Dry eye syndrome, also known as dry eye disease or keratoconjunctivitis sicca, is one of the most prevalent ocular surface disorders affecting millions worldwide. Characterized by a deficiency in tear production, poor tear quality, or both, dry eye leads to chronic irritation, visual disturbances, and reduced quality of life. The multifactorial nature of this disease makes management challenging, often requiring a personalized approach. This in-depth guide explores the latest understanding of dry eye syndrome, conventional and pharmacological therapies, surgical options, and the cutting edge of emerging innovations to help you or your loved ones achieve lasting relief and healthier eyes.
Table of Contents
- The Basics and Global Prevalence of Dry Eye Syndrome
- Mainstay Therapies and Medical Treatments
- Surgical and Procedural Approaches for Severe Cases
- Breakthroughs and Next-Generation Solutions in Dry Eye Care
- Clinical Trials and the Future of Dry Eye Treatment
- Frequently Asked Questions
The Basics and Global Prevalence of Dry Eye Syndrome
Dry eye syndrome is a chronic, multifactorial disorder of the tear film and ocular surface, resulting in discomfort, visual disturbances, and potential damage to the eye’s surface. The disorder arises when the eye fails to produce enough tears or when the quality of tears is inadequate, leading to increased evaporation or instability of the tear film.
Pathophysiology of Dry Eye Syndrome:
- Tear Deficiency: Reduced production of the aqueous component of tears, often from dysfunction of the lacrimal glands.
- Evaporative Dry Eye: Rapid loss of tears due to poor quality or dysfunction of the lipid layer, commonly due to meibomian gland dysfunction (MGD).
- Mixed Mechanisms: Many patients have overlapping features of both types.
Symptoms:
- Gritty, burning, or stinging sensations
- Sensitivity to light
- Fluctuating vision, especially with reading or computer use
- Redness, irritation, or feeling of “something in the eye”
- Excessive tearing (paradoxical response to dryness)
- Difficulty wearing contact lenses
Epidemiology and Prevalence:
- Estimates suggest 5% to 34% of adults globally have dry eye symptoms, with higher rates among women and older adults.
- Prevalence increases with age, hormonal changes (especially postmenopausal women), and prolonged screen time.
- Environmental factors like air conditioning, low humidity, and pollution contribute to higher risk.
Risk Factors:
- Female gender and advancing age
- Hormonal changes (pregnancy, menopause)
- Autoimmune diseases (Sjogren’s syndrome, rheumatoid arthritis, lupus)
- Contact lens use
- Digital device overuse (reduced blink rate)
- Certain medications (antihistamines, antidepressants, diuretics, beta-blockers)
- Refractive surgeries (LASIK, PRK)
- Environmental exposure (wind, smoke, dry climates)
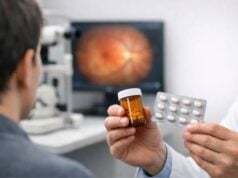
Diagnosis:
- Symptom Surveys: OSDI (Ocular Surface Disease Index), SPEED questionnaire
- Clinical Evaluation: Slit-lamp exam, tear breakup time (TBUT), Schirmer’s test, ocular surface staining, meibography
- Tear Film Analysis: Osmolarity measurement, inflammatory marker testing
Practical Advice:
If you experience persistent dryness, irritation, or fluctuating vision, schedule a comprehensive eye exam. Early diagnosis can prevent progression and improve comfort.
Mainstay Therapies and Medical Treatments
The management of dry eye syndrome typically begins with lifestyle changes and medical therapies. Effective treatment is personalized, often requiring a stepwise approach to control symptoms and prevent long-term complications.
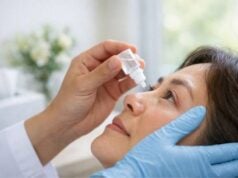
1. Artificial Tears and Lubricating Drops
- Over-the-counter artificial tears provide symptomatic relief and help restore the tear film.
- Preservative-free options are preferred for frequent use.
- Gels and ointments may be recommended for nighttime dryness.
2. Eyelid Hygiene and Warm Compresses
- Daily cleansing of the eyelids and lashes removes debris, bacteria, and reduces inflammation.
- Warm compresses help open meibomian glands, improving lipid layer quality.
3. Omega-3 Fatty Acid Supplementation
- Dietary omega-3s (from fish oil, flaxseed oil) may reduce inflammation and support tear production in some patients.
4. Prescription Eye Drops
- Cyclosporine (Restasis®, Cequa®): Reduces ocular surface inflammation and increases tear production.
