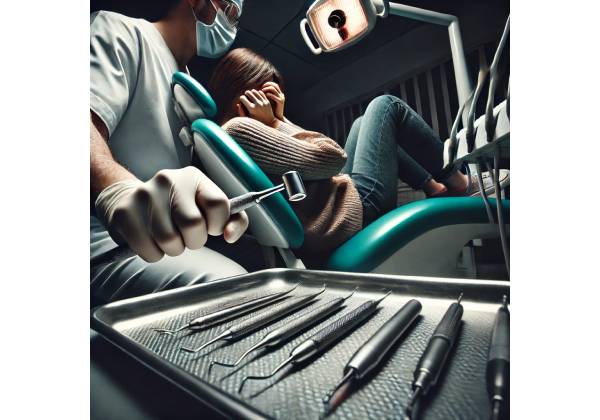
A routine dental visit can feel mildly stressful for almost anyone. Dentophobia is different. It is an intense, persistent fear of dental care that can trigger panic, avoidance, and a strong sense of helplessness long before a person reaches the chair. Some people fear drills, needles, pain, gagging, loss of control, or bad news about their teeth. Others react to the sounds, smells, or memory of a difficult past experience. Over time, this fear can become more than a passing problem. It can delay cleanings, worsen oral health, and turn small, manageable issues into urgent and costly ones. Because dentophobia often hides behind missed appointments, embarrassment, or “I will go later,” it is frequently misunderstood. Recognizing the pattern early matters. With the right assessment, supportive dental care, and evidence-based treatment, this fear can become far more manageable.
Table of Contents
- What Dentophobia Means
- Signs and Symptoms
- Causes and Risk Factors
- Diagnosis and Assessment
- Daily Life and Complications
- Treatment Options
- Management and When to Seek Help
What Dentophobia Means
Dentophobia is an intense fear of dental treatment or the dental setting. It is also commonly called odontophobia or severe dental phobia. In everyday conversation, people often use the terms dental fear, dental anxiety, and dental phobia interchangeably, but they are not identical. Dental fear may be brief and tied to a specific procedure. Dental anxiety may involve worry before an appointment, even when the person still goes through with care. Dentophobia usually describes the more severe end of the spectrum, where the fear is persistent, feels overwhelming, and leads to strong avoidance or extreme distress.
That distinction matters because many people dislike dental work without meeting the threshold of a phobia. Dentophobia becomes more clinically important when the reaction is clearly out of proportion to the actual risk and begins to shape behavior. A person may cancel repeatedly, postpone care for years, or tolerate dental visits only with intense panic, dissociation, or rigid coping rituals. The fear may center on pain, injections, drilling, choking, gagging, helplessness, shame about oral health, or the possibility of hearing bad news from the dentist.
For some people, the trigger is narrow. They may cope with an exam but panic at the idea of an extraction or local anesthetic. For others, the trigger is broader and starts before the visit itself. Booking the appointment, sitting in the waiting room, smelling the clinic, hearing instruments, or seeing staff prepare equipment can all set off the response. Children may not describe the fear clearly, but they may cling, cry, freeze, become angry, or refuse treatment.
Dentophobia is not simply stubbornness or poor motivation. It is a real fear pattern that can become self-reinforcing. Avoidance brings short-term relief, which teaches the brain that staying away was the only safe option. Over time, that can make the next appointment feel even more threatening. This is one reason dentophobia can quietly worsen over months or years.
A useful way to understand the condition is to ask two questions: What exactly feels dangerous, and what does the person do to stay safe? The answers reveal the structure of the fear. Once that pattern is clear, treatment becomes more focused and much more effective.
Signs and Symptoms
The symptoms of dentophobia can appear well before treatment begins. Some people feel anxious for days or weeks before an appointment. Others experience a sharp, immediate reaction as soon as they think about the dentist. The most common feature is a strong fear response that feels difficult to control, even when the person knows the level of danger is probably exaggerated.
Emotional symptoms often include:
- dread before appointments
- panic or near-panic in the clinic
- intense worry about pain, choking, injections, or loss of control
- embarrassment about the condition of the teeth or gums
- shame after cancelling or avoiding care
- irritability or agitation when dental treatment is discussed
Physical symptoms may include:
- sweating
- trembling
- nausea
- dizziness
- rapid heartbeat
- shortness of breath
- muscle tension
- dry mouth
- feeling faint or detached
These reactions can occur in the waiting room, during the dental examination, or even while trying to schedule a visit. In severe cases, the body responds as if the person is facing immediate danger, not routine care.
