-based treatment may improve hair density and thickness in some people with pattern hair loss.
- Exosomes may work best as a physician-led add-on approach rather than a replacement for proven therapies.
- The evidence is still limited by small studies, short follow-up, and major differences in products and treatment methods.
- In the United States, exosome products for therapeutic use are not FDA-approved for hair loss.
- Before considering treatment, ask for the product source, how it is tested, how it is delivered, and what proven alternatives were reviewed first.
Table of Contents
- What exosome therapy actually means
- How it could affect follicles
- What the human evidence shows
- Safety red flags to watch for
- How it compares with standard options
- Questions to ask before you pay
What exosome therapy actually means
Exosomes are tiny membrane-bound vesicles released by cells. Think of them as biological packages that help cells communicate. They can carry growth-related proteins, lipids, and fragments of RNA that influence how nearby cells behave. In hair medicine, clinics often describe them as a “cell-free regenerative treatment,” which means the therapy uses signaling material rather than living stem cells themselves.
That description is useful, but it leaves out an important problem: in the real world, “exosome therapy” is not one standardized treatment. Clinics may use products derived from adipose tissue, bone marrow, umbilical-cord-related tissues, placental material, or cultured mesenchymal cells. Some use purified extracellular vesicles. Others use mixtures that may include conditioned media, growth factors, peptides, or other secreted material. A patient may hear the word exosome and assume every product is basically the same. It is not.
Delivery also varies. Some clinicians inject the product across thinning areas. Others combine it with microneedling so the scalp surface becomes more permeable. Some protocols use a single treatment; others involve several sessions spaced weeks apart. Concentration, particle count, storage method, thawing, and scalp-prep steps also differ. Those details matter because biologic products are sensitive to processing. Two treatments sold under the same buzzword may be very different in potency and consistency.
Another point readers often miss is the difference between a cosmetic claim and a medical claim. When a clinic says a product “supports scalp vitality,” that sounds softer than saying it treats androgenetic alopecia, but the practical message to the patient may be the same. If you are paying to improve thinning hair, you are effectively being sold a medical outcome, even when the language is styled as wellness or aesthetics.
This is why exosome therapy can feel confusing. The science behind extracellular vesicles is real and active. The marketplace around them is much less tidy. A careful reader should treat “exosome therapy” not as a single proven intervention, but as a broad category of biologic products with major differences in source, processing, and quality control. That distinction is central to understanding both the early promise and the serious caution around these treatments.
How it could affect follicles
Hair follicles are not passive tubes that either grow or stop growing. They are active mini-organs that cycle through growth, transition, rest, and shedding. If you want a refresher on that rhythm, the hair growth cycle explains why small changes in follicle signaling can alter density over time. Exosome therapy matters because it is designed to influence that signaling environment.
The main biological targets are thought to include dermal papilla cells, follicle stem-cell niches, outer root sheath cells, and the inflammatory environment around the follicle. In lab and animal research, exosomes appear able to deliver messages that may encourage proliferation, improve follicle-cell survival, and push follicles toward a longer anagen, or active growth, phase. Several signaling pathways often come up in this research, including Wnt, sonic hedgehog, BMP, and TGF-beta related pathways. For the average reader, the practical translation is simple: the treatment aims to make vulnerable follicles behave more like healthier, growing follicles.
That may be especially relevant in androgenetic alopecia, where follicles miniaturize over time. Miniaturized follicles produce shorter, finer hairs and spend less time in robust growth. If a therapy can reduce inflammatory stress, improve cellular communication, or support matrix and dermal papilla function, it could theoretically help those follicles produce thicker fibers or stay in growth longer.
There is also interest in exosomes as partners rather than solo treatments. Microneedling is commonly paired with them because it may create channels that improve delivery and may independently stimulate repair responses in the scalp. Some clinics also combine exosomes with established treatments such as minoxidil or platelet-rich plasma. This may make sense biologically, but it creates another evidence problem: when multiple treatments are used together, it becomes harder to know what is actually driving the improvement.
One more nuance matters. A better scalp environment is not the same as guaranteed regrowth. Hair biology is constrained by diagnosis. A follicle that is dormant but still viable is different from a follicle destroyed by scarring alopecia. Exosomes may be more plausible for nonscarring conditions, especially pattern hair loss, than for areas where follicles are permanently lost.
So the mechanism story is promising but incomplete. Exosomes may influence the follicle’s signaling language in useful ways. That does not automatically mean every exosome product, every source material, or every delivery method will produce meaningful clinical results. The biology offers a rationale. It does not, by itself, settle the question of real-world benefit.
What the human evidence shows
The human evidence is better than pure marketing, but not yet strong enough to erase caution. Recent reviews found that published hair-loss studies are still limited in number, often small, and highly variable in design. That matters because results can look impressive on paper while still being hard to compare across studies.
