Brain fog can feel like slow thinking, poor concentration, word-finding trouble, forgetfulness, or a sense that your mind is not as sharp as usual. Vitamin B12 deficiency is one possible cause, especially when cognitive symptoms come with fatigue, numbness, tingling, balance problems, anemia, digestive conditions, medication risk factors, or a diet low in animal-based foods.
Testing matters because B12 deficiency is treatable, but it can be missed. Some people develop nerve or cognitive symptoms before obvious anemia appears. At the same time, brain fog has many other causes, so B12 testing is most useful when symptoms and risk factors make deficiency plausible, or when a clinician is ruling out common medical contributors to cognitive changes.
Table of Contents
- When B12 Testing Matters
- How B12 Affects Brain Function
- Symptoms That Raise Suspicion
- Risk Factors for Low B12
- B12 Tests and Result Interpretation
- What Happens After Testing
- When to Look Beyond B12
When B12 Testing Matters
Vitamin B12 testing is most useful when brain fog is persistent, unexplained, or accompanied by symptoms that fit a possible deficiency. It is not a universal answer for every episode of poor focus, but it is a reasonable part of a medical workup when the pattern points beyond ordinary tiredness or stress.
Brain fog from B12 deficiency is usually not a single isolated symptom. People may describe slower thinking, trouble concentrating, forgetfulness, low mental energy, or feeling detached from their usual sharpness. These symptoms overlap with sleep loss, depression, anxiety, thyroid disease, iron deficiency, medication effects, blood sugar swings, long COVID, menopause, substance use, and many neurological conditions. That overlap is why testing works best as part of a broader clinical picture rather than as a stand-alone explanation.
Testing becomes more important when cognitive symptoms are new, lasting, worsening, or interfering with work, school, driving, finances, medication management, or daily routines. It also matters when there are neurological clues, such as tingling in the hands or feet, numbness, burning pain, balance changes, clumsiness, walking difficulty, or reduced sense of vibration or position. These symptoms can suggest nerve involvement, which deserves timely evaluation.
A clinician may also order B12 testing during a broader assessment of fatigue, memory change, depression-like symptoms, or poor concentration. In that context, B12 is often checked along with a complete blood count, thyroid tests, iron studies, folate, metabolic markers, and sometimes blood sugar testing. For a broader view of how clinicians approach similar symptoms, see brain fog testing and poor concentration.
Testing is especially relevant because B12 deficiency can exist without obvious anemia. Some people assume their B12 status is fine if their hemoglobin is normal, but neurological or cognitive symptoms may appear before classic blood-count changes. A normal complete blood count does not always end the question if the symptom pattern and risk factors still fit.
That said, B12 testing is not usually recommended as routine screening for people with no symptoms and no risk factors. Low-normal or borderline results can be hard to interpret, and unnecessary testing can lead to confusion, repeat labs, or supplements that obscure the diagnosis later. The decision is strongest when testing can answer a practical question: Could a treatable deficiency be contributing to these symptoms, and would the result change next steps?
How B12 Affects Brain Function
Vitamin B12 supports nerve health, red blood cell formation, DNA synthesis, and key metabolic pathways involved in brain and nervous system function. When levels are too low, the effects may show up as cognitive, mood, sensory, or balance symptoms.
B12 is needed for myelin maintenance. Myelin is the protective covering around many nerves that helps signals travel efficiently. When B12 deficiency affects myelin and nerve function, symptoms can include tingling, numbness, burning sensations, altered vibration sense, balance problems, and in more serious cases, spinal cord involvement. Cognitive symptoms may appear alongside these nerve signs or may be the main complaint early on.
B12 is also involved in one-carbon metabolism, a set of biochemical pathways that helps regulate methylation and homocysteine. When B12 is low, methylmalonic acid and homocysteine may rise. These markers are not “brain fog tests” by themselves, but they can help show whether the body is functionally short of usable B12.
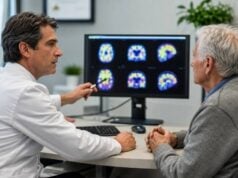
The mental and emotional symptoms of B12 deficiency can be subtle. Some people report mental fatigue, slowed processing, low mood, irritability, apathy, or reduced motivation. In older adults, B12 deficiency may be considered during evaluation for cognitive decline, especially when symptoms develop with gait change, neuropathy, anemia, weight loss, malnutrition, or gastrointestinal risk factors. B12 deficiency is not the same as dementia, but it is one of the medical issues clinicians may look for because it is potentially reversible or improvable.
The relationship between B12 and cognition is not simple. Low B12 can contribute to cognitive symptoms, but taking B12 does not reliably improve brain performance in people who are not deficient. Supplements are most medically meaningful when they correct a true deficiency, address a high-risk situation, or prevent deficiency in someone with reduced intake or absorption.
