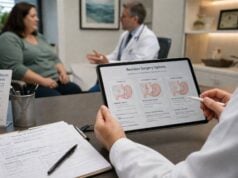
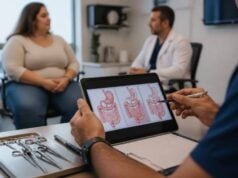
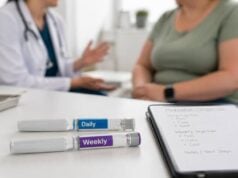
Saxenda is a prescription weight loss medication that uses liraglutide, a GLP-1 receptor agonist, to reduce appetite and help people eat less without relying only on willpower. It can work well, but it is not a magic fix, and it is not the most powerful option now available. Its real value is that it can make a calorie deficit feel more manageable by reducing hunger, increasing fullness, and lowering the urge to keep eating after a normal meal.
For people deciding whether Saxenda is worth trying, the practical questions matter most: how it works, how much weight people usually lose, how fast results show up, what side effects are common, and when it makes sense to consider a newer alternative instead. Those are also the issues that matter most when weight loss slows, when side effects become a problem, or when long-term maintenance is the real goal rather than just a fast start.
Table of Contents
- What Saxenda is and how it works
- Who Saxenda is for and how to take it
- Saxenda results and how long they take
- Common side effects and how to manage them
- Who should avoid Saxenda and key warnings
- Saxenda vs newer weight loss medications
- Plateaus, stopping and long-term maintenance
What Saxenda is and how it works
Saxenda is the brand name for liraglutide 3 mg, a once-daily injectable medicine used for chronic weight management. It belongs to the same broad medication family as other GLP-1 drugs, but it is older and shorter-acting than the weekly options that get most of the attention now.
Its main job is not to “burn fat” directly. It helps with weight loss by changing appetite signals. Liraglutide mimics GLP-1, a gut hormone involved in hunger, fullness, and food intake. In practice, that usually means three things happen at once:
- meals feel more filling
- hunger tends to come back more slowly
- it becomes easier to stop eating sooner
That combination is why some people describe Saxenda as reducing both appetite and “food noise.” The effect is not identical for everyone. Some notice less physical hunger. Others notice less grazing, less snacking between meals, or less drive to keep eating after dinner.
Saxenda also slows stomach emptying, at least in part, which contributes to feeling fuller. That helps explain both its benefits and many of its side effects. The same mechanism that helps someone feel satisfied on a smaller portion can also make them feel nauseated, overly full, burpy, or constipated if the dose rises too fast or meals stay too large.
A useful way to think about Saxenda is that it does not replace a weight loss plan. It changes the biology so the plan becomes easier to follow. That difference matters. People often get the best results when they use Saxenda to support a simple eating structure rather than trying to eat as little as possible. It is one member of a much larger medication group, so readers comparing drug classes may also want a broader look at GLP-1 medications for weight loss and a bigger-picture overview of who qualifies for prescription weight loss medications.
One practical advantage of Saxenda that gets overlooked is its daily schedule. That is a disadvantage for convenience, but it can be an advantage for fine-tuning. If side effects flare, clinicians sometimes have more room to slow titration or hold a dose step before moving higher. That makes Saxenda feel more adjustable for some people, even though it usually produces less weight loss than newer weekly drugs.
Who Saxenda is for and how to take it
Saxenda is generally used for long-term weight management in adults with obesity, or in adults with overweight plus at least one weight-related condition. In the current U.S. labeling, it is also approved for certain adolescents aged 12 and older with obesity. Exact eligibility, insurance rules, and prescribing habits can vary by country and health system, so the label is only the starting point.
The medication is injected once daily under the skin of the abdomen, thigh, or upper arm. It can be taken at any time of day, with or without food. The big rule is consistency. Most people do better when they pick a time they can repeat reliably.
