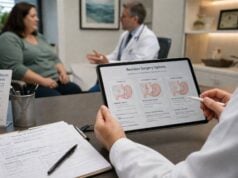
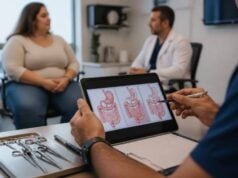
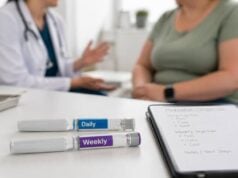
There is a real connection between vitamin D and weight loss, but it is not the simple cause-and-effect story that supplement marketing often implies. People with overweight and obesity are more likely to have low vitamin D levels, and losing weight can sometimes improve vitamin D status. But that does not mean vitamin D supplements directly make fat loss happen.
For most adults, the evidence suggests vitamin D is better understood as a related health factor than a stand-alone weight loss tool. Correcting a true deficiency can still matter for bone health, energy, muscle function, and overall well-being, and those things can affect how well someone sticks with a fat loss plan. The more useful question is not whether vitamin D is a hidden fat burner. It is whether low vitamin D is one piece of a bigger picture that may influence progress, recovery, and long-term maintenance.
Table of Contents
- What the real connection looks like
- Why low vitamin D is common in obesity
- Does vitamin D supplementation cause weight loss
- When vitamin D can still matter for progress
- Should you test or supplement
- Safe dosing, food and upper limits
- How vitamin D fits into plateaus and maintenance
What the real connection looks like
The most accurate short answer is this: vitamin D has a real relationship with body weight, but the evidence does not support treating it as a proven fat-loss supplement.
That distinction matters because two ideas often get blended together online:
- Idea one: people with obesity are more likely to have lower vitamin D levels.
- Idea two: taking vitamin D will help people lose weight.
The first statement is well supported. The second is much weaker.
Vitamin D is best known for its role in calcium balance, bone health, and muscle function, but it also interacts with immune activity, inflammation, and some metabolic pathways. That broader biological role is one reason people have wondered whether low vitamin D could make fat loss harder. It is a reasonable question. If deficiency affects energy, muscle function, mood, or general health, then it could indirectly make it harder to train well, recover well, stay active, or stick with a calorie deficit.
Still, indirect is not the same as direct. A supplement can support health without being a true weight loss driver.
A practical way to think about the evidence is this:
| Question | Most evidence-supported answer |
|---|---|
| Is low vitamin D more common at higher body weights? | Yes |
| Does vitamin D deficiency automatically explain a weight loss stall? | No |
| Does taking vitamin D alone usually cause meaningful fat loss? | No |
| Can correcting a true deficiency still matter for health and consistency? | Yes |
| Can weight loss itself improve vitamin D status? | Often, yes |
That is why vitamin D belongs in a weight loss conversation, but usually not as the main answer. If progress is slow, it is more often because of calorie creep, lower daily movement, low protein, poor sleep, inconsistent weekends, or a plateau that is not being judged over enough time. Readers sorting through those broader issues may find what to check first in a weight loss plateau or what you might be missing when the scale is not moving more useful than jumping straight to supplements.
Why low vitamin D is common in obesity
One reason the topic gets confusing is that low vitamin D is clearly linked with obesity, but the direction of that relationship is not as simple as “low vitamin D causes weight gain.”
Several mechanisms may help explain why vitamin D levels tend to be lower in people with higher body weight.
First, vitamin D is fat-soluble. That means it can be distributed into a larger body mass and stored in adipose tissue, leaving less circulating in blood tests. This is one reason researchers often describe obesity as being associated with lower measured vitamin D status rather than with poor intake alone.
Second, heavier body weight may blunt the response to supplementation. Two people can take the same daily dose and still end up with different blood levels. In practice, higher-BMI individuals often show a smaller increase in blood vitamin D levels from the same supplement dose.
