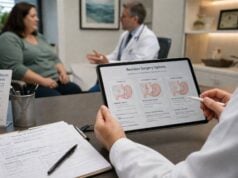
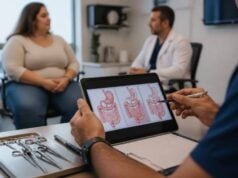
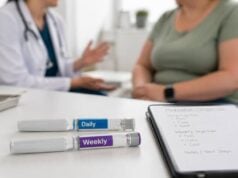
Traveling with weight loss injections is usually manageable, but it gets harder when people assume their usual routine will work without any planning. The main problems are predictable: temperature control, airport security, time-zone changes, missed doses, and travel habits that make side effects worse. A good plan prevents most of them.
For many people using weekly or daily GLP-1 injections, travel does not fail because of one big mistake. It fails because of a chain of small ones: the medication goes in checked luggage, the cooling pack is poorly packed, the dose day lands in the middle of a long-haul flight, meals get erratic, and a few days of bloating get mistaken for fat regain. The practical goal is simple: protect the medication, keep dosing safe, and make the trip easier on your stomach and schedule.
Table of Contents
- What to do before you travel
- How to store weight loss injections safely
- Flying with pens, needles, and cooling packs
- How to handle dose timing and time zones
- Food, hydration, and side effects on the road
- Special plans for hotels, road trips, and hot weather
- What to do if a dose is missed or damaged
What to do before you travel
The easiest travel mistakes happen before the trip even starts. People wait too long to refill the prescription, forget that their destination may have different medication rules, or assume they can sort out dose timing once they land. That approach works until there is a delay, a lost bag, or a long customs line.
Start by checking four basics at least a week or two before departure:
- how many doses you will need for the full trip
- whether you need a refill early
- what your exact product’s storage rules are
- whether your destination or layover country has restrictions on prescription medications, needles, or injectable devices
International travel deserves extra caution. Some countries are stricter than travelers expect, especially when syringes, injectable devices, or larger medication quantities are involved. Bring your medicine in its original packaging, keep the prescription label intact, and carry a copy of your prescription. For longer or more complicated trips, a clinician’s letter listing the generic and brand name of your medication can save time and confusion.
This is also the right time to simplify the rest of your routine. If you are due for a dose increase right before a red-eye flight, a wedding weekend, or a long international itinerary, that is often poor timing. The escalation phase is when nausea, fullness, reflux, and bowel changes are more likely to flare up. A trip is usually easier when you are already stable on your current dose rather than testing a new one.
A useful travel checklist includes:
- medication plus one or two extra doses or supplies if your clinician and refill schedule allow it
- needles or pen needles if your medication requires them
- alcohol swabs if you normally use them
- a travel case and, if needed, a cooling pouch
- a hard-sided sharps container or a thick substitute container approved for temporary use
- printed prescription information and insurance details
- a backup plan in case of cancellation, heat exposure, or a missed dose
Travel can also expose weak points in routine. If injections already feel rushed or inconsistent at home, fix that before you leave. It helps to review the basics of injecting weight loss medications correctly and build a realistic plan around when you will actually dose, not when you hope you will remember.
Finally, think beyond the medication itself. Travel often shifts meal timing, sleep, step count, bowel habits, and hydration. Those changes can make the medication feel different even when the drug is working exactly the same way. A looser travel rhythm is easier to handle when you already have a simple framework like a travel routine for weight loss instead of trying to improvise everything on the move.
How to store weight loss injections safely
Storage is the first real travel problem because “keep refrigerated” is only part of the story. Many weight loss injections can spend some time at room temperature, but the allowed window differs by drug and device. That means the right question is not just, “Does this need a cooler?” The better question is, “How long can my exact pen or vial stay out of the refrigerator, at what temperature, and can it go back in afterward?”
That distinction matters a lot on flights, road trips, cruises, and hotel stays.
| Medication type | Travel storage snapshot | Timing note |
|---|---|---|
| Weekly semaglutide pens such as Wegovy | Usually refrigerated before travel, but many pens can stay at room temperature for a limited period if kept in the original carton and protected from heat and light. | Weekly dose day can be moved, but only within the product’s spacing rules. |
| Weekly tirzepatide products such as Zepbound | Usually refrigerated before travel. Some presentations can stay at room temperature for a limited number of days, but the allowed window depends on the exact device. | Do not assume one Zepbound device follows the same storage rule as another. |
| Daily liraglutide pens such as Saxenda | Often refrigerated before first use, then allowed a limited room-temperature window once in use. | Missing several days may change how you restart, so check your specific instructions. |
A few principles are more important than memorizing every number:
- Never let the medication freeze.