Saxenda is not started at the full dose. It is titrated upward to reduce gastrointestinal side effects.
| Week | Daily dose | Practical note |
|---|---|---|
| 1 | 0.6 mg | Starter dose to improve tolerance |
| 2 | 1.2 mg | Move up only if the prior week is tolerable |
| 3 | 1.8 mg | Fullness usually becomes more noticeable here |
| 4 | 2.4 mg | Side effects often peak during this middle phase |
| 5 and onward | 3 mg | Target maintenance dose for adults |
For adults, 3 mg is the intended maintenance dose. Lower doses are mainly for titration. If an adult cannot tolerate the 3 mg dose, the current prescribing information says Saxenda should be discontinued rather than used indefinitely at a lower adult maintenance dose.
A few practical points matter more than people expect:
- If side effects show up during dose escalation, clinicians may delay the next increase by about a week instead of pushing through.
- If more than 3 days pass after the last dose, the medication is usually restarted at the lowest dose and titrated again.
- Saxenda should not be combined with other liraglutide-containing products or with another GLP-1 receptor agonist.
- Injection site rotation matters, especially with daily use.
The daily pen schedule is one reason technique and routine matter. Missed doses, rushed eating, and inconsistent meal timing often make early treatment feel harder than it needs to. People who are new to injectable obesity treatment usually benefit from learning the basics of how to inject weight loss medications correctly before they start, rather than after they have already built anxiety around the pen.
Saxenda results and how long they take
Saxenda can work, but expectations need to be realistic. It is effective enough to be clinically useful, yet its average results are more modest than those of semaglutide and tirzepatide.
In the major adult weight management trials, average weight loss with liraglutide 3 mg over 56 weeks was roughly in the mid-single digits to high-single digits as a percentage of body weight, depending on the population being studied. In the main adult obesity or overweight-with-comorbidity study summarized in the current label, mean weight change at 56 weeks was about 7.4 percent with Saxenda versus 3.0 percent with placebo. About 62 percent of Saxenda-treated participants lost at least 5 percent of body weight, and about 34 percent lost more than 10 percent.
Those numbers are useful because they frame what “good” looks like. Saxenda is usually not a medication that produces dramatic weight loss in most people. Instead, it often delivers a meaningful, steady drop that can improve blood sugar, waist size, appetite control, and the odds of maintaining a deficit long enough for other habits to become more automatic.
Results also do not happen all at once. The first few weeks are often more about tolerance than scale change. Many people notice appetite changes before they see major weight loss. That can still be a good sign. Smaller portions, fewer late-night snacks, and less preoccupation with food often show up before body weight fully reflects the change.
A practical timeline usually looks like this:
- Weeks 1 to 4: appetite changes may start, but side effects often dominate the experience.
- Weeks 5 to 8: once the dose is higher, fullness and portion control usually become clearer.
- Months 3 to 6: the pattern of response is easier to judge.
- Around week 16: this is the key checkpoint for adults, because current labeling recommends stopping if at least 4 percent of baseline body weight has not been lost by then.
That 16-week rule matters. It keeps people from staying on a daily injectable medication for months when the response is too weak to justify the burden, cost, and side effects. Readers who want a broader sense of what timelines look like across the medication category can compare this with how long weight loss medications take to work.
One more useful insight: how Saxenda changes eating behavior can matter as much as the number on the scale. If someone is eating less impulsively, feeling fuller sooner, and finding it easier to stay consistent, those changes often predict better long-term value even when weekly scale loss is not flashy.
Common side effects and how to manage them
Most Saxenda side effects are gastrointestinal, and that is not accidental. The same physiology that helps reduce appetite can also make digestion feel slower and less comfortable.
The most common side effects include:
- nausea
- diarrhea
- constipation
- vomiting
- injection site reactions
- headache
- indigestion or dyspepsia
- fatigue
- dizziness
- abdominal pain
Nausea is the one that defines the early experience for many people. It is often worst during dose increases and often improves after the body adjusts. The people who struggle most are often doing one of two things without realizing it: raising the dose too aggressively, or continuing to eat like they did before the medication.
A few simple adjustments often help:
- Eat smaller meals than usual, especially during titration.
