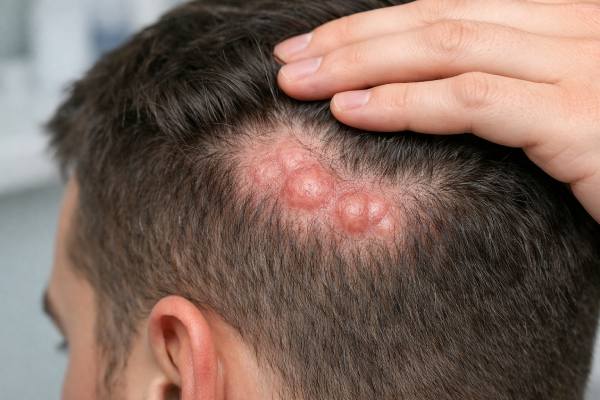
Dissecting cellulitis of the scalp is a rare but life-disrupting inflammatory condition that can start like a few tender bumps and progress into deep nodules, draining tunnels under the skin, and permanent scarring hair loss. It is sometimes called “Hoffman disease” or “perifolliculitis capitis abscedens et suffodiens,” and it belongs to a group of disorders driven by follicle blockage and rupture. What makes it especially challenging is that it often looks like an infection, yet the core issue is not simple “dirty scalp” or routine folliculitis.
The most important message is also the most practical: early recognition and proper treatment can reduce pain, limit drainage, and help prevent the irreversible stage—cicatricial (scarring) alopecia. This article explains what to watch for, what a dermatologist looks for, and which treatments are most commonly used, from topical care and oral medications to procedures when disease is advanced. You will also learn how to protect the scalp between flares and when urgent evaluation matters.
Quick Facts
- Dissecting cellulitis causes painful nodules and abscesses that can form draining sinus tracts and lead to permanent scarring hair loss.
- It often flares in cycles, and delays in treatment increase the chance of irreversible alopecia.
- Care usually requires prescription therapy, often combining anti-inflammatory and antimicrobial approaches.
- Do not squeeze or “drain” lesions at home; seek dermatology care early for a tailored plan.
- Gentle cleansing, avoiding scalp trauma, and consistent follow-up reduce recurrence and complications.
Table of Contents
- What dissecting cellulitis of the scalp is
- Painful nodules, drainage, and how it progresses
- Why it happens and who is at risk
- How it is diagnosed and what it can mimic
- Treatment options from medications to procedures
- Long-term care to limit scarring and relapse
What dissecting cellulitis of the scalp is
Dissecting cellulitis of the scalp is a chronic, inflammatory disorder centered on hair follicles. Despite the name, it is not the same as typical bacterial “cellulitis” of the skin. The condition begins in and around follicles, then spreads into deeper tissue as inflammation intensifies. Over time, this can create boggy, tender areas, interconnected tunnels (sinus tracts), and scarring that permanently damages follicles.
You may also see it described by older or alternate names:
- Perifolliculitis capitis abscedens et suffodiens (often shortened to PCAS)
- Hoffman disease
- Dissecting folliculitis
Clinically, it is often grouped within the “follicular occlusion” family of disorders—conditions where follicles become blocked, rupture, and trigger an exaggerated inflammatory response. In that cluster, it is common to see overlap with nodulocystic acne, hidradenitis suppurativa, or pilonidal disease. When these conditions co-exist, treatment decisions often need to account for the whole pattern, not just the scalp.
A helpful way to understand dissecting cellulitis is to separate the early and late stages:
- Early stage: inflamed follicular bumps or pustules, localized tenderness, intermittent flares, and minimal scarring.
- Progressive stage: deeper nodules and abscesses, drainage, and the start of sinus tracts.
- Late stage: scarring alopecia, thickened or uneven scalp texture, and fewer “active” follicles in affected zones.
Because scarring alopecia is irreversible in the areas where follicles are destroyed, timing matters. The goal is to calm inflammation before tunnels and scars dominate. That does not always mean aggressive treatment immediately, but it does mean you should take recurring painful nodules seriously and avoid months of DIY experimentation.
It is also important to know what dissecting cellulitis is not. It is not caused by poor hygiene, and it is rarely fixed by changing shampoos alone. Cleansing and topical care can support comfort, but most moderate to severe cases need prescription therapy to reduce inflammation and prevent structural damage to the scalp.