Third, lifestyle patterns that travel with obesity can also contribute. Less outdoor time, lower sunlight exposure, lower fitness, more sedentary time, less dietary variety, and certain health conditions or medications can all affect vitamin D status.
That is why low vitamin D often behaves more like a marker of the broader situation than like a single root cause. Someone with obesity, low activity, poor sleep, low fish intake, limited sun exposure, and a mostly indoor routine may have low vitamin D because those factors cluster together. Correcting the deficiency can still be useful, but it does not erase the rest of the picture.
There is also a helpful reverse observation: when people lose weight, vitamin D status often improves. That supports the idea that higher body weight itself contributes to lower circulating vitamin D, not just the other way around.
This is a good example of why “one blood marker explains everything” is usually the wrong model for stalled fat loss. Low vitamin D can matter, but it often sits beside other issues instead of replacing them. In real life, the better question is usually, “Is vitamin D one of several things making adherence, recovery, or health harder?” not “Is vitamin D the reason I cannot lose weight?”
If your situation also includes fatigue, muscle weakness, low mood, bone concerns, limited sun exposure, or other medical questions, it can make sense to look more broadly at possible barriers instead of assuming the answer is only nutritional. In that setting, blood tests to ask about when you cannot lose weight and medical reasons to consider when weight loss feels unusually hard may be more relevant than supplement claims alone.
Does vitamin D supplementation cause weight loss
For most adults, vitamin D supplementation alone does not appear to cause meaningful weight loss.
That is the main answer people usually want, and it is also where disappointment tends to happen. The supplement industry often frames vitamin D as a metabolic upgrade that will unlock fat loss once your levels are “optimized.” Clinical evidence does not support that kind of promise.
The best summary of the current evidence looks like this:
- observational studies often find that higher body weight and lower vitamin D levels travel together
- randomized trials usually do not show that vitamin D supplements alone lead to major reductions in body weight
- some meta-analyses report small improvements in certain body composition or waist-related measures
- newer reviews tend to find that any effect is inconsistent, modest, or limited to specific subgroups rather than broadly reliable
That last point matters. The evidence is not perfectly one-sided. Some pooled analyses suggest vitamin D may slightly improve a few anthropometric measures in some settings. But when newer and more condition-specific reviews look at adults with obesity or metabolic disorders, the overall effect on body weight is usually weak or absent.
In other words, even where there may be small subgroup effects, vitamin D is not performing like a dependable weight loss intervention.
This is why it helps to separate three different goals:
- Treating deficiency
- Supporting general health
- Trying to lose body fat
Vitamin D may be appropriate for the first two. It is not strongly supported as a primary tool for the third.
A common misunderstanding is that because deficiency is linked with obesity, supplementation must reverse obesity. That does not follow automatically. Many health markers move with weight without acting as independent levers for fat loss. Sleep quality, inflammation, blood pressure, insulin sensitivity, and vitamin D status can all improve when body composition improves. That does not mean pushing one marker upward by itself recreates the whole effect of weight loss.
The more grounded approach is to see vitamin D as supportive, not central. If you are truly deficient, correcting that may help you feel better overall. But the day-to-day drivers of fat loss still tend to be calorie intake, dietary quality, protein, activity, sleep, and consistency. People who want to focus on the levers that most directly affect progress are often better served by tightening the basics in what to eat in a calorie deficit or by fixing common diet mistakes that stall weight loss before expecting a supplement to move the scale.
When vitamin D can still matter for progress
Saying vitamin D is not a proven fat-loss supplement does not mean it is irrelevant. It can still matter in practical ways that influence progress.
The clearest case is true deficiency. If vitamin D is low enough to affect bone health, muscle function, or general well-being, that can make a weight loss plan harder to follow. Someone who feels worn down, less active, more achy, or generally unwell may struggle to train consistently, walk enough, or stay engaged with food prep and routines. The vitamin is not “burning fat,” but fixing a deficiency can remove friction.
