A corneal laceration—an open wound or cut on the transparent front surface of the eye—is a vision-threatening emergency that requires rapid assessment and expert management. Whether caused by trauma, sharp objects, or accidents, corneal lacerations demand urgent care to prevent complications such as infection, vision loss, or even loss of the eye itself. This comprehensive guide covers what you need to know about corneal laceration: from recognizing the injury and risk factors, through current and advanced treatments, to future innovations on the horizon for eye health.
Table of Contents
- Defining Corneal Lacerations and Risk Factors
- Non-Surgical Management and Pharmacological Support
- Surgical and Procedural Interventions for Corneal Injury
- Cutting-Edge Advancements and Emerging Technologies
- Current Research Trials and Future Perspectives
- Frequently Asked Questions
Defining Corneal Lacerations and Risk Factors
A corneal laceration occurs when the cornea—the clear, protective layer covering the front of the eye—suffers a cut or tear deep enough to penetrate its full thickness or close to it. These injuries are distinct from superficial corneal abrasions, which affect only the surface layer (epithelium). Lacerations are particularly serious because they can open a direct path for infection into the eye and may be associated with other internal ocular injuries.
How Corneal Lacerations Occur
- Trauma from Sharp Objects: Common causes include accidents with glass, metal, wood, or projectiles (e.g., sports equipment, power tools, or broken household items).
- High-Speed Accidents: Motor vehicle crashes, workplace mishaps, or explosions may also produce high-velocity fragments capable of penetrating the cornea.
- Physical Assault or Falls: Less commonly, direct blows or falls onto sharp objects can lead to lacerations.
Pathophysiology and Injury Types
- Partial-Thickness Lacerations: These cuts do not penetrate the entire corneal thickness. The risk of infection remains, but structural integrity is usually maintained.
- Full-Thickness (Open-Globe) Lacerations: The wound goes through all corneal layers and may extend into deeper structures. These represent ocular emergencies and are associated with higher risks of vision loss and infection.
Prevalence and At-Risk Populations
- Prevalence: Corneal lacerations are less common than other eye injuries but carry greater risk of long-term damage.
- Risk Factors: Young males (often involved in high-risk jobs or sports), children, and individuals working with tools or machinery are at greatest risk. Lack of protective eyewear is a frequent contributing factor.
Immediate Symptoms and Red Flags
- Sudden pain and tearing
- Loss or blurring of vision
- Bleeding from the eye or a visible wound
- Photophobia (light sensitivity)
- Feeling of something stuck in the eye
Practical Advice:
If you or someone nearby sustains an eye injury, avoid rubbing or pressing on the eye. Do not attempt to remove any embedded objects. Cover the eye lightly with a rigid shield (not cotton), and seek emergency care immediately.
Non-Surgical Management and Pharmacological Support
Initial care for corneal lacerations centers on stabilizing the eye, preventing infection, and minimizing further damage while preparing for possible surgery. In select cases of minor, partial-thickness lacerations, conservative therapies may suffice.
First Response and Emergency Measures
- Shielding the Eye: Place a rigid eye shield (not a patch) to protect the area. Avoid pressure or manipulation.
- Immediate Medical Evaluation: Rapid assessment is crucial, especially to rule out open-globe injury or intraocular foreign bodies.
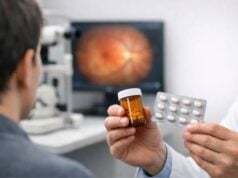
Pharmacological Treatments
- Topical Antibiotics:
- Prevents bacterial infection, which is a primary concern after corneal trauma.
- Common options: fluoroquinolone or broad-spectrum antibiotic drops or ointments.
- Frequency: Often prescribed every 2–4 hours, depending on severity.
- Systemic Antibiotics:
- May be indicated if there is suspicion of deep or contaminated wounds.
- Tetanus Prophylaxis:
- Tetanus vaccination status should be checked and updated if necessary.
- Pain Management:
- Oral analgesics (acetaminophen, ibuprofen).
- Topical cycloplegic drops (to relax the eye muscles and reduce pain in select cases).
Adjunctive Support
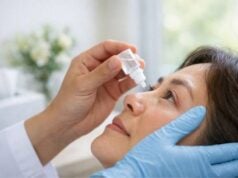
- Antiemetics: To prevent vomiting and possible increased intraocular pressure.
