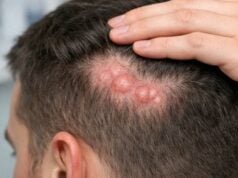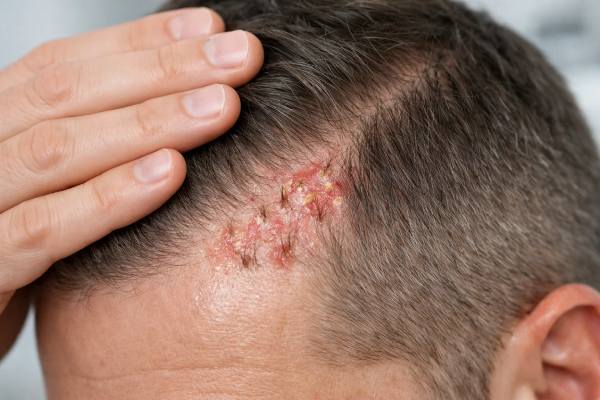
Folliculitis decalvans is an uncommon but important cause of permanent scalp hair loss. It does not behave like ordinary dandruff, a few scalp pimples, or routine shedding. Instead, it is a chronic inflammatory disorder in which painful or itchy follicular pustules, crusting, and repeated flares gradually damage the follicle and replace it with scar tissue. That combination makes early recognition especially valuable: the main goal is not simply to calm the scalp for a few days, but to stop ongoing destruction before more hair is lost for good.
For many people, the hardest part is that the condition can look deceptively familiar at first. It may start as tenderness, bumps, or patchy thinning at the crown or back of the scalp, then slowly reveal a more specific pattern such as tufted hairs and shiny scarred areas. Understanding what folliculitis decalvans looks like, how it is diagnosed, and which treatments are used can make the path forward far clearer and far more realistic.
Quick Overview
- Folliculitis decalvans is a chronic scarring scalp disorder, so early treatment can limit permanent hair loss.
- Recurrent pustules, crusts, tenderness, and clusters of hairs growing from one opening are key clues.
- Treatment usually aims to control inflammation and prevent spread rather than restore hair in fully scarred areas.
- Flares often need prescription treatment, and self-treating it as simple dandruff can delay diagnosis.
- Taking scalp photos every 4 weeks can make it easier to track whether inflammation is improving or expanding.
Table of Contents
- What Folliculitis Decalvans Actually Is
- Symptoms and Early Warning Signs
- Why It Happens and Who Gets It
- How the Diagnosis Is Confirmed
- Treatment Options and What Results Are Realistic
- Long-Term Outlook and Daily Management
What Folliculitis Decalvans Actually Is
Folliculitis decalvans is a primary neutrophilic scarring alopecia, which means the disease begins around the hair follicle itself, attracts a strong inflammatory response, and can leave permanent bald areas once follicles are destroyed. That is the central fact readers need to understand from the start: this is not just a temporary scalp irritation. It is a relapsing inflammatory condition that can move in cycles of activity and quiet, with each active phase carrying a risk of additional scarring.
The disorder most often affects the scalp, especially the crown and occipital area, although the exact pattern varies. In active disease, the skin may show follicular pustules, perifollicular redness, yellowish crusts, tenderness, and a sense that the scalp is inflamed even before hair loss becomes dramatic. Over time, damaged areas may become smoother, shinier, and less able to grow hair because the follicular openings are partly or completely lost.
One of the most recognizable features is tufting. Instead of each hair emerging from its own opening, several hairs appear to come out together from a single widened follicular opening. This “doll’s hair” or tufted look is highly suggestive, though it is not exclusive to folliculitis decalvans and has to be interpreted with the rest of the exam.
A common point of confusion is the name itself. “Folliculitis” makes many people assume this is just a simple infection of the hair follicles. In reality, the picture is more complex. Bacteria, especially Staphylococcus aureus, may play an important role in some patients, but the disease is not simply a matter of poor hygiene or a minor skin infection that disappears with a few washes. It behaves more like a chronic inflammatory follicular disease with microbial and immune components.
That distinction matters because the treatment goals are different from those for ordinary scalp folliculitis. In folliculitis decalvans, doctors aim to reduce inflammation, suppress new pustules and crusting, relieve symptoms, and most importantly prevent the scarred area from widening. Once a follicle is replaced by scar tissue, full regrowth is not a realistic expectation. However, hair at the edge of active inflammation may still be salvageable if treatment begins early enough.