- Never leave it in a hot car, on a sunny windowsill, or in a bag sitting on pavement.
- Keep it in the original carton when possible to protect it from light and mix-ups.
- Do not place the pen directly against ice or dry ice.
- If your product has a “room temperature clock,” track when that clock started.
That last point is where people get sloppy. They remember that the pen “can be out for a while,” but forget when it first left the refrigerator. Once travel starts, those hours are easy to lose track of. A simple note in your phone helps: “Pen removed from fridge Tuesday 9:00 AM.”
Hotel refrigerators create their own problems. Some are too warm. Others freeze items placed near the back wall or cooling element. If your medication still needs refrigeration, do not assume the minibar is accurate. When possible, ask the hotel for a medical refrigerator or confirm the fridge temperature after check-in.
If you are unsure whether the medication got too hot, too cold, or spent too long out of refrigeration, treat that as a real issue, not a minor guess. Weight loss injections are expensive, and “it probably looks fine” is not the same as properly stored.
This is also where broader travel planning helps. If your trip includes beach days, theme parks, long drives, hiking, or outdoor events, you need a temperature plan rather than just a bag. Many people focus on airport screening but forget that a six-hour excursion in hot weather may be the riskier part of the trip.
Flying with pens, needles, and cooling packs
For air travel, the safest default is simple: keep your weight loss injection and related supplies in your carry-on, not your checked bag. Even when checked baggage is technically allowed, it is the worse option. Bags get delayed, lost, overheated on the tarmac, or exposed to cold in cargo handling. Carry-on storage gives you more control and fewer surprises.
Pack the medication so it is easy to inspect without turning security screening into a scavenger hunt. That usually means one medical pouch or travel case that contains:
- the medication in original packaging
- needles or pen needles if needed
- alcohol swabs
- a cooling pack or travel cooler if required
- your prescription copy or clinician letter
- a sharps container or temporary puncture-resistant backup
For airport screening, the practical goal is to make the contents recognizable and organized. Injectable medications and related supplies are common enough that they usually do not create major trouble when they are packed clearly. Cooling accessories can help, but they should be used carefully. You want the medicine cool, not frozen. A barrier such as the carton, a sleeve, or cloth between the pen and the cold pack is safer than direct contact.
Needles and sharps deserve more attention than they usually get. Unused needles are one thing; used sharps are another. Do not toss used pen needles loose into a toiletry bag, hotel trash can, or airport bin. Use a proper sharps container or, if you are stuck temporarily, a thick puncture-resistant container that closes securely. The point is not only hygiene. It is protecting other people from accidental needle sticks.
A few airport-specific habits help:
- Keep the medication easy to reach.
- Give yourself more time than usual at security.
- Keep documentation handy but do not wave it around unless needed.
- Avoid packing the medication among snacks, cosmetics, and chargers where it can be crushed or forgotten.
- Check your carry-on before leaving the plane. Medical pouches are easy to leave in the seat pocket.
If your trip involves a connection, remember that long transit days increase the chance of small mistakes. A pen left in a hot shuttle bus or forgotten in an airport bathroom is more likely than a dramatic security problem.
One underappreciated point: flights can make side effects feel worse even when the medication is stored properly. Dehydration, motion, airport food, and long gaps between meals can all exaggerate nausea, bloating, or constipation. So “traveling with injections” is not just about getting the pen through security. It is about arriving with the medication intact and your stomach still manageable.
How to handle dose timing and time zones
Time-zone changes create more anxiety than they usually deserve, especially with weekly injections. In most cases, the answer is not to chase the clock perfectly. It is to respect the product’s spacing rules and avoid turning a stable routine into a guessing game.
For weekly injections, the main issue is the interval between doses. Some products allow you to change the day of the week, but only if enough time has passed since the last dose. That means the safest travel question is not, “What date is it where I land?” It is, “How many hours or days will have passed between doses if I move it?”