- Artificial Tears: Used sparingly to maintain surface lubrication if appropriate.
Non-Surgical Observation
- Very Small, Non-Penetrating Lacerations:
- May be managed conservatively with close follow-up.
- Daily or twice-daily ophthalmic examination to monitor for infection, wound healing, and complications.
What Not to Do
- Do not use contact lenses until cleared by your doctor.
- Avoid eye makeup, swimming, or exposure to dust during healing.
- Never self-medicate or delay professional assessment for deep or contaminated eye wounds.
Long-Tail Keywords Used Here:
- emergency treatment for corneal laceration
- antibiotic drops for eye cuts
- corneal injury first aid steps
Practical Advice:
Keep a pair of safety glasses handy at home and work, especially when handling sharp objects, chemicals, or engaging in activities with risk of flying debris.
Surgical and Procedural Interventions for Corneal Injury
The cornerstone of corneal laceration management—especially for moderate to severe or full-thickness injuries—is prompt, expert surgical intervention. Early surgery is vital for restoring the eye’s integrity, preserving vision, and preventing complications such as infection or scarring.
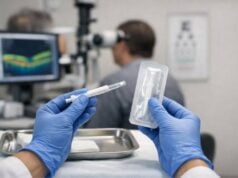
Primary Surgical Approaches
- Corneal Wound Repair
- Suturing: The majority of moderate to severe corneal lacerations are closed using very fine, dissolvable or non-dissolvable sutures under a microscope. The goal is to re-appose the wound edges, restore a watertight seal, and promote healing.
- Technique: Micro-surgical instruments and magnification ensure precise alignment. Suture placement and tension are critical for optimal visual outcomes.
- Practical Advice: Following surgery, protect your eye from accidental trauma, and avoid bending or lifting until cleared by your surgeon.
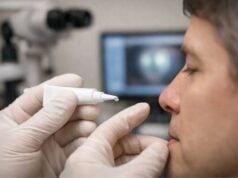
- Use of Tissue Adhesives (Glues)
- Indications: Small, partial-thickness lacerations may be closed using medical-grade tissue adhesives. This is a quick, non-suturing approach ideal for selected injuries.
- Limitations: Not suitable for deep, contaminated, or irregular wounds.
- Anterior Chamber Reformation
- If the eye’s internal fluid leaks out (flat anterior chamber), it may be necessary to inject a sterile fluid (balanced salt solution) to restore normal structure during surgery.
- Foreign Body Removal
- If a foreign object is present, it must be removed with great care to avoid further injury.
- Adjunct Procedures
- Corneal Patch Grafts: In cases where tissue is lost or the wound cannot be closed directly, a patch of donor cornea may be grafted in place.
- Combined Lens or Vitreoretinal Surgery: If the lens, retina, or other intraocular structures are injured, additional surgeries may be needed.
Postoperative Management
- Topical Antibiotics and Steroids: Prevent infection and control inflammation.
- Follow-Up Visits: Essential for suture removal (if necessary), monitoring healing, and early identification of complications.
Risks and Recovery
- Infection, suture-related problems, irregular astigmatism, or scarring may occur.
- With timely, skilled surgery, many patients recover significant vision.
Long-Tail Keywords Used Here:
- corneal laceration surgery steps
- wound closure techniques for eye injuries
- eye trauma repair procedures
Practical Advice:
Arrange for someone to drive you home after surgery, and keep all post-operative appointments for best results.
Cutting-Edge Advancements and Emerging Technologies
Eye trauma care is advancing rapidly, with new innovations promising to improve outcomes, reduce complications, and speed up healing for those with corneal lacerations.
Recent Breakthroughs in Repair and Healing
- Femtosecond Laser-Assisted Repair
- These lasers provide ultra-precise, minimally invasive wound closure in some cases, reducing tissue damage and improving healing consistency.
- Useful for complex lacerations where conventional suturing is challenging.
- Biodegradable and Smart Sutures
- New suture materials can dissolve at rates matched to individual healing, minimizing follow-up visits and reducing the risk of suture-related irritation.
- Some experimental sutures are embedded with medication, slowly releasing antibiotics or anti-inflammatory drugs.
- Next-Generation Tissue Adhesives
- Bioengineered glues now offer greater strength, flexibility, and biocompatibility, expanding the range of injuries that can be treated without sutures.
