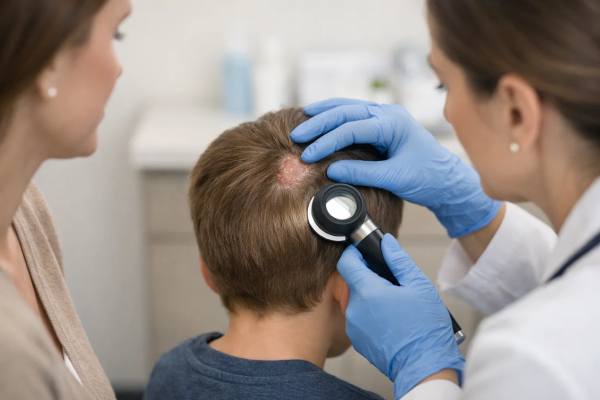
A child with a flaky patch of scalp and a few broken hairs may look as if they simply have dandruff. An adult with a tender, crusted area might be treated for folliculitis or eczema first. But ringworm of the scalp, also called tinea capitis, often hides behind those familiar labels. It is a contagious fungal infection of the scalp and hair shafts, not a worm, and it can spread quickly through close contact, shared grooming items, and sometimes pets.
What makes this condition important is not just the rash. Tinea capitis can cause patchy hair loss, swollen lymph nodes, pain, and, in more inflammatory cases, a boggy mass called a kerion that can raise the risk of scarring if treatment is delayed. The good news is that it is treatable. The key is recognizing the pattern early and understanding that medicated creams alone are usually not enough for scalp infection.
Essential Insights
- Tinea capitis often causes patchy hair loss, scale, broken hairs, and sometimes tender swollen areas on the scalp.
- Prompt treatment usually clears the infection and lowers the chance of lasting hair loss.
- Oral antifungal medicine is usually required because scalp ringworm affects the hair shaft and follicles, not just the surface skin.
- A painful, pus-filled, or rapidly worsening scalp lesion needs medical assessment quickly because kerion can scar.
- If scalp ringworm is suspected, avoid sharing combs, brushes, hats, pillows, and hair accessories until treatment is underway.
Table of Contents
- What tinea capitis is and how it spreads
- Symptoms and signs that stand out
- How diagnosis is confirmed
- What treatment usually involves
- Recovery timeline and possible complications
- How to prevent spread and reinfection
What tinea capitis is and how it spreads
Tinea capitis is a fungal infection caused by dermatophytes, a group of fungi that feed on keratin in skin and hair. On the scalp, that means the infection does not stay on the surface. It can invade the hair shaft and the opening of the follicle, which is why a simple cream or lotion usually does not reach it well enough to clear it.
This infection is most common in children, especially those in the preschool and school-age years, but adults can get it too. Adults are less often diagnosed, which can make the condition easier to miss. In older adults, especially postmenopausal women, tinea capitis can be mistaken for inflammatory scalp disease, seborrheic dermatitis, or bacterial folliculitis.
How it spreads
Tinea capitis is contagious. The fungus spreads through:
- Direct scalp-to-scalp contact.
- Shared combs, brushes, hats, scarves, helmets, pillows, and hair accessories.
- Contact with contaminated barber or salon tools when cleaning is inadequate.
- Contact with infected animals, especially cats, kittens, dogs, and sometimes farm animals.
- Less commonly, contaminated household surfaces, bedding, or upholstery.
Transmission patterns vary by fungal species. Some fungi spread mainly person to person. Others are more often linked to pets or livestock. That is one reason clinicians sometimes ask about a new kitten, a child with a similar scalp rash, wrestling, crowded living conditions, or recent contact with animals.
Why the scalp is different from other ringworm
Many people know ringworm as a circular rash on the body, but scalp ringworm often looks different. It may show up as a scaly patch, scattered broken hairs, black dots where hairs have snapped at the scalp, or an inflamed tender plaque. Because hair is involved, the infection also tends to need systemic treatment.
