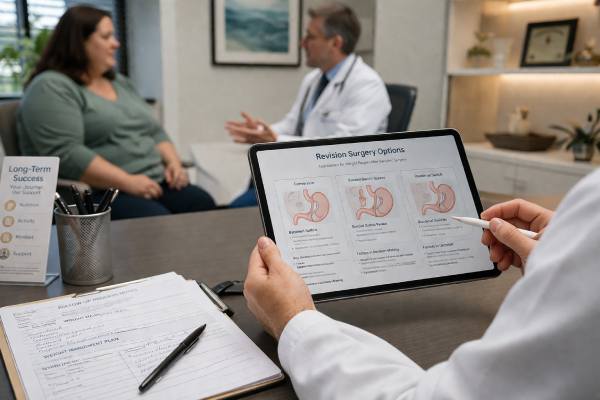
Weight regain after bariatric surgery does not automatically mean the first operation failed, and it does not automatically mean you need another one. Some regain from the lowest post-op weight is common over time. The harder question is whether the regain is large enough, persistent enough, or tied to symptoms and health problems strongly enough to justify revision bariatric surgery.
A second procedure can help selected patients after sleeve gastrectomy or Roux-en-Y gastric bypass, but it is not a simple reset button. The right next step depends on anatomy, eating patterns, reflux, medication use, nutritional status, and how much benefit is realistically expected from another operation. This article explains when revision is worth considering, what evaluation should happen first, which options are used after sleeve or bypass, when endoscopic or medical treatment may be a better fit, and what trade-offs matter before moving forward.
Table of Contents
- What weight regain means after bariatric surgery
- When revision surgery should be considered
- How the pre-revision workup is done
- Options after sleeve gastrectomy
- Options after Roux-en-Y gastric bypass
- Surgery, endoscopy, and medication compared
- Risks, recovery, and long-term expectations
What weight regain means after bariatric surgery
One of the biggest mistakes in this topic is treating any upward move on the scale as proof that bariatric surgery stopped working. That is not how long-term weight regulation usually works. Most patients lose weight rapidly, reach a lowest weight somewhere around 12 to 24 months depending on the operation, and then experience some degree of drift upward. A small rebound is common. The harder question is when that rebound becomes clinically important.
There is no single universal definition of weight regain after bariatric surgery. Some practices look at the percentage regained from nadir weight. Others pay more attention to whether obesity-related conditions are returning, whether eating capacity has clearly changed, or whether the patient has lost enough of the original benefit that daily life and health are worsening again. That variability matters, because patients often hear dramatically different opinions depending on where they are seen.
A practical way to think about it is this: revision is more likely to come up when weight regain is sustained, not just a temporary fluctuation, and when it is paired with one or more of the following:
- return of type 2 diabetes, sleep apnea, hypertension, or fatty liver concerns
- severe reflux, especially after sleeve gastrectomy
- loss of satiety and ability to eat far more than before
- an anatomical problem such as sleeve dilation, enlarged pouch, enlarged gastrojejunal outlet, or fistula
- repeated failure of structured non-surgical treatment after the reasons for regain are properly assessed
This is why the best conversations about revision do not start with “How many pounds did you regain?” They start with “What changed?” The answer may be anatomy. It may be gradual grazing, liquid calories, alcohol, medication-related gain, untreated depression, binge-type eating, loss of follow-up, or a combination of several factors. Many patients need a broader evaluation of weight regain after bariatric surgery before deciding whether another procedure makes sense.
Another important point is that revision is often more helpful when there was a good initial response followed by later recurrence than when the first operation never produced meaningful loss at all. That is not an absolute rule, but it is useful. If the first surgery worked well for a period and then anatomy or physiology changed, a targeted revision may solve a real problem. If the first surgery never produced meaningful adherence, follow-up, or response, a second operation alone may disappoint.
That distinction matters because revision works best as part of long-term obesity treatment, not as a rescue attempt driven only by frustration with the scale.
When revision surgery should be considered
Revision bariatric surgery is usually considered when there is a clear reason to believe another intervention can meaningfully improve outcomes. That reason may be weight recurrence, inadequate initial weight loss, uncontrolled reflux, mechanical problems, or recurrence of major comorbidities. The key word is clear. Good candidates are not simply people who want faster weight loss again. They are people whose current anatomy, symptoms, and treatment history suggest that another procedure could solve a defined problem.
That often means the discussion becomes more specific than patients expect. After sleeve gastrectomy, severe reflux can be just as strong a reason for revision as weight regain. After Roux-en-Y gastric bypass, weight recurrence may be driven by an enlarged outlet or pouch, but in other patients it may have much more to do with eating pattern drift or the natural biology of chronic obesity. Those are not the same situation, and they should not lead automatically to the same recommendation.