Painful nodules, drainage, and how it progresses
The symptom pattern of dissecting cellulitis is distinctive once you know what to look for: pain first, then swelling and drainage, then scarring hair loss. Many people describe the scalp as tender “from the inside,” with lesions that feel deeper than typical pimples.
Common symptoms include:
- Painful, firm or fluctuant nodules (often on the vertex or occipital scalp)
- Abscess-like lumps that may enlarge over days to weeks
- Drainage of pus or blood-tinged fluid, sometimes with a noticeable odor
- Crusting at the surface after drainage
- Itch that tends to be secondary to inflammation, not the main symptom
- Areas where hair thins, breaks, or stops growing due to scarring
As disease progresses, sinus tracts can form—channels under the skin that connect multiple lesions. This is one reason the condition can feel as if it “moves” across the scalp. The skin may look swollen or “boggy,” and pressure on one area can sometimes express fluid from another. Those tunnels are a major reason home squeezing is risky: it can widen inflammation, increase tissue trauma, and worsen scarring.
Many people notice flares that follow recognizable triggers:
- Heat and sweating, especially under hats or helmets
- Close shaving or frequent scalp friction
- Stress, sleep disruption, or illness
- Smoking, which is associated with worse outcomes in several follicular occlusion disorders
- Delayed treatment after early symptoms start
Pain deserves special attention because it is often the earliest warning sign that inflammation is deep. If you have burning, tenderness, or “bruised” scalp discomfort, it can help to compare symptoms with other causes of scalp pain so you can recognize when a deeper inflammatory condition is more likely than simple sensitivity. A practical overview is in burning scalp sensations and common triggers.
Hair loss in dissecting cellulitis can be confusing: early on, shedding may be mild even when pain is intense. Later, hair loss becomes more visible, but some of that loss is now permanent because follicles have been replaced by scar tissue. This is why the best “hair growth” strategy is not a supplement—it is controlling inflammation quickly and consistently.
Finally, the psychological load is real. Drainage, odor concerns, visible scalp changes, and unpredictable flares can affect work, relationships, and confidence. A good treatment plan should address pain control and quality of life alongside the skin findings. If pain and drainage are severe, seeking dermatology care sooner rather than later is not just medical—it is practical.
Why it happens and who is at risk
The exact cause of dissecting cellulitis is not fully understood, but most experts describe a multi-step process: follicle blockage, follicle rupture, and an intense inflammatory response that spreads beyond the follicle. This “follicular occlusion” framework explains why the condition can behave like a recurring abscess problem even when standard hygiene measures are excellent.
Key contributors that are commonly discussed include:
1) Follicle occlusion and rupture
Follicles can become plugged by keratin and sebum. When that plug persists, the follicle expands, weakens, and can rupture. Once follicular contents spill into surrounding tissue, the immune system treats it as a major inflammatory event.
2) Immune and microbiologic factors
Bacteria are often present in draining lesions, but they are not always the original driver. In many cases, bacteria may represent secondary colonization that worsens inflammation rather than starting it. This is part of why antibiotics can help some people (reducing bacterial load and inflammation) but do not always create lasting remission on their own.
3) Genetics and hair and scalp characteristics
Dissecting cellulitis is reported more often in young adult men and is frequently described in Black men, though it can affect any sex and any ethnicity. Hair grooming practices that increase scalp trauma—such as very close shaving—may contribute to follicle injury in vulnerable scalps.
4) Overlap with follicular occlusion disorders
Some people have dissecting cellulitis alongside hidradenitis suppurativa or severe acne. When that happens, treatment often needs to be coordinated, because therapies like retinoids or biologics may be chosen to address multiple sites of disease.
5) Lifestyle and systemic factors
Smoking is frequently cited as a risk factor for more severe disease or poorer control in follicular occlusion conditions. If you smoke and are dealing with recurrent inflammatory scalp disease, the link between tobacco exposure and hair and scalp outcomes is worth understanding, and how smoking affects hair and follicles provides a clear overview.
It is also important to avoid a common misconception: dissecting cellulitis is not caused by “dirty hair.” Overwashing and harsh scrubbing can actually irritate the scalp barrier and worsen symptoms. The goal is gentle, consistent scalp care plus medical therapy that reduces the deeper inflammatory process.
If you are trying to identify your own risk, focus less on a single factor and more on the pattern: deep painful nodules, recurrent drainage, and areas of hair loss that start to look scar-like. That pattern is a strong signal that you need evaluation rather than trial-and-error.