This distinction is important for brain fog. If symptoms come from B12 deficiency, treatment may help, although nerve recovery can be slow and sometimes incomplete if deficiency has been severe or prolonged. If symptoms come from sleep apnea, hypothyroidism, depression, iron deficiency, medication side effects, or blood sugar instability, B12 alone will not solve the underlying problem. That is why testing matters: it helps separate a plausible deficiency from guesswork.
For readers trying to understand B12’s broader role in cognition and nerve symptoms, B12 and brain function may be a useful companion topic.
Symptoms That Raise Suspicion
B12 deficiency becomes more likely when brain fog appears with neurological, blood-related, digestive, or dietary clues. The more of these clues are present, the more useful testing becomes.
Common symptoms and signs that may support B12 testing include:
- Persistent fatigue, weakness, or reduced stamina
- Brain fog, poor concentration, forgetfulness, or slowed thinking
- Numbness, tingling, burning, or “pins and needles” in the hands or feet
- Balance problems, unsteady walking, clumsiness, or falls
- Sore tongue, mouth ulcers, appetite changes, or unexplained weight loss
- Pale skin, shortness of breath, dizziness, or palpitations related to anemia
- Low mood, irritability, apathy, or personality change
- Memory concerns, especially when paired with neuropathy or gait changes
Some symptoms are nonspecific. Fatigue and poor concentration are common in many conditions. Numbness and tingling can come from diabetes, thyroid disease, nerve compression, alcohol use, autoimmune disease, medication effects, or anxiety-related hyperventilation. Memory complaints can be caused by sleep deprivation, depression, stress, menopause, ADHD, medication side effects, or early neurocognitive disorders. B12 testing is useful because it can identify one treatable contributor, not because it explains every symptom.
A key safety point is that neurological symptoms deserve attention even without anemia. Classic teaching links B12 deficiency with megaloblastic anemia, but cognitive and nerve symptoms do not always wait for obvious blood-count changes. Someone with tingling, balance changes, and brain fog should not assume B12 is normal just because they have not been told they are anemic.
Sudden symptoms are different. B12 deficiency usually develops gradually. Sudden confusion, one-sided weakness, facial drooping, new trouble speaking, new severe headache, chest pain, fainting, new seizures, or rapidly worsening walking problems need urgent medical evaluation. Severe depression, suicidal thoughts, hallucinations, or dangerous behavior also require prompt professional help. A gradual B12 workup should not delay urgent care for possible stroke, severe infection, metabolic crisis, medication toxicity, or acute psychiatric emergency. For a more general safety framework, see urgent neurological or mental health symptoms.
It is also worth noting that “brain fog” can be hard to describe during an appointment. Specific examples help: missing familiar turns while driving, rereading the same paragraph repeatedly, forgetting bills, losing track of conversations, making unusual work errors, or struggling with tasks that used to be automatic. These examples help clinicians decide whether the issue sounds like attention, memory, language, sleepiness, mood, medication effect, or a neurological problem.
Risk Factors for Low B12
B12 testing is more likely to be helpful when brain fog occurs in someone with reduced B12 intake, impaired absorption, certain medication exposures, or gastrointestinal surgery. Risk factors often matter as much as the symptom itself.
Vitamin B12 is found naturally in animal-based foods such as meat, fish, eggs, and dairy, and it may be added to fortified foods. People who follow vegan diets, and some people who follow vegetarian or very restricted diets, may not get enough B12 unless they use reliable fortified foods or supplements. Dietary deficiency can develop gradually because the body stores B12, but intake still matters over time.
Absorption problems are another major pathway. B12 from food must be released in the stomach, bind to intrinsic factor, and be absorbed in the terminal ileum, the last part of the small intestine. Problems at any step can lead to deficiency. Autoimmune gastritis, historically associated with pernicious anemia, can reduce intrinsic factor and stomach acid. Gastric bypass, gastrectomy, ileal resection, Crohn disease affecting the ileum, untreated celiac disease, and other malabsorptive conditions can also increase risk.
Medication history matters. Long-term metformin, proton pump inhibitors, H2 blockers, and some other medicines have been associated with lower B12 status in certain people. This does not mean these medicines should be stopped without medical advice. It means persistent cognitive, nerve, or anemia symptoms in someone taking these medicines may justify testing and review.
Nitrous oxide exposure is a special case. Recreational nitrous oxide can inactivate B12 and cause serious neurological problems, sometimes even when standard B12 levels are not clearly low. Someone with nitrous oxide exposure plus numbness, weakness, balance problems, bladder changes, or cognitive symptoms needs prompt medical assessment.