That matters most for:
- crossing multiple time zones
- overnight flights
- crossing the International Date Line
- trips that start or end on your usual injection day
- vacations where your regular dose time lands in the middle of transit
In practical terms, many travelers do well with one of these approaches:
- Keep the home schedule.
Best for short trips or modest time-zone changes. - Move the dose slightly before departure.
Best when the regular dose would otherwise land during a chaotic travel window. This only works if your medication’s minimum spacing rule allows it. - Shift to a new local routine.
Best for longer stays when sticking to home time would become awkward.
Daily injections are different. The goal is usually to stay roughly 24 hours apart and take the medication at a time you can repeat reliably. For many people, “with breakfast” or “before bed” works better than trying to preserve a home time that becomes impractical abroad.
A few rules make travel dosing safer:
- Do not double up because you are confused about the date.
- Do not shorten the interval just to keep the same weekday label.
- Do not use a travel day as a good moment to improvise a dose increase.
- Put the dose into your calendar in both home time and destination time before you leave.
This is where it helps to understand your own medication’s escalation and maintenance structure. If you are not clear on that, review your weight loss medication dosing schedule before the trip rather than making decisions in an airport lounge.
The most useful mindset is that consistency matters more than perfection. A safe, slightly adjusted schedule is better than a theoretically perfect schedule that you cannot actually follow. And if your trip causes confusion around a weekly GLP-1 dose, do not guess. Check the product instructions or use a conservative approach based on official missed-dose guidance, especially if you are close to the minimum interval threshold described in resources like missed dose guidance for Wegovy and Zepbound.
Food, hydration, and side effects on the road
Travel changes how people eat even when they are not trying to “cheat.” Meals get delayed. Portions get larger. Protein gets replaced by convenience food. Water intake drops. Sleep gets worse. All of that can make a weight loss injection feel harsher and make the trip feel less controlled than it really is.
The biggest travel-side-effect traps are usually:
- eating too little all day and then overeating at night
- very rich restaurant meals on top of a dose escalation
- drinking less water than usual
- alcohol on an already sensitive stomach
- relying on sweets, pastries, or airport snack mixes because nothing else is available
If your medication already makes you feel full quickly, travel is a bad time to test how much fried food, buffet food, or vacation desserts your stomach can handle. That does not mean travel has to be joyless. It means the medication is easier to live with when meals stay moderate, slower, and more predictable.
A practical food strategy is to travel with a small “stomach-friendly” backup kit:
- protein bars or shakes you already tolerate
- plain crackers or another bland option that works for you
- electrolyte packets if long travel days leave you depleted
- one or two familiar snacks that are easy on your stomach
That matters even more if you are still titrating upward or you tend to get nausea. Travel-day eating works best when it is lighter and steadier than people expect, not heavier. Many users do better with smaller meals, moderate fat, slower eating, and less alcohol rather than trying to “save calories” and then hitting a huge dinner.
Hydration is just as important. Long flights, walking-heavy itineraries, heat, and gastrointestinal side effects can quietly create the kind of dehydration that makes dizziness, constipation, and headaches worse. If nausea has been part of your experience, it helps to review a plan for managing nausea on GLP-1 medications before you travel instead of waiting until you feel bad in transit.
Food structure also matters for consistency. Travel does not erase the value of high-protein, lower-chaos eating. If you need a simple framework, a meal plan for people on GLP-1 medications can be adapted into travel meals more easily than trying to rebuild your routine from scratch every day.
One final point: a few days of restaurant sodium, less fiber, and irregular bowel movements can make the scale jump quickly. That is not proof your medication stopped working. Often it is just travel physiology and digestion.
Special plans for hotels, road trips, and hot weather
Not all travel challenges start at the airport. Hotels, road trips, cruises, and hot-weather destinations create different risks, and each one changes how careful you need to be.
Hotels are easiest when you assume nothing. Confirm refrigeration after you check in, not before. Some mini-fridges are barely cool. Others freeze anything placed near the back. If refrigeration matters for your specific device, ask for a proper medical fridge when possible, or at least avoid putting the medication directly against the cold plate.