In general, revision moves higher on the list when:
- the regain is substantial and sustained rather than a short plateau or seasonal fluctuation
- obesity-related health problems are returning or not well controlled
- imaging or endoscopy shows an anatomical target that fits the symptoms
- lifestyle, nutritional, and behavioral contributors have been addressed honestly
- the patient understands that a second procedure usually brings more risk and less predictability than the first
That last point is easy to underestimate. Revision can be very effective, but the benefit is not usually a replay of the original “honeymoon” phase. Secondary loss may be slower, smaller, or more dependent on ongoing medical and behavioral support. A realistic patient often does better than a highly hopeful but poorly prepared one.
It is also important to recognize when revision may not be the best first move. If the main issues are medication-related appetite change, untreated binge eating, major depression, heavy alcohol use, chronic liquid calories, or poor follow-up, surgery may not be the most efficient starting point. In some patients, anti-obesity medication is tried before revision or alongside it. That is especially relevant now that GLP-1 medications after bariatric surgery are being used more often for weight recurrence.
A useful rule is this: the more the problem looks anatomical, the more revision rises on the list. The more it looks behavioral, pharmacologic, or metabolic without a correctable anatomical driver, the more important non-surgical treatment becomes. Most real patients land somewhere in the middle, which is why multidisciplinary evaluation matters so much.
How the pre-revision workup is done
A good revision plan starts with a better workup than many patients got before their original surgery. That is not criticism of the first operation. It is simply a reflection of how much more specific the second decision needs to be. Before anyone recommends revision, the team should understand what the original anatomy looks like now, what the patient’s actual daily pattern is, and whether there are nutritional or medical issues that would make another operation less safe or less effective.
A typical pre-revision workup often includes:
- a detailed weight history, including pre-op weight, nadir weight, timing of regain, and return of comorbidities
- a review of the original operative report if available
- nutrition assessment focused on meal structure, protein intake, liquid calories, alcohol, grazing, and tolerance
- behavioral screening for binge eating, depression, anxiety, night eating, trauma history, and follow-up fatigue
- medication review, including drugs that may promote weight gain or have changed absorption after surgery
- lab testing for anemia, iron, B12, folate, vitamin D, calcium, parathyroid hormone, and other deficiencies when relevant
- upper endoscopy and sometimes an upper GI contrast study to evaluate pouch size, sleeve shape, stoma size, reflux, ulcer disease, fistula, or technical problems
This part matters because revision should be matched to the problem. A patient with severe reflux and sleeve anatomy issues may need a very different solution from a patient with a bypass and a clearly enlarged gastrojejunal outlet. Likewise, a patient whose intake is already low but whose nutrition is poor may be a poor candidate for a more malabsorptive revision.
This is also where red flags show up. Persistent vomiting, ulcer symptoms, severe reflux, abdominal pain, dysphagia, or anemia can indicate more than simple regain. A careful review of bariatric surgery complications is sometimes just as important as the weight discussion itself. In bypass patients especially, marginal ulcers, fistulas, and internal hernia symptoms need to be taken seriously.
Medication review is another underappreciated step. After sleeve or bypass, not every medication behaves the same way it did before surgery. Extended-release products, acid-dependent drugs, and some supplements may need a second look. That is one reason some centers revisit medication absorption after bariatric surgery before finalizing a revision plan.
The most useful insight from this workup is often not “you need another surgery.” It is “you need a specific kind of surgery,” or sometimes “you are not ready for revision yet because the main problem is somewhere else.” That is a good outcome, not a delay tactic. Revision decisions are safest when they are narrow, targeted, and evidence-based rather than driven by desperation.
Options after sleeve gastrectomy
Sleeve gastrectomy creates one of the most common revision pathways in bariatric practice. The reason is not that sleeves are poor operations. It is that they are widely used, and over time some patients develop substantial reflux, weight recurrence, or both. When that happens, the best revision depends heavily on what is driving the problem.
If reflux is prominent, conversion to Roux-en-Y gastric bypass is often the most common and most practical choice. That is because it can address two issues at once: persistent reflux from sleeve anatomy and the need for additional weight control. This is the most important nuance after sleeve. A revision that is best for extra weight loss is not always the revision that is best for reflux, and vice versa. Patients with severe heartburn, regurgitation, esophagitis, or Barrett-related concerns often end up favoring bypass even if another malabsorptive option might produce greater secondary weight loss.
If reflux is not the dominant issue and the main goal is stronger weight loss, more malabsorptive conversions may enter the conversation. These include SADI-S and biliopancreatic diversion with duodenal switch–type procedures. In selected patients, these can produce more additional weight loss than conversion to bypass, but that benefit comes with a real trade-off: more nutritional surveillance, higher risk of protein and micronutrient deficiencies, and less room for casual follow-up. Patients thinking about stronger bypass-type revisions often benefit from reviewing the basics of bariatric surgery options and the specific profile of SADI-S before deciding.