Vitamin D may also matter more in a few specific situations:
- limited sun exposure for long periods
- darker skin living in low-sun environments
- older age
- bariatric surgery history
- malabsorption disorders
- certain medications that affect vitamin D metabolism
- fracture risk, osteopenia, or osteoporosis concerns
In these settings, the goal is not cosmetic weight loss. The goal is correcting a health issue that could undermine energy, recovery, or long-term resilience.
There is also a body-composition angle worth mentioning. During fat loss, especially aggressive fat loss, people need enough resistance training, protein, sleep, and recovery to protect lean mass. Vitamin D is not the star of that process, but it sits in the background of musculoskeletal health. A deficiency is not something you want to ignore while trying to preserve performance and function.
This is where nuance helps. If someone says, “I am in a deficit but feel tired, flat, weak, and less active than usual,” vitamin D might be one of several things worth checking. If someone says, “I feel fine but the scale has not moved for 10 days,” vitamin D is much less likely to be the key issue than normal fluctuation, undercounting, sodium shifts, constipation, or a shrinking deficit.
That is also why supplement decisions should be matched to the real problem. A person whose main issue is an unstructured diet does not need vitamin D as a plateau solution. A person with documented deficiency, minimal daylight exposure, and a history that makes deficiency more likely may reasonably need both a better plan and correction of a nutrient issue.
For readers who are trying to sort out whether the problem is a true stall or a misleading short-term fluctuation, how to tell whether you are in a real plateau and water, glycogen and sodium when the scale is not moving are usually more directly useful than assuming the answer is biochemical.
Should you test or supplement
This is where practical judgment matters more than hype.
Not everyone trying to lose weight needs vitamin D testing. In fact, routine screening of otherwise healthy adults simply because they have obesity is not something guidelines strongly support in every case. But that does not mean testing is never useful. It means testing should be tied to risk, symptoms, history, or a clear reason to act on the result.
Testing makes more sense when there are additional clues, such as:
- very limited sun exposure
- a history of deficiency
- bariatric surgery
- osteoporosis or fracture risk
- malabsorption conditions
- chronic fatigue or muscle weakness without a clear explanation
- medications or health issues that make deficiency more likely
Supplementing without testing can also be reasonable in some cases, especially when the dose is modest and the goal is general adequacy rather than aggressive correction. But it is different from treating a confirmed deficiency. A basic maintenance supplement is one thing. High-dose repletion without knowing the starting point is another.
A sensible framework looks like this:
| Situation | Practical approach |
|---|---|
| Healthy adult with overweight and no clear risk factors | Routine testing is often unnecessary |
| High deficiency risk or symptoms suggestive of low vitamin D | Discuss testing with a clinician |
| Known deficiency | Treat based on clinician guidance and recheck if appropriate |
| General health maintenance with low sun exposure | A modest supplement may be reasonable |
| Trying to force faster fat loss | Vitamin D is not the right main tool |
One more important point: blood levels are part of the decision, but so is context. The “right” plan is not just a number. It is the number plus symptoms, medical history, diet, sun exposure, and what problem you are actually trying to solve.
If you are unsure whether your issue belongs in the supplement bucket or the medical-evaluation bucket, when to talk to a doctor before weight loss and when to see a doctor about weight gain or trouble losing weight are usually more helpful than guessing.
Safe dosing, food and upper limits
Vitamin D is one of those nutrients that sounds harmless enough to encourage casual overuse. That is a mistake. It is fat-soluble, which means excessive supplementation can build up and create real problems, especially through high calcium levels.
For many adults, the conversation is not about megadoses. It is about getting enough consistently and safely.
Vitamin D can come from three main places:
- sunlight exposure
- food
- supplements
Food sources include fatty fish, fortified dairy products, fortified plant milks, fortified cereals, and egg yolks, though diet alone is often not enough for people with limited sun exposure or higher needs. Supplements usually come as vitamin D3 or vitamin D2, with D3 commonly used in over-the-counter products.