Road trips seem simple, but parked cars are one of the fastest ways to ruin injectable medication. Even mild weather can produce dangerous interior temperatures. Do not leave the pen in the glove compartment, center console, trunk, or a tote bag sitting in the sun. Take it with you whenever you leave the vehicle.
Cruises and all-inclusive resorts often create a different problem: constant access to rich food and alcohol. That can turn a normally tolerable dose into several days of nausea, reflux, or bloating. If your medication has been working well, keep the trip enjoyable by staying a little more moderate than the environment encourages.
Beach trips, outdoor tours, and theme parks are really heat-management problems. A long day in sun and humidity can stress both the medication and your hydration. This is where a proper cooling setup matters more than at the airport itself. Keep the medicine shaded, insulated, and out of direct sun. Do not assume a backpack is enough protection if it is sitting on hot ground or in a locked rental car.
Active trips can create another kind of mismatch. If you are walking far more than usual while eating irregularly, you may notice lower energy, more nausea, or a stronger aversion to heavy meals. That does not mean the medication is wrong for you. It usually means your travel pattern changed faster than your fueling pattern.
If the trip is mostly about maintenance rather than active fat loss, it can help to shift your mindset away from “perfect dieting” and toward damage control. A strong travel week is often one where medication stays safe, meals stay reasonably structured, and you come home without a multi-week backslide. That mindset fits especially well with broader holiday and travel maintenance strategies, where the goal is steadiness rather than overcorrection.
What to do if a dose is missed or damaged
This is where panic causes the worst decisions. A flight delay, lost pen, questionable fridge, or missed dose can make people jump straight to doubling up, taking the dose early, or buying replacement medication in a hurry. Those are exactly the moments to slow down.
If a dose is missed, the first question is which type of medication you take:
- weekly injections usually have a specific “take it within X days or skip it” rule
- daily injections usually have a different restart rule and may require extra caution if several days are missed
That is why generic advice is risky here. The right response for one GLP-1 may be wrong for another. If you are in doubt, use the product instructions and your clinician’s advice, not memory from a social media post.
Treat the medication as potentially unusable if:
- it froze
- it sat above the allowed temperature too long
- it has been out of the fridge beyond the allowed window
- the solution looks cloudy, discolored, or contains particles when it should not
- the pen or vial was physically damaged
- you can no longer confirm how it was stored
If that happens while traveling, the next step depends on where you are. On a short trip, it may be safer to miss or delay a dose according to official instructions than to scramble for an unfamiliar refill. On a longer trip, contact your prescribing clinician, pharmacy, or insurer early. Do not wait until your last intact dose is gone.
A few situations deserve same-day help:
- severe vomiting with inability to keep fluids down
- significant dehydration
- severe abdominal pain
- repeated dosing confusion
- multiple missed daily doses during dose escalation
- a lost supply during an extended trip
Also, do not misread travel weight changes. A couple of days of constipation, sodium-heavy food, less sleep, or menstrual-cycle timing can look like regain or a stalled response when it is really temporary water and digestive change. That is one reason travel can make people think they have hit a medication plateau when they have not. If that concern sounds familiar, it is worth comparing normal travel fluctuations with a true weight loss plateau on GLP-1 medications before you conclude the drug stopped working.
The best reset after a messy trip is usually boring: resume your normal schedule, get hydration back up, return to familiar meals, and stop treating a few travel days as proof that everything unraveled. Weight loss injections work best when the response to disruption is calm and procedural, not dramatic.
References
- Traveling Abroad with Medicine | Travelers’ Health | CDC 2025 (Government Guidance)
- Medicine and Health | Travel.State.gov 2025 (Government Guidance)
- WEGOVY (semaglutide) injection, for subcutaneous use 2025 (Prescribing Information)
- ZEPBOUND (tirzepatide) injection, for subcutaneous use 2025 (Prescribing Information)
- Safely Using Sharps (Needles and Syringes) at Home, at Work and on Travel | FDA 2021 (Government Guidance)
Disclaimer
This article is for general educational purposes only and is not a substitute for medical advice, diagnosis, or treatment. Storage limits, missed-dose instructions, and travel timing rules can differ by medication, device, dose stage, and your medical history, so follow your product instructions and your prescriber’s guidance if they differ from general travel advice.
If this article helped, please consider sharing it on Facebook, X, or another platform where it could make someone else’s trip easier.