- Lifitegrast (Xiidra®): Inhibits T-cell mediated inflammation, improving symptoms and signs.
- Corticosteroid Drops: Short-term use for acute flares, with careful monitoring for side effects.
- Autologous Serum Drops: Derived from the patient’s own blood, these drops contain growth factors to promote healing in severe cases.
5. Punctal Plugs
- Small devices inserted into tear ducts to slow tear drainage and conserve natural tears.
- Temporary (dissolvable) or permanent (silicone) options available.
6. Environmental and Lifestyle Modifications
- Use of humidifiers in dry environments
- Taking breaks from screens (“20-20-20 rule”: every 20 minutes, look at something 20 feet away for 20 seconds)
- Wearing wraparound sunglasses outdoors
- Staying hydrated and avoiding air vents directly blowing toward your face
7. Managing Contributing Medications
- Review your medication list with a healthcare provider; some drugs can exacerbate dry eye symptoms.
8. Systemic Therapies for Underlying Disease
- Treating associated autoimmune or hormonal disorders (e.g., Sjogren’s syndrome, thyroid disease) can improve ocular surface health.
Practical Advice:
Consistency is key—daily eyelid hygiene and regular use of artificial tears often make the biggest difference. Don’t hesitate to ask your eye doctor for custom recommendations.
Keywords Integrated:
- artificial tears for dry eye
- cyclosporine eye drops for dry eye
- warm compresses for meibomian gland dysfunction
- punctal plugs for chronic dry eye
Surgical and Procedural Approaches for Severe Cases
For patients with moderate to severe dry eye syndrome that remains uncontrolled with medical therapy, a range of in-office procedures and surgical treatments can provide significant relief and preserve ocular surface health.
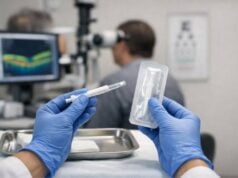
1. Punctal Occlusion Procedures
- Surgical closure of tear drainage ducts when plugs are ineffective or not tolerated.
- Provides lasting retention of tears, reducing the need for frequent lubricating drops.
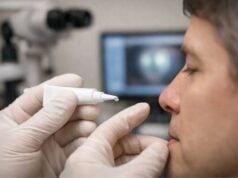
2. Meibomian Gland Expression
- Manual or device-assisted expression of blocked meibomian glands by an eye care professional.
- Can be combined with heating technologies for greater effectiveness.
3. Thermal Pulsation Devices
- In-office treatments (e.g., LipiFlow®, iLux®) use heat and gentle pressure to unclog and rejuvenate meibomian glands.
- Show significant improvement in symptoms for patients with evaporative dry eye.
4. Intense Pulsed Light (IPL) Therapy
- IPL targets abnormal blood vessels and inflammation along the eyelid margin.
- Helps restore healthy meibomian gland function and reduce ocular surface inflammation.
5. Amniotic Membrane Transplantation
- For severe or recalcitrant cases, especially when there is significant ocular surface damage.
- Amniotic membranes (placed on the eye) promote healing and reduce inflammation.
6. Tarsorrhaphy
- Partial surgical closure of the eyelids to decrease exposure in cases of extreme dryness or corneal ulceration.
7. Scleral Contact Lenses
- Large-diameter lenses that vault over the cornea, creating a reservoir of fluid to bathe and protect the ocular surface.
8. Other Advanced Procedures
- Blepharoplasty to correct eyelid malpositions contributing to exposure.
- Conjunctival or salivary gland transplantation (rare, specialized cases).
Practical Advice:
If your dry eye symptoms are severe and impacting daily life despite standard treatments, ask your provider about advanced in-office or surgical options. Early intervention can protect vision and prevent complications.
Keywords Integrated:
- punctal occlusion surgery for dry eye
- LipiFlow for meibomian gland dysfunction
- intense pulsed light therapy for dry eye
- scleral lenses for ocular surface disease
Breakthroughs and Next-Generation Solutions in Dry Eye Care
The past few years have witnessed significant progress in understanding dry eye syndrome’s pathogenesis and in the development of novel diagnostics, therapeutics, and digital solutions.
1. New Prescription Medications
- Reproxalap: A novel anti-inflammatory agent targeting aldehyde pathways, now in late-stage trials.
- NOV03 (Perfluorohexyloctane): A first-in-class therapy for evaporative dry eye, especially for patients with meibomian gland dysfunction.
- Topical Nerve Growth Factor (NGF): For severe neurotrophic keratitis and corneal healing.
2. Biologic and Gene-Based Therapies
- Stem cell–derived products, cytokine modulators, and gene editing approaches are being explored for severe, refractory cases and underlying autoimmune causes.