- Regenerative Cell Therapies
- Early studies are investigating the use of stem cells and regenerative medicine to enhance corneal healing and reduce scarring, potentially restoring better visual outcomes after severe lacerations.
- AI-Enhanced Diagnostics
- Artificial intelligence is now assisting in the rapid assessment of trauma, predicting risk of complications, and helping customize treatment plans for each patient.
Practical Advice:
Ask your ophthalmologist about clinical trials or new technologies available in your region. Participating in research can provide early access to cutting-edge treatments and help advance eye care for others.
Long-Tail Keywords Used Here:
- laser-assisted corneal repair
- advanced glue for eye wounds
- new corneal healing technology
Current Research Trials and Future Perspectives
The landscape of corneal trauma research is active, with multiple ongoing clinical trials and promising discoveries on the horizon.
Current and Upcoming Clinical Trials
- Novel Tissue Adhesives:
- Trials are evaluating bioactive glues that may outperform traditional sutures for select corneal lacerations, potentially reducing surgical time and scarring.
- Stem Cell and Growth Factor Therapies:
- Research is underway into stem cell-derived products and topical growth factors to stimulate corneal regeneration after injury.
- Smart Imaging and Telemedicine:
- New studies are testing AI-driven diagnostics and telemedicine triage systems for faster, more accurate emergency care, especially in rural or underserved areas.
- Customized Suture Materials:
- Investigational materials aim to tailor wound support and medication delivery directly to individual healing profiles.
Expected Advancements
- Faster healing with less scarring and better visual results
- Safer, more effective alternatives to suturing in selected cases
- Personalized care pathways based on advanced imaging and AI analysis
- Expanded access to expert trauma care through tele-ophthalmology
How to Stay Informed and Engaged
- Ask your ophthalmologist about new treatment options and research opportunities.
- Check for local or regional clinical trials via trusted registries.
- Join online or local eye health support groups to connect with others facing similar challenges.
Long-Tail Keywords Used Here:
- clinical trials for corneal injury
- future treatments for eye lacerations
- regenerative therapy for corneal wounds
Practical Advice:
Consider joining a clinical trial if eligible—it may open doors to new therapies and contribute to future breakthroughs in corneal trauma care.
Frequently Asked Questions
What is the most effective treatment for a corneal laceration?
The best treatment for corneal laceration depends on the depth and size of the wound. Surgical repair with fine sutures is the gold standard for most full-thickness injuries, while small, partial-thickness lacerations may heal with antibiotics and close monitoring.
How long does it take to recover from a corneal laceration?
Recovery can take from several days to a few months, depending on the injury’s severity and treatment type. Minor lacerations may heal within weeks, while deeper or surgically repaired wounds require longer healing and regular follow-up.
Can a corneal laceration heal without surgery?
Superficial or very small partial-thickness lacerations can sometimes heal with medical management and antibiotics. Full-thickness or deep wounds almost always need surgical intervention to prevent infection and preserve vision.
What are the risks of untreated corneal lacerations?
If left untreated, corneal lacerations may lead to severe infection (endophthalmitis), permanent scarring, vision loss, or even loss of the eye. Immediate evaluation and care are essential for the best prognosis.
Are there any new surgical techniques for repairing eye cuts?
Yes, innovations like femtosecond laser-assisted repair, bioengineered adhesives, and smart suture materials are transforming the way corneal injuries are treated, offering faster healing and better cosmetic and visual outcomes.
What should I do immediately if I suspect a corneal laceration?
Avoid touching or pressing on the eye, shield it gently (do not use a patch), and seek emergency medical attention right away. Do not attempt to remove any foreign body or use eye drops without a doctor’s approval.
Is vision always restored after corneal laceration repair?
Many people regain significant vision after timely repair, but outcomes depend on wound location, size, complications, and adherence to follow-up care. Some may experience permanent changes such as scarring or astigmatism.
Disclaimer:
This article is provided for educational and informational purposes only and does not replace professional medical advice. If you experience an eye injury or suspect a corneal laceration, seek immediate medical attention from a qualified healthcare provider.
If you found this resource helpful, please share it on Facebook, X (formerly Twitter), or any social media you enjoy. Your support helps us create more high-quality, accessible eye health guides for the community. Follow us for updates and new articles—thank you for making a difference!