- Stop eating at the first sign of fullness instead of finishing out of habit.
- Keep high-fat, very greasy, or very large meals modest while adjusting.
- Drink fluids steadily rather than chugging large amounts with meals.
- Slow down. Saxenda punishes rushed eating more than many people expect.
Constipation is another common issue, especially if total food volume drops quickly and hydration falls with it. This is one reason some people mistakenly think the drug “stopped working” when the scale stalls. In reality, slowed bowel habits can temporarily hide fat loss. If nausea and constipation are both present, the fix is often not “eat less.” It is usually better hydration, gentler meal size, enough protein, and enough fiber that the person can actually tolerate.
That is where food selection matters. On Saxenda, bland but protein-poor eating can keep nausea down for a few days, but it often backfires later by making fullness weaker and muscle retention worse. In practice, many people do best with simple meals built around lean protein, easy-to-digest produce, and portions that feel almost too small at first. For medication-specific nausea strategies, managing nausea on GLP-1 medications is a useful companion resource, and people who want meal structure rather than guesswork often do better with a meal plan designed for GLP-1 medication use.
A less obvious side effect issue is that “too full” can become its own problem. Some people assume that stronger fullness is always better and keep escalating even though they are eating uncomfortably little, struggling to hit protein, or feeling wiped out in workouts. That is not a good trade. A tolerable, sustainable response usually beats the harshest possible appetite suppression.
The right question is not whether Saxenda causes side effects. It often does. The right question is whether the side effects are easing, manageable, and worth the benefit. If they are getting worse, staying intense, or interfering with hydration and normal function, the plan needs to be adjusted.
Who should avoid Saxenda and key warnings
Saxenda is not appropriate for everyone, and this is where reading past the headline benefits matters most.
The current prescribing information includes a boxed warning about thyroid C-cell tumors based on rodent data. It is contraindicated in people with a personal or family history of medullary thyroid carcinoma or with multiple endocrine neoplasia syndrome type 2. That warning tends to get simplified online, but the practical takeaway is straightforward: if that history applies, Saxenda is generally off the table.
Other important safety issues include pancreatitis, gallbladder disease, dehydration-related kidney injury, increased heart rate, serious hypersensitivity reactions, and severe gastrointestinal adverse reactions. Saxenda is also not recommended in severe gastroparesis, which makes sense given that it slows gastric emptying.
A newer practical point that deserves more attention is surgery and anesthesia. Because Saxenda can delay stomach emptying, people should tell their medical team before planned procedures involving general anesthesia or deep sedation. That is not a small technicality. It can affect procedural safety planning.
Saxenda also deserves extra caution or review in situations such as:
- current or past pancreatitis
- gallstones or gallbladder symptoms
- significant dehydration from vomiting or diarrhea
- use of insulin or a sulfonylurea, which can increase hypoglycemia risk
- severe digestive motility problems
- pregnancy or plans to become pregnant
Pregnancy is especially important. Saxenda is not a medication to continue through pregnancy planning by default, and it should be discussed early rather than after a positive test. For people navigating that issue, weight loss medications and pregnancy is the more relevant next read than general weight loss advice.
Not every warning means a medication is unsafe for you. It means the fit has to be individualized. Someone with a strong history of slow stomach emptying, chronic nausea, or upper abdominal pain may be a poor candidate even if they qualify by BMI. Likewise, someone with persistent vomiting on other GLP-1 drugs may not suddenly tolerate Saxenda well just because it is a daily injection. A more focused discussion of one important exclusion area is in gastroparesis and GLP-1 weight loss drugs.
The bigger point is that obesity treatment should be personalized. A medication can be appropriate in theory and still be the wrong choice in practice because the side effect burden, medical history, or lifestyle fit is poor.
Saxenda vs newer weight loss medications
Saxenda still has a place, but it is no longer the obvious first choice for many adults who want prescription treatment. The main reason is simple: newer medications usually produce more weight loss with less frequent dosing.