3. Digital and AI-Driven Diagnostics
- Automated tear film analysis (osmolarity, lipid layer assessment) via smartphone-connected devices.
- AI-assisted grading of ocular surface staining and meibography for precise monitoring.
- Wearable blink sensors and mobile reminders to promote healthy blinking.
4. Next-Generation Devices and Implants
- Smart punctal plugs that release medications over time.
- Ocular surface microstimulation devices to enhance tear production.
5. Advanced Contact Lens Technologies
- Drug-eluting and biosensing contact lenses for both treatment and monitoring of dry eye disease.
6. Personalized and Integrative Approaches
- Tailoring therapy based on inflammatory biomarkers, genetics, and real-time symptom tracking.
- Integrating lifestyle, nutrition, and environmental monitoring into comprehensive care plans.
Practical Advice:
Stay informed about clinical trials and new therapies—many are now available at specialty centers. Consider enrolling in a registry or research study to access cutting-edge care and contribute to scientific progress.
Keywords Integrated:
- latest treatments for dry eye syndrome
- AI diagnostics for dry eye
- gene therapy for ocular surface disease
- biologic eye drops for dry eye
Clinical Trials and the Future of Dry Eye Treatment
Research into dry eye syndrome continues to accelerate, with a robust pipeline of new therapies and diagnostic innovations poised to reshape clinical practice.
Current Areas of Focus:
- Novel Drug Candidates:
- Anti-inflammatory, anti-oxidant, and tear-stabilizing molecules in phase II/III trials.
- Repurposing of immunomodulatory agents from other autoimmune diseases.
- Regenerative and Cellular Therapies:
- Stem cell transplantation for glandular repair.
- Autologous platelet-rich plasma and amniotic exosomes for advanced cases.
- Implantable and Drug Delivery Devices:
- Long-acting punctal plugs and ocular inserts releasing medications over weeks or months.
- Digital Health and Telemedicine:
- Remote monitoring of ocular surface health using connected devices.
- Virtual reality–based rehabilitation for patients with vision loss from chronic dry eye.
Ongoing Clinical Trials:
- Recruitment is active for many therapies targeting tear film stability, inflammation, and neurotrophic factors.
- Trials for device-based therapies (thermal pulsation, smart plugs, and biosensors) are expanding access to new technology.
Expected Advancements:
- More personalized, biomarker-driven approaches for subtyping and targeting therapy.
- Expanded access to advanced diagnostics, especially in primary care and remote settings.
- Incorporation of AI for earlier detection and ongoing management.
Engaging with Clinical Research:
- Discuss with your eye doctor or a research coordinator about trials you may qualify for.
- Participation may provide access to new treatments and specialized care.
Practical Advice:
Check national and international clinical trial registries for studies recruiting dry eye patients. Patient advocacy organizations are valuable for learning about the latest advances and connecting with research centers.
Keywords Integrated:
- clinical trials for dry eye treatments
- regenerative medicine for dry eye
- future therapies for dry eye disease
- digital health for ocular surface disorders
Frequently Asked Questions
What causes dry eye syndrome?
Dry eye syndrome is caused by insufficient tear production or poor tear quality, often due to age, hormonal changes, autoimmune disease, medications, or environmental factors.
What is the best treatment for dry eye?
The best treatment is personalized, often combining artificial tears, prescription eye drops, eyelid hygiene, lifestyle changes, and, if needed, advanced procedures like punctal plugs or thermal pulsation.
How do you permanently treat dry eye?
Permanent cures are rare, but controlling underlying causes, daily lid hygiene, medical treatments, and in some cases, surgery, can greatly reduce symptoms and prevent progression.
Can dry eye syndrome be serious?
If left untreated, dry eye can cause vision impairment, corneal ulcers, or scarring. Early diagnosis and proper management usually prevent serious complications.
Are there new treatments for dry eye syndrome?
Yes, new drugs, biologics, advanced devices, and gene therapies are under investigation, with several approved in recent years and more in clinical trials.
Can diet help dry eye disease?
A diet rich in omega-3 fatty acids and antioxidants may support eye surface health. Staying hydrated and limiting alcohol/caffeine can also help reduce symptoms.
Disclaimer:
This guide is for educational purposes only and should not be used as a substitute for professional medical advice, diagnosis, or treatment. Always consult a qualified healthcare provider with questions about your eye health or any medical condition.
If you found this article helpful, please share it on Facebook, X (formerly Twitter), or any platform you prefer, and consider following us for more up-to-date eye care resources. Your support helps us continue to produce quality content for everyone.