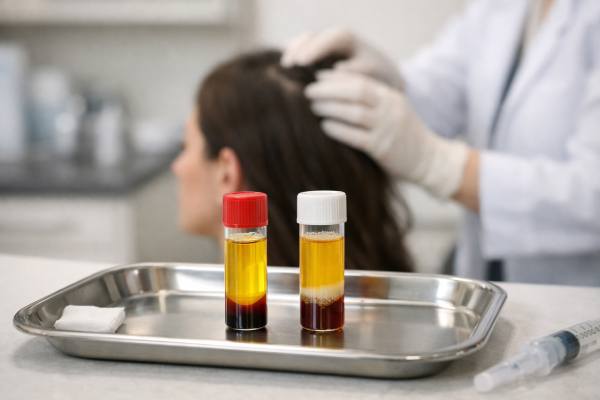
Hair thinning often pushes people into a fast-moving world of acronyms, clinic claims, and before-and-after photos that rarely explain what really matters. PRP and PRF are both blood-derived scalp treatments, and at first glance they can sound almost interchangeable. They are not. The difference is not just a letter. It changes how the product is prepared, how long growth factors may stay active, how predictable the protocol is, and how confidently a clinician can talk about expected results.
For readers trying to choose between them, the real question is less “Which one is newer?” and more “Which one fits my pattern of hair loss, my tolerance for maintenance, and the quality of evidence I am comfortable with?” That is the lens this comparison uses. Below, you will find a practical breakdown of how PRF and PRP differ, what downtime is usually like, who tends to respond best, and where the strongest results usually come from.
Quick Comparison
- PRP has the larger clinical evidence base and usually offers modest improvements in density, thickness, and shedding over several months.
- PRF may provide a slower release of growth factors and promising early results, but the hair-loss data are still much smaller and less standardized.
- Downtime is usually mild for both, with tenderness, redness, swelling, or pinpoint bleeding that often settles within 24 to 48 hours.
- Neither treatment reliably restores long-bare scalp, and both work best when follicles are still alive but miniaturizing.
- A series of sessions plus a longer-term plan usually matters more than choosing the newer acronym.
Table of Contents
- How They Are Made
- Which One Works Better
- Downtime Pain and Side Effects
- Best Candidates and Poor Candidates
- What Treatment Timelines Look Like
- How to Choose Between Them
How They Are Made
PRP stands for platelet-rich plasma. PRF stands for platelet-rich fibrin. Both start the same way: a small blood draw from the patient, followed by centrifugation and then scalp injections. The split happens during processing.
PRP is usually prepared to keep the final product as a liquid plasma concentrate with a high platelet count. In many protocols, an anticoagulant is used so the sample stays fluid while it is processed and injected. The goal is to deliver a platelet-dense solution that releases growth factors linked to wound repair, vessel formation, and follicle support. In hair treatment, that matters because miniaturized follicles need a better growth environment, not just a cosmetic cover-up.
PRF is considered a newer-generation platelet concentrate. It is generally prepared without an added anticoagulant and with a lower-speed, more time-sensitive spin. That produces a fibrin-rich matrix containing platelets and often more leukocytes. The fibrin works like a loose biologic scaffold. Instead of acting only as a carrier, it may help hold signaling molecules in place and release them more gradually.
That biological distinction is the main reason PRF attracts attention. On paper, a slower, steadier release sounds ideal for tissue repair. It is one reason some clinicians believe PRF may offer a more sustained regenerative signal than standard PRP. But biology is only part of the story. Clinic execution matters just as much.
One practical difference readers often overlook is protocol sensitivity. PRP has many variations, but it is generally easier to keep injectable as a liquid during treatment. PRF is more technique-dependent because timing, tube type, centrifuge settings, and injection speed matter. A clinic that says it “does PRF” without being precise about how it prepares and injects it is not giving you enough information.
Another point matters even more: neither PRP nor PRF creates brand-new follicles. They support existing follicles that are weakened, miniaturized, or cycling poorly. That is why both tend to work better for pattern thinning than for shiny, long-bare scalp with little follicular activity left. If you want a clearer sense of the follicle environment that supports regrowth, a good companion topic is the scalp environment that supports hair growth.