Compared with weekly semaglutide and tirzepatide, Saxenda asks more from the user and usually gives back less. It is a daily injection, it often produces mid-single-digit to high-single-digit percentage weight loss rather than the larger averages seen with newer agents, and it can still cause the same broad family of gastrointestinal side effects.
That does not make it obsolete. It just makes the choice more specific.
Saxenda may still make sense when:
- a clinician wants a GLP-1 option with slower, more adjustable escalation
- the patient has done well with liraglutide before
- coverage or availability makes it the most realistic option
- the goal is meaningful appetite help, not necessarily the strongest current average weight loss
There is also a subtle behavioral difference worth noting. Because Saxenda is daily, some people feel more “in touch” with the medication and more able to adjust around side effects. Weekly drugs are more convenient, but once the dose is in, it is in. That matters for sensitive patients, though convenience usually wins for adherence over time.
Still, if someone is starting from scratch and wants the highest-likelihood medical option for stronger weight loss, Saxenda is often not the current front-runner. In those cases, comparing it against newer drugs such as tirzepatide for weight loss is often more useful than comparing it only to older stimulant medications.
The real decision is not whether Saxenda works. It does. The real decision is whether it is the best fit now that better average performers exist. For some people, the answer is still yes. For many others, Saxenda ends up being a reasonable second-choice GLP-1 rather than the preferred first one.
Plateaus, stopping and long-term maintenance
Saxenda can help people lose weight, but the more important question is what happens after the early momentum fades. This is where many treatments look better at month three than they do at month twelve.
A plateau on Saxenda does not automatically mean the drug failed. Common reasons progress slows include:
- the body now needs fewer calories at a lower weight
- early appetite benefits have been partly offset by habit drift
- weekend eating or restaurant meals have crept up
- movement has dropped as body weight has fallen
- constipation, sodium, or hormonal shifts are masking scale loss
- the dose never became fully tolerable, so treatment stayed half-effective
The first step is to ask what changed. If hunger is back, the medication may no longer be doing enough. If hunger is mostly controlled but portions, alcohol, takeout, or snacking have crept up, the issue may be behavior rather than biology. That distinction matters, because switching medications does not fix sloppy maintenance habits.
Stopping Saxenda is another key point. Appetite often returns when treatment stops, and weight regain becomes much more likely unless there is a strong maintenance plan underneath it. That is not a moral failure and not proof that the medication “ruined” metabolism. It usually means the biology the drug was helping to manage is no longer being held in check.
That is why the best long-term use of Saxenda is usually not “take it until the scale number looks good.” It is “use it to build a repeatable system.” That system usually includes:
- enough protein to protect lean mass and support satiety
- some resistance training or at least regular strength work
- a short list of meals you can repeat without decision fatigue
- regular weigh-ins or other simple monitoring
- a plan for what you will do if regain starts
If progress has flattened despite good adherence, it helps to assess whether the issue is a true drug plateau or a broader routine problem. For that specific situation, what to do with a GLP-1 weight loss plateau is the most relevant next step. And once the focus shifts from losing to holding the result, the bigger challenge is usually maintaining weight loss after medication, not finding ever harsher restriction.
One honest conclusion about Saxenda is that it can still be a solid tool, but it works best when it is used as part of a long-term system, not as a temporary appetite shortcut.
References
- Label: SAXENDA- liraglutide injection, solution 2026 (Prescribing Information)
- A Randomized, Controlled Trial of 3.0 mg of Liraglutide in Weight Management 2015 (RCT)
- Healthy Weight Loss Maintenance with Exercise, Liraglutide, or Both Combined 2021 (RCT)
- Medications for Obesity: A Review 2024 (Review)
- Pharmacotherapy for obesity management in adults: 2025 clinical practice guideline update 2025 (Guideline)
Disclaimer
This article is for general educational purposes only and is not a substitute for medical advice, diagnosis, or treatment. Saxenda can cause important side effects and is not appropriate for everyone, so decisions about starting, stopping, or switching treatment should be made with a qualified clinician.
If you found this article useful, please consider sharing it on Facebook, X (formerly Twitter), or another platform that fits your audience.