Behavioral signs are often easier for family members, dentists, and the person themselves to notice. These can include:
- repeatedly delaying checkups or cleanings
- cancelling appointments at the last minute
- only seeking care when pain becomes severe
- insisting on very specific conditions before attending
- avoiding certain procedures, such as injections or extractions
- needing repeated reassurance
- leaving during treatment or refusing to sit in the chair
Children may show a different pattern. Instead of describing fear directly, they may cry, cling to a caregiver, shut down, resist opening the mouth, or become disruptive. Adults may hide the fear behind excuses about money, timing, or being too busy, even when the emotional reason is stronger.
Dentophobia often becomes more concerning when avoidance starts to spread. A person may first avoid one type of procedure, then all invasive treatment, then routine exams, and eventually the whole dental setting. At that point, the condition affects not only anxiety levels but also general health, confidence, eating comfort, speech, and appearance. The fear is no longer limited to the appointment. It begins to shape daily life.
Causes and Risk Factors
Dentophobia usually develops through a combination of experience, personality, learned expectations, and physical sensitivity. There is rarely one single cause. In many cases, the fear can be traced to a difficult dental or medical experience, especially one that involved pain, restraint, choking sensations, poor communication, or feeling trapped. A frightening event in childhood may remain vivid for years, even if later dental techniques are gentler and more effective.
Several common causes and contributing factors stand out:
- previous painful or traumatic dental treatment
- fear of injections, drills, bleeding, or extractions
- a strong gag reflex or fear of choking
- hearing stories about painful dental experiences from others
- feeling ashamed about oral health and expecting judgment
- high general anxiety or panic sensitivity
- past trauma unrelated to dentistry, especially when close physical proximity feels threatening
The sensory aspect of dentistry can also play a powerful role. The smell of dental materials, the sound of a drill, the bright lights, the vibration of instruments, and the physical position in the chair can all become conditioned triggers. Once the brain links those cues to danger, the environment itself can provoke anxiety even before treatment begins.
Loss of control is another major factor. Dental care requires a person to lie back, keep the mouth open, and tolerate tools they cannot easily see or predict. For individuals who are already sensitive to vulnerability, that can be especially difficult. Some people do not primarily fear pain. They fear not being able to stop the procedure, speak freely, swallow comfortably, or regain control quickly.
Family and developmental influences matter too. Children may absorb fear from anxious parents or from repeated warnings that frame dentistry as threatening. On the other hand, overly delayed first visits can also make the setting feel unfamiliar and alarming. Adults with longstanding dentophobia often describe a pattern that began early and was strengthened by years of avoidance.
Certain risk factors increase the chance that dental fear becomes severe:
- childhood trauma linked to healthcare or dentistry
- a history of fainting, panic attacks, or strong bodily anxiety
- highly sensitive pain expectations
- neurodevelopmental differences that make sensory overload more likely
- limited trust in healthcare settings
- irregular dental attendance, which increases the chance of needing invasive treatment later
This last point creates a common cycle. Fear leads to avoidance. Avoidance leads to worsening oral problems. Worsening oral problems make the next visit more complex, painful, embarrassing, or expensive. That, in turn, strengthens the fear. Breaking that cycle is central to recovery.
Diagnosis and Assessment
There is no blood test or scan that diagnoses dentophobia. Identification begins with a careful history and an honest description of what happens before, during, and after dental care. A clinician, dentist, psychologist, or physician may ask what the person fears most, how long the fear has been present, what situations are avoided, and how much the problem interferes with health or daily functioning.
One useful clinical question is simple: Is this discomfort, anxiety, or phobia? Many people feel tense in the dental chair, but a phobic pattern usually involves intense fear, strong avoidance, and distress that is clearly greater than the situation would normally justify. The person may know the reaction is excessive, yet still feel unable to control it. Diagnosis also involves understanding how predictable the response is. If nearly every dental contact leads to panic, refusal, or severe distress, the pattern is more likely to be clinically significant.