The scalp can also hold fungal spores even when symptoms seem subtle. That is why household spread happens so easily, especially among siblings. Shared grooming habits matter more than many people realize. A practical prevention step is better hair brush hygiene and cleaning habits, particularly when one person in the home has an unexplained scaly scalp or patchy hair loss.
Tinea capitis is therefore best thought of as both an infection and a household management issue. Treating the scalp matters, but so does reducing exposure during the weeks when the fungus can still spread.
Symptoms and signs that stand out
The symptoms of scalp ringworm can be subtle at first. A child may only have a flaky patch that seems a little itchy. An adult may notice tenderness, broken hairs, or a patch that will not respond to ordinary dandruff shampoo. The appearance depends partly on the fungal species and partly on how strongly the immune system reacts.
Common symptoms
Typical signs include:
- One or more scaly patches on the scalp.
- Patchy hair loss.
- Hairs broken close to the scalp, sometimes leaving black dots.
- Itching, though not always severe.
- Redness, mild swelling, or pustules.
- Enlarged or tender lymph nodes in the neck.
- A dry, flaky surface that can resemble dandruff.
Some infections stay relatively non-inflammatory. Others produce much more redness, crusting, pustules, and discomfort. One of the most important severe forms is kerion, a swollen, boggy, tender mass that may ooze or crust. It is not just a “bad patch.” It reflects a strong inflammatory reaction to the infection and needs prompt care because delayed treatment increases the risk of permanent scarring hair loss.
Favus is another less common but important form. It can cause thick crusts and a distinct matted appearance, and it may also scar if not treated quickly.
Why it is often confused with other scalp problems
Tinea capitis is easy to misread because it overlaps with several common conditions. It may look like dandruff, seborrheic dermatitis, psoriasis, folliculitis, traction-related breakage, or even patchy alopecia areata. The difference is that ringworm often combines scale with broken hairs and contagious spread. A sibling with a similar patch, a new pet with a skin problem, or a child whose scalp gets worse despite routine dandruff care should raise suspicion.
Another clue is texture. Hair in the affected area often feels fragile, stubby, or uneven because the fungus weakens the shaft. People may describe the patch as “brittle,” “stubbly,” or “like the hair just snapped off.”
Symptoms that need faster action
Certain features deserve prompt medical evaluation:
- Painful scalp swelling.
- Pus, crusting, or drainage.
- Fast enlargement of the patch.
- Fever or marked lymph node swelling.
- Eyebrow or lash involvement.
- Hair loss that looks like it may scar.
The earlier the infection is recognized, the more likely hair will regrow normally. Waiting too long can turn a treatable fungal infection into an inflammatory scalp problem that is much harder to reverse.
How diagnosis is confirmed
A clinician may suspect tinea capitis from the pattern alone, but confirmation is often useful, especially when the scalp looks unusual, treatment has already failed, or the person affected is an adult. That is because scalp ringworm can mimic several inflammatory and hair-loss disorders, and the treatment plan changes considerably depending on what is actually present.
What the evaluation usually includes
Diagnosis often starts with a close scalp examination and a brief history. Helpful questions include:
- When did the patch begin?
- Is it itchy, painful, or draining?
- Has anyone else at home developed a similar rash?
- Are there pets with bald or scaly areas?
- Has there been recent contact sports exposure?
- Were steroid creams, antibiotic lotions, or medicated shampoos already tried?
The clinician then looks for clues such as black dots, broken hairs, perifollicular scale, pustules, crusting, and patch shape. The neck lymph nodes may also be checked because they can enlarge with scalp infection.
Common tests
Several tools may be used:
- KOH preparation: A scraping or plucked hair is examined for fungal elements.
- Fungal culture: This helps confirm the diagnosis and identify the organism, though results can take time.
- Trichoscopy or dermoscopy: This office-based magnified exam can reveal features such as comma hairs, corkscrew hairs, broken hairs, and black dots.
- Wood’s lamp: Some species fluoresce, though many common causes do not, so a normal result does not rule out infection.
In many real-world cases, treatment begins before culture results return if the pattern strongly suggests tinea capitis. That is sensible because waiting for every test result can delay care. Still, testing is valuable when the case is severe, recurring, or diagnostically confusing.