A few practical points help keep the topic grounded:
- More is not automatically better.
- Taking vitamin D “for metabolism” is not a reason to use high doses indefinitely.
- People with obesity may not raise blood levels as much from the same dose as lower-weight individuals, but that still does not justify self-prescribing very large amounts.
- Vitamin D can interact with certain medical conditions and some medications.
- Very high intakes can lead to hypercalcemia, kidney problems, digestive symptoms, and other complications.
That last point matters because supplement advice online often drifts upward fast. People start with a reasonable maintenance dose, then stack multiple products, then add calcium, then stop checking what their total intake actually is.
Moderate, consistent supplementation makes more sense than random large doses driven by social media claims. In everyday use, the safer mindset is “enough to correct or maintain adequacy” rather than “enough to force a metabolic effect.”
Food quality still matters too. A person relying on supplements while eating poorly is usually missing the bigger picture. Vitamin D does not replace protein, fiber, diet quality, recovery, or activity. It works best as one small part of an overall health plan rather than as a shortcut. People who want the basics in place first usually get more return from building meals around protein, fiber and volume foods and from using a high-protein, high-fiber meal structure than from hunting for special nutrient hacks.
How vitamin D fits into plateaus and maintenance
Vitamin D is usually not the first thing to blame for a weight loss plateau, but it can still belong in the maintenance conversation.
During active fat loss, people often want one hidden reason to explain why progress slowed. The temptation is to focus on something interesting and invisible rather than something ordinary and fixable. That is why supplements, hormones, and blood markers get so much attention. They feel more precise than saying, “Your weekend intake drifted up and your daily movement drifted down.”
Most true stalls are still explained by familiar factors:
- the calorie deficit has narrowed as body weight dropped
- food tracking got less accurate
- activity outside workouts fell
- hunger increased and portions crept up
- sleep worsened
- social eating increased
- scale noise is hiding slow progress
Vitamin D is more likely to matter at the edges than at the center. It matters when deficiency adds fatigue, lower activity, poorer recovery, or health complications that make consistency harder. It matters when someone has real risk factors for low vitamin D and the issue is being ignored. It matters after bariatric surgery or in other higher-risk medical settings. But it is rarely the main reason a plateau exists.
The same logic applies in maintenance. Vitamin D will not “lock in” weight loss. Still, maintenance is easier when overall health is not working against you. Adequate nutrient status, better musculoskeletal function, enough sleep, enough protein, and a sustainable routine all make it easier to hold the result. Maintenance tends to fail because systems get loose, not because one supplement stopped being magical.
That is the most useful final answer to the title question. Yes, there is a real connection between vitamin D and weight loss. But the connection is mostly about association, deficiency risk, and general health support, not about vitamin D directly melting body fat. For most people, correcting deficiency is worthwhile when it is present. Treating vitamin D as a fat-loss solution is usually a distraction from the habits and structures that actually drive progress and keep it going.
References
- Vitamin D – Health Professional Fact Sheet 2025 (Government Fact Sheet)
- Vitamin D for the Prevention of Disease | Endocrine Society 2024 (Guideline)
- Association of Body Weight With Response to Vitamin D Supplementation and Metabolism 2023 (Cohort Study)
- Effect of vitamin D supplementation on body composition, lipid profile, and glycemic indices in patients with obesity-associated metabolic syndrome: a systematic review and meta-analysis 2025 (Systematic Review)
- Vitamin D supplementation positively affects anthropometric indices: Evidence obtained from an umbrella meta-analysis 2022 (Umbrella Meta-Analysis)
Disclaimer
This article is for general educational purposes only and is not a substitute for medical advice, diagnosis, or treatment. Vitamin D deficiency, testing, and supplementation should be discussed with a qualified clinician when symptoms, medical conditions, medications, or high-dose supplements are involved.
If this article helped you, please consider sharing it on Facebook, X (formerly Twitter), or another platform your audience uses.