The encouraging part is that several studies reported gains in hair density, thickness, or patient satisfaction. A recent systematic review identified 11 clinical studies across different alopecia types. Reported improvements included density gains in the rough range of about 9.5 to 35 hairs per square centimeter, depending on the product and protocol. In one randomized trial that tested an exosome-containing plant extract formulation in male alopecia, the treatment group showed higher median hair growth than placebo. In a prospective study of 30 men with androgenetic alopecia, hair density improved at both 4 and 12 weeks after scalp injections. Other reports using adipose-derived or extracellular-vesicle-based products also found short-term improvements in density and thickness.
That sounds persuasive until you look closer. The studies do not use one uniform intervention. They involve different sources, different purification methods, different treatment schedules, and different delivery methods. Some use intradermal injection. Some use topical application after microneedling. Some combine exosomes with other regenerative materials. Follow-up is often short. Several studies are open-label, retrospective, or uncontrolled, which raises the chance that expectation effects, selection bias, and natural variation in shedding could influence the outcome.
Another key limitation is outcome consistency. Some studies measure hair density with imaging software. Others emphasize patient satisfaction or physician assessment. Those are not interchangeable. A happy patient matters, but a subjective improvement score is not the same as a blinded, standardized hair-count endpoint.
The safety story in the studies is also easy to overread. Reported side effects in hair-loss studies have often been mild, such as brief redness or scalp irritation. That is reassuring, but it does not mean the overall safety question is closed. One recent clinical review found only 125 hair-loss patients across the relevant clinical studies it identified. That is far too small to rule out uncommon but meaningful harms, especially when manufacturing standards differ between products.
The fairest summary is this: exosome therapy for pattern hair loss has biologic plausibility and early human signals of benefit, but the evidence is still pre-mature for strong confidence. It is more accurate to call it emerging than established. If you are comparing it with familiar treatments, think of it as a promising but not yet settled option. And if a clinic presents it as the next obvious standard of care, that is a sign the sales pitch may be running ahead of the science. For readers also considering combination plans, it helps to understand typical microneedling schedules for hair growth, because some exosome protocols borrow that framework even though the products themselves are not standardized.
Safety red flags to watch for
This is the section many people skip, and it is the section that matters most. The biggest safety issue is not just whether exosomes can irritate the scalp. It is whether the product in front of you is well-characterized, legally handled, properly screened, sterile, and appropriate for human use in the first place.
In the United States, exosome products for therapeutic use are regulated as biologic products, and there are no FDA-approved exosome products for hair loss. That does not automatically mean every clinic is acting recklessly, but it does mean the burden of caution should be high. If a clinic presents the treatment as routine, fully established, or government-cleared for hair restoration, that is a serious warning sign.
The next red flag is vagueness. A trustworthy clinic should be able to explain:
- the source of the exosomes or extracellular vesicles,
- whether the material is human-derived, animal-derived, plant-derived, or mixed,
- how it is processed and stored,
- what sterility and infectious-disease screening steps are used,
- how the material is characterized, and
- whether there is a lot number and documentation for traceability.
If those answers are fuzzy, that is not a minor customer-service issue. It suggests the clinic may not have a strong grasp of the product itself.
Another concern is contamination and biologic unpredictability. Exosomes are not inert beauty ingredients. They are biologically active particles. Poor processing, poor storage, or weak donor screening raises the possibility of contamination, immune reactions, inflammation, or simply a product that behaves inconsistently from batch to batch. Even if major complications are rare, the combination of biological activity plus weak standardization is exactly what makes this field hard to trust at the consumer level.
Watch for exaggerated claims. Red-flag language includes phrases such as “works for all hair loss,” “replaces minoxidil and finasteride,” “one session is enough,” or “no risk because it is natural.” Hair disorders are too varied for those promises to be credible. Pattern hair loss, telogen effluvium, traction damage, inflammatory scalp disease, and scarring alopecia are different problems. A clinic that does not slow down to make the diagnosis is not practicing careful hair medicine.
Also pay attention to the scalp itself. If you already have active itching, burning, redness, pustules, flaking, or tenderness, the treatment conversation should start with scalp evaluation, not a regenerative add-on. A stressed scalp rarely benefits from rushing into procedures before the underlying issue is identified. Understanding the follicle environment and scalp health can help you see why inflammation control often deserves attention before premium procedures.
A useful rule of thumb is this: if the clinic spends more time on branding than on diagnosis, product characterization, and alternatives, walk away.
How it compares with standard options
Exosome therapy is often marketed as though it belongs in the same evidence tier as standard hair-loss treatments. It does not. The most important comparison is not whether exosomes are interesting, but whether they have enough data to compete with established options on reliability, reproducibility, and long-term value.
For androgenetic alopecia, standard options still come first for most people. Topical minoxidil has a long track record, defined use patterns, and real-world familiarity. Oral therapies such as finasteride, dutasteride, spironolactone, or low-dose oral minoxidil may be appropriate in selected patients under medical supervision. Devices such as low-level laser therapy and office procedures such as microneedling or platelet-rich plasma also have varying but more developed evidence bases than exosome therapy in many settings. A good starting point is understanding the tradeoffs between topical and oral minoxidil, because that conversation is often more grounded than jumping straight to a premium biologic procedure.