Re-sleeve is sometimes discussed when the sleeve is clearly enlarged and the patient initially did well, but it is not the universal answer many people expect. It may be reasonable in carefully selected anatomy, yet it does not help reflux and may not match the long-term power of conversion procedures. The risk profile also deserves respect because staple-line revision is not trivial.
A practical way to view sleeve revision is that it usually falls into one of three buckets:
| Primary problem | Often considered option | Main advantage | Main trade-off |
|---|---|---|---|
| Severe reflux with regain | Conversion to Roux-en-Y gastric bypass | Addresses reflux and can add weight loss | More complex surgery than the original sleeve |
| Major weight recurrence without dominant reflux | SADI-S or duodenal switch–type conversion | Usually stronger secondary weight loss | Higher nutritional and malabsorption burden |
| Dilated sleeve in selected anatomy | Re-sleeve or endoscopic sleeve revision | Preserves sleeve-based anatomy | Less useful for reflux and not right for every case |
The main strategic point after sleeve is simple: do not choose a revision based only on which operation sounds strongest. Choose the operation that matches the dominant failure pattern. That usually leads to better outcomes and fewer regrets.
Options after Roux-en-Y gastric bypass
Revision after Roux-en-Y gastric bypass is usually more nuanced than many patients expect. Bypass is already a mixed restrictive and malabsorptive operation, so second-stage options often involve either tightening a part of the anatomy, changing limb length, or using endoscopy rather than another major reconstruction. The right option depends on what has actually changed.
One common driver of regain after bypass is enlargement of the gastrojejunal outlet, sometimes along with pouch enlargement. When that happens, endoscopic treatment often enters the discussion early. Transoral outlet reduction, commonly called TORe, is used to reduce the outlet size and restore more restriction and satiety without another abdominal operation. It tends to be less invasive than surgical revision and is especially relevant when anatomy suggests that the outlet is part of the problem. Patients comparing routes after bypass often want a separate look at endoscopic revision after bariatric surgery because it occupies an important middle ground between medication and surgery.
Surgical revision after bypass may involve pouch revision, gastrojejunal revision, limb distalization, or more complex conversion strategies. These options can produce additional weight loss, but they also raise the nutritional stakes. Distalization, for example, can increase malabsorption and may be powerful in selected patients with severe recurrence, but it also increases the risk of diarrhea, protein malnutrition, fat-soluble vitamin deficiency, and ongoing surveillance burden. That can be acceptable in the right patient and a poor fit in the wrong one.
Another important issue after bypass is that weight regain is not always the only problem. Some patients also have marginal ulcers, fistulas, dumping symptoms, post-prandial hypoglycemia, or chronic abdominal complaints. Those findings can change the revision plan completely. A patient with an enlarged outlet and dumping may be very different from a patient whose main issue is major regain with intact anatomy and poor dietary structure.
That is why bypass revision is usually less about “What is the standard next surgery?” and more about “Which part of the current anatomy is failing?” A few patterns are common:
- enlarged outlet with prior good response often points toward endoscopic outlet reduction
- enlarged pouch or clear technical issue may push toward surgical pouch or anastomotic revision
- major weight recurrence with severe obesity and metabolic relapse may lead to discussion of distalization or another more malabsorptive strategy
- symptoms suggesting ulcer, fistula, or complication require correction of the complication, not just a weight-loss plan
The big practical lesson is that revision after bypass often becomes less predictable as the anatomy becomes more complex. Weight loss may still improve, but the price of stronger metabolic effect is usually stronger nutritional risk. That is why bypass revision should be chosen with more caution than enthusiasm.
Surgery, endoscopy, and medication compared
Patients often think the choice is between “do revision” and “do nothing.” In reality, the more useful comparison is between three categories of treatment: revisional surgery, endoscopic revision, and medical treatment with structured follow-up. Each has a place, and the smartest choice is often the one that matches the size of the problem rather than the one that sounds most aggressive.
Surgical revision is usually the strongest option when there is a major anatomical or symptom-based reason to change the original operation. It can produce the most meaningful additional weight loss, especially when converting a sleeve to a more malabsorptive procedure. It is also the main path when reflux, severe technical issues, or very high BMI recurrence make smaller interventions unlikely to be enough. The downside is obvious: more scar tissue, more operative complexity, longer recovery, and higher complication risk than with primary surgery.
