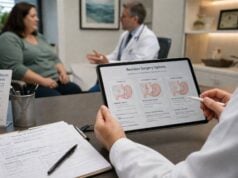
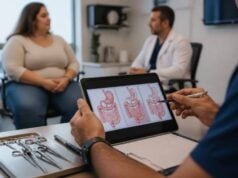
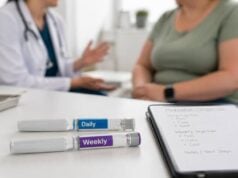
A weight loss medication dosing schedule is rarely just a calendar. It is a tolerability plan, a safety plan, and often the difference between staying on treatment and giving up too early. Many people assume the starting dose is supposed to create major appetite suppression right away, then worry that the drug is “not working” when the first few weeks feel underwhelming. In reality, many anti-obesity medications are designed to be increased gradually so your body can adapt before you reach the dose that does the heavier clinical lifting.
That is why it helps to know what titration is for, how dose increases usually work, when a schedule may be slowed down, and what counts as normal versus concerning. It also helps to know that different medications follow very different rules. Weekly injections, daily injections, combination tablets, and extended-release capsules are not escalated the same way, and trying to apply one schedule to another is a common source of frustration.
Table of Contents
- Why titration matters so much
- Common dosing schedules by medication
- What to expect after each dose increase
- When a dose increase gets delayed
- Missed doses, restarts and switches
- How clinicians decide to go up, stay or stop
- Common schedule mistakes that cause frustration
- How to make the schedule work in real life
Why titration matters so much
Titration means starting low and increasing gradually. In weight loss treatment, that usually has less to do with “easing you in emotionally” and more to do with helping your body tolerate the medication. This is especially true for GLP-1 receptor agonists and dual incretin drugs, where nausea, early fullness, reflux, vomiting, diarrhea, or constipation can become much worse if the dose rises faster than your body can adapt.
That point is easy to miss because many people measure success only by appetite and scale change. If your starting dose does not feel powerful, it can seem like wasted time. But the low starting dose often exists to reduce side effects, not to maximize fat loss in week one. For some medications, the starting dose is explicitly not considered a maintenance dose at all.
A few practical consequences follow from that:
- The first dose is often a tolerance test, not the “real” long-term dose.
- A bigger dose is not always better if it makes you too sick to eat normally, hydrate well, or continue treatment.
- Reaching the top dose is not the goal for every patient. Reaching the most effective tolerated dose is the goal.
- Weight loss often lags behind schedule changes, especially during the first escalation steps.
This is one reason people sometimes misjudge obesity treatment. They compare themselves with someone else using a different medication, a different dose, or a different speed of titration and assume something is wrong. In reality, the medication may be doing exactly what it is supposed to do.
It also helps to remember that titration schedules reflect drug design. Weekly injection schedules are often built around slower step-ups every four weeks. Daily injection schedules can move faster. Combination oral medications may build over one to four weeks, while some require response checkpoints before moving higher. In other words, “dose increase” is not one standard process across obesity medicine.
That is why it helps to understand the bigger picture of how weight loss medications are used before focusing only on the next pen, tablet, or milligram increase. The schedule is part of the treatment, not a minor technical detail. When patients understand that early, they tend to panic less, compare less, and make better day-to-day decisions.
Common dosing schedules by medication
The most useful way to compare weight loss medication dosing schedules is side by side. Even among commonly prescribed anti-obesity medications, the escalation pattern can be very different.
| Medication | How treatment starts | How the dose increases | Usual maintenance target | Key practical point |
|---|---|---|---|---|
| Wegovy injection | 0.25 mg once weekly for 4 weeks | Usually every 4 weeks to 0.5 mg, 1 mg, then 1.7 mg | 1.7 mg or 2.4 mg once weekly in many adults, depending on response and tolerability | Lower doses are part of initiation and escalation, not the main long-term target for most adults |
| Wegovy tablets | 1.5 mg once daily for 30 days | Then 4 mg for days 31 to 60, 9 mg for days 61 to 90 | 25 mg once daily from day 91 onward | Current semaglutide schedules now depend on formulation, so do not assume the injection and tablet versions work the same way |
| Zepbound | 2.5 mg once weekly for 4 weeks | Increase to 5 mg, then by 2.5 mg increments after at least 4 weeks on the current dose | 5 mg, 10 mg, or 15 mg once weekly for weight reduction | 2.5 mg is an initiation dose only, not a maintenance dose |
| Saxenda | 0.6 mg once daily for 1 week | Increase weekly to 1.2 mg, 1.8 mg, 2.4 mg, then 3 mg | 3 mg once daily in adults | Daily injections move faster than weekly titration, but GI side effects still often determine pacing |
| Contrave | 1 tablet in the morning during week 1 | Week 2: 1 tablet twice daily; week 3: 2 tablets in morning and 1 in evening | 2 tablets twice daily from week 4 onward | The dose builds over 4 weeks, and higher-fat meals are not a casual detail with this medication |
| Qsymia | 3.75 mg/23 mg once daily for 14 days | Then 7.5 mg/46 mg daily; higher escalation depends on response after 12 weeks | 7.5 mg/46 mg or, if needed and appropriate, 15 mg/92 mg | This is not an automatic climb to the highest dose; response checkpoints matter |
Two things stand out from that table.