Why diagnosis matters beyond the name
The reason confirmation matters is not academic. A flaky scalp may be treated with dandruff products for weeks when the real problem is fungal invasion of the hair shaft. A pustular patch may be labeled bacterial folliculitis and given antibiotics that do not solve the core infection. A child with patchy loss may be thought to have seborrheic dermatitis when the broken hairs and contagious spread point elsewhere.
Accurate diagnosis helps with three things at once: choosing the right oral antifungal, deciding whether adjunctive shampoo is useful, and identifying whether pets, siblings, or shared grooming tools may be involved in continued spread. It also helps set expectations. Once people understand that scalp ringworm lives in the hair and follicles, the need for oral treatment becomes much easier to accept.
What treatment usually involves
The most important treatment point is simple: tinea capitis usually needs an oral antifungal medicine. This is the piece many people miss. A shampoo, cream, or oil may reduce surface spores, but it usually cannot clear a scalp infection on its own because the fungus is inside the hair shaft and follicle opening.
The main treatment options
Common oral treatments include:
- Griseofulvin.
- Terbinafine.
- Itraconazole.
- Fluconazole.
The best choice depends on age, medical history, likely fungal species, drug interactions, availability, and clinician preference. In broad terms, terbinafine often performs well for many Trichophyton infections, while griseofulvin is still commonly favored when Microsporum infection is strongly suspected or confirmed. Treatment duration varies, but it is usually measured in weeks rather than days, and some cases require one to three months.
This is one reason it is unwise to stop early just because the patch looks better. Hair and scalp symptoms may improve before the fungus is fully cleared.
What shampoos do and do not do
Adjunctive shampoo can still play a useful role. Ketoconazole or selenium sulfide shampoos are often used several times weekly early in treatment to reduce fungal spores on the scalp surface and lower spread to others. They help with contagion and scale control, but they are support, not the main therapy. A good way to explain it is that oral treatment clears the infection from within the hair structure, while shampoo helps reduce what is shed outward.
For readers who want the background on one of these products, a guide to ketoconazole shampoo use can help clarify why it is supportive here rather than curative on its own.
What to avoid
A few common mistakes can delay improvement:
- Using only over-the-counter antifungal cream.
- Relying on tea tree oil, vinegar rinses, or other home remedies.
- Applying steroid creams to an undiagnosed scalp rash.
- Stopping oral medicine too early.
- Ignoring pets or household spread.
Steroids deserve special caution. They may temporarily reduce redness and itching, but they can also blur the appearance of fungal infection and delay proper treatment. A child or adult whose scalp “improves” briefly on steroids and then worsens should be reassessed.
Special situations
Kerion needs prompt attention because the inflammation can damage follicles. Severe cases may need closer follow-up, culture confirmation, or additional supportive treatment depending on the person’s symptoms. Adults, immunosuppressed patients, and people with stubborn or recurrent disease also need a more careful medication review because oral antifungals can interact with other drugs.
The goal of treatment is not only to calm the rash. It is to eradicate the fungus, reduce household spread, and protect the follicles while they recover.
Recovery timeline and possible complications
Recovery from tinea capitis is often slower than people expect, especially when hair loss is visible. The scalp may look calmer after a couple of weeks, but hair density takes longer to normalize. That delay does not always mean treatment failed. It often reflects the basic pace of hair cycling and regrowth.
What improvement usually looks like
A typical pattern of improvement is:
- Less itching, tenderness, and flaking over the first few weeks.
- Reduced crusting and swelling if the infection was inflammatory.
- Fewer broken hairs once new fungal damage stops.
- Gradual regrowth over the following months.
The timing varies with severity. A small, dry, scaly patch may recover faster than a large inflammatory plaque or kerion. Hair shafts that broke off need time to be replaced, and follicles that were inflamed may stay quiet for a while before returning to normal growth. That is why learning about the hair growth cycle helps set realistic expectations.
When hair usually grows back
In uncomplicated cases, hair often regrows after the infection clears. Regrowth may begin within weeks, but a fuller cosmetic recovery usually takes longer. The main exception is when inflammation was severe enough to scar the follicle. This is the complication clinicians work hardest to prevent by treating early.