Endoscopic revision is usually best understood as the middle option. It tends to make the most sense when the anatomy problem is real but limited, such as an enlarged outlet after bypass or a sleeve that may be amenable to endoscopic remodeling. It is less invasive, usually easier to recover from, and can be a good choice for patients who want a lower-risk approach or are not ideal candidates for another full operation. The trade-off is that weight loss is often more modest than with major surgical conversion.
Medication sits on the same decision tree, not outside it. Some patients with regain after surgery respond well to anti-obesity medication, especially when appetite, food noise, or slowed satiety are driving the recurrence more than a dramatic anatomical failure. In others, medication is used before revision to test whether the regain can be controlled less invasively. In still others, medication is added after endoscopic or surgical revision to protect the result.
| Approach | Often best for | Main upside | Main limitation |
|---|---|---|---|
| Revisional surgery | Clear anatomical failure, severe reflux, major recurrence, or need for stronger metabolic effect | Usually the most powerful secondary intervention | Higher risk and more nutritional burden |
| Endoscopic revision | Selected outlet or sleeve anatomy changes with a desire for less invasive treatment | No abdominal reoperation and faster recovery | Usually less weight loss than major surgery |
| Medication and intensive follow-up | Appetite-driven recurrence, mixed behavioral and biologic relapse, or patients not ready for revision | Least invasive and can be combined with other treatments | May be insufficient when anatomy is the main problem |
The most useful mindset is not choosing the biggest treatment first. It is choosing the smallest treatment that has a realistic chance of solving the real problem. That tends to reduce regret, preserve options, and keep the long-term plan more sustainable.
Risks, recovery, and long-term expectations
Revisional bariatric surgery is generally safe in experienced hands, but it is more complex than primary surgery. That complexity matters. Scar tissue, changed anatomy, prior staple lines, altered blood supply, and nutritional vulnerability all make the second procedure different from the first. Patients should go into revision expecting a more careful risk-benefit conversation, not a routine redo.
The main risks vary by procedure, but they can include:
- leak, bleeding, infection, and readmission
- stricture, ulcer, reflux issues, or internal hernia depending on the anatomy
- diarrhea, protein-calorie malnutrition, and fat-soluble vitamin deficiency after more malabsorptive revisions
- persistent nausea, food intolerance, or dehydration
- disappointment if expectations were set as though revision would recreate primary-surgery results
That last point deserves emphasis. Revision can work very well, but the goal is usually improvement, not perfection. A strong result may mean meaningful secondary loss, better satiety, improved reflux, and regained control rather than returning to the lowest weight ever reached. Patients who understand that tend to judge outcomes more accurately and stay more engaged with follow-up.
Recovery also depends on what is done. Endoscopic revision is often faster to recover from than full surgical conversion. Laparoscopic revisional surgery may still involve a short hospital stay and a few weeks of fatigue or diet progression. More malabsorptive conversions demand closer long-term monitoring because they do not stop being high-maintenance once the incisions heal.
Long-term success after revision depends heavily on the same fundamentals that matter after primary bariatric surgery:
- consistent protein intake
- structured meals rather than continual grazing
- lifelong vitamin and mineral supplementation
- periodic lab monitoring
- honest follow-up when symptoms, reflux, or regain start returning
- willingness to combine surgery with medication, nutrition care, or behavioral treatment when needed
That is why patients preparing for revision often need to revisit both protein after bariatric surgery and the basics of bariatric vitamins. The revision may change the anatomy, but long-term success still depends on what happens every day after the procedure.
A useful final question for any consultation is not just “What operation would you do?” but also “What problem are you trying to solve, how much extra loss is realistic, and what lifelong trade-off comes with that choice?” If the answers are clear, revision may be a smart next step. If the answers are vague, more workup is usually needed before another operation is worth the risk.
References
- 2022 American Society for Metabolic and Bariatric Surgery (ASMBS) and International Federation for the Surgery of Obesity and Metabolic Disorders (IFSO): Indications for Metabolic and Bariatric Surgery 2022 (Guideline)
- Revisional Procedures after Sleeve Gastrectomy for Weight Recurrence or Inadequate Weight Loss: An Analysis of the MBSAQIP Database 2023 (Database Analysis)
- Revision procedures after initial Roux-en-Y gastric bypass, treatment of weight regain: a systematic review and meta-analysis 2021 (Systematic Review and Meta-analysis)
- Endoscopic Management of Weight Recurrence Following Bariatric Surgery 2022 (Review)
Disclaimer
This article is for general educational purposes only. Revision bariatric surgery is a specialized medical decision that should be made with a bariatric surgeon and multidisciplinary team after review of your anatomy, nutrition, symptoms, and health history. It is not a substitute for personal medical advice, diagnosis, or treatment.
If you found this article useful, please consider sharing it on Facebook, X, or your preferred platform.