Older adults are also at higher risk because reduced stomach acid, autoimmune gastritis, medications, dietary changes, and other illnesses become more common with age. In older adults, B12 deficiency may be assessed during workups for memory loss, gait changes, neuropathy, anemia, depression-like symptoms, or functional decline.
Other contexts that may increase concern include pregnancy or breastfeeding with low intake or known deficiency, eating disorders or malnutrition, heavy alcohol use, chronic gastrointestinal symptoms, and a personal or family history of autoimmune conditions. If fatigue and brain fog are prominent, clinicians may also check related contributors such as iron status; iron and ferritin testing is often relevant when fatigue, restless legs, or low stamina are part of the picture.
Risk factors do not prove deficiency, and the absence of risk factors does not completely rule it out. But in practice, risk factors help decide when B12 testing is a targeted, useful step rather than a random lab.
B12 Tests and Result Interpretation
B12 testing is not as simple as “normal” or “low” in every case. Total B12 is commonly used first, but active B12, methylmalonic acid, homocysteine, blood counts, and cause-focused tests may be needed when results are borderline or the clinical picture is unclear.
A typical workup may include several of the following:
| Test | What it helps show | Important limitations |
|---|---|---|
| Total serum B12 | Measures B12 circulating in the blood and is often the first test ordered. | Can be borderline, falsely reassuring, or affected by binding proteins and supplements. |
| Active B12 | Measures holotranscobalamin, the fraction more available to cells. | Not available everywhere and still must be interpreted with symptoms and risk factors. |
| Methylmalonic acid | Can rise when cells do not have enough usable B12. | May be elevated with kidney disease and is not perfect in every patient. |
| Homocysteine | Can rise with B12 deficiency and may support a functional deficiency pattern. | Also rises with folate deficiency, vitamin B6 deficiency, kidney disease, hypothyroidism, and other factors. |
| Complete blood count | Checks for anemia, large red blood cells, and other blood abnormalities. | Can be normal even when neurological B12 symptoms are present. |
| Intrinsic factor antibody and related tests | Help evaluate autoimmune gastritis or pernicious anemia when suspected. | A negative intrinsic factor antibody test does not fully rule out autoimmune gastritis. |
Result interpretation depends on the laboratory and the clinical context. Some current guidance uses categories similar to these: total B12 below about 133 pmol/L may support likely deficiency, about 133 to 258 pmol/L may be indeterminate, and levels above that range may make deficiency less likely. For active B12, values below about 25 pmol/L may support deficiency, while 25 to 70 pmol/L may be indeterminate. Exact cutoffs vary, so the lab’s reference range and the clinician’s judgment matter.
Borderline results are common. A person with brain fog, tingling, gait change, and a borderline total B12 may need methylmalonic acid or homocysteine testing, or treatment while further testing is pending if symptoms are concerning. A person with no symptoms and a borderline result may need a different approach, such as repeat testing, dietary review, or monitoring.
Supplements can complicate interpretation. Taking B12 before testing may raise blood levels without proving that the underlying cause has been corrected, especially if symptoms are ongoing. When possible, diagnostic blood samples are often taken before starting treatment. However, treatment should not be dangerously delayed in someone with significant neurological symptoms.
B12 results also need to be considered alongside other common brain fog labs. Thyroid disease can mimic cognitive slowing, fatigue, mood changes, and poor concentration, so thyroid testing for brain fog may be part of the same workup. Blood sugar and A1C testing may also be relevant when symptoms fluctuate with meals, energy crashes, thirst, urination changes, or diabetes risk.
What Happens After Testing
The next step after B12 testing depends on whether deficiency is confirmed, borderline, unlikely, or still clinically suspected despite imperfect labs. Treatment decisions should be based on the cause, severity, symptoms, and whether absorption is likely to be reliable.
If testing confirms B12 deficiency, clinicians usually look for the cause rather than simply replacing B12 and moving on. A dietary cause may be addressed with reliable oral supplementation and diet planning. A malabsorption cause may require long-term or lifelong treatment. Autoimmune gastritis, major gastric surgery, or terminal ileal resection often changes the treatment plan because oral absorption may be inadequate or unreliable.
Treatment may be oral or intramuscular. Oral B12 can work well for many people with dietary deficiency and some less severe cases. Intramuscular B12 is often preferred when symptoms are significant, neurological signs are present, adherence is uncertain, or malabsorption is confirmed or strongly suspected. The dose and schedule vary by country, formulation, severity, and cause.
People often want to know how fast brain fog should improve. Some symptoms may begin improving within a few weeks, but recovery can take months. Blood abnormalities may correct faster than nerve symptoms. Tingling, numbness, balance problems, and cognitive symptoms can improve gradually, and recovery may be incomplete if deficiency has been severe or long-standing. This is one reason early testing matters when neurological symptoms are present.