So, the short version is this: PRP is the more established liquid platelet concentrate, while PRF adds a fibrin framework that may extend growth-factor release. The gap between them is real, but it does not automatically mean newer is better in practice.
Which One Works Better
If the question is which treatment has the stronger evidence for hair loss today, PRP still has the clearer lead. It has been studied longer, across more randomized and controlled trials, and in more systematic reviews. That does not make it perfect. The evidence is still messy, with wide variation in platelet concentration, spin methods, activation, injection depth, treatment intervals, and outcome measures. But there is enough published data to say PRP can improve hair density and hair count in many people with androgenetic alopecia, especially over the first three to six months.
The catch is that “works” needs careful framing. PRP is not a miracle reset for advanced baldness. The best studies show modest but meaningful gains: less shedding, thicker shafts, better density on trichoscopy, and improved visual coverage. One 2024 meta-analysis found a pooled increase in hair density compared with placebo, but it also emphasized high heterogeneity and low overall evidence quality. That is an important reality check. Positive results exist, but they are not uniform enough to promise a standard outcome to every patient.
PRF is where the conversation becomes more interesting and more uncertain. The early clinical signal is encouraging. Small studies and reviews suggest improvements in hair density and visible regrowth, and the biologic rationale is attractive because of the fibrin matrix and potentially prolonged growth-factor release. Still, the size of the evidence base is much smaller than PRP’s. Much of the current PRF literature for androgenetic alopecia consists of case series, small cohorts, and emerging protocols rather than large, well-controlled comparative trials.
That means there is a difference between promise and proof. PRF may eventually prove superior for some patients or some protocols. Right now, the better-supported statement is more restrained: PRF is promising, but PRP remains the more evidence-backed choice.
A useful way to think about results is to focus on what success usually looks like:
- slower daily shedding
- fuller coverage in areas that still have miniaturized hairs
- slightly thicker hair shafts
- better photographs under the same lighting and angle
What success usually does not look like is just as important:
- a completely restored juvenile hairline
- dramatic regrowth on smooth, long-bare scalp
- permanent results after one session
- identical response from every clinic and every protocol
This is where evidence maturity matters more than marketing language. A treatment can sound biologically elegant and still be less predictable in the real world. PRF may have a theoretical edge in release dynamics, but PRP still has the practical edge in published outcomes.
Both options make more sense when the follicle is still alive and cycling, even if it is weaker than it should be. That is why understanding the hair growth cycle helps set realistic expectations. You are usually trying to improve a compromised cycle, not replace one that has already shut down completely.
Downtime Pain and Side Effects
For most people, downtime is not the hardest part of choosing between PRF and PRP. Uncertainty about the result is harder than the recovery. Both procedures are usually office-based, minimally invasive, and fairly quick. A typical visit includes blood draw, processing time, and multiple small scalp injections. In many clinics, the full appointment lands somewhere around 45 to 60 minutes.
During the treatment itself, the main issue is discomfort. The scalp is sensitive, so even with numbing cream, cooling, vibration devices, or local anesthetic, most people still feel pressure, stinging, or repeated pinches. Some tolerate the crown well but find the frontal hairline more uncomfortable. That is normal.
Afterward, the most common short-term effects are mild and temporary:
- scalp tenderness
- redness
- pinpoint bleeding at injection sites
- swelling or puffiness
- a dull headache
- occasional mild bruising
For many patients, these effects fade the same day or by the next day. Others need 24 to 48 hours before the scalp feels fully normal. If the treatment was more aggressive, or if the person bruises easily, a small amount of visible swelling can last a bit longer. In practical terms, most people can return to desk work and routine daily activity quickly.
The comparison between PRP and PRF on downtime is less dramatic than some clinic ads imply. There is not yet strong scalp-specific evidence showing that one clearly produces an easier recovery than the other. Anecdotally, some clinicians feel PRF can leave a slightly fuller or firmer post-injection feel because of the fibrin content, while others do not see a meaningful difference. The honest answer is that both usually involve mild downtime, and clinic technique likely influences comfort as much as the acronym does.