Assessment often includes screening tools. In adults, dentists and healthcare professionals may use short questionnaires such as the Modified Dental Anxiety Scale, which helps estimate the level of dental anxiety and identify people who may need extra support or referral. In children, age-appropriate rating scales, picture-based tools, and behavior observation methods are commonly used because younger patients may have trouble naming their fear precisely.
A thorough assessment usually covers:
- the exact trigger, such as injections, drilling, gagging, or the whole dental environment
- the person’s thoughts about what they believe will happen
- physical symptoms, including faintness, panic, or nausea
- avoidance patterns, missed appointments, and last-minute cancellations
- consequences for oral health, eating, sleep, self-confidence, and pain
- related conditions, such as generalized anxiety, trauma symptoms, sensory sensitivity, or depression
Good assessment also rules out issues that may need a different response. A severe gag reflex, temporomandibular pain, previous anesthetic complications, or trauma history can change how dental care should be planned. In some cases, the person is not only afraid. They have a legitimate physical or psychological vulnerability that deserves tailored treatment.
The goal of diagnosis is not to label someone as “difficult.” It is to identify barriers to safe and effective care. Once the pattern is clear, the dental team can decide whether routine chairside support is enough, whether behavioral treatment is needed, or whether sedation, trauma-informed planning, or specialist referral should be considered.
Daily Life and Complications
Dentophobia can affect far more than dental attendance. Because oral health is tied to comfort, appearance, nutrition, sleep, and social confidence, avoidance can gradually influence many areas of life. A person may begin by skipping routine cleanings, but the long-term effects often spread beyond the clinic.
One of the most common complications is delayed care. Small cavities, mild gum inflammation, and early tooth sensitivity are usually easier to treat than advanced decay, infection, or broken teeth. When fear leads to postponement, the eventual treatment is often more invasive, more expensive, and more stressful. That reinforces the person’s belief that dental care is something to dread.
Daily life may be affected in subtle ways. Some people chew only on one side, avoid cold foods, limit smiling, cover their mouth while speaking, or stop laughing freely because they are self-conscious about their teeth. Others live with chronic discomfort, bad breath, sleep disruption, or recurring infection because they feel unable to seek help promptly. The emotional burden can be heavy, especially when shame becomes part of the problem.
Dentophobia is also linked with a cycle of worsening oral health and reduced quality of life. Common consequences include:
- untreated cavities and tooth loss
- worsening gum disease
- dental abscesses or repeated infections
- difficulty eating certain foods
- visible damage that affects confidence
- dependence on painkillers instead of treatment
- emergency-only dental attendance
Children may develop their own version of this cycle. If they avoid care until pain is severe, visits may become more urgent and more frightening. That can make trust harder to build and can influence how they view dentistry into adolescence and adulthood.
The condition can also affect relationships with healthcare professionals. People with dentophobia sometimes expect criticism, disbelief, or pressure. As a result, they may avoid not only the dentist but also discussions about oral health with partners, family members, or doctors. The fear becomes isolating.
A key clinical point is that complications often develop slowly. Many people adapt to their fear and normalize a restricted, painful, or avoidant routine. They may not seek help until they face visible swelling, severe pain, or a major restorative need. Early recognition matters because it is easier to treat dentophobia before avoidance has shaped years of dental neglect and emotional distress.
Treatment Options
Effective treatment for dentophobia usually combines two goals: reducing the fear itself and making needed dental care possible in a safer, more tolerable way. The right plan depends on severity. Someone with mild to moderate anxiety may respond well to clear communication and gradual exposure inside the dental office. Someone with severe dentophobia may need structured psychological treatment, specialized dental planning, or temporary use of sedation to begin breaking the avoidance cycle.
The most established psychological treatment is cognitive behavioral therapy, often combined with graded exposure. This approach helps the person identify catastrophic expectations, understand how avoidance keeps fear alive, and practice approaching feared situations in small, manageable steps. Exposure may begin far from the actual procedure. It can involve talking about the dentist, looking at dental instruments, sitting in the waiting room, reclining in the chair, or practicing brief examinations before moving on to more difficult treatment steps.