How it is diagnosed and what it can mimic
Diagnosis usually begins with a careful scalp exam and a history that focuses on three questions: how long lesions have been recurring, whether there is drainage or tunnels, and whether hair loss looks scarring. Dermatologists often recognize dissecting cellulitis clinically, but testing can help confirm the diagnosis and rule out look-alikes.
Common parts of the evaluation include:
1) Visual and tactile scalp exam
A clinician looks for:
- Boggy nodules and fluctuant abscesses
- Sinus openings or multiple points of drainage
- Scarring alopecia (areas where follicle openings appear reduced)
- Patterns of involvement (often vertex and occiput)
2) Cultures when drainage is present
Swabs may be taken to guide antibiotic selection if infection is suspected or if lesions are actively draining. A positive culture does not necessarily mean the condition is “just infection,” but it can affect treatment choices.
3) Trichoscopy or dermoscopy
Scalp magnification may show follicular changes, scarring patterns, and inflammatory features that support the diagnosis.
4) Biopsy in unclear cases
A scalp biopsy can be useful when the diagnosis is uncertain, when multiple conditions may be overlapping, or when scarring alopecia needs classification. If you are curious what a biopsy can reveal and how results are interpreted, understanding scalp biopsy results offers a helpful framework.
What it can mimic
Dissecting cellulitis is most often confused with:
- Folliculitis decalvans: another neutrophilic scarring alopecia that can involve pustules and crusting, often with tufted hairs. A detailed comparison is in folliculitis decalvans symptoms and diagnosis.
- Tinea capitis: fungal infection that can cause scale, broken hairs, and inflammatory masses (kerion).
- Bacterial abscesses or recurrent infected cysts: especially if lesions are localized.
- Acne keloidalis nuchae: typically at the nape with firm papules and keloidal plaques.
- Scalp psoriasis or severe seborrheic dermatitis: usually more scale than deep nodules, though overlap can occur.
- Erosive pustular dermatosis or other inflammatory scalp conditions: particularly in older adults.
Because dissecting cellulitis can scar, it is safer to over-escalate evaluation than to under-evaluate. If you have deep pain, drainage, or a sense that lesions “connect,” those are not typical dandruff or mild folliculitis symptoms. Early dermatology assessment is one of the most protective steps you can take for long-term hair preservation.
Treatment options from medications to procedures
Treatment is usually individualized based on severity, presence of sinus tracts, and whether scarring alopecia is already present. Most plans combine approaches that reduce inflammation, limit secondary infection, and prevent new follicle rupture. The goal is fewer flares, less pain, and less progression into scarring.
Topical and supportive care
For milder disease or as add-on therapy, clinicians may use:
- Antiseptic or antimicrobial washes to reduce surface bacterial load
- Topical antibiotics for pustules or superficial infection patterns
- Intralesional corticosteroid injections for tender nodules
- Gentle cleansing and avoidance of mechanical trauma
Supportive care matters because people often make symptoms worse by trying to “scrub out” drainage or flaking. If your scalp has bumps, crusting, and tenderness, a safe baseline routine is often similar to what is recommended for inflammatory follicle conditions—gentle cleansing, minimal friction, and avoiding picking. A practical guide is scalp folliculitis bump care and treatment options, which can help you avoid common mistakes while you pursue definitive diagnosis and therapy.
Systemic antibiotics
Oral antibiotics are frequently used for anti-inflammatory benefit and to manage secondary infection. Options may include tetracyclines or combination regimens in more persistent disease. The choice depends on prior therapies, cultures, and tolerance.
Oral retinoids
Isotretinoin is commonly discussed in dissecting cellulitis because it can reduce follicular occlusion and sebaceous activity. It is not appropriate for everyone, and it requires monitoring and strict pregnancy prevention protocols where relevant. When it works, it often reduces active inflammation and new lesion formation, though relapses can occur after stopping.
Biologic and targeted immunomodulating therapies
For refractory disease, especially when there is overlap with hidradenitis suppurativa or severe inflammatory disease, biologic therapies may be considered. These can include tumor necrosis factor inhibitors and other targeted agents. This area is evolving quickly, and dermatologists often base decisions on disease severity, comorbidities, and the growing published experience.