Safety is also usually favorable, but “autologous” does not mean “risk free.” Because the material comes from your own blood, allergy risk is low. Still, injections can cause complications if the setting is not clean or the candidate is poorly chosen. Infection, inflammatory irritation, prolonged swelling, or disappointing results are all possible. Pain is still the most common reason people hesitate to repeat sessions.
Downtime also changes if the procedure is combined with something else. A scalp session paired with microneedling, for example, may bring more redness, tenderness, and aftercare demands than injections alone. That matters if you are comparing one clinic’s “PRP package” with another clinic’s simpler protocol. If you are considering a combined plan, it helps to understand how microneedling frequency for hair growth can affect irritation and recovery.
A calm way to frame recovery is this: expect a briefly sore scalp, not a true medical recovery period. Most people are not homebound, bandaged, or off work for days. The bigger question is whether the mild inconvenience is worth the likely degree of improvement.
Best Candidates and Poor Candidates
The best candidate for either PRP or PRF usually has active follicles that are weakening, not follicles that are gone. In real terms, that often means early to moderate androgenetic alopecia in men or women: a thinning crown, widening part, diffuse mid-scalp thinning, or a receding hairline with miniaturized hairs still present. These are the cases where blood-based injections can realistically improve hair caliber, support the anagen phase, and reduce shedding.
Good candidates often include:
- men with early vertex or frontal thinning
- women with diffuse pattern thinning
- patients who want a non-surgical office treatment
- people looking for an add-on rather than a stand-alone cure
- patients seeking support after a hair transplant, when recommended by their surgeon
The word “add-on” matters. PRP and PRF usually perform best when they are part of a broader plan rather than the entire plan. That might include topical minoxidil, oral medication, low-level laser therapy, treatment of scalp inflammation, or correction of nutritional and hormonal issues.
Poor candidates tend to fall into three broad groups. The first group has the wrong diagnosis. Not every thinning scalp is standard pattern hair loss. Scarring alopecia, untreated seborrheic dermatitis, psoriasis, fungal infection, traction damage, or autoimmune disease can completely change the treatment path. Injecting a scalp before clarifying the diagnosis can waste time or worsen inflammation.
The second group has too little salvageable follicle activity. If the scalp is smooth, shiny, and bald for a long time, injections are less likely to create meaningful cosmetic change. In those cases, surgical restoration may be more rational than repeated regenerative sessions. That is where reading about who makes a good hair transplant candidate can be more helpful than pursuing another injection cycle.
The third group includes people with medical or blood-related reasons to pause or avoid treatment. That can include major platelet dysfunction, clotting problems, significant anemia, anticoagulant use, active infection, uncontrolled systemic illness, and very low platelet counts. A careful clinic should review medications, basic blood history, and scalp status before treatment.
There is also a psychological side to candidacy. People who expect a one-session transformation are usually poor candidates for satisfaction, even if they are technically good medical candidates. The best responders are often the most realistic ones: they understand that improvement is incremental, maintenance matters, and better density is a win even if the hairline does not look twenty years younger.
If you remember one point from this section, make it this: the best candidate is not the person most eager for treatment. It is the person with the right diagnosis, living follicles, and realistic expectations.
What Treatment Timelines Look Like
One session is rarely the real story. For both PRP and PRF, outcomes depend heavily on the treatment plan over time. Most clinics use a loading phase followed by maintenance, even if their exact protocol differs.
For PRP, a common pattern is three monthly sessions up front, with later maintenance spaced every few months depending on response and ongoing hair loss. PRF clinics often use a similar rhythm, though protocols are even less standardized. Some use three sessions spaced about four weeks apart. Others add a fourth session or stretch the interval depending on scalp response and the amount of thinning.
The timeline for visible change is usually slower than social media makes it seem:
- First few weeks: the scalp may simply recover from injections, with little obvious visual change.
- Around 6 to 8 weeks: some patients notice less shedding or slightly better texture.
- Around 3 months: density changes may start to show in photos or trichoscopy.
- Around 4 to 6 months: the most noticeable improvement from an initial series often becomes clearer.
- After that: maintenance determines whether the gains hold, plateau, or gradually fade.
This is one reason standardized photography matters. Hair can look “better” because it is styled differently, dried differently, or photographed under kinder light. Clinics that track results well usually use consistent angles, consistent lighting, and objective measurements when possible.