Treatment often works best when it includes:
- a calm, nonjudgmental explanation of what will happen
- agreed stop signals so the patient feels more control
- shorter appointments at first
- staged treatment rather than one long session
- relaxation or breathing exercises
- gradual exposure to feared cues
- collaboration between dental and mental health professionals when needed
For children, behavior guidance is especially important. Techniques such as predictable communication, desensitization, distraction, modeling, and positive reinforcement can significantly improve cooperation and reduce anxiety. For severely anxious adults, similar principles still apply, even if the language and pacing differ.
Sedation can help some patients receive urgent or necessary care, but it is usually not the whole solution. Nitrous oxide, oral sedation, or other forms of conscious sedation may reduce immediate distress, especially when treatment cannot be delayed. In some cases, general anesthesia is considered, particularly when extensive work is needed and other approaches are not feasible. Still, sedation alone does not necessarily change the fear pattern long term. If the goal is lasting improvement, the underlying phobia also needs attention.
Trauma-informed care can be essential for certain patients. This means pacing treatment carefully, explaining each step, respecting boundaries, and reducing elements that can make the patient feel trapped or overwhelmed. For some people, the problem is not just dental pain. It is the emotional meaning of the dental setting.
Treatment is often more successful when the person does not wait for fear to vanish before taking action. Progress usually comes from repeated experiences of tolerating dental care more successfully than expected. That new learning, built gradually, is what begins to weaken the phobia.
Management and When to Seek Help
Self-management is not a replacement for treatment, but it can make dentophobia more workable and reduce the chance that avoidance keeps deepening. The most helpful mindset is practical rather than perfectionistic. The goal is not to become completely relaxed immediately. The goal is to make the next step possible.
Useful day-to-day strategies include:
- telling the dental office in advance about the fear
- scheduling early appointments to reduce time spent anticipating
- asking for a clear treatment plan before the visit
- agreeing on a stop signal, such as raising a hand
- bringing headphones or using guided breathing before the procedure
- starting with a consultation rather than treatment
- choosing one manageable goal for each visit
It also helps to identify safety behaviors that reduce panic briefly but keep fear strong over time. Examples include repeatedly cancelling, demanding constant reassurance, or delaying until pain forces emergency treatment. These patterns are understandable, but they usually make the long-term problem worse.
Keeping up with basic oral care at home matters as well. Good brushing, flossing, fluoride use, and prompt attention to early symptoms can reduce the chance that treatment becomes more invasive later. This does not solve the phobia, but it can lower the practical burden it creates.
Professional help is a good idea when:
- fear causes repeated cancellations or years without routine care
- dental problems are worsening because of avoidance
- panic symptoms are intense
- the person can attend only in crisis
- shame, depression, or hopelessness are becoming part of the picture
- past trauma seems closely tied to the fear
More urgent dental or medical attention is needed when there is facial swelling, fever, pus, uncontrolled bleeding, severe tooth pain, difficulty chewing, or signs of spreading infection. Waiting because of fear can allow serious problems to become dangerous.
The outlook for dentophobia is often better than people expect. Fear of the dentist can be deeply ingrained, but it is also treatable. Many people improve through a combination of careful dental support, graded exposure, and better control over the pace of care. Progress may start with something as small as attending an assessment visit without leaving. That still counts. In phobia treatment, small steps are often the ones that change the future.
References
- Etiology of Dental Anxiety and Dental Phobia: Review 2025. (Review)
- Assessment of Dental Fear and Anxiety Tools for Children: A Review 2025. (Review)
- Interdisciplinary CBT treatment for patients with odontophobia and dental anxiety related to psychological trauma experiences: a case series 2024. (Case Series)
- Impact of Dental Anxiety on Dental Care Routine and Oral-Health-Related Quality of Life in a German Adult Population—A Cross-Sectional Study 2023.
- Clinical standards for dental anxiety management 2023. (Guideline)
Disclaimer
This article is for educational purposes only and is not a substitute for dental, medical, or mental health care. Severe fear of dental treatment can overlap with trauma-related symptoms, panic, sensory intolerance, or other anxiety conditions, and untreated oral disease can become serious. If dentophobia is causing you to avoid care, live with pain, or delay urgent treatment, seek help from a qualified dentist, doctor, or mental health professional.
If this article was helpful, please share it on Facebook, X, or another platform that fits your audience.