First, a “weight loss medication dosing schedule” is not one thing. Weekly semaglutide and tirzepatide schedules are built around slow escalation, while Saxenda rises weekly and oral medications often follow a much shorter build. Second, some drugs aim for a fixed target, while others allow more flexibility. Tirzepatide, for example, may be maintained at 5 mg, 10 mg, or 15 mg depending on the patient. Qsymia may stop at an intermediate level or move up only after a response check.
This is also why comparing pills and injections on convenience alone misses something important. The schedule itself changes what treatment feels like. And if you are specifically using a GLP-1-based option, it helps to keep the broader context of GLP-1 medications in mind, because the way these drugs are titrated is one of the major reasons some people tolerate them well and others do not.
What to expect after each dose increase
Most dose increases do not create a dramatic overnight transformation. They usually produce one of three patterns.
The first pattern is increased satiety. You may notice that you get full faster, lose interest in finishing large meals, or feel less pulled toward snacks. This is often the effect people hope for, but it may show up gradually rather than all at once.
The second pattern is temporary side effects. This is especially common after each upward step with GLP-1-based treatment. Nausea, early fullness, burping, reflux, constipation, loose stools, or fatigue may increase for several days and then settle. That does not automatically mean the dose is wrong. It often means the body is adapting.
The third pattern is no obvious change right away. This can feel disappointing, but it is not unusual. Some patients do not notice a strong difference until later escalation steps, and even then the most meaningful outcome may be smaller portions and more consistent adherence rather than a dramatic sensation.
A useful way to think about dose increases is by phase:
- The first few days after an increase are often a tolerance phase.
This is when GI symptoms are most likely to flare. - The next one to two weeks are usually an adjustment phase.
Appetite changes become easier to interpret once the first wave of side effects settles. - By the end of the dosing block, you and your clinician can better judge whether the current dose is effective, tolerable, or too much.
That is why trying to evaluate a medication 24 to 72 hours after a dose increase often leads to bad conclusions. You are seeing the early adjustment period, not the full picture.
It also helps to change expectations around eating. After a dose increase, some people do best with smaller meals, slower eating, simpler foods, and more deliberate hydration. A medication will not make poor meal structure irrelevant. In fact, messy eating can make titration feel much worse. That is why people often do better when they use a simple meal plan built for GLP-1 treatment rather than trying to “wing it” through nausea and early fullness.
If nausea becomes the main issue, the fix is not always to quit or push through blindly. Sometimes it is a matter of spacing meals differently, lowering fat load for a few days, eating more slowly, or using the same dose longer before moving up. Practical symptom strategies can matter a lot here, especially if you are trying to manage nausea on GLP-1 medications without turning every dose increase into a miserable week.
When a dose increase gets delayed
A dosing schedule is a plan, not a commandment. One of the most useful things patients can understand is that clinicians often delay an increase on purpose.
The reason is simple: a patient who is barely tolerating the current dose usually does not do better by forcing the next one on time. In many cases, the smarter move is to hold the dose longer, let symptoms settle, and reassess. That is not “falling behind.” It is good medication management.
Common reasons a dose increase gets delayed include:
- persistent nausea that interferes with eating or fluids
- vomiting
- worsening reflux or upper abdominal discomfort
- severe constipation
- diarrhea that risks dehydration
- dizziness or weakness
- inability to meet basic food or hydration needs
- a clear drop in day-to-day functioning after the last increase
This is especially relevant with GLP-1-based drugs, because gastrointestinal tolerance is often what determines whether someone can stay on treatment long enough to benefit. A person who pushes from one dose to the next despite escalating symptoms may end up concluding that “the medication didn’t work,” when the real problem was outrunning tolerability.
There are also medication-specific reasons to slow down. Saxenda labeling, for example, allows clinicians to delay escalation about a week if a patient does not tolerate an increase. Wegovy labeling allows delaying escalation by four weeks. Qsymia does not follow a simple monthly ladder at all; it uses response checkpoints and may stay put or discontinue depending on results.