That does not mean exosomes have no role. They may end up as an adjunct for carefully selected patients, particularly those with early to moderate nonscarring thinning who want a physician-led add-on after standard treatments are discussed. They may also interest patients who cannot tolerate certain medications or who want a regenerative-style approach layered onto a broader plan. But “may” is the key word. At this stage, exosomes are not a proven replacement for foundational therapies.
Hair transplantation is another useful comparison. Transplants move follicles from one area to another and can create meaningful restoration when donor supply is good. Exosomes do not create new donor hair or rebuild a completely depleted frontal hairline by themselves. At best, they aim to improve the performance of existing follicles. That is a different goal. Someone with advanced miniaturization or large bare areas may get far more predictable value from assessing hair transplant candidacy and recovery than from paying for an unstandardized biologic procedure.
There is also the question of cost efficiency. Because exosome therapy is typically elective and cash-pay, the financial bar should be high. A treatment with limited long-term data and no standard protocol should not automatically outrank lower-cost, better-studied options.
In practical terms, exosomes belong near the “consider carefully” end of the treatment ladder, not the “start here” end. For some patients, they may eventually become a useful add-on in multi-modal care. For many others, they are still best viewed as experimental in spirit, even when sold in polished clinical settings.
Questions to ask before you pay
The best defense against hype is a short list of sharp questions. You do not need to sound technical. You just need to ask questions that force the clinic to move from marketing language to specifics.
Start with diagnosis. Ask exactly what type of hair loss you have and how that was determined. If the answer is vague, or if the clinic never discussed pattern hair loss versus inflammatory or scarring causes, pause there. Exosomes are not a shortcut around diagnosis.
Then ask about the product:
- What is the exact source material?
- Is it purified exosomes, extracellular vesicles, or a broader secretome product?
- Is it intended for topical use, injection, or both?
- How is it stored and prepared on treatment day?
- What documentation exists for lot tracking, sterility testing, and donor screening?
- What are the known short-term side effects and the unknowns?
Next, ask about the protocol. How many sessions are recommended, at what interval, and why? What objective outcomes will be measured? Will the clinic use standardized photographs, hair counts, or trichoscopy, or are they relying on casual before-and-after pictures? If the treatment plan sounds fixed before they have looked closely at your scalp, that is a weak sign.
You should also ask what proven options were considered first. A careful clinician should be able to explain why exosomes make sense for you after discussing medication, scalp care, procedural options, and realistic timelines. Hair growth is slow. Any clinic promising dramatic visible change within a few weeks should be treated with skepticism.
Finally, ask what would make the clinician say no. This is one of the most revealing questions in all of cosmetic and regenerative medicine. Good clinicians have exclusion criteria. They should hesitate in cases of active scalp disease, unclear diagnosis, pregnancy-related treatment constraints, severe scarring alopecia without a broader medical plan, or unrealistic expectations.
The goal is not to interrogate the clinic. The goal is to see whether the clinic behaves like a medical practice or a luxury service. If the answers are careful, specific, and balanced, that is encouraging. If the answers are evasive, oversimplified, or heavily scripted, trust that signal.
And if your shedding is sudden, patchy, painful, inflamed, or associated with other symptoms such as fatigue, weight change, or menstrual shifts, step back from elective procedures and get the cause assessed first. A treatment is only as good as the diagnosis behind it.
References
- Exosomes and Hair Regeneration: A Systematic Review of Clinical Evidence Across Alopecia Types and Exosome Sources – PMC 2025 (Systematic Review)
- Exosomes for Treating Hair Loss: A Review of Clinical Studies – PubMed 2024 (Review)
- A Pilot Randomized Controlled Trial (RCT) Evaluating the Efficacy of an Exosome-Containing Plant Extract Formulation for Treating Male Alopecia – PMC 2025 (RCT)
- Effectiveness of Exosome Treatment in Androgenetic Alopecia: Outcomes of a Prospective Study – PMC 2024 (Prospective Study)
- Important Patient and Consumer Information About Regenerative Medicine Therapies | FDA 2021 (Safety and Regulatory Guidance)
Disclaimer
This article is for educational purposes only and is not medical advice, diagnosis, or treatment. Hair loss has many causes, including hormonal, inflammatory, nutritional, autoimmune, medication-related, and scarring conditions. Exosome therapy is not a substitute for a proper diagnosis, and product quality, regulation, and clinical evidence remain uneven. If you have sudden shedding, patchy loss, scalp pain, significant redness, or worsening thinning, seek evaluation from a qualified clinician before starting any procedure.
If you found this article useful, please share it on Facebook, X, or your preferred platform to help more readers make safer, better-informed decisions.