Procedures
Procedures may be considered when disease is localized, when sinus tracts are extensive, or when medical therapy is not sufficient:
- Incision and drainage may provide short-term relief but does not treat the underlying condition and can recur.
- Laser-based approaches may help in selected cases by targeting follicles and reducing disease activity.
- Surgical excision can be an option for severe, scarring, refractory areas, often followed by reconstruction strategies.
Pain control and infection safety
Pain management should be part of the plan, not an afterthought. Warm compresses, appropriate analgesics, and prompt treatment of secondary infection can prevent spirals of worsening inflammation. Avoid squeezing or attempting to “tunnel clean” lesions at home; it increases trauma and scarring risk and can spread infection if present.
A realistic expectation is that treatment is often staged: an initial “calm the fire” phase, followed by a maintenance phase to prevent relapse. Consistency matters more than finding one perfect product.
Long-term care to limit scarring and relapse
Because dissecting cellulitis can become scarring, long-term care is as much about prevention as it is about flare treatment. Even when symptoms quiet down, the scalp remains vulnerable to recurrence if triggers and maintenance plans are not addressed.
What “remission” often means
Many people experience periods with no active drainage or severe pain, but the condition can relapse. The aim is durable control:
- Fewer inflammatory nodules
- No new sinus tracts
- Minimal pain and tenderness
- Stable hair density outside scarred areas
Scarring and regrowth expectations
Hair can regrow in areas where follicles are inflamed but not destroyed. Hair does not regrow in fully scarred zones where follicles have been replaced by fibrous tissue. This is why early control is so valuable: it protects follicles before they are permanently lost.
Maintenance habits that protect the scalp
- Keep cleansing gentle and consistent, especially after sweating.
- Avoid close shaving, harsh scalp scrubs, and frequent friction from tight hats or helmets.
- Treat flares early rather than waiting for drainage and tunnels.
- Use only a small number of products and avoid irritants if your scalp is reactive.
Monitoring without spiraling
Monthly photos of the same scalp zones can help you spot trends—new areas of redness, enlarging nodules, or expanding alopecia—without the stress of daily checking. If you notice increasing pain or tenderness, treat it as a signal to contact your clinician rather than simply switching shampoos.
When urgent care is appropriate
Seek prompt medical evaluation if you develop:
- Rapid swelling, spreading redness, fever, or chills
- Severe pain that escalates quickly
- Large areas of pus, foul-smelling drainage, or signs of systemic illness
- Sudden patchy hair loss beyond known affected zones
When specialist care should not be delayed
If you suspect scarring alopecia or you have recurring painful nodules for more than a few weeks, it is appropriate to seek dermatology evaluation rather than waiting. Guidance on escalation and red flags is summarized in when to see a dermatologist for hair loss concerns, and the principles apply strongly to scarring conditions.
Dissecting cellulitis can be emotionally heavy, but it is not hopeless. Many patients achieve meaningful relief and stability with consistent, specialist-guided treatment. The earlier that process starts, the better the odds of protecting remaining follicles and minimizing permanent change.
References
- Treatments for Dissecting Cellulitis of the Scalp: A Systematic Review and Treatment Algorithm 2023 (Systematic Review)
- Dissecting cellulitis of the scalp: clinical characteristics and impact on quality of life of 66 Brazilian patients 2024 (Observational Study)
- DISSECTING CELLULITIS OF THE SCALP 2022 (Guideline)
- A systematic review of tumor necrosis factor-α blockers, anti-interleukins, and small molecule inhibitors for dissecting cellulitis of the scalp treatment 2025 (Systematic Review)
Disclaimer
This article is for educational purposes and does not provide medical advice, diagnosis, or treatment. Dissecting cellulitis of the scalp is a potentially scarring inflammatory condition that can resemble infection and may require prescription medications, procedures, and ongoing monitoring. Do not squeeze, lance, or attempt to drain scalp nodules at home, and do not start or stop prescription treatments without guidance from a qualified clinician. Seek urgent care for fever, rapidly spreading redness, severe escalating pain, or signs of systemic illness. If you are pregnant, breastfeeding, immunocompromised, or taking medications that affect immunity, consult a healthcare professional promptly for individualized guidance.
If this article helped you recognize warning signs or feel more prepared for treatment, consider sharing it on Facebook, X (formerly Twitter), or your preferred platforms so others can seek timely care and reduce the risk of permanent hair loss.