In practical terms, a delayed increase is often the right move if:
- side effects are still improving but not yet controlled
- appetite is already meaningfully reduced at the current dose
- the next increase would likely worsen adherence
- the patient is losing weight steadily enough without rushing upward
- another issue, such as travel, illness, or poor oral intake, makes this a bad time to climb
This is also the point where side-effect management becomes more important than impatience. If constipation is building, addressing it early is better than waiting until it becomes severe enough to derail the entire schedule. That is one reason it helps to know how to handle GLP-1 constipation before the problem becomes a reason to stop treatment.
Pregnancy planning matters here too. Some anti-obesity medications are contraindicated in pregnancy, and some have medication-specific reproductive cautions during treatment and dose escalation. That is why anyone who could become pregnant should review the basics of weight loss medications and pregnancy before treating dose changes as just a routine calendar event.
Missed doses, restarts and switches
Missed doses are one of the most common reasons people accidentally make a medication schedule harder than it needs to be.
The first rule is that missed-dose instructions are medication-specific. Some weekly medications allow a catch-up window. Some daily medications do not. Some treatments may need partial or full re-escalation after enough time off. Guessing is where people get into trouble.
A few practical examples show how different these rules can be:
- Wegovy weekly injection generally has a 48-hour rule tied to how close the next dose is.
- Zepbound weekly dosing allows a longer catch-up window, up to 4 days after the missed dose.
- Saxenda is more restart-sensitive. If more than 3 days have passed since the last dose, the label instructs reinitiating at 0.6 mg daily and following the escalation schedule again.
- Oral medications such as Contrave and Qsymia generally should not be doubled to “catch up.”
This is where people often make the wrong assumption. They think missing a dose means they should just jump back to wherever they left off, at the same strength, on the next convenient day. Sometimes that is fine. Sometimes it predictably causes more side effects. The longer the gap, the less safe it is to assume your body will tolerate the previous dose exactly the same way.
Switches create another layer of confusion. Semaglutide schedules now vary by formulation, and current labeling includes both injection and tablet versions under the Wegovy name. That means a switch is not just “same drug, different format.” It may involve a completely different escalation pattern. The same principle applies to device changes, such as different pen or vial formats. A package change is not a reason to improvise dosing.
Another overlooked point is that dose escalation can matter for contraception planning. Current tirzepatide labeling advises people using oral contraceptives to switch to a non-oral method or add a barrier method for 4 weeks after treatment initiation and for 4 weeks after each dose escalation. That is a schedule issue, not just a side-effect issue.
If your question is specifically about what to do after missing a weekly GLP-1 dose, it helps to review the common scenarios around a missed Wegovy or Zepbound dose rather than relying on memory or a friend’s advice. Even one or two wrong assumptions can turn a simple missed week into a rough restart.
How clinicians decide to go up, stay or stop
Patients often assume the decision tree is simple: if weight is not dropping fast enough, go up. In reality, clinicians usually balance three things at once: tolerability, objective response, and medication-specific rules.
For some medications, the label provides clear reassessment checkpoints.
| Medication | When response is checked | What usually happens next |
|---|---|---|
| Saxenda | About 16 weeks after starting | Adults who have not lost at least 4% of baseline body weight are usually advised to discontinue |
| Contrave | After 12 weeks on maintenance dosage | If weight loss is under 5% of baseline, continuation is usually not recommended |
| Qsymia | After 12 weeks on 7.5 mg/46 mg, then again after 12 weeks on 15 mg/92 mg if escalated | Escalate if early response is inadequate, then discontinue if later response remains below target |
| Weekly semaglutide and tirzepatide regimens | Usually assessed over a longer maintenance window | The decision depends more on tolerability, adherence, trend over time, and whether the current dose is truly the best tolerated effective dose |
This matters because the right next move is not always escalation.
Sometimes the best decision is to stay put. If appetite is much better, weight is trending down, and side effects are acceptable, there may be no benefit to rushing higher. Sometimes the best decision is to go up, because the patient is tolerating treatment well and the current dose is clearly too weak. Sometimes the best decision is to stop, because the medication has been given a fair chance and is not producing enough meaningful benefit.
For patients, this can feel emotionally complicated. A slower response often brings the fear that the drug has “stopped working” or that they are headed for a stall. But schedule decisions need a broader view than one disappointing weigh-in. Water retention, bowel changes, menstrual cycle shifts, travel, and activity changes can all muddy the picture. A clinician is usually looking for trend, not a single data point.
That is especially important before assuming you need a different dose because your weight loss medication has stopped working. In many cases the problem is not that the medication failed, but that the dose has not been on board long enough, the side effects are interfering with consistency, or the patient has reached the stage where plateaus become more common.