Another practical truth is that the strongest plans are often combination plans. PRP in particular has evidence suggesting it can work better when layered with established therapy rather than used alone. In everyday care, that might mean injections plus topical minoxidil, oral therapy where appropriate, scalp inflammation control, or device-based options. If you are building a regimen, it helps to avoid common errors with starting a minoxidil routine because poor adherence can make a good injection series look weaker than it really is.
Maintenance deserves more attention than it gets. Many readers focus on the first three visits and ignore the next year. That is the expensive mistake. Hair loss is often chronic. Even when PRP or PRF works, the benefit can fade if the underlying process keeps advancing and nothing is done to support the result.
A smart way to judge timelines is not to ask, “How fast can I see regrowth?” but rather, “What does my twelve-month plan look like?” That question usually reveals whether a clinic is thinking like a long-term hair practice or simply selling a procedure.
How to Choose Between Them
If you are deciding between PRF and PRP today, the most balanced answer is this: PRP is the safer recommendation from an evidence standpoint, while PRF is the more intriguing but still emerging option.
Choose PRP first if you want the treatment with the broader clinical record, more published protocols, and a clearer range of expected outcomes. That does not guarantee better personal results, but it does give you firmer ground when you weigh benefit against cost and maintenance.
Choose PRF more confidently when three things are true: the clinic has real experience with scalp PRF, the physician can explain the preparation protocol clearly, and you understand that the published hair-loss evidence is still limited compared with PRP. In other words, PRF becomes more appealing when the operator is strong and your expectations are disciplined.
The better comparison is often not PRF versus PRP in isolation, but weak protocol versus strong protocol. Ask practical questions such as:
- What diagnosis are you treating?
- How many sessions are usually recommended before judging response?
- How is the product prepared?
- What objective measures do you use to track progress?
- What percentage of your hair-loss patients need maintenance?
- What happens if I respond only partially?
- What else should be treated at the same time?
Cost also deserves a smarter question than “What is the price per session?” A more useful question is “What is the likely cost of the first year, including maintenance and supportive treatment?” A cheap first visit can become an expensive weak plan. A pricier visit may still be poor value if the clinic cannot diagnose properly or document results.
For advanced thinning, broaden the conversation beyond injections. Some patients are better served by medication, some by surgery, and some by device-based add-ons such as low-level laser therapy for hair growth. The right comparison is not always between two injectable options. Sometimes the right comparison is between injections and a completely different strategy.
The most useful bottom line is simple. PRP is the current evidence-first option. PRF is the option to consider when you want a biologically promising, newer approach and you trust the clinic’s protocol enough to accept more uncertainty. If your goal is predictability, PRP usually gets the nod. If your goal is to explore the newer regenerative format with open eyes, PRF can be reasonable. The best choice is the one that fits your diagnosis, your budget, and your tolerance for both maintenance and ambiguity.
References
- Platelet-rich plasma (PRP) versus injectable platelet-rich fibrin (i-PRF): A systematic review across all fields of medicine 2025 (Systematic Review). ([PubMed][1])
- Platelet-rich fibrin: A review of its role as a new treatment in androgenetic alopecia 2024 (Review). ([PubMed][2])
- Effectiveness of Injectable Platelet-Rich Fibrin Therapy in Alopecia and Facial Rejuvenation: A Systematic Review 2024 (Systematic Review). ([PMC][3])
- The role of platelet-rich plasma in androgenetic alopecia: A systematic review 2024 (Systematic Review). ([PubMed][4])
- Is autologous platelet-rich plasma capable of increasing hair density in patients with androgenic alopecia? A systematic review and meta-analysis of randomized clinical trials 2024 (Systematic Review and Meta-analysis). ([PMC][5])
Disclaimer
This article is for general educational purposes and does not diagnose, treat, or replace medical care. Hair loss has many causes, and PRF or PRP should not be chosen without confirming the diagnosis, reviewing scalp findings, and considering medical history, medications, and blood-related factors. Results vary by cause of hair loss, protocol quality, and follicle viability.
If this article was helpful, consider sharing it on Facebook, X, or your preferred platform so others comparing PRF and PRP can make a more informed decision.