Complications to know about
Potential complications include:
- Kerion, with pain, swelling, and drainage.
- Scarring alopecia in severe or delayed cases.
- Secondary bacterial infection from scratching or broken skin.
- Spread to siblings, classmates, teammates, or pets.
- Ongoing carriage or recurrence if household sources are not addressed.
A few people also face treatment-related issues such as stomach upset, rash, or medication interactions. That is another reason follow-up matters, especially in adults taking other long-term medicines.
When to seek reassessment
Medical review is important if:
- The patch worsens after treatment starts.
- Pain, drainage, or swelling increases.
- New patches appear.
- Hair loss seems to be spreading rapidly.
- The scalp still looks clearly infected after the expected treatment period.
- The diagnosis remains uncertain.
Some hair loss after inflammation is temporary, and some is not. That uncertainty is exactly why a worsening or persistent case should not be managed by trial and error for too long. When there is any doubt, it is better to treat it like a hair-loss condition that needs proper diagnosis rather than a stubborn patch of dandruff.
How to prevent spread and reinfection
Preventing spread matters almost as much as treating the scalp itself. Tinea capitis is contagious, and reinfection can happen when fungal spores stay on shared objects, household surfaces, or infected pets. The best prevention plan is practical, not elaborate.
At home
These steps help lower spread:
- Do not share combs, brushes, hats, scarves, pillowcases, helmets, or hair accessories.
- Wash pillowcases, towels, hats, and similar items regularly during treatment.
- Clean brushes and combs and replace badly worn items when needed.
- Vacuum upholstered areas if an infected pet spends time there.
- Check household members for scaly patches, broken hairs, or itching.
- Arrange veterinary assessment if a pet has bald, crusted, or scaly areas.
Disinfection does not need to be obsessive, but it should be consistent. Shared fabric items and grooming tools are the main priority. In households with repeated cases, clinicians may also advise evaluating close contacts more directly, especially children.
At school, daycare, sports, and salons
Children do not need to be isolated forever, but they do need treatment and sensible precautions. Parents should tell the school or daycare if instructed by their clinician, especially if multiple children may have been exposed. Contact sports, especially wrestling or activities with shared headgear, deserve extra attention because close contact and shared gear can spread infection.
Barbers, stylists, and families should avoid using the same uncleaned tools from one scalp to another. Shared clippers, combs, and brushes can carry spores if sanitation is weak.
The goal is to break the cycle
The hardest cases are often not the most medically complex. They are the ones where the infection keeps circulating. A child gets treated, but a sibling has a subtle patch, a favorite hat keeps getting shared, or a kitten remains untreated. That is why prevention is part of treatment, not a separate afterthought.
One more practical point: persistent, patchy, or unexplained scalp hair loss deserves timely medical review, especially when scale or inflammation is present. A useful benchmark is knowing when hair loss should be assessed by a dermatologist rather than repeatedly self-treated.
Good treatment clears the fungus. Good prevention stops it from coming back through the same door.
References
- Comprehensive Review of Tinea Capitis in Adults: Epidemiology, Risk Factors, Clinical Presentations, and Management 2024 (Review)
- A Current Diagnostic and Therapeutic Challenge: Tinea Capitis 2024 (Review)
- Tinea capitis in Older Adults: A Neglected and Misdiagnosed Scalp Infection—A Systematic Review of Reported Cases 2025 (Systematic Review)
- Treatment of Ringworm 2026 (Government Guidance)
- Ringworm Prevention 2026 (Government Guidance)
Disclaimer
This article is for educational purposes only and is not a substitute for medical diagnosis or treatment. Scalp ringworm can resemble dandruff, eczema, psoriasis, folliculitis, and autoimmune hair loss, but it often needs prescription oral antifungal therapy. A painful, swollen, draining, or rapidly spreading scalp lesion should be assessed promptly, especially in a child, because delayed treatment can increase the risk of scarring and lasting hair loss.
If you found this article helpful, please share it on Facebook, X, or any platform your friends, family, or community use most.