This is why prompt recognition changes the conversation. The earlier the condition is identified, the better the chance of preserving still-living follicles and avoiding the frustration of repeated cycles of partial improvement followed by silent progression.
Symptoms and Early Warning Signs
Folliculitis decalvans often announces itself before the person realizes that hair loss is part of the problem. The earliest complaint may be a scalp that feels sore, itchy, burning, or unusually tender when brushing, washing, or lying on a pillow. Then come the visible changes: recurring pustules around follicles, crusting, areas of redness, and patches where hair density starts to look uneven.
Unlike diffuse shedding, this condition usually creates a more inflammatory picture. People may notice:
- painful or itchy bumps centered on hair follicles
- yellow or honey-colored crusts
- small pustules that recur in the same area
- patchy hair loss that slowly expands
- hairs emerging in clusters from one opening
- smooth or shiny areas where the skin looks scarred
- occasional bleeding or oozing after scratching or picking
The course is often chronic rather than explosive. A patch may improve, then flare again weeks later. New pustules may appear at the border while the center becomes more scarred and sparse. That edge-versus-center contrast is useful: active inflammation tends to sit at the margins, while older damage sits in the middle.
One reason diagnosis is delayed is that the symptoms overlap with more common scalp problems. Ordinary scalp folliculitis can also cause bumps and tenderness, and a guide to common scalp folliculitis bumps and treatment patterns can help explain why the two are not the same condition. Seborrheic dermatitis may cause flaking and itch. Psoriasis can create thick scale and soreness. Dissecting cellulitis can produce painful nodules and drainage. Tinea capitis can mimic inflammatory patchy loss in some patients. The difference is that folliculitis decalvans tends to keep returning in the same zones and leaves scarring behind.
The hair itself may also change in ways that are easy to miss. Instead of simple shedding, the scalp can look as if density is breaking apart into islands. Some hairs remain in tight grouped tufts while nearby follicles disappear. In more advanced disease, the skin may look smooth and pale compared with surrounding scalp, signaling established scar formation.
Pain is another important clue. Not every patient has significant discomfort, but when hair loss is accompanied by burning, tenderness, or a raw sensation, it should raise suspicion for an inflammatory cicatricial process rather than routine thinning.
A practical way to catch progression earlier is to look for pattern, not just severity. A few pustules on one day are less informative than the same area flaring again and again over months. Taking scalp photos in consistent lighting every few weeks can reveal widening patches, more crusting, or increased tufting long before those changes feel obvious in the mirror.
When recurrent inflammation and hair loss travel together, the question should not be “Which shampoo should I try next?” but “Could this be a scarring alopecia?” That shift in thinking often leads to faster diagnosis and less permanent loss.
Why It Happens and Who Gets It
The exact cause of folliculitis decalvans is still not fully settled, and that uncertainty is one reason treatment can be challenging. Most experts view it as a disease driven by a mix of abnormal host response and microbial factors rather than a single simple trigger. In other words, the scalp is not merely infected, and it is not purely autoimmune either. The condition seems to sit in a complicated middle ground.
Staphylococcus aureus has long been linked to folliculitis decalvans, and bacterial involvement remains one of the most important pieces of the puzzle. Yet newer work suggests the microbiology may be more heterogeneous than older descriptions implied. Some patients appear to have an altered follicular microbial environment along with an impaired or dysregulated immune response. That helps explain why antibiotics may help many people, but not always in a durable or uniform way.
Inflammation in this disease is predominantly neutrophilic, meaning neutrophils are a major part of the immune reaction damaging the follicle. When that inflammation keeps recurring, the follicle can be progressively injured and ultimately replaced by scar tissue. By the time the area looks smooth and inactive, the destructive phase may have already done much of its work.
Folliculitis decalvans is often described as more common in adults, especially middle-aged men, but women are affected too, and the condition can appear across a range of skin tones and hair types. It is not limited to one demographic group. Some case series suggest the vertex and occipital scalp are common sites regardless of sex.
What it does not mean is also important. It does not mean the scalp is dirty. It does not mean the person caused the condition by washing too little. It does not automatically mean the disease is contagious. These assumptions can add unnecessary shame and delay medical care. Good scalp hygiene can support comfort and reduce irritants, but hygiene alone does not solve a chronic scarring alopecia.
Mechanical irritation may worsen symptoms in some people even if it is not the root cause. Tight headwear, heavy occlusive products, scratching, aggressive brushing, and picking at crusts can all make an already inflamed scalp harder to settle. The same is true of repeated attempts to “scrub away” lesions with harsh cleansers.