Common schedule mistakes that cause frustration
A lot of dosing frustration comes from expectations and habits, not from the medication itself.
One common mistake is treating the escalation calendar like a race. Patients may feel that getting to the highest dose fastest is the most serious or motivated approach. Usually it is just the fastest way to discover whether side effects can overpower adherence.
Another mistake is comparing different drugs as though the numbers mean the same thing. A weekly 0.5 mg step on one medication does not translate emotionally or biologically to a daily 0.6 mg increase on another. The units are not the story. The schedule design is.
Other common errors include:
- assuming the starting dose should produce major weight loss
- judging a dose after only a few days
- restarting at the old dose after too much time off
- ignoring hydration when nausea or diarrhea increases
- eating large, heavy, or very fatty meals right after escalation
- doubling an oral dose after forgetting one
- pushing to a higher dose even though the current one is already working
- assuming everyone must eventually reach the highest available dose
A more subtle mistake is thinking the schedule can compensate for poor day-to-day structure. Medications can reduce appetite, but they do not eliminate the need for workable meals, hydration, protein, and some planning. If dose increases are repeatedly followed by undereating all day and then rebound overeating at night, the schedule is not the only problem.
This is also why people sometimes mistake medication side effects for treatment failure. A patient may think, “I am nauseated, so I should be losing faster,” or, “I am constipated, so the dose must be too high,” or, “I am not nauseated, so the drug must not be doing anything.” None of those assumptions is reliable.
The schedule works best when it is treated as one part of a broader plan. That includes knowing your next increase date, having a simple food backup plan for rough days, and recognizing that appetite improvement can show up before dramatic scale change. It also helps to remember that life events, travel, illness, and routine disruption often make titration feel worse. The medication did not suddenly change; the surrounding conditions did.
How to make the schedule work in real life
The people who do best with weight loss medication schedules usually are not the ones who white-knuckle every escalation. They are the ones who make the schedule easy to follow.
A practical approach looks like this:
- Know your exact formulation.
Do not rely on brand name alone. Check the pen, tablet, capsule, or vial strength and the instructions attached to that version. - Write down your escalation dates.
This matters more than most people think. Memory is unreliable once travel, weekends, illness, or life stress enters the picture. - Track three things, not just weight.
Track weight trend, side effects, and appetite pattern. A dose may be helpful even before the scale fully shows it. - Keep a simple “titration week” food plan.
Smaller meals, steady fluids, and less digestive chaos make escalation smoother. - Treat intolerability as information.
You are not failing if a dose is too rough. You are learning where the useful range may be. - Ask before improvising.
Switching schedules, stacking medications, catching up missed doses, or restarting after a gap are situations where guessing often backfires.
This mindset becomes even more important later, when the goal shifts from initial loss to long-term stability. A dosing schedule is not only about getting lighter; it is also about building a treatment pattern you can actually live with. For some patients, that means staying on an intermediate dose. For others, it means reaching full maintenance. For others, it means deciding a medication is not the right fit and moving on.
That long-view thinking is especially important if you are already wondering what comes after the active weight-loss phase. The schedule that helps you lose weight is not always identical to the strategy that helps you maintain it. That is why it helps to think ahead about weight loss maintenance after medication instead of treating maintenance like a separate problem to worry about later.
The bottom line is that titration is supposed to make treatment more sustainable, not more stressful. When you understand what the schedule is trying to accomplish, the dose increases stop feeling random. They start feeling like what they really are: controlled adjustments designed to find the most effective dose your body can realistically handle.
References
- DailyMed – WEGOVY- semaglutide injection, solution WEGOVY- semaglutide tablet 2026 (Official Label)
- DailyMed – ZEPBOUND- tirzepatide injection, solution ZEPBOUND- tirzepatide injection, solution ZEPBOUND KWIKPEN- tirzepatide injection, solution 2026 (Official Label)
- DailyMed – SAXENDA- liraglutide injection, solution 2024 (Official Label)
- DailyMed – CONTRAVE EXTENDED-RELEASE- naltrexone hydrochloride and bupropion hydrochloride tablet, extended release 2025 (Official Label)
- DailyMed – QSYMIA- phentermine and topiramate capsule, extended release 2026 (Official Label)
Disclaimer
This article is for general educational purposes only and is not a substitute for medical advice, diagnosis, or treatment. Weight loss medication schedules are drug-specific and can change based on side effects, missed doses, pregnancy status, other medications, kidney function, and your clinician’s judgment, so always follow the instructions for your exact prescription.
If this article helped, consider sharing it on Facebook, X, or another platform where it could make weight loss medication dosing less confusing for someone else.