Follow-up is not just about repeating a number. A good follow-up asks whether symptoms are improving, whether new symptoms have appeared, whether the person is taking the correct dose, and whether the cause has been addressed. If symptoms worsen or do not improve, clinicians may reconsider the diagnosis, check functional markers, adjust the route or dose, review adherence, or evaluate other causes.
If autoimmune gastritis is suspected, additional testing may include intrinsic factor antibodies, parietal cell antibodies, gastrin testing, celiac screening, or gastroenterology referral in selected cases. The goal is to identify whether the deficiency is reversible, medication-related, diet-related, or due to a long-term absorption problem.
People should avoid assuming that an over-the-counter B12 supplement is enough for every situation. Supplements vary in dose and form, and a person with neurological symptoms or malabsorption may need a specific medical regimen. At the same time, very high B12 blood levels after supplementation do not necessarily mean the original symptoms were caused by B12 deficiency or that all other causes have been ruled out.
If testing shows B12 deficiency is unlikely, the workup should not stop if brain fog is still affecting daily life. The result is useful because it redirects attention to other explanations rather than leaving the person guessing.
When to Look Beyond B12
B12 is only one part of a careful brain fog evaluation. If B12 results are normal, symptoms persist after treatment, or the symptom pattern does not fit deficiency, it is important to look for other medical, sleep, mood, medication, and neurological causes.
A broader workup may consider:
- Sleep disorders, especially sleep apnea, insomnia, circadian rhythm problems, or chronic sleep deprivation
- Thyroid disease, diabetes, prediabetes, blood sugar swings, kidney or liver problems
- Iron deficiency, folate deficiency, vitamin D deficiency, dehydration, or undernutrition
- Depression, anxiety, trauma-related symptoms, burnout, grief, or chronic stress
- Medication side effects, alcohol use, cannabis use, sedating antihistamines, or polypharmacy
- Long COVID, autoimmune disease, chronic infection, migraine, concussion, or neurological disorders
- Hormonal transitions such as perimenopause, pregnancy, postpartum changes, or endocrine disorders
Sleep deserves special attention because poor sleep can look very similar to cognitive dysfunction. Daytime sleepiness, morning headaches, snoring, gasping, high blood pressure, and waking unrefreshed may point toward sleep apnea or another sleep disorder. In that setting, a sleep study for brain fog and fatigue may be more useful than repeating vitamin labs.
Cognitive testing may be considered when symptoms are persistent, measurable, or affecting independence. Brief screening tests can help identify whether memory, attention, processing speed, language, or executive function is affected. More detailed neuropsychological testing may be useful when symptoms are complex, when work or school functioning is impaired, or when clinicians need to distinguish attention problems, mood-related cognitive symptoms, neurological disease, or recovery after injury. For a general explanation, see what cognitive testing measures.
It is also possible to have more than one contributor. A person may have borderline B12, poor sleep, low ferritin, and anxiety. Another may have treated B12 deficiency but ongoing cognitive symptoms from sleep apnea or depression. Improvement often requires identifying the full pattern rather than focusing on a single lab value.
The most practical approach is to treat confirmed deficiency, monitor symptom response, and keep evaluating if the story does not fit. B12 testing matters because it can catch a treatable cause of brain fog and nerve symptoms. It matters even more when it is used wisely: before prolonged symptoms are dismissed, but without assuming every foggy day is a vitamin problem.
References
- Vitamin B12 deficiency in over 16s: diagnosis and management 2024 (Guideline)
- Evidence review for diagnostic tests 2024 (Evidence Review)
- Vitamin B12 deficiency: testing and treatment 2026 (Review)
- A Brief Overview of the Diagnosis and Treatment of Cobalamin (B12) Deficiency 2024 (Review)
- Diagnosis, Treatment and Long-Term Management of Vitamin B12 Deficiency in Adults: A Delphi Expert Consensus 2024 (Consensus Review)
- Pernicious Anemia: The Hematological Presentation of a Multifaceted Disorder Caused by Cobalamin Deficiency 2022 (Review)
Disclaimer
This article is for general educational purposes only. Brain fog, memory changes, numbness, balance problems, anemia, and mood symptoms can have many causes, and B12 testing or supplementation should not replace professional medical evaluation, diagnosis, or treatment. Seek urgent care for sudden confusion, stroke-like symptoms, severe weakness, new seizures, suicidal thoughts, or rapidly worsening neurological symptoms.
Please share this article on Facebook, X (formerly Twitter), or your preferred platform to help others understand when B12 testing may matter for brain fog.