There is also an emotional dimension to the disease. The visible mix of inflammation and patchy scarring can be more distressing than the diagnosis sounds on paper. Some people feel they are dealing with both a skin disease and hair loss at the same time, because that is exactly what is happening.
The most accurate short summary is this: folliculitis decalvans appears to arise from a vulnerable follicle environment in which microbial imbalance and abnormal inflammation feed each other. That ongoing cycle, rather than one isolated event, is what makes the disease chronic and what makes early control so important.
How the Diagnosis Is Confirmed
The diagnosis of folliculitis decalvans starts with pattern recognition, but it should not end there. Because several scalp disorders can mimic one another, confirmation usually comes from a combination of history, close scalp examination, and selected tests rather than a single quick glance.
A dermatologist will usually begin by asking about the timeline. Key questions include whether the same area keeps flaring, whether pustules or crusts appear before hair loss widens, how much pain or burning is present, and whether previous antibiotics or steroid treatments gave only temporary relief. Recurrent inflammation in the same zones is a strong clue.
The scalp exam matters just as much. Doctors look for perifollicular erythema, pustules, crusts, grouped hairs, and scarring. In active areas, the scalp may appear inflamed and tender. In older areas, the skin may look smooth, shiny, or partly devoid of follicular openings. That mixture of ongoing border inflammation and central scarring is highly characteristic.
Trichoscopy, sometimes called scalp dermoscopy, is often the next step. This magnified view can help reveal clustered hair tufts, perifollicular scale, redness, pustules, crusts, and the loss of visible follicular openings in scarred skin. It is especially useful because it can show the difference between active inflammatory disease and older inactive scar. When doctors need tissue confirmation or want to distinguish between different scarring alopecias, a guide to how scalp biopsy results are used in hair loss diagnosis provides helpful context for why biopsy still matters.
A scalp biopsy is not required in every patient, but it is often recommended when the diagnosis is uncertain, when the disease looks atypical, or when there is concern for another cicatricial alopecia such as lichen planopilaris, central centrifugal cicatricial alopecia, or dissecting cellulitis. Biopsy is usually most informative when taken from an active edge rather than from a fully scarred center.
Bacterial culture may also be considered, especially when pustules, crusting, or drainage are prominent. Culture does not diagnose folliculitis decalvans by itself, but it can identify secondary bacterial involvement and help guide antibiotic selection. Blood tests are not the main diagnostic tool for this disease, though they may be ordered if another condition is suspected.
Differential diagnosis is a major part of the workup. Important look-alikes include:
- Dissecting cellulitis of the scalp
- Lichen planopilaris
- Central centrifugal cicatricial alopecia
- Inflamed tinea capitis
- Chronic bacterial scalp folliculitis
- Acne keloidalis nuchae in posterior scalp or neck zones
The goal of diagnosis is not only to attach a name to the condition. It is to determine whether scarring is active, how much inflammation is still present, and how aggressively treatment needs to begin. In a disease where permanent loss can accumulate quietly, precision is more than academic.
Treatment Options and What Results Are Realistic
Treatment for folliculitis decalvans is built around one central objective: stop the inflammatory process before it creates more scarred scalp. That means success is usually measured by fewer pustules, less pain, reduced redness and crusting, and stabilization of the hair-bearing area. Full regrowth in well-established scarred zones is rarely a realistic target.
For active disease, oral antibiotics are commonly used, especially when inflammation is moderate to severe. Tetracycline-class antibiotics are frequently chosen because they can provide both antimicrobial and anti-inflammatory effects. Combination therapy with clindamycin and rifampicin has also been used in many patients, particularly in more persistent disease. These regimens are usually prescribed for a defined course rather than as casual spot treatment.
Oral isotretinoin has emerged as an important option in selected cases, especially when disease is mild but active, or when more conventional antibiotic-based approaches do not produce durable control. In recent expert guidance, isotretinoin is treated less as an afterthought and more as a serious first-line or early-line option for certain patterns of active disease, especially when perifollicular erythema and hyperkeratosis dominate over heavy pustulation.
Topical therapy is usually an adjunct rather than the entire plan. Depending on the presentation, treatment may include topical antibiotics, antiseptic or medicated cleansers, and topical corticosteroids. Intralesional corticosteroid injections may be used for inflamed areas to reduce active perifollicular inflammation. In highly inflamed flares, a short course of oral corticosteroids may sometimes be used to bring the disease under faster control while a longer-term regimen is taking effect.
For refractory cases, treatment may widen. Dermatologists may consider agents such as dapsone, hydroxychloroquine, cyclosporine, or biologic therapy. Adalimumab has drawn attention in severe or treatment-resistant cases, though it is not a routine starting point. Some newer immune-targeting strategies are being discussed for difficult disease, but these remain specialist-level decisions rather than standard first-line care.
Timelines matter. Patients often hope for visible change within days, but a more realistic early window is several weeks. Reduced pustules and tenderness may be the first sign that treatment is working. Stabilization over 6 to 12 weeks is often more meaningful than immediate cosmetic improvement. The hair itself may lag behind the inflammatory response, and scarred areas may not refill even when the disease becomes quiet.
When inflammation has been inactive for a sustained period, procedural options may be discussed for selected patients. These can include surgical excision of very localized disease, laser-based approaches in certain cases, and hair transplantation only when the condition is clearly inactive. If the scalp is still flaring, transplantation is usually postponed because grafts placed into active inflammatory skin are at much higher risk of poor survival.
The most important expectation is honest one: treatment can often control the disease, but it may take time, adjustment, and maintenance. In folliculitis decalvans, stopping progression is often the biggest victory.
Long-Term Outlook and Daily Management
Folliculitis decalvans is usually a chronic relapsing condition, which means long-term management matters as much as the first prescription. Even when a flare settles, the scalp may remain vulnerable, and periods of improvement can be followed by renewed activity. For many patients, the most realistic goal is durable control rather than a permanent one-time cure.
The outlook depends heavily on timing. When diagnosis is made while inflammation is still active but substantial numbers of follicles remain alive, treatment can preserve hair and limit the size of the scarred area. When diagnosis comes late, the disease may already have left stable but permanent gaps. That is why some patients feel better medically long before they feel satisfied cosmetically.
Daily care should be gentle and boring in the best sense. The aim is to avoid additional mechanical stress on an already inflamed scalp. Helpful habits often include:
- washing often enough to remove crusts and product buildup without harsh scrubbing
- avoiding picking, squeezing, or scratching lesions
- limiting heavy occlusive products on inflamed areas
- reporting new tenderness, pustules, or rapid spread early instead of waiting for the next large flare
- using consistent photo tracking to compare the same zones over time
Haircuts and camouflage also deserve attention because appearance affects quality of life. A shorter cut can make patch edges less noticeable for some people, while others prefer longer styles that cover scars. Once disease has been inactive long enough, cosmetic approaches may become part of the plan. In selected stable cases, options such as scalp micropigmentation for scar camouflage may improve confidence even though they do not treat the underlying disease.
Patients should also know when to return promptly. A new increase in pustules, expanding tenderness, more crusting, or fresh loss around the edge of an old patch usually means the disease is active again. Follow-up is particularly important when treatment involves oral antibiotics, isotretinoin, corticosteroids, or other systemic medications that require monitoring and dose adjustments.
The psychological side should not be minimized. Chronic scalp pain, visible crusting, and scarring hair loss can wear people down. A condition does not have to be life-threatening to be deeply disruptive. Clear expectations often help: recently inflamed follicles may recover, but long-standing scar tissue usually will not. That distinction prevents false hope while still leaving room for meaningful improvement.
The long-term message is steady rather than dramatic. Folliculitis decalvans can often be controlled, sometimes for long stretches, but it rewards early action, close follow-up, and practical expectations. In a scarring alopecia, calm disease activity is the foundation on which every other improvement depends.
References
- Management of folliculitis decalvans: The EADV task force on hair diseases position statement 2025 (Guideline)
- Non-invasive Assessment and Management of Folliculitis Decalvans by Trichoscopy and Reflectance Confocal Microscopy 2024 (Clinical Study)
- Folliculitis Decalvans Has a Heterogeneous Microbiological Signature and Impaired Immunological Response 2023 (Observational Study)
- Updates in therapeutics for folliculitis decalvans: A systematic review with evidence-based analysis 2019 (Systematic Review)
- Folliculitis decalvans: Effectiveness of therapies and prognostic factors in a multicenter series of 60 patients with long-term follow-up 2018 (Multicenter Study)
Disclaimer
This article is for educational purposes only and is not a diagnosis or a substitute for medical care. Folliculitis decalvans is a scarring alopecia, so persistent scalp pustules, crusting, pain, or patchy hair loss should be assessed by a qualified dermatologist. Treatment choices depend on clinical exam findings, possible biopsy or culture results, medication risks, and whether the disease is still actively inflaming follicles.
If this article was useful, please share it on Facebook, X, or another platform where it might help someone recognize a scarring scalp condition earlier.